What to Know About Inflammatory Polyarthritis
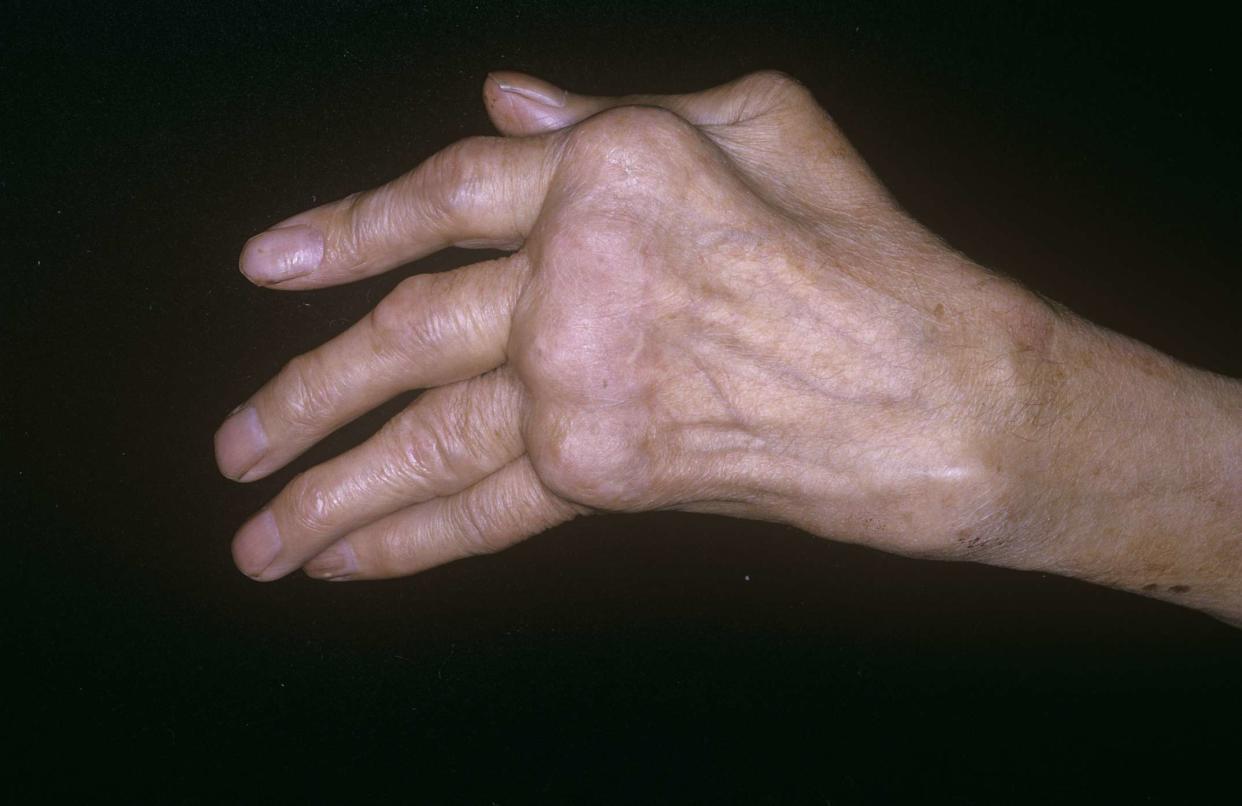
Mike Devlin / Science Photo Library / Getty Images
Medically reviewed by Anita C. Chandrasekaran, MD, MPH
Polyarthritis means that five or more joints in your body are affected by arthritis and inflammation. It's most often associated with autoimmune diseases such as rheumatoid arthritis (RA), but some viral infections can also trigger it.
If you're not already diagnosed with a condition that can lead to polyarthritis, your healthcare provider may use blood tests, imaging, and a physical exam to diagnose the underlying cause.
This article explains polyarthritis symptoms, causes, diagnosis, and treatment.
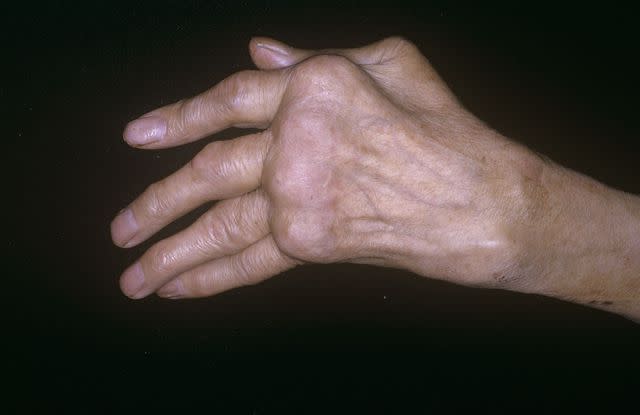
Mike Devlin / Science Photo Library / Getty Images
Other Names for Polyarthritis
Polyarticular arthritis
Inflammatory polyarthritis
Symptoms
Polyarthritis symptoms are similar to those of rheumatoid arthritis and other autoimmune diseases that affect the joints. They can come on suddenly or over many months.
A key sign of polyarthritis is inflammation. Signs of joint inflammation include:
Swelling
Warmth
Pain
Decreased range of motion
Morning stiffness and pain that gets with activity and worse with rest are classic symptoms of inflammatory arthritis.
Types of Inflammatory Arthritis
There are different kinds of inflammatory arthritis depending on which joints are affected and how many joints are affected. In oligoarthritis, four or fewer joints are affected. If five or more joints are affected, it’s called polyarthritis.
Autoimmune diseases can trigger an all-body response because they're systemic diseases that can cause various symptoms. Joint involvement generally does not appear on its own as it can with “wear and tear” arthritis that comes with aging (osteoarthritis).
Autoimmune causes of arthritis tend to have other symptoms including:
Lack of appetite
Rash
Sweating
Swollen lymph nodes
A temperature of 100.4 degrees or above
Tiredness or a lack of energy
Unexpected weight loss
In rare cases, the inflammatory disease that causes polyarthritis can also cause scarring in the lungs, dry eyes, skin rash, and inflammation in the sac surrounding the heart (pericarditis).
Joint Pain Without Inflammation
Having joint pain in multiple joints without inflammation is called polyarthralgia. This is common in people who get osteoarthritis as they get older.
Causes
Polyarthritis can be caused by an autoimmune disorder or an acute illness. It happens when inflammation affects joints in the body. The symptoms can be constant or may flare up when the underlying inflammatory condition flares up.
While there are some lifestyle strategies that can help keep your joints healthy as you age, you can’t always prevent a cause of inflammatory arthritis since conditions like autoimmune diseases are often linked to your genes.
Autoimmune Disorders
Polyarthritis is most often caused by autoimmune disorders. In these disorders, the immune system mistakenly attacks its cells and tissues. The causes of autoimmune diseases are not well understood but genetics and the environment are thought to play a major role.
The autoimmune disorders most commonly associated with polyarthritis include:
Sarcoidosis
Sjogren's syndrome
Learn More: What Is Inflammatory Arthritis?
Illness
Polyarthritis can also occur as part of an acute illness. In these cases, the inflammation may move between more than one joint.
Illnesses linked to polyarthritis include:
Alphaviral infections (including the Ross River virus, chikungunya virus, and Mayaro virus)
Dengue
Zika virus
Hepatitis
Epstein-Barr virus (EBV)
Cytomegalovirus (CMV)
Diagnosis
Polyarthritis is most commonly related to an underlying disease. Your healthcare provider will ask you if you have other signs and symptoms along with inflamed joints like tenderness, joint effusion (known as “water on the knee”), and swelling, which are common signs of autoimmune diseases.
Symmetry vs. Asymmetry
Your provider will ask whether your pain is symmetric or on both sides (for example, in both hands or knees) or asymmetric, meaning it’s just on one side (one hand).
People with RA tend to have symmetric symptoms. Those with psoriatic arthritis often have asymmetric symptoms.
Blood Tests
Bloodwork can help your provider narrow down a diagnosis. Tests to screen for RA commonly include:
Anti-cyclic citrullinated peptide (anti-CCP) antibody test
In addition, your healthcare provider may check your blood for:
Anemia
Elevated white blood cell count
Elevated platelets
Increased inflammatory markers, known as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP)
Other tests can help your provider look for antibodies related to specific autoimmune diseases (serology). Your provider can also test you for viruses if they think your symptoms could be related to an infection.
Imaging Tests
Depending on the possible cause, X-rays, a musculoskeletal ultrasound, magnetic resonance imaging (MRI), and a joint fluid analysis (arthrocentesis) can help your provider make a diagnosis.
Treatment
The treatments for polyarthritis are typically the same as for the autoimmune diseases that can bring it about.
Your provider might recommend medications for pain and inflammation, drugs that can slow or stop the progression of the disease, and at-home therapies to help you manage your symptoms.
Medication
There are many medications that can help with symptoms of polyarthritis, depending on what the cause is.
Over-the-Counter
Non-steroidal anti-inflammatory drugs (NSAIDs) like Advil (ibuprofen), Aleve (naproxen), and Voltaren (diclofenac) can help relieve pain and stiffness. These are available over-the-counter (OTC) with a prescription. Your provider might also prescribe a higher dose if you need it.
OTC options can be used for polyarthritis from a viral illness because while they won't help with the infection, they can help with your symptoms until you're better.
Prescription
If you need more treatment than OTC medications, your provider might recommend some prescription medications.
One example of a prescription treatment your provider might want you to try for polyarthritis is disease-modifying anti-rheumatic drugs (DMARDs). These medications help slow the course of autoimmune diseases. For example, providers may prescribe methotrexate to reduce joint damage caused by polyarthritis.
Biologics, including Remicade (infliximab) and Enbrel (etanercept), are other treatments your provider might recommend. They change the immune system to reduce inflammation.
Corticosteroids control inflammation and can help with pain. You can take steroids orally or by injection. However, they should only be used in the short term because they can cause serious side effects.
At-Home Therapies
Warming therapies you can do at home can temporarily relieve symptoms of polyarthritis. Examples include:
Warm baths
Warming mitts
OTC topical creams with a warming effect (e.g., Aspercreme)
Do not underestimate the value of exercise in managing polyarthritis symptoms. Low-impact activities like swimming, yoga, and stretching can help keep your joints healthy.
Summary
Polyarthritis is arthritis that affects five or more joints. Joint pain and inflammation are the most common symptoms, but you can also have rash, fever, and fatigue depending on the underlying cause.
Polyarthritis is most commonly caused by an autoimmune disorder but can also be triggered by an acute infection. The treatment involves medication, at-home strategies to manage your symptoms, and exercise to keep your joints flexible.
You need to see your provider for a proper diagnosis and treatment for polyarthritis. The sooner the better, as you want to prevent the condition from getting worse and causing permanent joint damage.
Frequently Asked Questions
How is polyarthritis treated?
Polyarthritis is treated similarly to arthritis and other autoimmune diseases. Potential treatments include disease-modifying anti-rheumatic drugs (DMARDs), non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids, surgery, medications, massage, and covered heat packs.
What is migratory polyarthritis?
Migratory polyarthritis refers to the gradual spread of arthritis to different joints. Arthritis will begin in one or two joints and appear to improve after several days, only to return and affect a different set of joints. It is considered acute polyarthritis when symptoms last fewer than six weeks and chronic if symptoms last longer.

