What to Know About Shingles
Shingles is a painful, blistering rash caused by the reactivation of the varicella-zoster virus, the same virus that causes chickenpox.
Although shingles is incurable, antiviral medications may speed healing and reduce pain. In addition, a vaccine can help protect against shingles and postherpetic neuralgia, a common complication of shingles.
This article will review essential facts about shingles, including its symptoms, risk factors, and treatment. Insight into whether shingles can recur or is contagious will also be provided.
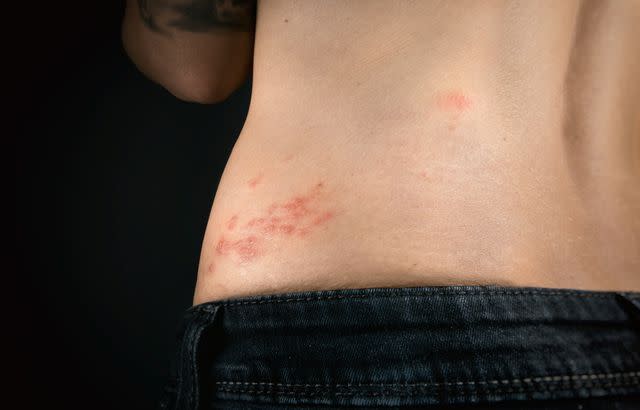
Petra Richli / Getty Images
Symptoms and Stages of Shingles
Shingles affects around 1 in 3 people in the United States during their lifetime, and the risk of developing this skin condition is highest in older adults.
The symptoms of shingles progress through two stages. The first is the preeruptive stage, the period before the rash appears.
Preeruptive Stage
At least two days before the shingles rash appears, a person may experience unusual sensations on one side of the body or face, often described as burning, tingly, or itchy.
Flu-like symptoms may occur during this stage and can include the following:
Fever and chills
Unusual tiredness
Body aches
Light sensitivity (photophobia)
Upset stomach
Acute Eruptive Stage
During this stage, painful blisters develop on one side of the face or body. The most common sites of rash are the chest, abdomen, and back, although shingles can occur anywhere.
A telltale sign of the shingles rash is that it appears as a band, belt, or stripe on the skin. This is because the blisters develop along a dermatome, an area of skin supplied by a single nerve starting at the spine.
Within a few days of the rash becoming visible, the blisters burst and form ulcers (open sores) before scabbing over in seven to 10 days.
The rash fully clears within two to four weeks for most people. For some, scarring and skin color changes may occur.
Learn More:What Shingles Looks Like
Uncommonly, shingles may present in the following way:
Disseminated zoster is when three or more dermatomes are affected, causing the shingles rash to be more widespread, resembling chickenpox.
Internal shingles, also known as zoster sine herpete (ZSH), is the reactivation of the varicella virus without the characteristic rash.
Complications of Shingles
Complications of shingles are more likely to develop in older adults and people with weakened immune systems.
Postherpetic neuralgia is the most common complication of shingles that develops in approximately 20% of people. Postherpetic neuralgia is a term used to describe abnormal burning or shock-like sensations that persists for 90 or more days after the rash appears.
Other complications of shingles include:
Bacterial skin infection, sometimes caused by scratching the blisters.
Vision loss if blisters develop near the eye (herpes zoster ophthalmicus).
Ramsay Hunt syndrome, which is associated with weakness on one side of the face, intense ear pain, and blisters in the ear canal or mouth.
Rarely, disseminated zoster can lead to internal organ problems, like pneumonia (lung infection), encephalitis (inflammation of the brain), and hepatitis (inflammation of the liver).
Learn More:Risks Associated With Shingles
Causes and Risk Factors of Shingles
After a person has chickenpox, the virus remains dormant in their nerve cells. Years, even decades, later, the virus may reactivate or reemerge in a single nerve root, leading to shingles in the area of skin connected to the nerve.
Several factors may increase a person's risk of developing shingles. They all generally share a common trait of weakening, or compromising, the immune system, which makes a person more prone to chickenpox virus reactivation.
Shingles risk factors include:
Increasing age: The risk of shingles rises sharply after age 50.
Diseases that weaken or alter the normal functioning of the immune system: Examples include cancer (especially leukemia and lymphoma), diabetes, human immunodeficiency virus (HIV), and autoimmune diseases like lupus or rheumatoid arthritis.
An immune-suppressing medication: Examples include chemotherapy, prednisone, and organ transplant drugs.
Stress, including emotional distress or physical trauma, or a family history of shingles, may also make a person more vulnerable to developing shingles. However, the scientific evidence supporting these factors remains under medical debate.
Learn More:What Causes Shingles?
How Chickenpox Impacts Immunity
When you have chickenpox, T-cells (immune system cells that play a critical role in fighting infection) leave the bloodstream and enter the infected skin tissue.
These T-cells remain in the skin after the chickenpox virus has been cleared. Their goal is to keep the chickenpox virus in check, preventing reactivation into shingles.
Chickenpox virus reactivation becomes more likely when T-cells are depleted or impaired. Advanced age and health-related factors (e.g., taking drugs that suppress the immune system) can trigger this depletion or decline in T-cell function.
Reinfection Risk
While not common, a person can get shingles multiple times. The recurrence of shingles is estimated to be nearly 4% in people with shingles age 45 or older. Like other shingles complications, recurrent shingles is more common in those with a suppressed immune system.
How Contagious Is Shingles?
Shingles is not contagious, so you cannot get shingles from another person.
However, you can get chickenpox from a person with shingles. This can only happen if you have never had chickenpox or received the chickenpox vaccine. Anyone who has had chickenpox can get shingles later in life.
Keep in mind that in the above scenario, to get chickenpox from a person with shingles, there must be skin-to-skin contact with the fluid from one or more shingles blisters. The virus cannot be spread before the blisters appear or after the blisters crust and scab over.
Learn More:How Shingles Can Spread
Diagnosing Shingles
Shingles is diagnosed by a healthcare provider such as a primary care physician or nurse practitioner or a specialist such as a dermatologist (a doctor specializing in skin conditions). They can usually diagnose the shingles rash based on its appearance since the location of a shingles rash is nearly always restricted to a single dermatome.
A polymerase chain reaction test (PCR) may be performed in the following circumstances:
The presentation is atypical (e.g., the rash is widespread or absent).
You have a weakened immune system.
You have received the recommended vaccination for shingles.
For PCR analysis, a healthcare provider uses a sterile swab to obtain fluid from the blister or a crust/scab sample.
If a rash is absent, but you have shingles-like pain, your healthcare provider may obtain a saliva or blood sample for PCR testing, although these fluid samples may lead to false negative results.
PCR testing can also help rule out alternative diagnoses conditions like herpes simplex virus (HSV), contact dermatitis, or dermatitis herpetiformis.
How to Treat Shingles
The standard treatment of shingles involves taking both an antiviral and pain-relieving medication.
Antiviral Medication
Antiviral medication aims to hasten the rash's healing, decrease the severity and duration of shingles-related pain, and minimize a person's chances of developing complications. Antiviral therapy should ideally start within 72 hours after the rash appears for optimal benefit.
Three antiviral medications used to treat shingles are:
Zovirax (acyclovir)
Shingles can occur during pregnancy, albeit rarely, and typically causes no harm to the fetus. Shingles in pregnancy is usually treated with acyclovir.
Pain Medication
The pain of shingles can be excruciating and debilitating, so medication for pain is often needed. The choice of pain-relieving medication depends on factors like the severity of the pain and your overall health and medical history.
Oral pain medication options include over-the-counter drugs like Tylenol (acetaminophen) or a nonsteroidal anti-inflammatory drug (NSAID) like Advil or Motrin (ibuprofen).
If the pain is severe, an opioid like OxyContin (oxycodone) may be prescribed temporarily.
Other Medications
Other medications that may be prescribed for shingles include the following:
A corticosteroid like prednisone for Ramsay Hunt syndrome or if shingles affects the eye
Antibiotics if the rash becomes infected with bacteria
A tricyclic antidepressant like Elavil (amitriptyline) or an antiseizure drug like Neurontin (gabapentin) for postherpetic neuralgia.
Home Remedies
In addition to medication, various at-home strategies can minimize the discomfort of shingles and maximize healing potential.
For example, applying a cool washcloth to the affected skin can ease pain and itching. Likewise, calamine lotion or colloidal oatmeal baths—warm baths mixed with oatmeal ground into a fine powder—can relieve skin itching and irritation.
After bathing or applying a cool washcloth, be sure to gently dry the affected skin area. Also, try not to disturb or scratch the blisters, which can lead to an infection.
Preventing Shingles
Receiving the shingles vaccine called Shingrix is crucial for preventing shingles and the most common complication, postherpetic neuralgia.
The Centers for Disease Control and Prevention (CDC) recommends that adults 50 and older get two doses of Shingrix. Individuals 19 and older with weakened immune systems should also get two doses of Shingrix.
Keep in mind that you can still get the vaccine even if you had shingles or received Zostavax or the chickenpox vaccine. Zostavax is a shingles vaccine no longer available for use in the United States.
However, you should not get the shingles vaccine if:
You currently have shingles.
You are pregnant.
You have had a severe allergic reaction after a dose of Shingrix or to one of the ingredients in the vaccine.
When getting Shingrix—a shot in your upper arm—you may experience side effects for two or three days. These side effects can include soreness, redness, or swelling at the injection site, tiredness, muscle aches, upset stomach, fever, and headache.
Related:Should You Get the Shingles Vaccine?
Outlook
Shingles is intensely painful, but the good news is that the rash usually clears within a few weeks and rarely recurs.
Nevertheless, if you are experiencing symptoms of shingles, it's essential to seek medical attention as soon as possible. Prompt antiviral therapy can reduce the severity and duration of your symptoms and lower your chances of developing complications.
Also, if you have already been diagnosed with shingles, don't hesitate to contact your healthcare provider if your pain is not controlled well. Several medication options can help you get through this uncomfortable time.
Moreover, seek medical care if you suspect a shingles complication, like an infection, signaled by redness, swelling, or increased tenderness around the rash.
Read Next:Coping With Shingles

