What a Rash After Surgery Could Mean
Near Incision or Elsewhere on the Body
Medically reviewed by David Hampton, MD
Surgery doesn't just impact the surgical site. Research shows that surgery can trigger a chain reaction of events throughout the body. These systemic reactions—as well as those linked to surgical tools and medications—are relatively common. Rashes are one type of these reactions that can develop after surgery for various reasons.
This article explores what a postoperative rash looks like, what these rashes could mean for your overall health and recovery, and available treatment options.
Justin Paget / Getty Images
Rash Location After Surgery
There are several reasons you may develop a rash after surgery. Some are linked to medications, cleansers, and other substances used during or after surgery. Others are related to your body's internal reaction to the medications and even the surgery itself.
The location, texture, color, and associated symptoms help healthcare providers identify the cause and proper treatment for a rash after surgery.
On or Around Incision
Disinfectants healthcare providers use to clean the skin before and after surgery, as well as tapes, glues, and other adhesives to close the surgical wound, are often associated with rashes at the surgical site.
Several studies reference rashes associated with various disinfectants. These rashes can appear on or near the surgical site.
These localized rashes are typically associated with cleansers like:
Chlorhexidine digluconate
Olanexidine glucuronide (Olanedine)
Disinfectants containing chlorhexidine decrease surgical site infections. However, these substances are also linked to contact dermatitis (skin irritation) and other skin reactions.
Adhesives like tape can also cause localized skin reactions, but many studies have identified surgical glue as the underlying cause of post-op rashes. One study estimates the overall prevalence of rashes from surgical glue to be around 2.8%. Surgeons often use these adhesives along with traditional sutures to provide a barrier against bacteria and promote quicker healing with less scarring.
People concerned about or at risk for reactions to disinfectants or surgical glues should have a skin patch test before surgery to identify sensitivities and prevent larger reactions.
Spreading to Other Body Parts
A rash that appears across larger areas of your body is usually a sign of a systemic (widespread) infection and is often the result of an allergic reaction to medications such as anesthesia, antibiotics, or neuromuscular blockades.
Immediate or delayed reactions to these medications can cause widespread rashes, hives, and other symptoms of an allergic reaction. Some of the most common medications associated with systemic rashes and other immediate or delayed reactions include the following:
Ceftriaxone (antibiotic)
Vancomycin (antibiotic)
Metronidazole (antibiotic)
Amoxicillin (antibiotic)
Piperacillin-tazobactim (antibiotic)
Augmentin (antibiotic)
Trimethoprim-sulfamethoxazole (antibiotic)
Dapsone (antibiotic)
Minocycline (antibiotic)
Oxcarbazepine (antiepileptic/nerve pain)
Levetiracetam (antiepileptic/nerve pain)
Carbamazepine (antiepileptic/nerve pain)
Thiopentone (anesthesia induction agent)
Propofol (anesthesia induction agent)
Midazolam (anesthesia induction agent)
Ketamine (anesthesia induction agent)
Succinylcholine (neuromuscular blocking drug)
Rocuronium (neuromuscular blocking drug)
Atracurium (neuromuscular blocking drug)
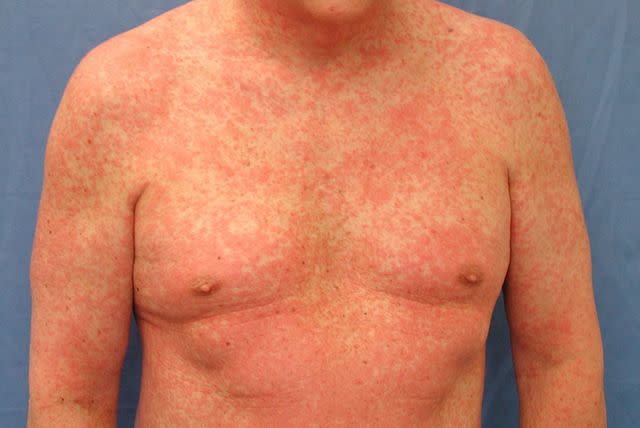
Reproduced with permission from © DermNet New Zealand www.dermnetnz.org 2023.
Learn More: 13 Pictures of Common Skin Rashes
When Are Post-Op Rash Symptoms Serious?
Skin rashes or hives are one of the more common ways a local or systemic allergic reaction may appear. However, anaphylactic reactions that impact your breathing are also possible with many of these medications.
In rare cases, it's possible to develop a widespread, multiorgan—and possibly fatal—reaction to certain medications used in surgery. This reaction is called a drug reaction with eosinophilia, and systemic symptoms (DRESS) can appear days or weeks after using certain medications. These hypersensitivity reactions can begin with a rash and lead to multiorgan failure if left untreated. They are primarily associated with certain antibiotics.
Provider Follow-Up vs. Emergency Room Visit
If you have recently had surgery and developed a local reaction or widespread rash without symptoms of anaphylaxis, follow up with your surgeon.
If you suddenly develop symptoms of anaphylaxis, such as difficulty breathing or swallowing, do not wait to be seen at an outpatient provider's office; seek immediate medical care at your nearest hospital emergency department.
Related: A Guide to Which Rashes You Should Worry About
Types of Surgical Glue and Allergy Risk
Healthcare providers have access to several materials for surgical adhesives; the overall allergy risk for each is unclear. Most studies that examined the link between surgical glue and rashes or other allergic reactions studied the adhesive Dermabond. However, other surgical glues have the same active ingredient—octyl-2-cyanoacrylate. These include:
SurgiSeal
LiquiBand Flex
OctylSeal
If you have a history of adhesive, tape, or latex allergies, talk to your surgical team before your operation about patch testing and closure options.
Related: Drug and Latex Allergies
Wound Care With Rash
Anti-itch, antihistamine, and anti-inflammatory medications can help manage rash symptoms. Some of these medications may also be used to manage systemic reactions after surgery.
Your surgical team will give you specific instructions for wound care after surgery, which should include information about how to spot an infection or other problems with healing. Rashes and other inflammatory reactions can make your skin more susceptible to bacteria and may increase your risk of developing a larger infection at your surgical site.
If you have a rash over your incision or other concerning symptoms after your surgery, call your surgical team for instructions on how to proceed. Your healthcare team may suggest additional wound care or, in severe cases, additional surgeries or removal of surgical implants.
Treatment for DRESS
If you develop a severe reaction like DRESS after surgery, treatment may include a combination of things steroids, corticosteroids, intravenous immunoglobulin (IVIG), and additional follow-up care depending on the extent of organ damage.
Timeline: How Long Does a Rash After Surgery Last?
Most rashes caused by hypersensitivity or allergic reactions to a medication or irritant clear up in about a week. A rash that lasts longer may require additional treatment. If you developed hives with your reaction, it may be several weeks before your skin returns to baseline.
See your healthcare provider for rashes that last a week or more or worsen throughout the week—with or without treatment.
Related: Alphabetical List of Common Rashes and Their Causes
Summary
Surgery involves various substances, such as disinfectants, surgical tools, anesthesia, and antibiotics, any of which could trigger a reaction. Rashes are one of the more common reactions you may notice after surgery.
In most cases, these rashes are minor, and you can discuss how best to manage them with your surgical team. However, rashes that appear with other signs of illness, like an infection or anaphylaxis, require immediate treatment. Before any medical procedure, ensure your list of allergies is up-to-date. You may also consider allergy or skin patch testing before surgery.
Read the original article on Verywell Health.

