Inside the Knockdown, Drag-Out War on Saturated Fat

ALBI SKENDERI IS sitting on a leather love seat in his studio apartment in Manhattan’s Meatpacking District. A road bike leans on a wall and a punching bag hangs in a corner.
Beneath it are a yoga mat, a medicine ball, and a few dumbbells. He’s wearing a Henley shirt that accentuates his build: six feet and 180 hard, veiny pounds.
The Meatpacking District is an aptly named neighborhood for Skenderi to live in. “I switched to a carnivore diet a couple months ago,” says Skenderi, who is 33 and works in finance. “One of my coworkers was heating up steak in the microwave at eight in the morning, smelling up the entire office. And I was like, ‘Dude, what are you doing?’”
His colleague had discovered the diet from listening to an episode of The Joe Rogan Experience podcast and replied, “Meat is all I’ve been eating for the last couple weeks. I have so much energy and my body is fantastic right now.”
Until then, Skenderi had been eating all vegetables all the time. “I’d become plant-based after watching The Game Changers,” he says, referring to the movie that catalogs the alleged perils of animal foods. “And I felt good on plants. But this guy made me wonder . . . Am I doing this all wrong? I went down a rabbit hole. I listened to a podcast and read The Carnivore Code. So I went to Whole Foods and bought a bunch of steak.”

Even crazier and more confusing than Skenderi’s dietary 180 is the fact that scientists can’t yet tell us for sure which approach to eating is healthier. At the heart of the debate is a nutrient most commonly associated with animal proteins—saturated fat—and whether or not eating too much of it will kill you.
The fact that podcasts, books, and movies can draw on research about meat and saturated fat—and if you should consume it—and come to opposite conclusions shouldn’t be surprising.
Nutritional science is less certain than you might imagine, and warring, possibly compromised camps are exploiting that squishiness to promote polar-opposite agendas. And not just in pop culture.
This war is taking place in our nation’s capital and in the halls of our most venerated academic institutions. It involves allegations of biased research funding from Big Beef and Nut Boards, a contrarian investigative journalist, and an esteemed Ivy League researcher railing against “the disinformation triangle.”
It has professors and deans at Harvard and Yale slinging mud. It includes accusations of data misrepresentation, fear mongering, political hardball, and all-around general bullshitting.
The war has grown more intense with the anticipated release of the federal government’s 2020-25 dietary guidelines, sending both sides into a blitzkrieg assault to either keep or kill the long-standing saturated-fat recommendations.
And the fallout from this war is hitting average Americans, driving more of us to search for dietary salvation at the poles. Veganism rose nearly 1,000 percent in the U.S. between 2010 and 2019. According to Nielsen, nearly 40 percent of Americans say they’re making an effort to eat more “plant-based” products.
Yet meat and dairy consumption has also ticked upward; there’s now a bevy of mail-order meat-subscription companies, and carnivore diet books are best sellers.
When those new guidelines do drop, most of us might be left to wonder: Who can we trust in this billion-dollar food fight? And what does all this mean for our health?
The Case for Caution
TO UNDERSTAND the history of governmental nutrition guidelines in the U.S., you have to know nutrition research at Harvard University. To do that, you have to know Walter Willett, M.D., Dr.P.H.
Dr. Willett, 75, is slim but sturdy, with a head of silver hair and a wispy white mustache. He graduated from the University of Michigan Medical School when Nixon was in office.
“When I was practicing medicine, I became frustrated because my patients had conditions like diabetes, hypertension, and heart disease that I couldn’t cure,” says Dr. Willett. “I wanted to understand what was causing the conditions to prevent them in the first place.”

Until the 1940s, most Americans didn’t really worry about whether food would blow up their waistlines or clog their arteries, says Adrienne Bitar, Ph.D., a food historian at Cornell University and the author of Diet and the Disease of Civilization. Food was considered medicine in the sense that eating a healthy diet moved you further away from malnutrition and disease.
Then, in the 1950s, Ancel Keys, Ph.D., a physiologist at the University of Minnesota, noticed a paradox. Rich guys in America were well-fed, but they suffered from a high rate of heart disease. Middle-aged men in the U.S. had a four- to ten-times-greater risk of the disease compared with men in postwar Europe, Japan, and other countries.
Keys believed diet, specifically a diet that included lots of saturated fat, was to blame. Fat made up 40 percent of the calories in the average American diet but just 20 percent in the Italian one.
Keys figured that if people ate less fat, they’d reduce their blood cholesterol and, therefore, their risk of heart disease. And, he’d find, foods higher in saturated fats seemed to raise blood cholesterol.

“Then in 1955, President Eisenhower had a heart attack,” says Bitar. “That’s when public attention cohered around the idea that heart disease was an epidemic. Eisenhower went on a low-fat diet.” Not long after, the federal government started raising concerns about fat in the diet.
In 1980, Dr. Willett earned his doctorate from the Harvard School of Public Health and joined the epidemiology department as a professor. He developed rigorous diet questionnaires, which researchers distributed to nearly 122,000 nurses, looking for links between eating habits and health.
“We set the study up to look at the type of fat because of the concern at that time,” he says of the landmark Nurses’ Health Study.
Dr. Willett’s work has consistently shown that, for heart disease, saturated fats aren’t necessarily bad. But they also aren’t good. “It’s really about comparison,” he says. “If you compare saturated fat to trans fats, then saturated fat looks good.”
For every 2 percent of your calories that come from trans fats (the FDA banned artificial trans fats in 2015, in part due to Dr. Willett’s work), for example, your coronary-heart-disease risk rises by 23 percent, according to a review in The New England Journal of Medicine. “But if you compare it to unsaturated fats, then saturated fat looks bad,” says Dr. Willett.
But Dr. Willett, despite his academic stature and decades of expertise, has his critics.
Poking the Bear
NINA TEICHOLZ, 55, was “something of a vegetarian for 25 years,” she says. She says she was constantly trying to lose 15 to 20 pounds and always “felt tired and depressed.”
Then around 2005 she began researching and writing The Big Fat Surprise: Why Butter, Meat, and Cheese Belong in a Healthy Diet, and while she started incorporating more animal products into her diet, she says her health started to improve.

“Saturated fat has been the rate-limiting factor in the consumption of animal foods,” says Teicholz. “Meat and dairy, principally, are foods that we depend on for essential nutrients and vitamins for human health. They’re the most calorically efficient way to get the vitamins and nutrients you need for life.”
Teicholz says there is evidence these foods are healthy even at nearly twice the current guideline recommendation. Suggesting that people limit saturated fats, she argues, steers people away from whole foods such as red meat and dairy.
Teicholz wrote a piece for this magazine in 2007 called “What If Bad Fat Is Actually Good for You?” and has appeared on The Joe Rogan Experience to talk about the topic.
In 2014 her career shifted after John Arnold tweeted an op-ed she wrote for The Wall Street Journal about saturated fat.
Arnold is a billionaire hedge-fund manager with a history of bankrolling counterintuitive nutritional ideas. For example, Arnold spent $40 million in 2012 and 2013 to launch the Nutrition Science Initiative, a project that “supports research that tests fundamental assumptions about the metabolic and hormonal causes of obesity and related disorders,” as stated on its website.
According to Teicholz, she reached out to Arnold after the tweet and he invited her to meet his team at the Arnold Foundation. That meeting eventually led to the Arnold Foundation funding Teicholz to conduct an analysis of the 2015 dietary-guidelines advisory-committee report, which was an independent project, she says.
“Following that, I was funded to start the Nutrition Coalition, whose main goal at that point was simply to educate policy makers about the need for an outside review of the dietary-guidelines process, since there had never been one,” she says.
Teicholz is the Nutrition Coalition’s executive director, a role that, at least as of 2018, was paying her $144,000 a year. The coalition, a 501(c)(3) nonprofit, reports that its funding comes from donations and grants. In 2018, it brought in roughly half a million dollars.

The Nutrition Coalition has argued that the government’s dietary guidelines are based on weak scientific evidence. “In order to continue the limits on saturated fat, health officials must show ample and consistent evidence that these fats damage health,” the coalition has stated. It points to some 20 review studies that have shown an inconsistent link between saturated fat and heart disease.
What’s more, the Nutrition Coalition charges that the members of the USDA’s 2020-25 guidelines committee have damning potential conflicts of interest. Three of the 20 members of the most recent committee, the coalition highlights in a post on its website, have previously received funding from nut commissions or the potato industry, or were affiliated with Nestlé or Dannon.
But the accusations fire both ways.
David L. Katz, M.D., M.P.H., Ph.D., founding director of Yale University’s Yale-Griffin Prevention Research Center, and other scientists believe the Nutrition Coalition is “lobbying” for the meat industry, which has been influencing U.S. dietary guidelines for decades.
Why would the beef industry care about the arguments for or against saturated fats?
Marion Nestle, Ph.D., M.P.H., a food and nutrition researcher at New York University, explains it this way: “The guidelines currently tell us to eat more in the context of foods but use nutrients when referring to what you should eat less of. Nutrients are euphemisms for foods. Saturated fat means meat. They don’t have to say, ‘Eat less of those foods’ directly, thereby saving a lot of political hell,” Nestle says.
There is no evidence that the Nutrition Coalition receives funding from the beef or dairy industry, or any industry at all, but its scientific board does include a member with ties to Virta Health, a company that recommends high-fat, ketogenic diets to help treat insulin resistance in people with diabetes.

And the coalition has supported the work of scientists who conduct research funded by the beef industry. And there’s another grenade critics of the Nutrition Coalition lob: a lack of necessary experience.
“The people who have positions of prominence [at the Nutrition Coalition] include many people with no formal training in nutrition or in science,” Dr. Katz says.
In fact, half of the coalition’s board had no previous experience in the health sector—Teicholz included. She has a B.A. in American studies and an M.A. in Latin American studies.
Despite the accusations made against it, the Nutrition Coalition has moved the dial.
According to Teicholz, her “most successful effort as an advocate was to plant the idea, in 2015, that Congress might consider an independent outside review of the dietary guidelines. The hope for this review was to improve the transparency and scientific rigor of the guidelines.”
And she has chosen to respond to her critics.
Teicholz is at odds with Harvard’s research, and in particular Dr. Willett, because “he has significant intellectual and financial conflicts of interest which he almost never declares in any of his papers,” she says, and “the studies he oversees are a significant part of the foundation of the dietary guidelines.”

Not to mention Dr. Willett is “an ideological vegan” whose work “supports the idea of moving towards a vegetarian-slash-vegan diet,” she says. Teicholz has published a ten-page dossier laying out the terms of how Dr. Willett’s vegan agenda can be explained by his ideological and financial conflicts.
Maybe scientists could write Teicholz off (and some within the field have). Except that more minds in nutrition are becoming sympathetic to the idea that perhaps animal foods aren’t as bad as science has previously made them seem.
“I kind of appreciate [what she’s doing],” says Tamar Haspel, a columnist for The Washington Post who has been covering nutrition and the food industry for two decades. “She’s poking the bear, and the bear needed to be poked.”
All Hell Breaks Loose
IN THE fall of 2019, a group of scientists dropped a series of six papers in the Annals of Internal Medicine, one of the most influential journals in the field, that reviewed the research on red and processed meats.
The papers included studies assessing the health risks of consuming those foods, ultimately questioning the validity of the health guidelines as they pertained to saturated fat.
The 49-person research team found that among study participants, those who ate about four to seven servings of red and processed meats a week had approximately the same risk of cancer, heart attack, or death from any cause as those who ate one to four servings a week.

The difference between the two groups meant that for every 1,000 people who eat less meat, only two would avoid the increased risk of death from any cause that comes with eating more meat.
Based on these findings, this group published its own “dietary guideline recommendations” for Americans: You enjoy beef and bacon, so continue eating it.
This research sent the other side, scientists who have shaped American food policy for the past four decades, scrambling into Defcon 1.
Reenter Dr. Katz, who also leads True Health Initiative (THI), a group of 500-plus health experts that derives its funding from 46 different non- and for-profit groups, most of which are in the fields of health care or nutrition and many of which promote plant-heavy diets or products.
When prerelease copies of the Annals papers landed on the desks of Dr. Katz and others at THI, “we started calling one another and saying in effect . . . Holy shit, this is not for print,” says Dr. Katz. “We thought [it was] going to hurt a lot of people.”
Dr. Katz, who is a Men’s Health advisor, believes the scientists who authored the Annals studies were leveraging the authority of the respected journal to issue their own set of “alternative ‘guidelines,’” as he put it, without any actual legitimate authority: “If they’d just published the [data] and not the guidelines, it would have been a yawn from us. But to devise guidelines directly at odds with your own findings and pretend like that’s business as usual . . . this is a provocation,” he says.

THI responded to the research by pulling together 14 leading scientists and collectively requesting that all six papers be preemptively retracted and given “due and appropriate review. . . . We do so on the basis of grave concerns about the potential for damage to public understanding and public health,” wrote Dr. Katz and his cosigners.
But as THI cooked up its academic retort, the work of the independent committee tasked with reviewing nutrition and health topics that would inform the 2020-25 dietary guidelines, including possible adjustments to saturated-fat caps, was already under way.
The Source of All This Confusion
"AT THE core of this conflict is the value of nutritional epidemiology,” says Stephan J. Guyenet, Ph.D., a neuroscientist and obesity researcher.
“So let’s say that people who eat lots of red meat have more heart attacks than people who eat less red meat,” says Guyenet. “You could see that and conclude that red meat causes heart disease. But maybe people who are eating a lot of red meat are also smoking more cigarettes.”

Teicholz says that when it comes to beef and dairy, the evidence on saturated fat is flawed. “These studies find extremely weak data associations, not causation,” she says.
Richard Feinman, Ph.D., a professor at SUNY Downstate Health Sciences University, puts it like this: “Willett’s textbook on nutritional epidemiology is quite good in that it’s thorough, but it doesn’t let you draw the right conclusions. In a toxic tort case in a court of law, for example, these studies wouldn’t hold up as evidence,” he says.
Dr. Willett believes his detractors and those who laud the supposed benefits of beef, in particular, are part of what he calls the disinformation triangle. “It’s a triangle of interests that are people not working together to guide consumers,” he says.
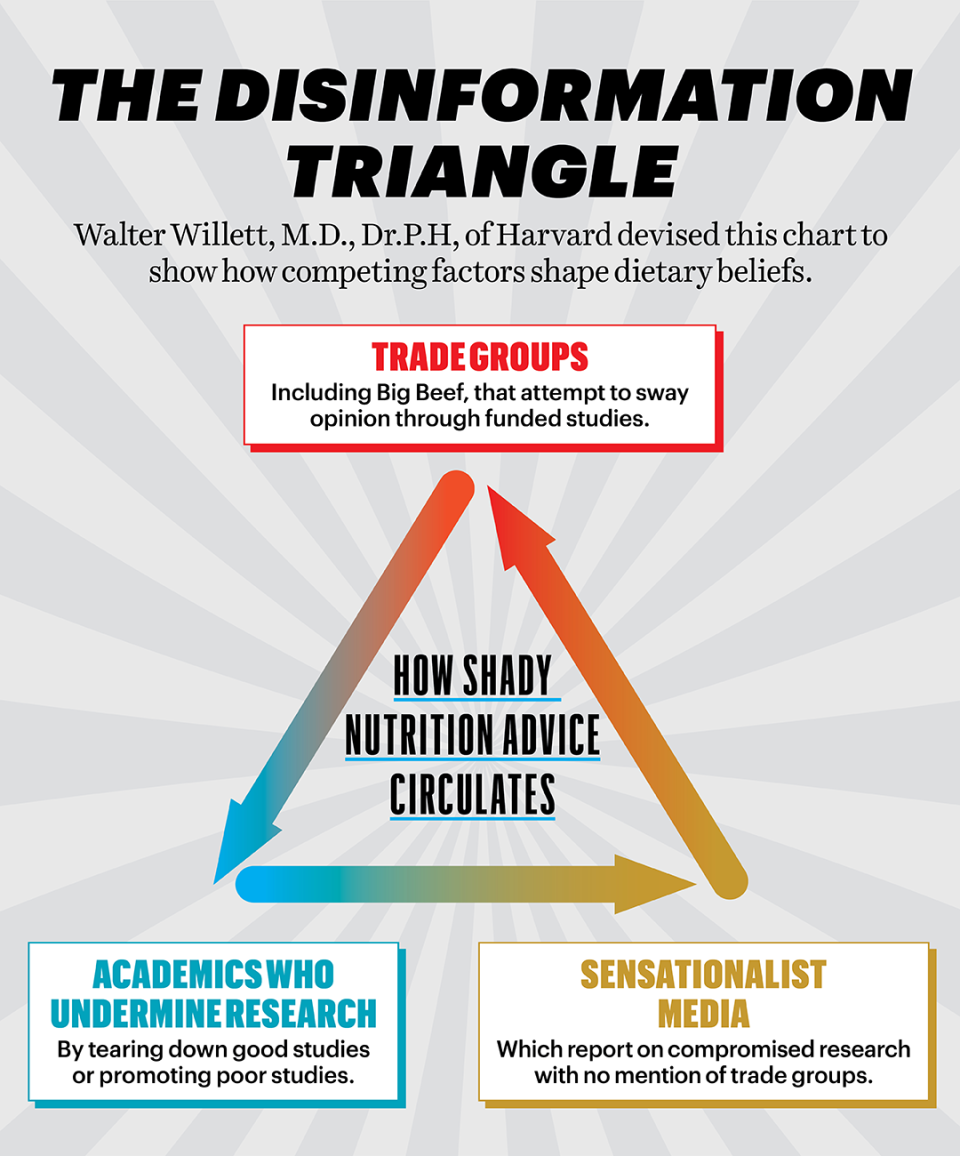
Its three points are food-industry groups, such as Big Beef; academics who make a career bashing others’ epidemiological research and/or supporting industry research that misleads the public; and the sensationalist media, which reports on that industry-funded research.
His critics, he says, are missing the larger point: His food-frequency questionnaires were never designed to be perfect.
A perfect nutrition study would be unfeasible, and downright unethical—scientists would have to hold many thousands of people in a lab and feed them specific diets over the entirety of their lives. Dr. Willett says his type of studies are good enough to make rational decisions.
But he isn’t off the hook.
Teicholz points out that Dr. Willett and Harvard’s nutrition department have conducted studies funded by nut boards or other trade groups.
Nestle, the NYU nutrition researcher, is also aware of this funding and says, “I really wish they wouldn’t do that.”
The Danger of Isolationism
THERE'S YET another complicating factor to all this: Although the saturated-fat debate centers primarily on red meat, the nutrient is found in many other foods.
“It’s not possible to eat saturated fat in isolation. Therefore you have to question the significance of studies that study saturated fat as opposed to the foods that contain it,” says Nestle.

Perhaps the strongest statement suggesting a rethink on saturated-fat caps came out in The BMJ in 2019.
Nineteen leading scientists (many of whom declared ties to the dairy, nut, and other industries) concluded that the established guidelines “fail to take into account considerable evidence that the health effects vary for different saturated fatty acids and that the composition of the food in which they are found is crucially important.”
The saturated fats found in a square of dark chocolate or in nuts are different from those in a rib-eye steak. And they have different effects in the body, says Ronald Krauss, M.D., Ph.D., director of atherosclerosis research at Children’s Hospital Oakland Research Institute, who helped develop the American Heart Association’s dietary guidelines in 2000.
“There’s not just one LDL cholesterol particle. They vary in size from large to small,” says Dr. Krauss. “The smaller LDL particles have properties that make them more likely to have adverse effects in the artery and promote [heart disease]. This is why zoning in on saturated fat as a single macronutrient category as the basis for the nutritional recommendation, to me, is a flawed approach.”
Lumping together all saturated fats, some scientists now believe, may steer the food-marketing industry toward advertising foods that are low in saturated fat, yes, but also high in refined starch and sugar.
This effect happens often with many broad recommendations based upon single nutrients, says Trevor Kashey, Ph.D., a former cancer researcher who now owns Trevor Kashey Nutrition.
In fact, it’s happened in the recent past: The recommendation to eat more fiber is meant to encourage people to eat that nutrient from whole-food sources, says Kashey. Whole foods like grains, fruits, and vegetables. “But then,” Kashey says, “bakeries start making bran muffins.”
So: Is Saturated Fat Bad or Not?
FORMER U.S. secretary of health and human services Sylvia Burwell and former secretary of agriculture Tom Vilsack oversaw the development of the current nutritional guidelines.
And in 2015 Congress pulled the two into a hearing to ask about them. “The key here is taking a look at the preponderance, the greater weight of the evidence, and trying to make a judgment . . . this is really about well-informed opinion. I wish there were scientific facts,” said Vilsack.

And so was born a new directive for the scientific committee: to look at the totality of the nutrition and health research for those facts.
Five years later, the 20 scientists on the advisory committee whose report forms the basis of the 2020-25 nutritional guidelines looked at the evidence about saturated fat and are recommending changing . . . nothing.
And, in all likelihood, the eventual government dietary guidelines will reflect that exact recommendation: Americans should consider swapping saturated fats with unsaturated fats and limit their saturated-fat intake to 10 percent or less of their total calories per day.
But the report also stated that it’s more important to account for a person’s overall diet than individual nutrients. “People do not consume nutrients or foods in isolation but in various combinations over time,” the scientists wrote.
Instead, people should aim for “higher intake of vegetables, fruits, legumes, whole grains, low- or nonfat dairy, lean meat and poultry, seafood, nuts, and unsaturated vegetable oils and low consumption of red and processed meats, sugar-sweetened foods and drinks, and refined grains.”
That part of the report is a good one, nutrition experts argue.
“We don’t eat saturated fat,” says Kashey. “We eat bacon cheeseburgers and ice cream.”
Just 28 percent of the saturated fat the average American eats comes from proteins and dairy, such as a piece of meat or glass of milk. Sixty percent of it comes from multi-ingredient foods.
“If people actually followed the guidelines and stopped eating all the bacon cheeseburgers and ice cream, they’d be healthier,” says Kashey.

Nestle takes it even one step further to say that if people eat mostly whole foods and move more, saturated fat becomes practically irrelevant.
In fact, 10 percent saturated fat in a diet of whole foods isn’t all that limiting—something like three eggs, two slices of bacon, a serving of full-fat Greek yogurt, and a broiled six-ounce New York strip topped with a pat of butter and washed down with a glass of whole milk in one day.
All this said, the committee report does not offer the equivalent of a dietary blank check.
“There aren’t many true academics—even the ones funded by the beef industry—recommending people eat a ton of beef,” says Haspel.
The scientists and dietitians interviewed in this article suggested consuming up to four weekly servings of it.
“If people want to eat red meat, we generally steer people toward leaner cuts,” says Brian St. Pierre, R.D., C.S.C.S., director of nutrition at Precision Nutrition. “Because that makes it easier to control intake.” Not because of saturated fat specifically but calories generally.
And the experts also agreed that the best diet isn’t nutrient focused—it’s food focused. The best diet takes into account food preference, variety, and enjoyment. It’s the sum of its parts.
And the best diet, they agreed, isn’t carnivore—and it isn’t vegan, either. It’s where the warring sides of nutrition infighting can’t often meet: somewhere in the middle.
A version of this article originally appeared in the January/February 2021 issue of Men's Health.

‣ Editors' Note: Since the publication of this piece in the January/February 2021 issue, the government released the Dietary Guidelines for Americans 2020-2025. The recommendation for saturated fat did not change: Starting at age two, individuals should limit their saturated fat intake to less than 10 percent of total daily calories. In addition, Nina Teicholz contacted Men’s Health to note that the Nutrition Coalition does not receive funds from industry, which is consistent with our reporting, and that its Scientific Council is composed of eight health experts. Further, we have added David Katz’s affiliation as a Men’s Health Advisor to the digital version of this article. Katz receives no payment for his role on our Advisory Board.
You Might Also Like
