How Do Trans Men Breastfeed Their Babies?

Trevor MacDonald just wants to be the best dad possible for his son, Jacob. As a trans man, however, his version of fatherhood doesn't fit the picture typically painted by pamphlets and self-help books. When he and his partner decided to become pregnant, MacDonald knew he wanted to nurse his son despite having had his breasts removed. He recounts this struggle in a blog post, originally published on the Huffington Post: "I don't know how much I'll be able to breast-feed," he explained to the group of women during his first meeting with La Leche League. "But I really want to try."
Chestfeeding (a spin on "breastfeeding") is a term coined to include trans men who nurse their infants. And if it's new to you, that's understandable - it's not something typically talked about in mainstream pregnancy circles. But a recent article in The Atlantic shed a light on the obstacles trans men face when trying to chestfeed their children and how they're working to make the medical community more inclusive of the practice.
While Dr. Deena Blanchard of Premier Pediatrics is adamant (and most sane people agree) parents should be allowed to make their own decisions when it comes to breastfeeding, she tells Cosmopolitan.com there are benefits of skin-to-skin breastfeeding, as opposed to formula-feeding, that explain why a parent's ability to chestfeed is so important.
"There are immunological benefits," Dr. Blanchard explains. "In such that when you breast-feed, the immunoglobulins [the parent] is making get passed to the baby in the breast milk ... there has been research that suggests that babies who are breastfed get less ear infections, are less likely to get stomach viruses, and that kind of stuff." For many parents, however, it's emotional. "It's very cozy, it increases bonding," she continues.
The term "chestfeeding" is meaningful because it's a neutral term for something that is so often gendered, and recognizing this is the first step toward making chestfeeding more accessible. Here are five things you need to know.
1. The term is applicable to everyone, but accommodates those who undergo a transgender mastectomy or an FTM top surgery. An FTM top surgery is the most common initial procedure for transmasculine patients, according to Dr. Scott Mosser, a cosmetic surgeon in San Francisco, whose work primarily focuses on chest and body contouring surgery.
Depending on the amount of loose skin and breast tissue, the FTM top surgery can be one of three procedures: keyhole surgery (a tiny incision along the border of the areola to remove all of the breast tissue), periareolar surgery (an incision all the way around the areola to remove some skin as well as the breast tissue), or a double incision procedure. The double incision procedure is more extensive, resulting "in a horizontal line across the two sides of the chest, usually located in a similar region to the lower border of the muscle, and then placement of the nipples as skin grafts into the proper location relative to where the muscle borders are on the chest."
Having this surgery, however, doesn't eliminate the possibility of breastfeeding. While milk production will likely be lower than usual, as was the case with MacDonald and many others, it's still completely possible. The bigger obstacle is the heteronormative medical system.
2. There's no one right way to breast- or chestfeed. "It's not an all-or-nothing," Dr. Blanchard says. "And that's where I think people get really tripped up about breastfeeding." There's a misconception parents either feed the baby on the breast or give them formula from a bottle, and nothing in the middle. When a parent is breast- or chestfeeding, this often is not the case.
"If you've had breast surgery and your milk supply is not adequate, you'll just do some supplementing with formula," she explains. "But you're still breastfeeding. So if the baby's drinking breast milk 50 percent of the time, 70 percent of the time, 30 percent of the time, 10 percent of the time, whatever it is, they're still getting the breast milk, and you are still a breastfeeding parent."
Dr. Blanchard believes we should remove the emphasis from one way or the other, and instead work on expanding our definition of breastfeeding so it covers every type of family and opportunity.
3. Like breastfeeding, chestfeeding can have complications. "Generally, if you've had surgery on the breast and it affects the nipple, it can affect your milk supply and often it does," says Dr. Blanchard. In the case of mastectomies or FTM top surgeries, this doesn't mean breastfeeding is impossible - it just comes with some complications.
MacDonald detailed some of these issues in a blog post. Getting his baby to latch, for instance, was solved through persistence. Getting enough milk was the next step.
"When he was four days old, it became clear that he wasn't gaining weight adequately, and that we needed to start supplementing him," MacDonald writes. The family used an SNS, or a supplemental nursing system, in combination with chestfeeding as a compromise.
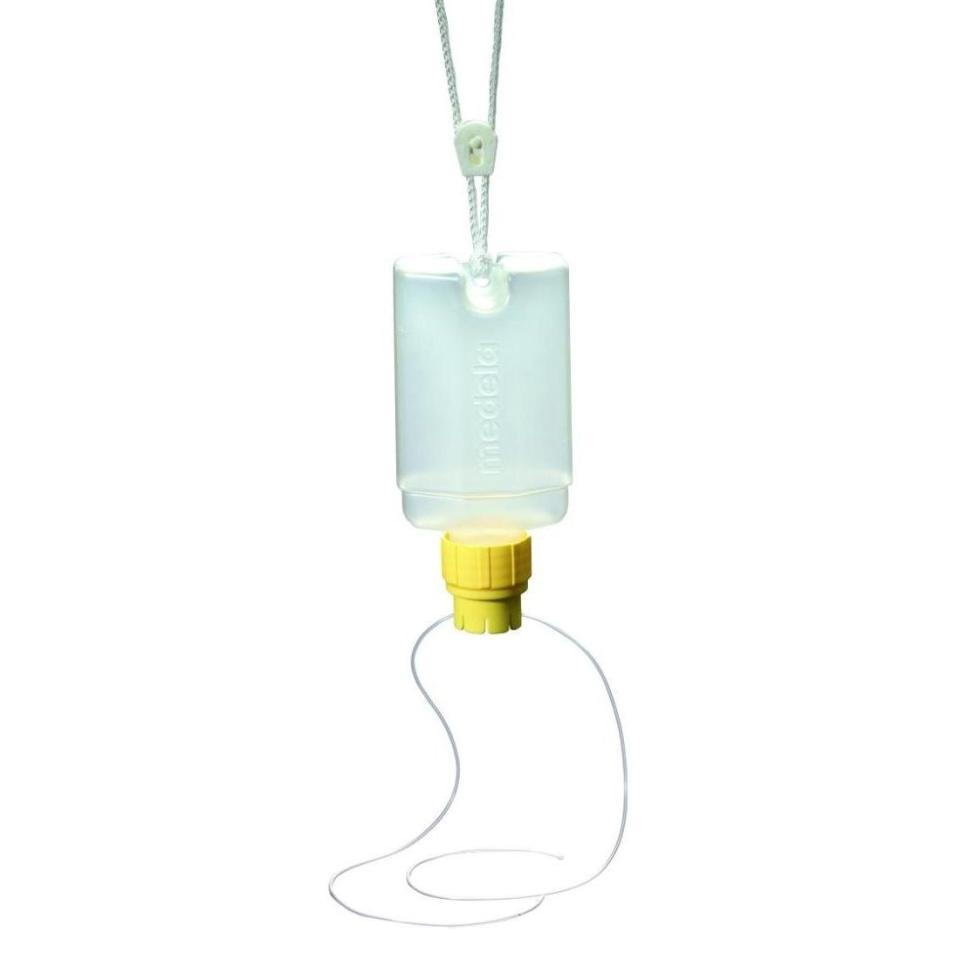
By giving Jacob both MacDonald's nipple and supplementing through the tube of the SNS at the same time, MacDonald created a "breast tissue sandwich" which was effective in giving Jacob the nutrients he needed while still allowing MacDonald to successfully chestfeed.
4. Medical professionals are often not prepared for it. The Atlantic details the necessary next steps toward making chestfeeding easier for trans parents. While an SNS is a helpful tool, there's nothing created specifically for trans parents. In the case of Emmett, who is referred to by first name only in a study conducted by MacDonald on transmasculine experiences with chestfeeding called "Transmasculine individuals' experiences with lactation, chestfeeding, and gender identity," it was a struggle just getting access to the right clothes.
"I was producing a ton of milk," he said. "I had no way to stop the milk from leaking through my chest. I had no appropriate … male clothes for nursing."
Then, there are issues like mastitis (an infection of the breast tissue sometimes caused by a blocked milk duct) and engorgement. Some participants in the study reported their doctors weren't prepared to deal with those conditions because they assumed no milk would come in due to the chest surgery. This indicates trans health issues, especially in regards to pregnancy, are not universally taught.
5. It's not just a physical issue, it's a mental health issue. Two chestfeeding participants in MacDonald's study reported feeling "overwhelming gender dysphoria," struggling with the clash of feeling and presenting as a man, but participating in something we've been conditioned to believe is a solely feminine act. After spending their whole lives knowing they were men, and then undergoing surgery to lessen the dissonance between their mental and physical selves, chestfeeders may feel thrown back into a world of uncertainty, which takes a toll. This is often worsened by doctors who neglect to use inclusive and gender-neutral terminology when interacting with their patients.
This is exactly why MacDonald calls for further research. Not enough doctors are aware of chestfeeding and how to properly address trans patients who are making some difficult decisions. Dr. Mosser says his patients often cite "concerns about sensitivity of their medical practitioners toward their unique circumstances, and concern about having a hysterectomy or removal of the ovaries before making a final decision with regards to whether or not they want to get pregnant in the future."
Here's where there are some unanswered questions. MacDonald says the next step is to take a closer look at the effects of chest-masculinization surgery on lactation and milk production, as well as the effects of testosterone when it comes to nursing. Ultimately, everyone wants the same thing: a safe and healthy baby. It's just important doctors and the medical community acknowledge, facilitate, and celebrate the many ways to get there.
Follow Kathryn on Twitter.

