Here's What Really Happens When You Get an IUD Inserted (and Removed)
When recent TikTok threads about surprising and extreme intrauterine device (IUD) insertion pain popped up in my social media channels, I had a visceral reaction. My uterus basically shouted: me too!
I got my IUD a few months after my second daughter was born. After two very intense deliveries with no pain medication (the first time the epidural didn’t take and the other time, I elected to do a “natural” birth), I considered myself a veteran of obstetrical discomfort. It didn’t really occur to me that this small procedure would hurt, but it did – big time. Both in the stirrups and for many days afterwards, as I nursed severe cramps and heavy bleeding.
Five-plus years later, as I scrolled through the many agonizing insertion stories, I realized how much time had truly passed since I got my own IUD – and that my device was set to expire. I had to wonder what it was going to feel like to get it out.
Why get an IUD?
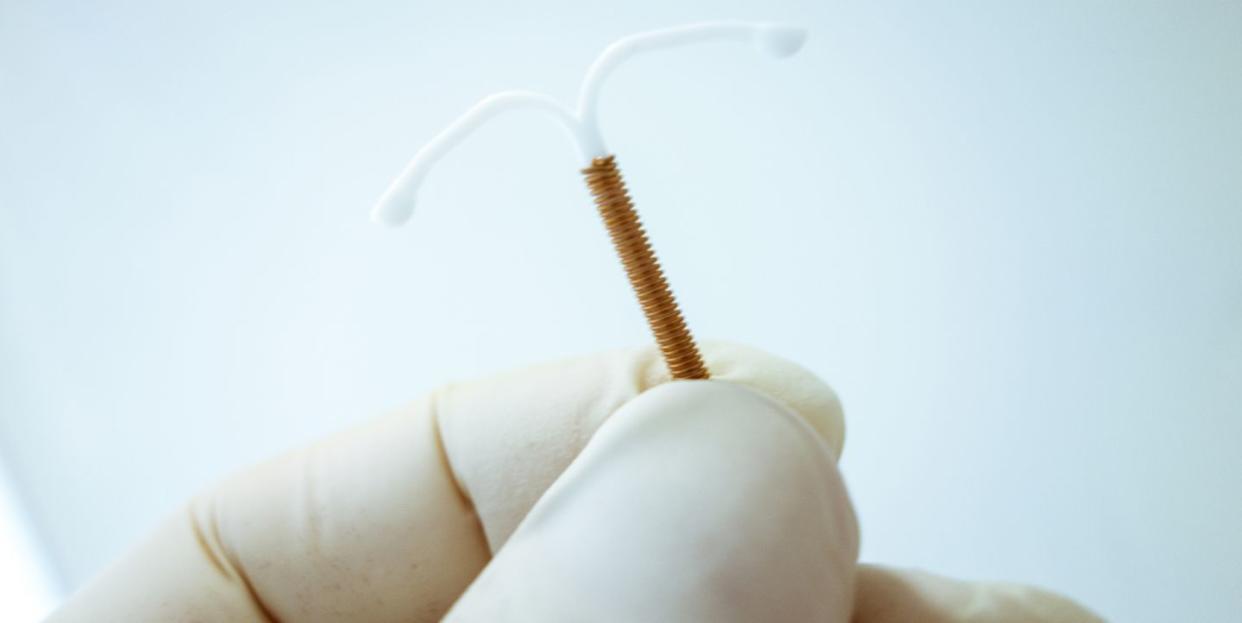
An IUD is a tiny T-shaped contraceptive device that is inserted through the cervix into the uterus. There are two types: hormonal IUDs and the non-hormonal copper IUD. Both work to prevent sperm from reaching an egg. Hormonal IUDs release progestin, which thickens cervical mucus, making it harder for the sperm to enter the uterus, and thins the lining of the uterus, making implantation nearly impossible. The non-hormonal IUD releases copper, which interferes with sperm mobility. Once an IUD is in place, it’s 99% effective at preventing pregnancy.
It takes only a few minutes to insert an IUD, and once you leave the OB/GYN’s office, you don’t have to do a thing – literally for years. “An IUD is recommended for any patient who is interested in a method of birth control that gives them long-term ‘set it and forget it’ pregnancy prevention, since IUDs can work for three to 12 years, depending on the type,” says Meera Shah, M.D., chief medical officer of Planned Parenthood Hudson Peconic in New York. “It means no trips to the pharmacy, no birth control pill to take or ring to put in, and nothing you have to do before sex to prevent pregnancy,” she says. (Though you may still need a barrier method, like a condom, to protect against sexually transmitted infections.)
Getting an IUD can cost as much as $1,300, but there are free or low-cost options with many health insurance plans, some government programs or through Medicaid. It’s one of the most cost-effective options in the long run, considering birth control pills can add up to $226 per year, even with insurance.
“Another thing is that up to 40% of people won’t get a period while they have a hormonal IUD in place,” says Shauna L. Pagel, a certified nurse practitioner with The MetroHealth System in Cleveland. (A non-hormonal copper IUD, on the other hand, can make periods heavier and cramps worse.) I was such a fan of my barely-there periods courtesy of my IUD, that I kept it in even after my husband got a vasectomy and I technically didn’t need it anymore. I figured it was already in place, and, after the very uncomfortable insertion experience, I wasn’t in a rush to go through a removal.
How painful is it to get an IUD inserted?
Although IUD insertion discomfort is often described by both practitioners and the medical literature, as “mild,” or “a pinch,” many people who have gone through it will tell you otherwise. A petition originating in the U.K. demanding better access to pain management during the procedure has amassed nearly 35,000 signatures. Roughly 43% of those who also shared their experiences rated their insertion pain as a 7 or higher on a scale of 0 to 10. Some described it as “worse than childbirth.”
IUD insertion pain may be another example of the gender pain gap, an adjacent topic that has recently been experiencing a swell of attention. It’s based on the understanding that there is an implicit bias in health care rooted in sexism and racism that has led to the underserving of women in medical settings. Even if your practitioner is another person with a uterus, and a person of color, they are working within a system that still doesn’t adequately legitimize pain experienced by women or marginalized folks. “The pain gap is particularly pronounced when it comes to gynecological services, because for most of medical history, and up until now, women’s voices about what they are experiencing have been disregarded, minimized and trivialized,” says Leigh Senderowicz, a health disparities research scholar at the University of Wisconsin School of Medicine and Public Health.
What pain relief options are offered for IUD insertion?
“There are a wide variety of experiences people can have when getting an IUD placed, which can range from feeling no pain or discomfort at all to feeling minor discomfort to experiencing true pain,” says Dr. Shah. “The good news is that it’s a quick process and most IUD users think it’s worth it in the end.”
If your practitioner doesn’t mention pain management during your IUD consultation, be sure to ask what your options are. Protocols vary depending on the hospital or health center. “Most of our patients do well with over-the-counter medicine like acetaminophen or ibuprofen. In rare instances we can provide oral sedation or sedation through an IV,” says Dr. Shah. Some practitioners can also provide a paracervical block (a type of anesthesia) to assist with pain, and a small 2018 study found that this did help with the insertion pain. But the block itself can be quite uncomfortable as well, even more so than the IUD placement itself, says Pagel. “I usually recommend patients come in while on their period to have the IUD placed. Usually, the cervix is opened a little, making it easier for the provider and patient,” she says. “I also recommend taking ibuprofen, if the patient is able, prior to the visit.”
Will there be pain after an IUD insertion?
Unfortunately, for some women the discomfort doesn’t end in the stirrups. “The most common side effects after placement are spotting and cramping,” says Pagel. Both should ease after a few days. If you experience heavy bleeding (defined by the American College of Obstetricians and Gynecologists [ACOG] as soaking through one or more pads in an hour, for several hours in a row), pain that continues after two days, or notice a foul-smelling discharge, call your practitioner.
Serious complications with an IUD are very rare, but still, they do happen. According to ACOG, uterine perforations occur in approximately 1 out of 1,000 cases. A very small percentage of IUDs are involuntarily expelled from the cervix, a complication that can cause extreme pain.
It’s a good idea to talk with your practitioner about what to expect before you’re in the stirrups. “My advice for anyone worried about pain is to ask their nurse or doctor about medicine or other ways to help with pain management when making the appointment. That way you have information upfront – before the insertion,” says Dr. Shah.
Senderowicz agrees: “Have those conversations before you are in that uniquely disempowered position. I also think people are often afraid to interview providers before they select one, but remember that you can choose who will perform this medical procedure. And you can ask them about the removal process as well.”
When do IUDs need to be removed?
The timeline for removal varies depending on the device:
Mirena will prevent pregnancy for up to 7 years.
Kyleena for up to five years,.
Liletta should be removed after six years
Skyla is good for three years
Paragard (the most common non-hormonal IUD) will prevent pregnancy for up to 10 years
You can get your IUD removed earlier than any of these recommendations, though, if you’d like to get pregnant, or if you think another form of contraception will suit you better.
What happens during an IUD removal?
Taking out an IUD is much the same as a routine pelvic exam; I even booked mine to coincide with my Pap smear. You’ll lay on the exam table with your feet in stirrups and your doctor will insert a speculum to open your vagina. They will look for the IUD threads or strings, then use forceps to grasp them and pull them downward, triggering the arms of the IUD to fold up so the device can slide out. The whole procedure takes under five minutes. In rare cases your practitioner may have trouble seeing the strings (if, say, they were cut a bit too short at insertion), or if they’ve curled up into the cervix. In those situations, the doctor or nurse can use ultrasound to guide the procedure, if necessary.
Despite how simple it sounds – and the recent alarming “remove your IUD at home” TikTok challenge – this isn’t something you can or should DIY. Removal should always be performed by a doctor, or other qualified health practitioner. Improper removal could cause tearing and bleeding on the way out, or for the device to become improperly positioned, which could cause serious cramping and discomfort until you can get an appointment with a doctor.
Many insurance providers will cover the removal fees, but according to research in the journal Contraception, cost is a serious factor driving some women to consider removing their IUD themselves. If this is you, Planned Parenthood can assist with finding a low-cost clinic in your area.

Does IUD removal hurt more than insertion?
In my case, the removal was literally over before I realized it. My (thankfully very experienced and friendly) doctor got me chatting about my kids and summer camps and before I could even finish sharing my family’s holiday plans, she declared it was all done. I didn’t feel a thing – until I got home.
“Having an IUD removed is usually much less uncomfortable,” says Pagel. But there can be side effects. As with insertion, if you experience heavy spotting or pain that continues after two days, call your practitioner.
I had moderate cramping (reminiscent of the PMS cramps I experienced pre-IUD) for two days, followed by a spotty sort-of period for about six more. It wasn’t nothing, but, luckily, it wasn’t a huge deal, either.
How long is the recovery from an IUD removal?
Being prepared for my IUD removal made the experience much easier. I arrived at my appointment already dosed with two extra-strength acetaminophens, and a list of questions for doctor about the procedure and after-care. (How long does it take to remove it, exactly? What are the chances of complications? Will it hurt as much on the way out as it on the way in?)
Afterwards, my doctor suggested going home and curling up on the couch with a heating pad and Netflix for the rest of the afternoon. I took her up on that, grateful for the permission to take a few hours to myself and binge a new show. “It can be a luxury to take time to care for ourselves, but it should be a serious part of the process,” says Senderowicz. “An IUD is a medical device that’s being inserted and removed – to the extent that you can, give your mind and body ample time and space to recover.”
You Might Also Like

