Mumps is making a comeback — here's what you need to know
Every once in a while, news of a mumps outbreak makes headlines. The highly contagious viral disease has popped up on college campuses across the U.S. and even among players on the 2014 Pittsburgh Penguins. Researchers now say they know why: The mumps vaccine becomes less effective over time.
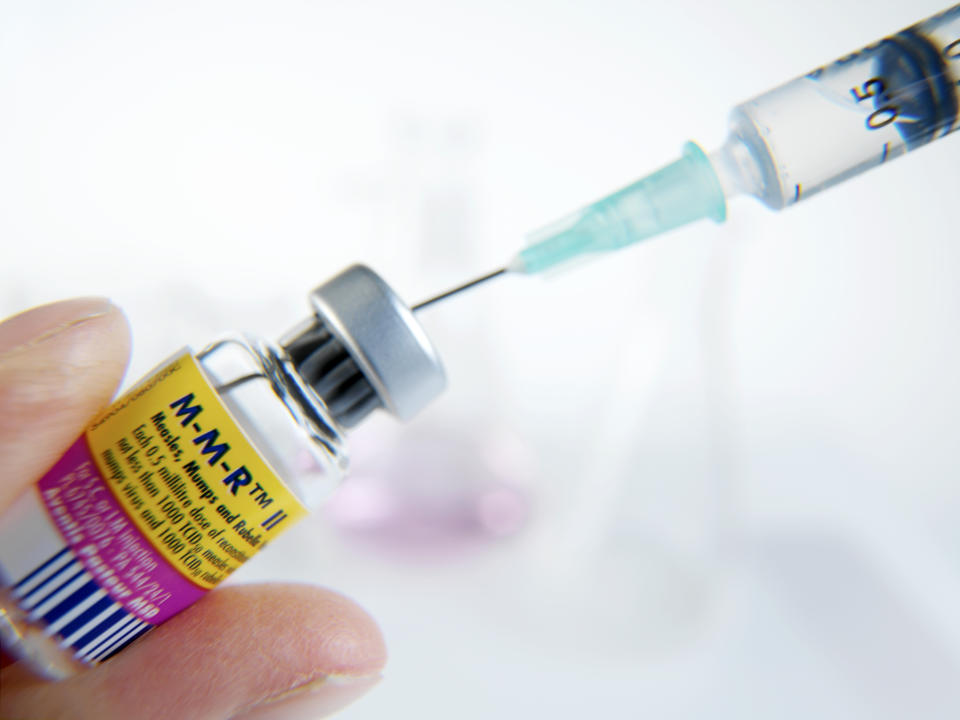
Researchers behind a new study published in Science Translational Medicine analyzed data from epidemiological studies and mathematical models and found that recent outbreaks of mumps have been largely in people between the ages of 18 and 29 — most of whom received the recommended two shots of the measles, mumps, and rubella (MMR) vaccine as kids.
The researchers found that about 25 percent of people who receive the MMR vaccine will lose their immunity in eight years, 50 percent will lose it in 19 years, and 75 percent will lose it in 38 years.
It would seem that the solution to waning immunity would be simple — just give people another dose of the vaccine, but it’s a little more complicated than that, Amesh A. Adalja, MD, a board-certified infectious disease physician and senior scholar at the Johns Hopkins University Center for Health Security, tells Yahoo Lifestyle. “It’s too premature to think that the general population needs to have a third vaccine,” he says. When outbreaks occur, it’s recommended that people who may come into contact with those infected get a third dose of the vaccine (for example, everyone on a college campus that’s seeing a mumps outbreak) to help quash the outbreak, he says. Otherwise, there’s no official line.
That doesn’t mean the idea of everyone getting a third dose of the vaccine hasn’t been considered. It’s been discussed at the CDC’s Advisory Committee on Immunization Practices, William Schaffner, MD, an infectious disease specialist and professor at the Vanderbilt University School of Medicine, tells Yahoo Lifestyle. But so far, no concrete recommendations have come out of that, and there are a few reasons why. One is that it may not be cost-effective to immunize everyone again, and the other is that there’s no good data to say how long that third dose would actually last, Schaffner says. Still, “it’s been much debated,” he says.
Luckily, having the recommended two doses of the MMR vaccine does seem to make cases of mumps less severe than if you weren’t vaccinated at all, Frank Esper, MD, a pediatric infectious disease physician at Cleveland Clinic Children’s Hospital, tells Yahoo Lifestyle. But overall, the illness isn’t usually severe, making it hard for experts to definitively say that having the mumps vaccine makes a huge difference if your immunity has waned. “For the most part, mumps is a very mild disease,” Esper says. “It’s difficult to say if you have a severe mild disease or mild mild disease.”
In 2016, the U.S. experienced more than 6,000 cases of mumps — more mumps cases than the country had seen annually in 10 years, according to data from the Centers for Disease Control and Prevention (CDC). The number of cases fell a little in 2017, but numbers were still well above what they had been in years prior to 2016. In 2018, 304 cases have been reported so far.
Mumps causes fever, headache, muscle aches, fatigue, loss of appetite, and swollen and sore salivary glands under the ears on one or both sides, according to the CDC. It also causes characteristic puffy cheeks and a swollen jaw in sufferers. Most people with mumps recover completely within a few weeks.
Still, mumps vaccination and its effectiveness is being closely watched by the public health community. Mumps generally happens in the U.S. when someone from a different country with less common vaccination practices introduces it to people here, Esper says. And given that the world is only getting smaller, he expects this to continue to be an issue. “I would say that we’re more likely to see more cases in the future than we’ve seen in the past 10 years,” he says. “We very well may get to a point where we will go ahead and recommend a booster dose.”
Read more from Yahoo Lifestyle:
Follow us on Instagram, Facebook, and Twitter for nonstop inspiration delivered fresh to your feed, every day.

