Medical Infusion Therapy: What It Is and What to Expect
Medical Infusion Therapy: Uses, Benefits, and Side Effects
Medically reviewed by Rochelle Collins, DO
Infusion therapy is a procedure in which medications are delivered directly into the bloodstream, usually with a needle and catheter that's inserted into a vein.
Infusion therapy is needed when a patient cannot take a drug orally. It's also a method of delivering medications in larger or more controlled amounts, such as during chemotherapy for cancer or with pain medication during childbirth.
You can get infusion therapy in a medical setting or at home. Insulin shots are an example of home infusion therapy.
This article explains the uses, benefits, and potential side effects of different kinds of infusion therapy.
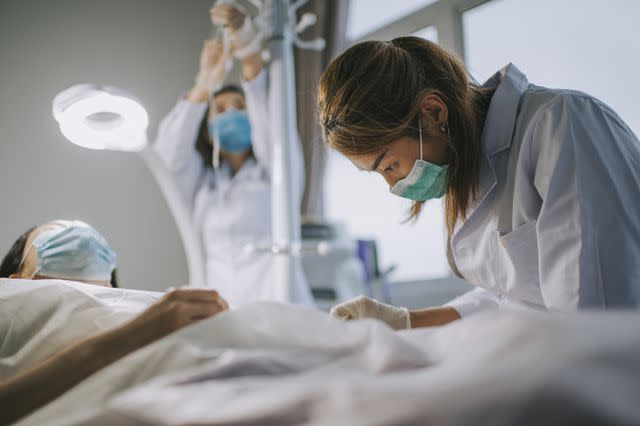
Edwin Tan / Getty Images
Types of Infusion Therapy and Conditions Treated
The types of infusion therapy include:
Intravenous (IV)
Epidural
Subcutaneous
Intravenous (IV)
Intravenous therapy is when medications or fluids are injected directly into the bloodstream. IV therapy is commonly used for:
Maintaining fluids in the body after dehydration, diarrhea, vomiting, or surgery
Chronic conditions, such as chemotherapy or immunotherapy for cancer
Antibiotic therapy (to treat conditions such as Lyme disease and meningitis)
Administering anesthesia before surgery
Blood transfusions
Providing nutrients, like iron and B vitamins, when they are chronically low
Epidural
An epidural is a type of infusion therapy that is inserted around the spinal nerves in the lower back. Epidurals block pain signals from being sent from the spine to the brain. An epidural can administer the following:
Analgesia (pain relief)
Anesthesia (numbing)
Steroids for pain, as with acute back pain
Epidurals are best known as a way to prevent or numb the pain of childbirth, but they can also be used to prevent pain during and after surgery. Epidurals might also help relieve acute pain.
Intramuscular
Intramuscular infusion therapy involves medication inserted into muscle tissue. Uses of intramuscular infusion therapy include:
Hormone therapy, such as testosterone or estrogen injections for cancer treatment
Antibiotics to treat conditions like gonorrhea and syphilis
Vaccines against conditions like diphtheria-tetanus-pertussis (DTaP, Tdap) and Covid-19
Antibodies (immunoglobulins), which are proteins made by cells to help the immune system fight bacteria, viruses, or other harmful substances
Subcutaneous
Subcutaneous infusion therapy involves drugs injected into fat underneath the skin. Subcutaneous injection sites include the upper arms, stomach, upper thighs, lower back, and buttocks. Subcutaneous therapy includes:
Insulin therapy for diabetics
Opioids for pain relief
Allergy medications like epinephrine
Heparin, a medication used to prevent blood clots
What is the difference between a transfusion and an infusion?
A transfusion occurs when blood or parts of blood are donated from another person and put into a patient's bloodstream. An infusion, on the other hand, involves substances such as medication, anesthetics, vitamins, and vaccines inserted into the bloodstream.
Benefits of Infusion Therapy
The benefits of infusion therapy include:
Fast-acting relief, especially in emergency situations, like after an allergic reaction or during childbirth
Medication for those who cannot take pills orally
Administering larger and/or controlled amounts of medication
Intramuscular and subcutaneous injections help drugs remain in the body longer
High success rates for several conditions
Infusion Therapy Success Rates
Several studies have shown high success rates for infusion therapies. For example:
Epidurals are about 98%–99% successful in relieving pain for people giving birth.
Monoclonal antibody treatments for COVID-19 reduced viral burden—the amount of virus healthcare providers can find in your body—by 90% in trial participants, and emergency room visits and infection time were cut by almost half. However, most of the monoclonal antibodies authorized for treating or preventing COVID-19 have been revoked due to limited effectiveness against newer variants.
Ketamine infusion therapy could be a fast and effective treatment for chronic depression, with about half of patients in one study responding to treatment.
Some cancers respond better to chemotherapy, a type of infusion therapy that kills harmful cells, than others. For example, a recent study found prostate cancer patients were about 10% more likely to survive with chemotherapy than other cancer treatments. However, there are other infusion therapies available to treat cancer that have fewer side effects than chemotherapy. These include hormone therapy and antibodies. It also encompasses vaccines and immunotherapy.
How to Prepare and What to Expect
To prepare for infusion therapy, ask your practitioner about the following:
If you have to avoid any foods or modify your medication schedule before treatment
If others are allowed to come with you to the procedure
If there will be pain and something to relieve that pain
What will be used to treat allergic reactions if they arise
How many sessions are required for treatment
Any side effects you should monitor at home
How many training sessions you and your caregivers will receive for home infusion therapy
How to measure medications accurately for home infusion therapy
Expect the following during infusion therapy:
There will be a comfortable chair to rest in throughout the treatment
The injection site and needles will be disinfected
Anesthesia may be used when larger needles are necessary during treatment
You will be monitored throughout your therapy
The injection site will be covered after your treatment
You and your caregiver(s) will receive adequate training and follow-up appointments for home fusion
How long infusion therapy takes depends on the condition being treated. Chemotherapy for cancer, for example, can take about three to six months. Epidurals, on the other hand, last about one to two hours. Hormone therapy for prostate cancer can last months to years and ketamine infusions can last anywhere from 30 minutes to several hours.
Side Effects of Infusion Therapy
Infusion therapy side effects might include:
Redness at the site of injection
Swelling
Injury at the injection site
Muscle pain
Allergic reactions like rash, difficulty breathing, and confusion
The following are some risks associated with each type of infusion therapy.
IV Therapy Complications
IV therapy complications may include:
Burning, stinging, or redness if IV solution leaks onto skin surrounding the injection site
Pus leaking from injection if infected
Pulmonary edema, or excess lung fluid: This requires quick medical attention and is marked by shortness of breath and coughing up a frothy substance.
Air embolism (when air enters the vein): Symptoms include shortness of breath, increased heart rate, shoulder pain, light-headedness, and confusion.
Epidural Therapy Complications
Epidural therapy complications may include:
Low blood pressure
Headache
Hot flashes
Damaged blood vessel
Damage to injection site nerves
Losing bladder and bowel control
Intramuscular Therapy Complications
Intramuscular therapy complications may include:
Nerve damage
Medication leaking into surrounding tissue
Muscle atrophy, or when a muscle loses strength
Bone injury
Subcutaneous Therapy Complications
Subcutaneous therapy complications may include:
Blister at injection site
Headache
Sore throat
Nausea
Kidney problems
Blood clots
Who Should Not Get Infusion Therapy?
Infusion therapy isn't for everybody, including:
Some children under 12
Some older adults
In some cases, people with high blood pressure or high cholesterol
Those with a history of heart problems
People experiencing heavy bleeding, including during childbirth
Those who've had blood clots in the past
People giving birth who are experiencing low blood pressure
Before undergoing infusion therapy, it's important to share your medical history and any concerns you have with your healthcare provider.
Summary
Infusion therapy involves a medication or nutrient inserted directly into a person's system. Infusion therapy can be intravenous (IV), meaning through an IV needle; an epidural, which is inserted around nerves in the spinal cord; intramuscular, which is inserted in muscle tissue; or subcutaneous, inserted into body fat under the skin.
Read the original article on Verywell Health.

