'Every time I close my eyes, he is with me': A former nurse on life after a manslaughter conviction

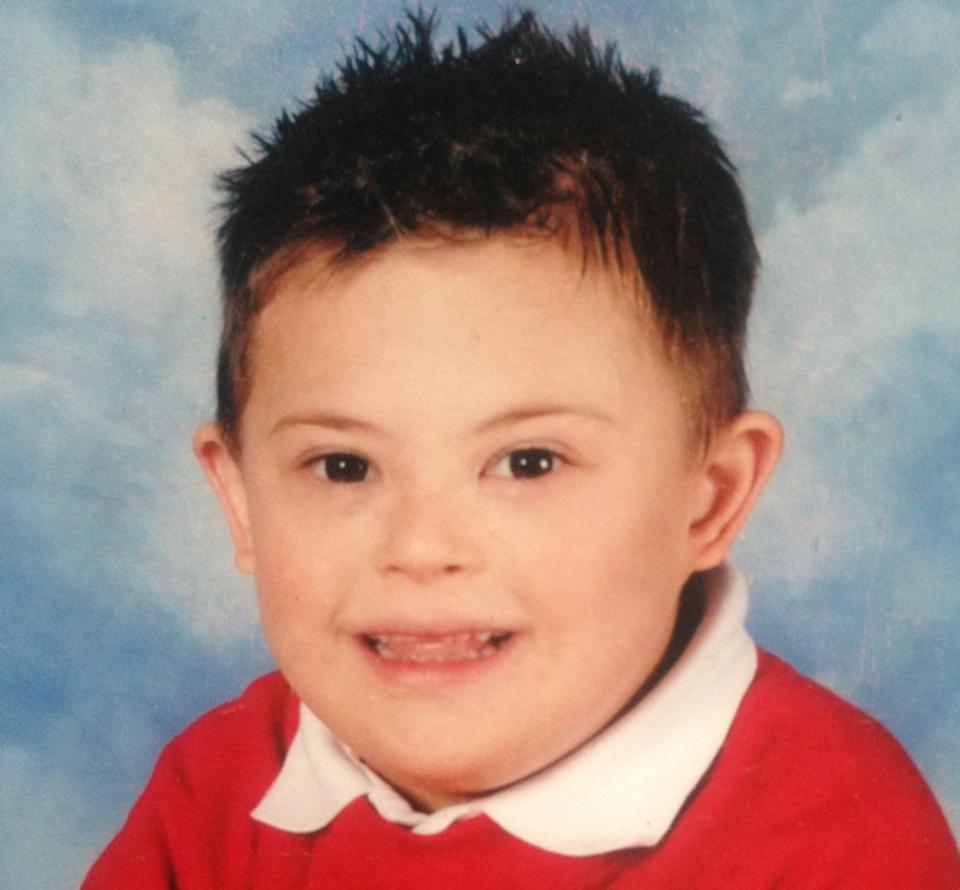
Jack Adcock was a lively little six-year-old, who loved dancing and football, and should never have died.
His mother Nicola had taken him to Leicester Royal Infirmary for a check-up after he developed a temperature, sickness and diarrhoea one morning. She wasn’t unduly concerned – Jack had Down’s syndrome so, although otherwise healthy, such visits were routine.
Yet after they arrived, Jack’s condition deteriorated. Wrongly diagnosed with gastroenteritis, Jack was actually suffering from sepsis – a condition fatal when left undetected and one that caused his organs to stop functioning, prompting a heart attack brought on by septic shock.
Jack’s death in February 2011, 11 hours after being admitted to hospital, not only devastated the lives of Nicola and her husband Victor, but unleashed a controversial legal case that spanned the following decade.
Accused of making a string of medical errors, Jack’s paediatrician, Dr Hadiza Bawa-Garba, and his nurse, Isabel Amaro – both of whom had held unblemished careers in the medical profession – were charged with manslaughter by gross negligence.
They were convicted after a four-week trial at Nottingham Crown Court in November 2015 and both given two-year suspended prison sentences (a second nurse, Theresa Taylor, was cleared).
Dr Bawa-Garba was found to have made mistakes from failing to act on Jack’s abnormal blood tests to mistaking him with another patient under a do-not-resuscitate order. Amaro had failed to keep accurate records of Jack’s blood pressure, temperature and fluid input-output, and to escalate concerns appropriately.
Yet the verdict caused uproar among doctors, who claimed Dr Bawa-Garba had been scapegoated for multiple failings within a beleaguered NHS – that her working environment was one of intolerable pressure in which mistakes were bound to happen. After she was struck off the medical register in January 2018, thousands of doctors crowdfunded more than £360,000 to support a successful appeal. In July 2019 she was allowed to return to work under supervision.
But what of Isabel Amaro? While Dr Bawa-Garba’s case became a cause célèbre, the nurse convicted alongside her has been largely ignored, the support from her own profession conspicuous only in its absence.
‘I have been made a scapegoat,’ says Amaro, speaking for the first time since the conviction seven years ago. ‘We should have been treated equally and we weren’t.’
The difference is stark. Whereas Dr Bawa-Garba, a trainee paediatrician who had qualified in 2003, continued to work at Leicester Royal Infirmary for four years, until her trial, Amaro, an agency nurse, says she was suspended from her agency within days of Jack’s death.
Whereas the group of doctors crowdfunding for Dr Bawa-Garba had the money to instruct Tim Johnson Law for her appeal, Amaro was forced to represent herself at her 2016 hearing in front of the Nursing and Midwifery Council’s Conduct and Competence Committee (CCC), which resulted in her being struck off.
And while, last July, the Medical Practitioners Tribunal Service (MPTS) lifted all remaining restrictions on Dr Bawa-Garba, who is a practising doctor again, Amaro has not worked since she was suspended from nursing in 2014.
Unable to marry her criminal status with her desire to be a nurse, she is haunted by both the loss of her patient and those who have failed to support her. She has made three suicide attempts, and was deemed too ill even to give evidence at her criminal trial. She has been abandoned by all but one of her friends, subjected to death threats, and lives alone in a one-bedroom housing association flat.
After years of seeing a psychologist, she has regained emotional strength, and is now determined to share her story publicly for the first time. She sits on a sofa in her flat in Manchester as we speak over FaceTime, her expression a mixture of anguish, defiance and regret, and her recollections punctuated with tears.
‘I apologise for Jack’s death and can understand his parents wanting justice. I think about Jack every single day and wish I could ease the family’s pain,’ says Amaro, 54. ‘I don’t expect their sympathy, but I have been ruined too. My job was my life and without it I am nothing.’

Having followed this case closely, I have spoken to Amaro several times in the past three years. She is not an easy person to interview. She gets distracted, confused and defensive, and I can see why she might have tested the patience of authorities she has encountered since Jack died. But her account of her involvement in Jack’s death has been constant throughout our conversations. She doesn’t accept all the findings of her conviction.
‘I acknowledge I made mistakes in paperwork, because I was so overwhelmed. I said Jack didn’t go to school when he did. But I don’t think those mistakes were relevant.’ Amaro is referring to her record keeping and observations, which, her barrister argued at her 2015 trial, despite being flawed, had no bearing on Jack Adcock’s treatment, because Dr Bawa-Garba never looked at them.
‘What I do know now, after all these years, is that I should have tried harder to raise my concerns that Jack should have been transferred to intensive care. But I was just an agency nurse. Nobody would listen. I’ve had no contact with Dr Bawa-Garba. I don’t feel an affinity with her. She’s had all the support.’
She is not alone in feeling she has been treated unfairly. Nicola Adcock herself tells me: ‘I don’t want either of them to work again, but where was the nurse’s support? I have to agree – the way she has been treated, compared to the way the doctor has been treated, is not right.’
She says Amaro apologised to Nicola in court for the loss of her son, who would have been 18 last month. ‘Due to those two people, he’s no longer here. I will never forgive her, but I appreciate her being remorseful and saying sorry many times.’
Amaro – who qualified as a nurse in her native Portugal in 1991 – was already working on a paediatric ward when she found out that gynaecological problems meant she couldn’t have children. ‘Being able to work with children eased the pain of knowing I wouldn’t have my own.’
She moved to the UK in 2008 and became an agency nurse for the NHS. She was put on an open contract to Leicester Royal Infirmary in December 2010.

She says working conditions on her shifts were ‘chaotic’ there, adding: ‘We were all agency staff, we were understaffed. But I loved children and could cope with stress.’ She took time to assuage parents’ concerns: ‘I listened, I reassured. I wouldn’t have been the nurse I was if I hadn’t.’
When Jack was brought to the children’s assessment unit at 10am on 18 February 2011, Amaro had been working for 11 days straight. She and one other agency nurse were looking after eight other children, three of them critically ill. ‘I had four children who needed constant attention. I worked through my break. I was busy but trying my hardest and I attempted to take all of Jack’s readings every hour.’
She insists Jack’s agitated demeanour meant she couldn’t accurately test his blood pressure. ‘He’d say, “No, no, no,” when I tried. If I put pressure on him the reading wouldn’t have been accurate, so I didn’t have anything to write down,’ says Amaro.
Neither could she assess Jack’s oxygen saturation levels, she claims, because Jack’s temperature was spiking, that left his hands and feet frozen, which meant the probe used to do the assessment, which would normally be applied to his fingers or toes, wouldn’t take the reading.
She couldn’t do a fluid balance chart, she adds, because to do that she would need to weigh all of Jack’s nappies, and some had been changed without her knowledge and thrown away when soiled. ‘I was accused of not taking into consideration the results of an X-ray, but as an agency nurse I couldn’t log myself into the computer to access it,’ says Amaro.
She says the results of blood tests Dr Bawa-Garba had taken shortly after Jack’s admission showed high levels of lactate, which indicated Jack had sepsis, and she reported her concerns to a senior staff nurse.
‘I said, “Who shall I raise my concerns to? Because Jack needs to be on a high-dependency unit,”’ she recalls. ‘She said, “Don’t talk to anyone, you are only a nurse, this is why we’ve got doctors who know more than us.”’
Amaro says this was not brought up at her trial. She doesn’t know why. She adds that she raised concerns that Jack’s temperature had spiked to 38.8 degrees at 3pm, but claims Dr Bawa-Garba refused to take those concerns seriously. ‘I should have said he should have been transferred. But I felt powerless. Nobody seemed to care what I said. Dr Bawa-Garba seemed overwhelmed. The IT systems had gone down. Everything that could have gone wrong, did.’
The last time she saw Jack, after she had been told to transfer him to the hospital’s paediatric ward that evening, he waggled his fingers at her and smiled. Shortly afterwards he suffered a septic shock.
She learned Jack had died at 9am, when she returned to work the following morning. ‘I felt I’d been punched in the stomach. It shouldn’t have happened. I knew Jack had sepsis and should have said so,’ says Amaro, who says, however, that there was no suggestion she was implicated in his death as she worked a 19-hour shift that day, her sadness palpable to colleagues: ‘I was told I’d have a lot of support.’
A week later, however, she says she received an email from her agency to tell her she’d been suspended, with little further explanation, and was evicted from the hospital accommodation she’d been staying in.
While Dr Bawa-Garba was spoken to as part of her training by Leicester Royal Infirmary, Amaro had no further contact with the hospital. ‘I was hurt, confused, shut out and unsupported.’ She says she returned to the hospital three times to try to find out why she had been suspended, but was refused access to the notes she’d made. ‘I left my phone number and email address but the nurses were increasingly dismissive of me,’ says Amaro.
Richard Mitchell, chief executive at University Hospitals of Leicester NHS Trust, said: ‘Jack Adcock’s death in 2011 was tragic and we are deeply sorry he died whilst under our care.
‘It may be difficult to identify specific actions taken 11 years ago, but we recognise the enormous impact the loss of Jack has had on his family and loved ones, and we have learned many lessons from this.
‘We would be happy to hear from Isabel about her experience as part of our ongoing commitment to be a supportive employer.’
Amaro moved back to Manchester and carried on working as a locum nurse through another agency until, in January 2014, the NMC told her she was suspended, pending a hearing into her fitness to practise. She says: ‘I became depressed. I had no family in Britain to talk to.’
An internal inquiry by Leicester Royal Infirmary that concluded in 2012 recommended some 100 changes following Jack’s death, with failures detected including medical and nursing staff shortages, IT system failures and deficiencies in handover.
By Jack’s inquest in July 2013, experts had decided there may be sufficient grounds to prosecute. In December 2014, Amaro and Dr Bawa-Garba were charged with manslaughter by gross negligence. Amaro’s depression accelerated. ‘I couldn’t believe I was being branded a criminal. I thought my life was over,’ she says.

Around this time, she was diagnosed with spinal muscular atrophy, a genetic condition that makes the muscles weaker, and made her more prone to falling. One of the medications she was put on has agitation and anxiety as a side effect.
She missed a pre-court hearing in 2015 because she was in hospital, having attempted to take her own life, the first of three suicide attempts. ‘My neighbours called the police, who smashed my door down. I just wanted to die.’
As her trial approached, Amaro – who’d been pictured in the press – was abused in the street. ‘People asked, “Why did you do it?” One said, “I would kill you but you don’t deserve my time.” I became scared to leave the house and stayed in bed all day,’ she says. All but one friend, who still supports her today, stopped contacting her: ‘To them I was a criminal. It hurt.’
By the time of her trial Amaro’s depression was so severe she could ‘barely function’ and she didn’t give evidence. ‘I could see the damage. I could see what it had done to her. She was very unstable,’ remembers Nicola Adcock.
For her own well-being, she was detained at HMP Peterborough after the jury went out, where she recalls being branded a ‘cow and a bitch’ by fellow inmates. ‘I was frightened and confused,’ she says.
On sentencing her and Dr Bawa-Garba at Nottingham Crown Court, judge Mr Justice Nicol told both that they would never work again. ‘When the verdict was read out, I was standing in the dock and started shaking and crying. I couldn’t look at anyone. I felt empty, finished,’ says Amaro, who was, nonetheless, apparently considered well enough by authorities to return to her Manchester flat on probation.
Ahead of her two-day hearing in front of the CCC the following year, she says she asked the Royal College of Nursing, her union body, to provide her legal support, but didn’t hear back.
An RCN spokesperson said: ‘We advised Ms Amaro in relation to her referral to the Nursing and Midwifery Council [NMC]. Any suggestion we did not reply to her requests about representation is untrue.’ The RCN would not elaborate on the nature of their advice.
Amaro represented herself at the NMC in London in August 2016. ‘She was sending documents to the wrong places. She didn’t know the case law in the way that Bawa-Garba’s lawyers knew the case law,’ says Dr Nathan Hodson, academic clinical fellow at the University of Warwick, who wrote a paper comparing the treatment of Dr Bawa-Gaba and Isabel Amaro, published in the journal Nursing Ethics in 2019.
And whereas the MPTS and Appeal Court determining Dr Bawa-Gaba’s fate came to the conclusion that the judge’s comments on her career could be disregarded, the CCC panel said it ‘bore in mind’ the judge’s sentencing remarks, with panel chair Karen Heenan claiming ‘a striking off order is the only appropriate and proportionate sanction sufficient to satisfy the public interest’.
Amaro left the hearing before it had finished before suffering a panic attack. By the time she felt strong enough to meet NMC Watch, a service that supports nurses going through fitness to practise investigations, her 28-day window to appeal had passed and she had ‘no ability to launch a big campaign like the… campaign for Dr Bawa-Garba’, says a spokesperson at the organisation, who has asked not to be named for fear of a ‘backlash’.

‘The two cases highlight how both the public and professions react to different healthcare professionals. There is always a lot of support for doctors – their colleagues raise funds quickly and are able to access legal support. In the case of a nurse, the same support doesn’t seem to be readily available.
‘I don’t feel Izzy was treated fairly.’
Explaining the decision, Andrea Sutcliffe, chief executive and registrar at the NMC, said: ‘In 2016, an independent fitness to practise panel decided to remove Ms Amaro from the NMC register, taking her criminal conviction for gross negligence manslaughter of a patient and suspended custodial sentence into account. Convictions of this kind are extremely rare and will always warrant very careful consideration by regulators. Since there was no appeal, the decision stood.’
Dr Hodson was a junior doctor working at Leicester Royal Infirmary during Dr Bawa-Gaba’s hearing to determine whether she should be struck off in 2017. ‘I remember sitting in the canteen and all the doctors discussing the implications for them and their practice. No-one was talking about Isabel Amaro. She seemed to be such a footnote,’ he says.
‘Doctors have a culture of support. We pool our resources to pay for lawyers. We spend a lot of money on the BMA which advocates hard for us. We all make significantly more than nurses. All of this sets up a culture that allows this discrepancy.’
Sutcliffe added: ‘We recognise fitness to practise proceedings can be distressing for everyone involved, including families and nursing and midwifery professionals. We have a range of support in place, including an independent careline so that professionals can speak to someone in confidence to get the emotional support, practical help and advice they need.’
Yet Amaro insists she wasn’t made aware of a careline: ‘I didn’t have any support from the NMC or RCN. It was as if they didn’t want to know me.’
Given that five years have passed since she was struck off, she could apply to be restored to the nursing register. But her health has worsened – she is now reliant on a mobility scooter and only leaves the house for medical appointments – and her attitude towards the profession she dedicated herself to has soured.
‘Jack should have been able to grow up, and I’ll always feel sorry he can’t. Every time I close my eyes he is with me,’ she says.
‘But I have suffered for my mistakes. I have been badly let down.’

