What You Need to Know About Allergy Testing
Getty Images
Whether you suffer from watery eyes and unstoppable sneezes every spring or develop an upset stomach after wolfing down a few slices of bread, you probably want some clarity on the exact cause of these reactions. Even more so, you'll likely want to know how to avoid those unpleasant symptoms in the first place. And luckily, allergy testing can help you do just that.
But what does allergy testing look like, exactly? And how do you about getting tested? Here, Purvi Parikh, M.D., an adult and pediatric allergist and immunologist with Allergy & Asthma Network, breaks down the entire allergy testing process, including the different types of tests available and reactions you may develop. Plus, she explains how to make sense of your results if you do have an allergy.
Why Pursue Allergy Testing?
To understand why allergy testing is so important, you'll first need some background on allergies overall. ICYDK, allergies occur when you're exposed to a typically harmless, foreign substance (think: pollen, dust mites, animal dander, a particular food) and your immune system mistakenly identifies it as a threat. In response, your body releases certain chemicals known as histamines that can cause sneezing, runny nose, congestion, or red, watery, or itchy eyes, according to the Centers for Disease Control and Prevention. You may also develop a cough, a scratchy throat, hives, rashes, and, in severe cases, breathing trouble, asthma attacks, anaphylaxis (a serious reaction in which your blood pressure drops suddenly and your airways narrow), and even death, according to the Asthma and Allergy Foundation of America.
Because of those uncomfortable and potentially life-threatening physiological responses to allergens, Dr. Parikh generally recommends anyone who's experienced any type of allergic reaction receive an allergy test from a board-certified allergist. Similarly, individuals who suffer from asthma or eczema should get an allergy test, as the conditions are often triggered by allergens, she explains. In doing so, your doctor will be able to pinpoint the exact culprits causing your symptoms and guide you on how to avoid them, says Dr. Parikh.
More importantly, allergy testing can help determine if the symptoms you're experiencing after eating a particular food are because of a legit allergy or just an intolerance or sensitivity, she says. Reminder: A food allergy is an immune system reaction that can affect various organs and cause harmful side effects, such as itchy or swelling in the mouth, vomiting, diarrhea, or abdominal pain, hives, difficulty breathing, or anaphylaxis, according to the U.S. National Library of Medicine. A food sensitivity, however, is when your body can't properly digest a certain food or the food simply bothers your digestive system, causing abdominal pain, nausea, gas, and diarrhea, according to the NLM. "[A food intolerance] is not something that's necessarily dangerous whereas an allergy can be," says Dr. Parikh. "So it's important to know if you're allergic or not because an allergy involves your immune system, and [in turn,] the treatment and the avoidant strategies are very different."
That said, Dr. Parikh cautions against getting an allergy test willy-nilly. "I would only get one if you have symptoms," she says. "If you have no symptoms of any type of food or environmental allergy, I would not get an allergy test because it's kind of a waste of your time. There's no good evidence behind mass testing for no reason." (Wait, is your wintertime cold actually allergies?)
Common Types of Allergy Testing
If you're no stranger to pollen-induced sniffles or sneezing non-stop around your neighbor's cat, book an appointment with a board-certified allergist for a test, says Dr. Parikh. There, your doctor will take a detailed account of your reaction(s), the substances you came in contact with, and your medical history to determine the best type of allergy test for you, such as the commonly used blood, skin, or patch tests, she explains. This consultation is particularly important when your reaction happened out of the blue, and you're not quite sure what allergen may have been the cause. "It's not a good idea to necessarily test for everything — it's better to do guided testing," adds Dr. Parikh. "That's why the allergist is very important." (Related: The Most Common Allergy Symptoms to Look Out for, Broken Down By Season)
Most insurance plans will cover the cost of allergy tests, which can run anywhere from $200 to $1,000, according to the Cleveland Clinic. Still, you'll want to check with your insurance provider ahead of your appointment to find out what you're responsible for paying depending on your coverage.
Blood Test
Of the most common types of allergy testing, the blood test is the most straightforward. A doctor will draw blood from your arm and send it off to a lab, where the number of Immunoglobulin E (IgE) antibodies — the allergy antibody — for specific allergens is measured, says Dr. Parikh. (Refresher: Antibodies are proteins made by the immune system that "attack" the allergen.) If your doctor suspects, for example, a peanut allergy, they might measure the IgE levels for peanuts, she says. Everyone naturally has small amounts of IgE antibodies in their blood, but if you have an allergy, you might have more of these antibodies, according to an article published by the Institute for Quality and Efficiency in Health Care.
An allergist might call for an allergy blood test if you've taken an antihistamine in the last 48 hours to 72 hours. The drug will suppress any reactions and provide inaccurate results during a skin test (more on that in a sec), but it won't affect the results of a blood test, says Dr. Parikh. The same recommendation is often given to folks who run the risk of severe allergic reactions, according to the Institute's article, or who have super sensitive skin that reacts to any substance, leading to faulty results on skin tests, she explains. The downside: It'll take a few days to get the results of a blood test, she adds. (Related: Is It Really Okay to Take Benadryl for Sleep?)
Skin Test
If your allergist wants to understand and diagnose your allergy fairly quickly (such as in cases of food allergies, which can often be life-threatening) or you suffer from bad eczema (which causes high total levels of IgE antibodies and may lead to false-positive blood tests), they might turn to the skin test, says Dr. Parikh.
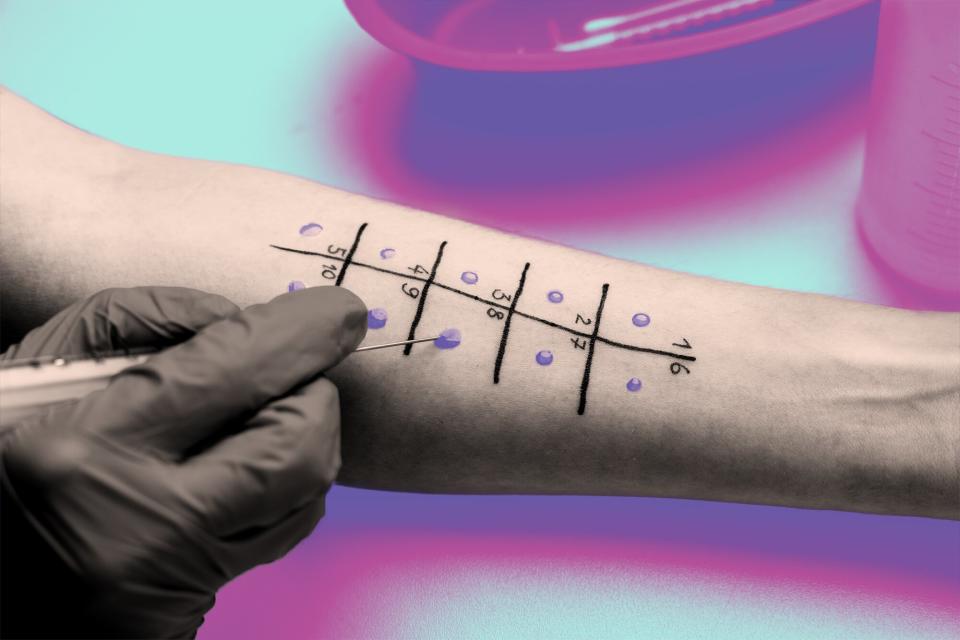
First, the doctor will clean the testing area — typically the forearm for adults and the back for children — with alcohol and draw small marks on the skin. Then, they'll gently prick the surface of the skin in the marked area, inserting a tiny amount of a potential allergen, according to the Mayo Clinic. All skin contains mast cells, which are cells that cause an immediate allergic reaction. So if you're allergic to one of the tested substances, you'll quickly develop a small, mosquito bite-looking bump or an itchy hive in that spot, providing results in just 15 minutes, explains Dr. Parikh. The bigger the bump, the more sensitive you might be to the allergen, according to the American College of Allergy, Asthma & Immunology.
That redness and itching are typically as severe of a reaction as you'll get (seriously, you won't even bleed), and it will likely fade within an hour, says Dr. Parikh. "We usually will put anti-itch cream or spray on it to make them more comfortable," she adds. "But let's say you're very allergic and it's still bothering you after you leave, then you can take an antihistamine to help with the symptoms." Forty-eight to 72 hours ahead of the allergy skin test, though, you'll need to avoid taking any antihistamines, as the drug will suppress those reactions that help the doctor determine if you're allergic or not, she says.
Depending on your medical history and age, your doctor might test anywhere from 20 to 70 allergens in one sitting, she says. "They won't do more than that because it's then just kind of uncomfortable for the patient," explains Dr. Parikh, who adds that docs will do test even fewer allergens for children. "We streamline what's really necessary because you don't want to torture the poor kid."
If a standard skin test is inconclusive (read: you didn't have a strong enough reaction to determine a result), your doctor might recommend an intradermal skin test. During this form of allergy testing, your provider will inject a small amount of the potential allergen just below the skin's surface, according to the Cleveland Clinic. As with the regular skin tests, your doctor will watch for a raised, red, itchy bump at the injection site — signs you may be allergic — for about 15 minutes, according to the American College of Allergy, Asthma & Immunology.
Still, there are some instances in which a blood test is a better option, and, again, your doctor will take a thorough account of your prior allergic reactions and medical history to determine when that's needed. "For some very severely allergic people [think: those at risk of anaphylaxis], we might decide not to do a skin test and we'll [do a] blood test instead because very rarely, you'll get a severe allergic reaction to the skin test," says Dr. Parikh. "It is very, very rare, but it can occur. That's why you want to do it under the supervision of a board-certified allergist who can determine who's safe to get tested and who isn't. But for over 90 percent of people, there are no issues." (See also: Yes, You Can Be Allergic to Semen)
Patch Test
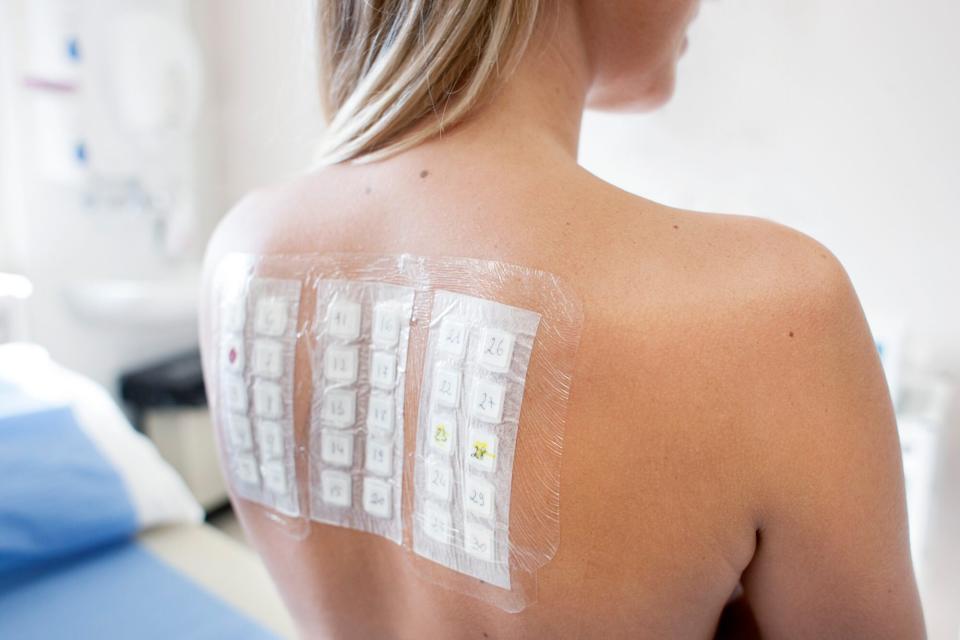
If your doctor suspects an allergy to certain chemicals (such as preservatives and fragrance), metals (such as those in jewelry), or latex — which typically only show symptoms a few days after contact — they might recommend a patch test. For this test, your doctor will place a patch containing the potential allergens on a flat spot of your back, which you'll leave there for 48 hours, says Dr. Parikh. (Hold on, can you be allergic to hair dye?)
During that period, you'll have to keep the patch dry, so exercising until you're sweaty or taking showers and baths isn't recommended. Unlike with the skin test, you can continue taking antihistamines while wearing the patch, but you'll need to avoid steroids, which can interfere with the test results, says Dr. Parikh. Once those 48 hours are complete, your allergist will remove the patch and look for allergy symptoms such as a rash, blistering, redness, or swelling in the area, she explains. (These celebs wouldn't have a problem going shower-free.)
Science Photo Library/Getty
What Happens After Allergy Testing?
When an allergy test confirms you do in fact have an allergy, your doctor will advise you on the best treatment plan depending on the type of allergen. To temporarily soothe your sniffles and relieve other symptoms, you might consider trying over-the-counter, 24-hour antihistamine tablets such as Zyrtec, Allegra, or Claritin, Dr. Parikh previously told Shape.
But if you want to take steps to permanently alleviate symptoms, you've got options. "For the environmental allergens [such as pollen, animal dander, or mold], you can even actually make your allergies less severe over time by doing allergy shots or immunotherapy," says Dr. Parikh. "What that does is over time, it actually desensitizes you to the allergen so that you no longer react as strongly." For six months, your allergist will inject you with tiny, diluted doses of your allergen weekly, gradually increasing the amount, to help your body develop a tolerance to the allergen, she says. After that, you'll get your shot once monthly for three to five years, she explains. (In the meantime, these home remedies may ease your sniffles.)
For food allergies, the primary course of action is to avoid contact with the food entirely and, particularly if you're at risk of anaphylactic shock, carry an EpiPen or other type of emergency epinephrine device. These devices deliver a dose of epinephrine, a medicine that slows down the allergic reaction and stops the airway from swelling. In some cases, immunotherapy (treatment that desensitizes the immune system to an allergen) may be an option. "They're now starting to study desensitization for foods, but so far the only FDA-approved one is for peanuts called Palforzia," says Dr. Parikh. The treatment, a powder that's mixed into food, can be started only in 4- to 17-year-old children with a confirmed diagnosis of peanut allergy, and they still need to avoid peanuts in their diets, according to the U.S. Food and Drug Administration.
Even if you do test positive for an allergy, you might not automatically have to start treating or avoiding the cause altogether. If you've never developed any allergy symptoms after coming in contact with ragweed pollen, for example, but a skin test shows you have a mild allergy to it, you wouldn't necessarily start immunotherapy ASAP. "There has to be some type of clinical symptom or history or reaction to accompany it [to start treatment]," says Dr. Parikh.
What About At-Home Allergy Tests?
As tempting as it may be to skip all the time-consuming allergist appointments and use an at-home allergy test instead, Dr. Parikh strongly discourages doing so. "I would not do home allergy tests because they're not very legit, and you don't know how to interpret them," she says. "They could be misinterpreted and you might label yourself with an allergy that you don't have or miss an actual allergy that you do have." (One at-home test you can do? This one for stress.)
Instead, Dr. Parikh recommends receiving allergy testing only under the care of a board-certified allergist, who has a valid medical license, completed two years of a fellowship in an allergy/immunology program, and attended a training program, among other requirements. To find a doc who fits the bill, search the American Academy of Allergy, Asthma & Immunology's directory for an allergist in your area, then confirm they're board-certified on CertificationMatters.org. With all those mandates, you can be sure your doctor will be able to properly interpret your allergy testing results and determine a game plan if you do have an allergy, says Dr. Parikh. "There's a reason why that training occurs."

