Lentigo (Liver Spots)
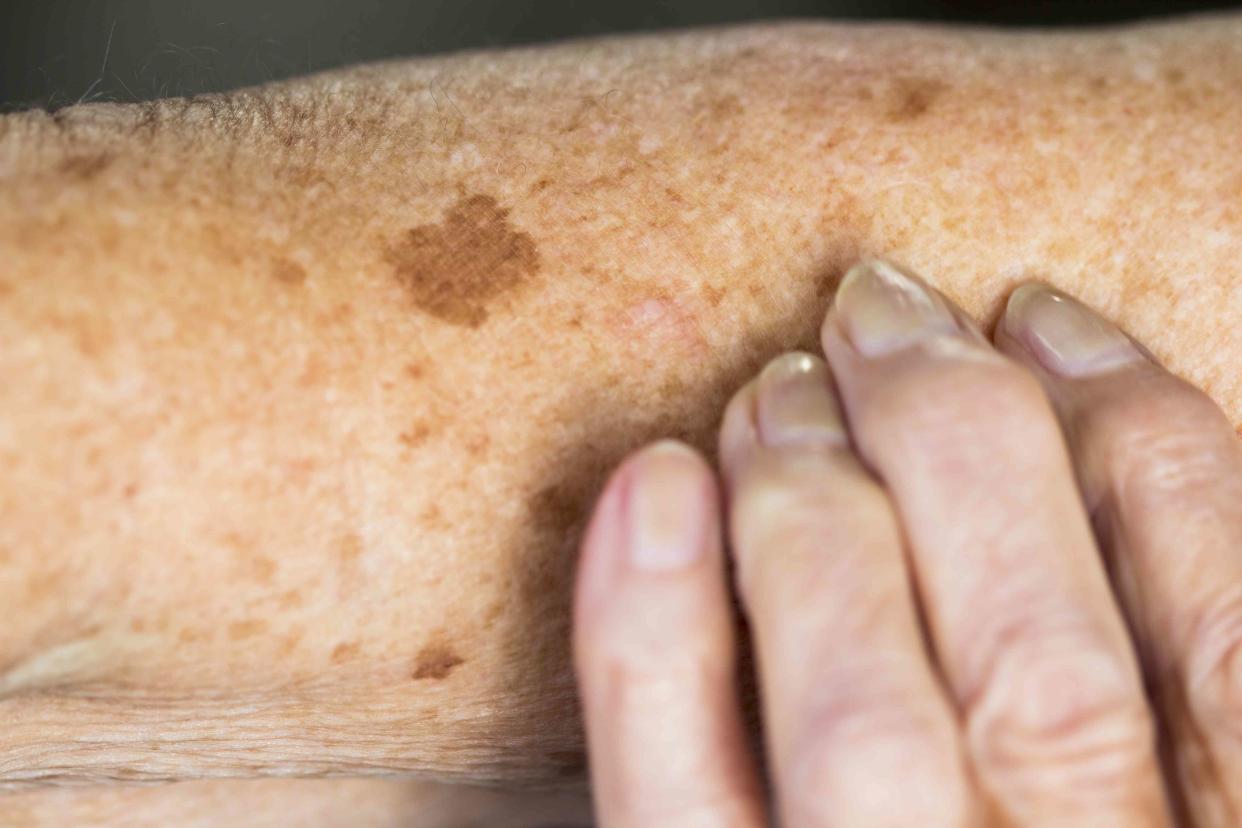
CRISTINA PEDRAZZINI/SCIENCE PHOTO LIBRARY / Getty Images
Medically reviewed by Susan Bard, MD
Lentigo is the term for light brown or dark spots on the skin, which are sometimes also referred to as liver spots. Lentigines refer to more than one spot. These spots can show up slowly over time or suddenly. Solar lentigo and lentigo simplex are harmless. However, lentigo maligna (LM) is a precancerous spot that can lead to melanoma (skin cancer). A few differences in the characteristics of these spots can help you tell the difference between the types.
Always see a dermatologist (a medical doctor who specializes in skin conditions) yearly—or sooner if you are unsure about an area on your skin. They can use specific tools to rule out harmful skin conditions and give you options for over-the-counter (OTC) or prescription treatments when necessary.
Types of Liver Spots
Common types of lentigo include solar lentigo and lentigo simplex.
Lentigo simplex: Also known as simple lentigo, this is the most common type. It's present at birth or during childhood.
Solar lentigo: Also known as age spots, liver spots, and ink spots, this occurs with age and sun exposure.
Lentigo maligna (LM): LM is a separate condition from solar lentigo or lentigo simplex. It is precancerous and can turn into melanoma (a type of skin cancer).
Lentigo Symptoms
Solar lentigines typically occur where you’ve had the most sun exposure, such as on your arms, face, hands, and neck. However, they can also occur in other areas. They may increase in number with age, get darker in the sun, and don’t typically fade in the winter.
Lentigo simplex may be present at birth or occur during childhood. Lentigines can appear anywhere on your body, regardless of sun exposure.
Other lentigo characteristics include:
Clear margins (edges are not blurry, jagged, or notched)
Even color
Flat, oval shape
Painless
May look like inkspots
Stays a fairly consistent size
Tan to dark brown color
It can be challenging to distinguish harmless solar lentigo from lentigo maligna initially. However, if LM progresses to lentigo maligna melanoma (LMM), the spot may:
Have fuzzy borders
Feel raised rather than flat
Invade surrounding structures like hair follicles
Mimic scar tissue
Cause discomfort, itching, or bleeding
What Causes Lentigo?
Solar lentigines form with prolonged exposure to ultraviolet (UV) light from sunlight, tanning beds, medical radiation treatment, or UV therapy. This triggers your body to produce excess melanin (the pigment that gives skin its color), forming dark spots.
Sun exposure does not cause simple lentigo, but the exact cause is unclear. It sometimes occurs with certain genetic conditions.
Risk Factors
Solar lentigo can affect anyone. However, the following factors increase your risk.
Fair skin
Older age
Sunburns
Frequent exposure to sunlight or tanning beds
Psoralen (an oral medication used to treat certain skin conditions) plus ultraviolet A (PUVA) therapy
Diagnosis
To diagnose lentigo, a dermatologist will check the appearance of the spots. They will ask about your medical history, family history, risk factors, and additional symptoms. The provider will aim to differentiate lentigines from other skin conditions, including skin cancer.
The ABCDE Approach
The ABCDE approach helps evaluate skin spots. The following characteristics typically indicate a more serious skin condition, such as skin cancer:
Asymmetry (A): Uneven shape
Border (B): Irregular, jagged, blurry, or poorly defined edges
Color (C): Uneven coloring with multiple shades of brown, black, blue, red, or white
Diameter (D): Typically larger than 6 millimeters (mm)—about the size of a pencil eraser—but can be smaller
Evolution or Elevation (E): May change in size, shape, color, texture, or elevation
Tools and Tests
Providers also commonly use diagnostic tools and tests to distinguish harmless spots from precancerous or cancerous areas. These include:
Dermoscopy: A handheld dermatoscope allows providers to visualize structures within the skin and identify irregularities.
Skin biopsy: The provider sends small skin samples to a laboratory for microscopic examination.
Wood's lamp examination: The provider uses UV light to detect certain skin conditions by highlighting fluorescence patterns.
Reflectance confocal microscopy (RCM): The provider uses a non-invasive imaging tool with laser light to examine skin cells.
Stages of Lentigo Maligna Melanoma
Solar lentigines and lentigo simplex do not have stages. However, you may experience the darkening of existing age spots or the development of new spots.
Lentigo maligna is precancerous in the in situ stage, meaning it's limited to the top layer of skin. If it becomes melanoma, it is in the invasive stage, meaning it spreads into deeper layers of the skin.
Treating Liver Spots
Solar lentigo and lentigo simplex do require medical treatment. However, some people wish to conceal it with makeup or use topical (on the skin) over-the-counter (OTC) or prescription treatments. A dermatologist may also suggest medical procedures like laser therapy.
Some treatments can cause redness, irritation, or peeling. They usually take time and multiple sessions to work.
Over-The-Counter (OTC) Creams
Before trying topical treatments, perform a patch test. Put a small amount of a product on your skin to see if it causes any irritation or allergic reactions. Wait a day or two before using it more widely.
In addition to using sunscreen with SPF 30 or higher to keep spots from getting darker, you can try lightening serums, creams, or gels. OTC skincare products typically contain ingredients such as:
Alpha hydroxy acids: Chemicals that help you shed dark skin cells, like glycolic acid
Retinoids: Vitamin A products like retinol
Vitamin C: For example, tetrahexyldecyl ascorbate
Kojic acid: Fermented rice wine that helps reduce the production of melanin
Lotus sprout extract: Liquid from young lotus plants
Hydroquinone: A bleaching agent
Prescription Medications
A dermatologist may prescribe topical treatments if OTC treatments don't work. Some prescriptions have the same ingredients as OTC treatments but typically involve higher strengths or concentrations. Prescription ingredients usually include:
Hydroquinone
Retinoids
Azelaic acid (a natural compound that reduces melanin production)
Cysteamine (a substance that inhibits melanin production)
Procedures
A licensed esthetician typically performs certain procedures in a dermatology office. The techniques may differ, but each one aims to destroy the excess melanocytes responsible for the dark pigmentation of the spots and promote the growth of new, lighter skin cells. Possible procedures include:
Cryotherapy: Freezing using liquid nitrogen
Intense pulsed light (IPL) therapy: Broad-spectrum light
Laser therapy: Focused beams of light
Chemical peels: Chemical solutions that exfoliate the top layer of skin
Dermabrasion: A rotating instrument with texture that exfoliates
Prevention
Preventing UV damage helps reduce the risk of lentigo and decrease the darkness of current spots. This includes limiting sun exposure during peak hours (10 am-3 pm), wearing protective clothing and sunglasses, regularly applying sunscreen, and avoiding tanning beds.
Related Conditions
Actinic keratosis (rough patches from sun exposure) and seborrheic keratosis (waxy, raised spots with a warty surface) can resemble lentigo. Underlying health conditions, like Addison's disease (when the body doesn't make enough cortisol hormone) and vitamin B12 deficiency, can also lead to lentigo.
Lentigines can appear with rare genetic syndromes. For example, Peutz-Jeghers syndrome (PJS) can cause lentigines on the lips, palms, and soles. Other examples of these rare genetic syndromes include:
Inherited patterned lentiginosis
Carney complex
LEOPARD syndrome
Laugier-Hunziker syndromes
Psoralen plus ultraviolet A (PUVA) therapy, a treatment for skin conditions like eczema (red, itchy, swollen skin patches) or psoriasis (thick, scaly patches), can cause lentigines. Psoralen plus ultraviolet A (PUVA) therapy combines psoralen (a chemical that makes the skin more sensitive to light) and UV light.
Living With Lentigo
Solar lentigo and simple lentigo are harmless and don't need treatment. However, lentigo maligna (LM) can progress to lentigo maligna melanoma (LMM). If you're unsure about a spot, consult a healthcare provider to confirm if it's lentigo and not another skin condition.
You can prevent lentigo by protecting your skin from UV exposure. You can also consider OTC creams, prescription topical treatments, and cosmetic procedures like laser therapy or chemical peels.
Frequently Asked Questions
Can lentigo turn into melanoma?
Solar lentigo and simple lentigo do not directly become cancerous. However, melanoma can develop in the same skin areas, giving the impression that lentigo has become melanoma.
Lentigo maligna (LM) is a separate precancerous condition that may resemble solar lentigo. It can progress to lentigo maligna melanoma (LMM). It’s important to report changes in lentigo spots to a healthcare provider so they can rule out lentigo maligna.
Is a lentigo cancerous?
Solar and simple lentigines are noncancerous. However, lentigo maligna, a slow-growing precancerous condition, can lead to melanoma (a type of skin cancer).
In the early stages of lentigo maligna, it can be difficult to distinguish other types of lentigo, so it's important to consult a dermatology provider if you notice new spots or changes in existing ones.
How fast does lentigo grow?
Solar or simple lentigo spots don’t grow much. Lentigo maligna, a precancerous condition that can resemble these types of lentigo in the early stage, grows slowly. It can take anywhere from 10 years to over 50 years for lentigo maligna to turn into lentigo maligna melanoma, a type of skin cancer.
For more Health.com news, make sure to sign up for our newsletter!
Read the original article on Health.com.

