Vasculitis Rash: Symptoms to Know and Treatment Options
Medically reviewed by Susan Bard, MD
Vasculitis is a diverse group of diseases characterized by inflammation of small, medium, or large blood vessels within the body. It can occur in any organ, including the skin, and depending on the severity of inflammation, it can present in different ways.
Skin manifestations from vasculitis—what's known as cutaneous vasculitis—commonly arise on the lower legs as purple, red, or brown bumps. However, other locations and findings, such as open sores, blisters, and patterns of skin discoloration, are also possible.
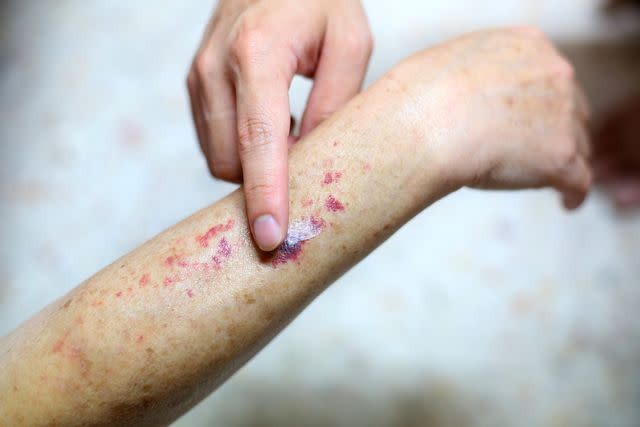
This article will review the unique appearances, potential causes, accompanying symptoms, and treatment of a vasculitis rash.
Vasculitis Rash Symptoms
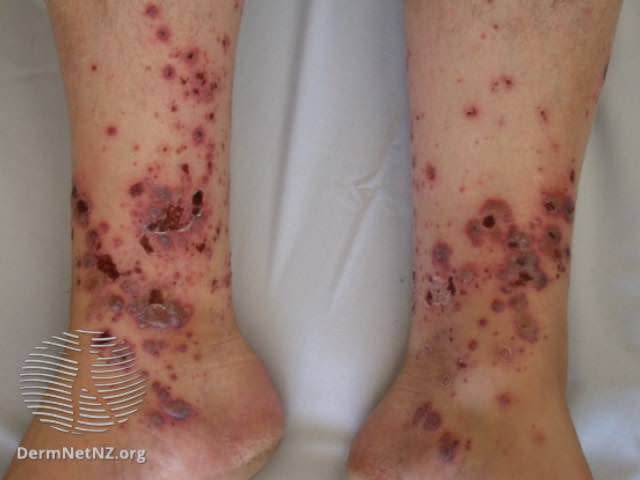
DermNet / CC BY-NC-ND
The skin is a waterproof protective barrier between a person's inner body and the environment. It's divided into three layers, as follows:
The epidermis is the outer layer of skin, containing dead skin cells and brown pigment-producing cells (melanocytes).
The dermis is the middle layer of the skin, containing blood vessels, nerves, hair follicles, and oil and sweat glands.
The hypodermis is the deepest subcutaneous layer. It comprises blood vessels, nerves, and fatty tissue, providing insulation and storing calories.
Learn More: The Anatomy of the Skin
A vasculitis rash indicates that blood vessels within the dermis or hypodermis are damaged, causing their walls to swell, weaken, narrow, thicken, bulge, or leak.
Location
Rashes from vasculitis most commonly appear on the lower legs but can occur anywhere, especially in areas prone to trauma or pressure. For example, a vasculitis rash can develop on the feet, thighs, buttocks, arms, trunk, head, and neck.
Onset of Symptoms
There are different types of vasculitis rashes. While they may occur at any age, they are more common in adults than children.
The specific onset of rash symptoms depends on various factors, such as the underlying trigger. For instance, a vasculitis rash that develops as a reaction to a medication often develops seven to 10 days after the drug exposure.
Moreover, vasculitis rashes can arise suddenly or gradually. They can also evolve in appearance over time as the blood vessels become more and more damaged.
Appearance and Shape
A vasculitis rash involving small blood vessels occurs in the top portion of the dermis.
Cutaneous small vessel vasculitis, formerly called hypersensitivity vasculitis, is the most common vasculitis rash. It usually arises from a reaction to a drug or infection.
With this condition, inflamed small blood vessels in the skin become leaky, and small areas of bleeding develop, causing raised, red, purple, or brown spots (depending on skin tone) to form on the legs, known as palpable purpura.
Another type of cutaneous small vessel vasculitis is exercise-induced vasculitis, also called golfer's vasculitis or the Disney rash. This rash develops on one or both legs after prolonged exposure in hot weather, such as below the leg opening of shorts that people would wear playing golf or at theme parks. It appears as red patches, purpura, or weals (itchy, red, or skin-colored welts).
Other possible skin findings in small vessel vasculitis include:
Petechiae: Pinpoint, flat dots that are purple, red, or brown
Ulcers: Open sores on the skin's surface
Nodules: Lumps underneath the skin
Hemorrhagic bullae: Blood-filled blisters
Atrophic papules: Red raised spots with a white, depressed center

Reproduced with permission from ©DermNet New Zealand and © Raimo Suhonen www.dermnetnz.org 2023.
PurpuraRelated: Distinguishing Petechiae From Purpura
Medium Vessel
A vasculitis rash involving medium blood vessels occurs deep in the dermis or the subcutaneous layer. Skin findings may include:
Subcutaneous nodules: Firm lumps, often tender, felt deep underneath the skin
Infarcts: Purple or black patches representing dying (necrotic) tissue from poor blood flow
Deep ulcers: Open wound or crater extending far into the skin
Livedo racemosa: Broken, irregularly patterned reddish-violet skin discoloration
Livedo reticularis: Lacelike, reddish-blue to purple skin discoloration
Related: Causes and Pictures of Livedo Reticularis
Large Vessel
Skin manifestations are rare with large vessel vasculitis, although they can occur with giant cell arteritis.
This type of vasculitis primarily affects the branches of the external carotid artery, a large artery in the neck. It causes symptoms like headache, scalp tenderness, visual disturbances, and jaw pain when chewing.
If skin findings are present, they may include:
Thickening or, less commonly, redness or nodules of the arteries in the temple
Necrosis of the scalp and tongue
Bruising around the eyes (periorbital ecchymosis)
Sensations
Pain, itching, stinging, tingling, numbing, or burning sensations can accompany vasculitis rashes.
Rash, Vascular Disease, and Inflammation
Skin manifestations of vasculitis are related to impaired blood vessel structure and function from inflammation.
The cause of the inflammation in vasculitis varies, potentially stemming from one of the following:
Infection—for example, the viruses human immunodeficiency virus (HIV) and hepatitis B or C, and the bacteria Streptococcus pyogenes
Medication or drug exposure—for example, nonsteroidal anti-inflammatory drugs (NSAIDs), antibiotics, thiazide diuretics (water pills), and cocaine
Autoimmune diseases, namely rheumatoid arthritis, lupus, or Sjögren's syndrome
The inflammatory bowel diseases Crohn's disease and ulcerative colitis
Cancer, especially lymphoma and multiple myeloma
How to Confirm If You Have Vasculitis Rash
If you think you have a vasculitis rash, it's important to see a healthcare provider and, if possible, a dermatologist (a physician specializing in skin diseases).
During the diagnostic process, a dermatologist will:
Analyze your symptoms
Look for abnormalities in a physical examination
Evaluate the results of various tests, including blood work and a skin biopsy
Medical History and Physical Exam
When evaluating for possible cutaneous vasculitis, a dermatologist will ask about skin symptoms, drug exposures, family medical histories, and past or present health conditions, such as a recent viral infection.
They will also inquire about other non-skin symptoms, which, if present, can suggest systemic vasculitis (affecting other areas of the body) or an underlying disease.
Systemic vasculitis indicates that blood vessels in organs other than the skin—for example, the liver, kidney, joints, or nerves—are inflamed.
Symptoms of Systemic Vasculitis
Systemic vasculitis is a more serious, potentially dangerous condition than vasculitis limited to the skin. Symptoms of systemic vasculitis can include:
Fever, chills, and night sweats
Unintended weight loss
Fatigue and malaise (generalized feeling of being unwell)
Joint and muscle aches
Abdominal pain
Blood in the urine or stool
Numbness and weakness
Cough or sinus inflammation
Vision changes
Next, a dermatologist will carefully inspect the affected skin area and perform a complete body examination.
Skin Biopsy
A skin biopsy is necessary to confirm or exclude a diagnosis for any skin finding resembling a vasculitis rash.
Though there are different types of skin biopsy techniques, a punch biopsy is often used when a vasculitis rash is suspected because it can go deep into the skin's layers.
During a punch biopsy, a dermatologist will perform the following steps:
Clean and disinfect an area of the skin where the rash is present.
Inject the targeted area with a numbing medication. This may cause a slight stinging sensation.
"Punch" into the skin using a tube-shaped device to remove a small skin sample.
Apply pressure to the biopsied area and, depending on its size, potentially close it with stitches.
Gently place petroleum jelly and a bandage over the skin.
The obtained skin sample will then be sent to a laboratory, where a pathologist (a physician who analyzes tissues) will examine it under a microscope for signs of blood vessel damage.
Other Diagnostic Tests
Initial tests commonly ordered when vasculitis is suspected include:
A complete blood count (CBC) can provide clues about the trigger of vasculitis, such as infection, blood cancer, or autoimmune disease. It can also help rule out alternative diagnoses (e.g., platelet disorders)
A comprehensive metabolic panel (CMP) evaluates for kidney and liver problems.
An erythrocyte sedimentation rate (ESR) checks for nonspecific inflammation in the body
A urinalysis looks for blood or protein in the urine.
Rule Out Alternative Diagnoses
Several conditions may mimic a vasculitis rash. Examples include:
Insect bite reactions (e.g., bedbug bites)
Chronic sun exposure (solar purpura)
Poor circulation in the legs (stasis dermatitis)
Infection of a heart valve's inner lining (infective endocarditis)
Blood-clotting disorders (e.g., antiphospholipid syndrome)
Acute or chronic hives (urticaria)
Pyoderma gangrenosum (rare skin disorder causing painful, open wounds on the legs)
How to Treat Acute Vasculitis Rash
Most vasculitis rashes (without systemic involvement) resolve on their own with simple home therapies.
These therapies include:
Rest, especially avoiding prolonged standing or walking
Elevation and compression of the affected area
Pain relief with an NSAID, such as Advil or Motrin (ibuprofen) or Aleve (naproxen)
Eliminating or managing underlying triggers (e.g., discontinuing a medication or taking an antiviral for a viral infection).
Though vasculitis rashes tend to go away over a few weeks, in some cases, new skin findings can develop over several weeks to months before resolving completely. Rarely does vasculitis limited to the skin recur or become chronic.
If a vasculitis rash is unresponsive to the above interventions or recurrent, corticosteroids ("steroids") taken by mouth may be prescribed. Alternative medication options include colchicine or dapsone.
If systemic vasculitis is present, strong medications that suppress the immune system, such as Imuran (azathioprine), CellCept (mycophenolate mofetil), or Rituxan (rituximab), are often considered.
Learn More: Vasculitis Medications: List of Options for Mild to Severe Symptoms
When to Check In With a Healthcare Provider
See a healthcare provider if you have any skin findings or other symptoms of vasculitis. The spectrum of vasculitis in terms of organ involvement and severity is broad, and some types that involve the skin can progress quickly and be serious.
A prompt and accurate diagnosis is necessary to create the most effective treatment plan.
Summary
Vasculitis is a condition of blood vessel inflammation that may occur in any organ, including the skin. The most common vasculitis rash affects the lower legs and appears as palpable red, purple, or brown spots, depending on skin tone.
Other vasculitis skin findings include lumps, open sores, blisters, and blotchy, lacelike discoloration. Itching, stinging, numbing, or burning sensation can accompany such findings.
There are many possible causes of a vasculitis rash, such as infection or drug exposure. In some cases, the rash is a sign of systemic vasculitis or an underlying disease process like cancer or an autoimmune condition.
A skin biopsy is the hallmark diagnostic test for vasculitis rash. Treatment depends on the severity of the rash, the underlying trigger, and whether or not other organs are involved.
Most vasculitis rashes resolve within a few weeks with simple measures like rest, pain control, and elimination or management of the underlying trigger. For severe or recurrent vasculitis rashes and systemic vasculitis, oral medications that suppress the immune system are considered.
Read the original article on Verywell Health.

