What Is Erythematous Mucosa?
FG Trade / Getty Images
Medically reviewed by Kumkum Sarkar Patel, MD
Erythematous mucosa refers to abnormal redness of the mucosa, the inner lining of your gastrointestinal (GI) tract, which runs from your mouth to your anus. The erythema (redness) is a sign that an underlying condition is causing inflammation and increased blood flow in part of your digestive tract.
Your gastrointestinal tract has four major regions: mouth, pharynx and esophagus, stomach, and small and large intestines (including the rectum and anus). Conditions causing inflammation in any of these regions can lead to erythematous mucosa, including stomatitis, esophagitis, gastritis, colitis, and proctitis.
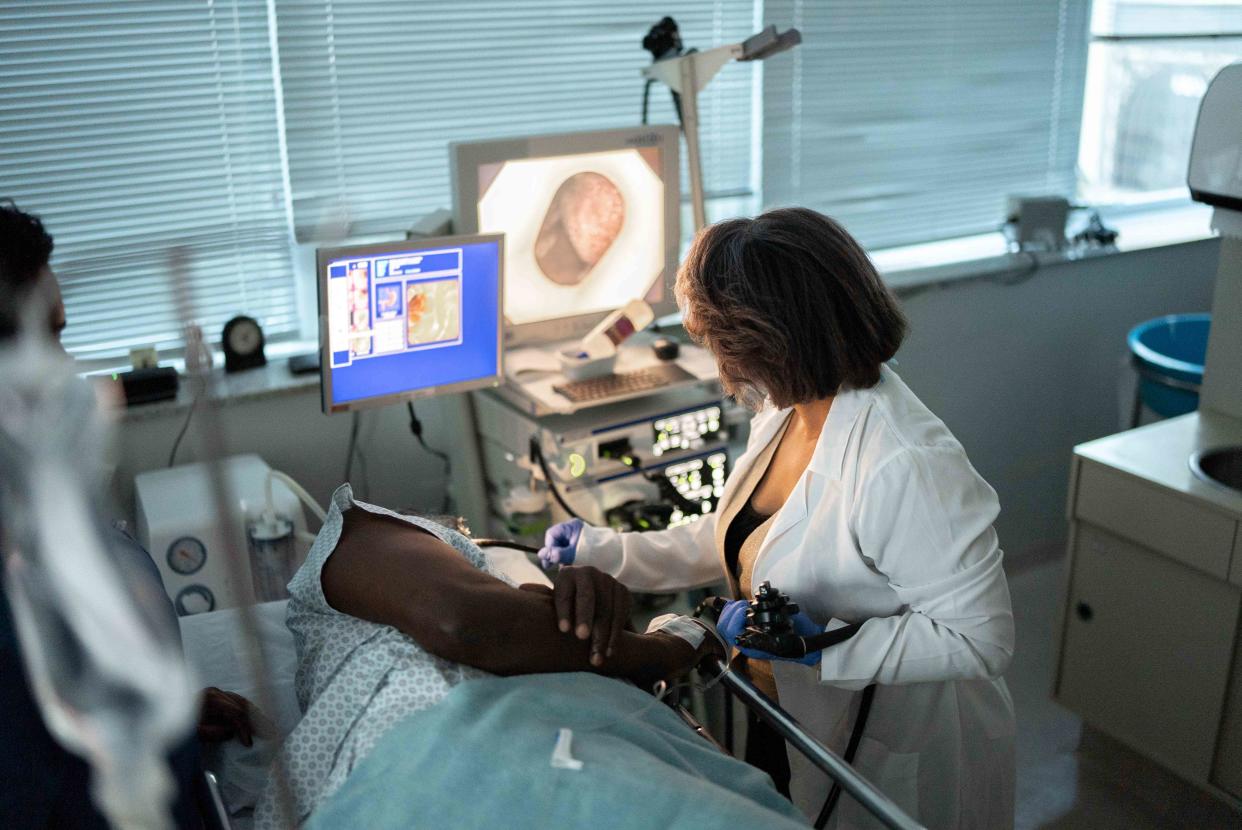
Healthcare providers often detect erythematous mucosa during an endoscopy, which uses a long, thin tube (endoscope) equipped with a camera to look inside the body. Symptoms and treatment options vary, depending on which part of your GI tract is affected.
Erythematous Mucosa Symptoms
Symptoms of erythematous mucosa vary depending on the specific location of the inflammation within your digestive tract.
Mouth (Stomatitis)
Stomatitis is inflammation of the mucosa (lining) of your mouth. Symptoms of stomatitis can affect your gums, inner cheeks, inner lips, or tongue and may include:
Pain or burning sensation in your mouth
Difficulty eating or drinking
Redness and swelling of your gums or tongue
Ulcers (sores) on your inner cheeks, gums, tongue, or inside of your lips
Esophagus (Esophagitis)
The esophagus is a tube that carries food from your mouth to your stomach. Esophagitis, or inflammation of the esophageal lining, may cause symptoms such as:
Cough
Sore throat
Difficulty or painful swallowing
Hoarseness (raspy or strained voice)
Stomach or Antrum (Gastritis)
Gastritis is inflammation in your stomach lining. It might occur in the corpus (central area), antrum (lower stomach), or entire stomach. Gastritis can cause symptoms such as:
Upper abdominal pain or discomfort
Nausea and vomiting
Loss of appetite
Black stools or vomiting blood (if inflammation causes bleeding in your stomach's lining)
Large Intestine (Colitis)
Colitis is inflammation of the lining of your colon (large intestine). Symptoms may include:
Abdominal cramping or pain
Bloating
Bloody stools
Diarrhea
Persistent urge to have a bowel movement
Rectum (Proctitis)
Proctitis is inflammation of your rectum, the second-to-last part of your digestive tract, right before your anus. It can cause symptoms like:
Rectal pain or discomfort, especially during bowel movements
Rectal bleeding
Bloody stools
Mucus or pus discharge from your rectum
What Causes Erythematous Mucosa?
Erythematous mucosa occurs when the inner lining of your digestive tract becomes irritated and inflamed. This inflammation increases blood flow to the affected area and disrupts the mucosa's normal functioning. The gastrointestinal mucosa has several functions, including:
Secreting mucus, digestive enzymes, and hormones to support digestion
Protecting against abrasion (e.g., scraping, damage) in your mouth and anus
Absorbing of nutrients from the foods you eat
Supporting your immune system by protecting against and clearing out foreign invaders like bacteria and viruses
Several factors can trigger inflammation in the gastrointestinal mucosa and cause erythematous mucosa. The specific cause of erythematous mucosa varies depending on the location of the inflammation.
Stomatitis Causes
Anything that causes inflammation in the lining of your mouth can lead to erythematous mucosa. The most common causes include:
Tobacco use (e.g., smoking, smokeless tobacco)
Viral infections, including herpes simplex virus (HSV) and herpes zoster (shingles)
Fungal infections, such as Candida albicans (thrush)
Allergic reactions or irritation from certain foods or chemicals
Esophagitis Causes
Inflammation of your esophageal lining can develop due to factors such as:
Smoking
Alcohol use
Vomiting
Lying down soon after a large meal
Recent surgery or radiation to the chest
Taking certain medications (e.g., doxycycline, potassium tablets) without drinking water
Fungal or viral infections, including Candida albicans (yeast) and herpes simplex virus (HSV)
Gastritis Causes
Inflammation of your stomach mucosal lining has many possible causes, including:
Excessive alcohol consumption
Helicobacter pylori (H. pylori) bacterial infection
Taking non-steroidal anti-inflammatory drugs (NSAIDs), such as Advil (ibuprofen) or Aleve (naproxen)
Autoimmune disorders (e.g., pernicious anemia, low red blood cell count caused by a vitamin B12 deficiency)
Cocaine use
Stress
Colitis Causes
In most cases, the causes of inflammation of your colon lining are unknown. Identifiable causes of colitis include:
Inflammatory bowel disease (IBD), such as Crohn's disease and ulcerative colitis
Food poisoning
Viral and parasitic intestinal infections
Clostridium difficile bacterial infection
Ischemic colitis (reduced blood flow to your colon)
Proctitis Causes
Inflammation of your rectum has many possible causes, including:
IBD
Sexually transmitted infections (STIs), including gonorrhea, chlamydia, and herpes
Radiation therapy to your pelvic region
Inserting harmful substances into your rectum
How Is Erythematous Mucosa Diagnosed?
Erythematous mucosa isn't a diagnosis. It's a sign of gastrointestinal tract inflammation due to an underlying condition affecting part of your digestive system. Your healthcare provider may detect redness of your gastrointestinal lining during an endoscopy when trying to determine the cause of your symptoms and provide an accurate diagnosis. They may also perform diagnostic tests.
Endoscopy
An endoscopy is a procedure that uses a thin tube equipped with a light and camera to visualize the inside of your digestive tract. There are different types of endoscopies, depending on the suspected location of inflammation and the source of your symptoms. Endoscopy types that help healthcare providers visualize the inside of the gastrointestinal tract include:
Anoscopy: Viewing the rectum and anus by inserting the endoscope through the anus
Colonoscopy: Viewing the entire length of the colon by inserting the endoscope through the anus
Esophagoscopy: Viewing the esophagus by inserting the endoscope through the mouth and throat
Gastroscopy: Viewing the stomach and duodenum (the top section of the small intestine) by inserting the endoscope through the mouth
Proctoscopy: Viewing the rectum by inserting the endoscope into the anus
Diagnostic Tests
To determine the underlying cause of erythematous mucosa, your healthcare provider will review your medical history, perform a physical examination, and order additional diagnostic tests (along with an endoscopy). These tests may include:
Blood tests: A complete blood count (CBC) and other blood tests can check for infections or anemia (low red blood cell count or hemoglobin) and measure inflammatory markers that may point to the cause of erythematous mucosa.
Stool test: A stool sample can help identify viral, bacterial, and parasitic gastrointestinal infections.
Biopsy: During an endoscopy, your healthcare provider may take a tissue sample from the affected area for further analysis under a microscope.
Barium swallow X-ray: Also known as an upper GI and small bowel series, this test involves drinking a milkshake-like drink (barium) before your healthcare provider takes a series of X-ray pictures to see how the barium fluid moves through your esophagus, stomach, and small intestine.
Treatments for Erythematous Mucosa
Erythematous mucosa treatment addresses the underlying cause to reduce inflammation and relieve symptoms. The treatment your healthcare provider recommends will depend on which part of the digestive tract is inflamed and your diagnosis (e.g., gastritis, stomatitis).
Stomatitis Treatments
Treatments for inflammation of the lining in your mouth help ease symptoms like pain and discomfort, making eating and drinking easier. Depending on the cause, treatment may include:
Anesthetics (pain relievers)
Oral rinses (e.g., "magic mouthwash") that help coat and numb the mouth for pain relief, such as lidocaine and sucralfate
Corticosteroids to reduce inflammation
Antifungal medications for fungal infections
Antiviral medications for viral infections
Esophagitis Treatments
Treatment for inflammation of the lining of the esophagus can include:
Acid-blocking medications (e.g., proton pump inhibitors) to reduce stomach acid
Antibiotics to treat bacterial infections
Oral (taken by mouth) corticosteroids to control inflammation
Medications that coat the lining of the esophagus to treat damage from swallowing pills without water
Dietary changes to avoid foods that trigger symptoms
Lifestyle modifications (e.g., avoiding smoking)
Gastritis Treatments
Treatments for stomach lining inflammation include:
Antibiotics to eradicate H. pylori bacterial infection
Medications to reduce stomach acid (e.g., antacids, H2 agonists, proton pump inhibitors)
Stopping medications that may cause or worsen gastritis symptoms, such as Advil (ibuprofen) or Aleve (naproxen)
Colitis Treatments
Treatments for colon lining inflammation vary widely depending on the underlying cause. Treatments may include:
Anti-inflammatory medications, such as corticosteroids
Immunosuppressants to regulate the immune system
Antibiotics to treat bacterial infections
Surgery, in severe cases
Proctitis Treatments
Healthcare providers make proctitis treatment decisions based on the cause. Treatments for inflammation in the rectum may include:
Antibiotics to treat bacterial infections
Antiviral drugs to treat viral infections
Anti-inflammatory drugs like corticosteroids to control inflammation
Immunosuppressant drugs to modulate the immune system
How To Prevent Erythematous Mucosa
There is no one-size-fits-all approach to preventing erythematous mucosa because there are many possible causes. Adopting certain lifestyle habits can protect your gastrointestinal health and lower your risk of conditions that contribute to inflammation in the digestive tract. This includes:
Focusing on a nutritious diet: A balanced diet rich in foods like fruits, vegetables, whole grains, and lean proteins provides your body with essential nutrients to support digestive and overall health. High-fiber, plant-based foods promote healthy gastrointestinal mucosa and reduce intestinal inflammation.
Managing stress: Chronic (long-term) stress can trigger or worsen digestive problems, leading to diarrhea, constipation, or inflammation. Relaxation techniques like meditation, yoga, or deep breathing exercises can help manage stress and lower your risk of gut inflammation.
Engaging in regular exercise: Exercise supports healthy digestive function and reduces systemic (whole-body) inflammation, which benefits your gut and overall health.
Avoiding smoking: Smoking can trigger or worsen intestinal inflammation. Quitting smoking reduces inflammation and lowers the risk of gastrointestinal disorders or symptom flare-ups in people with gastrointestinal disorders (e.g., IBD).
Complications
Untreated or chronic inflammation causing erythematous mucosa can lead to complications, such as:
Ulcers: Chronic inflammation can erode the mucosa (lining of the digestive tract) and cause painful, open sores called ulcers.
Nutrient deficiencies: Inflammation can impair your body's ability to absorb nutrients, leading to deficiencies in important nutrients like iron, zinc, and vitamins A, B, and D.
Bleeding: Over time, inflammation can cause bleeding in the gastrointestinal tract, which may lead to bloody stools or vomiting blood and blood loss, depending on the severity of the bleeding.
Strictures: Chronic inflammation can cause scarring and narrowing of the digestive tract, leading to bowel obstruction (difficulty passing stool).
Increased risk of certain cancers: Chronic inflammation in the gastrointestinal tract increases the risk of certain cancers. Gastritis increases the risk of stomach cancer, and IBD (e.g., Crohn's disease) increases the risk of colon cancer.
Early diagnosis and treatment of the underlying cause of erythematous mucosa can help lower your risk of developing complications.
A Quick Review
Erythematous mucosa isn't a diagnosis itself. It's a sign of inflammation in your digestive tract lining. It can affect any part of the digestive tract, from your mouth to your rectum. Depending on the location, inflammation can cause symptoms like pain, discomfort, and digestive challenges.
Infections, certain medications, and chronic (long-term) digestive conditions can cause erythematous mucosa. Treatment addresses the underlying cause and may involve medications, dietary changes, and lifestyle modifications.
Frequently Asked Questions
Is erythematous mucosa serious?
Erythematous mucosa is a sign of inflammation in your digestive tract. Possible causes range from mild, acute infections to more serious, chronic conditions. Your healthcare provider will order diagnostic tests to determine the cause and develop an appropriate treatment plan.
Can stress cause erythematous mucosa?
Stress can trigger inflammation in your gastrointestinal tract, contributing to erythematous mucosa and associated conditions, such as gastritis. It can also worsen symptoms of inflammatory digestive conditions, like ulcerative colitis.
Should you avoid any foods if you have erythematous mucosa?
Certain foods can trigger or worsen inflammation and erythematous mucosa. Depending on your diagnosis, your healthcare provider may recommend avoiding certain foods and beverages, including alcohol, high-fat or processed foods, sugary foods, and certain spices and seasonings, such as chili peppers.
For more Health.com news, make sure to sign up for our newsletter!
Read the original article on Health.com.

