Common Types of Nail Disease: How to Spot and Treat Each
Medically reviewed by Susan Bard, MD
There are many types of nail diseases. They can occur for a wide range of causes that can be acute (short-term) or chronic (long-lasting).
Nail diseases can cause physical changes in how your nails look and function. These changes can lead to feelings of self-consciousness and depression in severe cases.
Many nail diseases occur as a symptom of a body-wide problem. While some nail diseases can be treated with home care, some nail problems should be seen by a healthcare provider or podiatrist. Getting the right treatment as early as possible can improve your results.
This article describes some of the most common nail diseases, their causes, symptoms, and treatments. It also explains when to seek medical care.
Nail Psoriasis
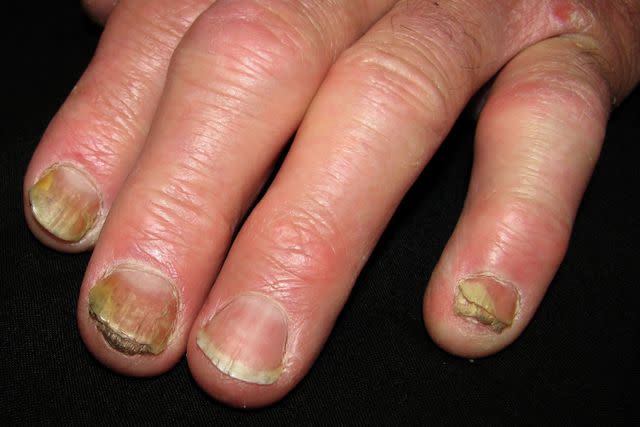
Reproduced with permission from ©DermNet NZ www.dermnetnz.org 2022
Nail psoriasis occurs when psoriasis affects your nails.
Causes
Nail psoriasis affects 90% of people with psoriasis at some point. Psoriasis is a chronic condition caused by dysfunction of the autoimmune system. As a result, the autoimmune system speeds up skin cell growth so fast that the cells do not have time to shed but accumulate as skin patches called plaques.
About half of all people with psoriasis have nail symptoms at their diagnosis. Nail psoriasis typically appears about 10 years after skin psoriasis. It can also occur without psoriasis and may be linked to other whole-body or skin diseases.
Symptoms
Since symptoms of nail psoriasis are visible and can reduce manual dexterity, nail psoriasis can severely impact your quality of life. Its association with psoriatic arthritis can also contribute to the functional decline that nail psoriasis causes.
Symptoms of nail psoriasis can appear on your fingernails and toenails, though the condition affects fingernails more often. More than one digit is typically affected. Symptoms include:
Pitting: Deep or shallow lines, ridges, dents, or dots in your nail
Deformation: Changes in the normal nail shape
Leukonychia: White spots within your nail plate
Thickening of the nail: There will also be build-up under your nail
Thinning and crumbling of the nail
Onycholysis: Separation of the nail from the nail bed
White, brown, or yellow discoloration
Blood under your nail
Treatment
Contact your healthcare provider if you have psoriasis and notice changes on your fingernails. Keeping your nails short and protecting them from damage can help prevent the condition from worsening.
Treatment involves prescribed therapies, though achieving results is a slow process. Treatments for nail psoriasis include:
Corticosteroid injections into, under, or near the nail
Systemic therapies, like disease-modifying anti-rheumatic drugs (DMARDs), Otrexup, Rasuvo, and others (methotrexate), Sandimmune (cyclosporine), Otezla (apremilast), Biologics, and Humira (adalimumab), Cosentyx (secukinumab)
Learn More: What Does Psoriasis Look Like?
Brittle Splitting Nails
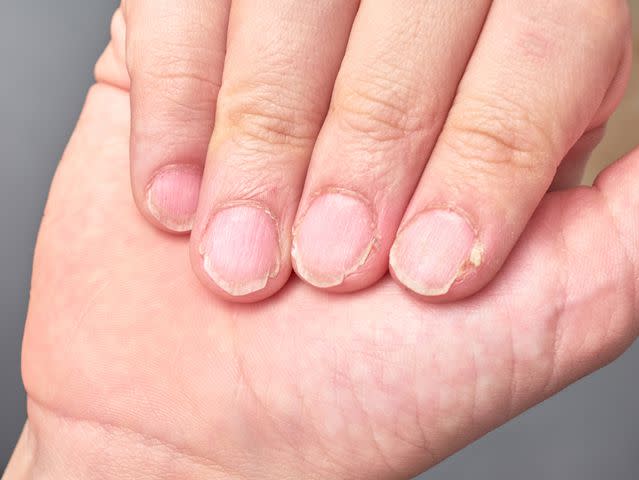
Carlos Andres / Getty Images
Brittle-splitting nails, or onychoschizia, have become thin, weak, and fragile.
Causes
While little information is known about the cause of onychoschizia, it is commonly linked to the following conditions:
Repeated wetting and drying of the fingernails
Excessive immersion in water with detergents
Recurrent application of nail polish
Frequent use of solvents to remove nail polish
Old age
Systemic (body-wide) diseases
Certain drugs
Polycythemia, which is a blood disorder that causes too many red blood cells
Symptoms
Onychoschizia causes horizontal splitting of the nail plates. The following changes to the nail can also occur:
Nails that split, flake, and crumble
Nails that become soft and lose elasticity
Longitudinal splitting
Shallow parallel furrows running on the superficial layer of the nail
Superficial granulation of keratin appearing as dry, white areas
Worn-down nails
Significant cosmetic and functional problems in performing daily or occupational activities
Pain from deep nail splitting and the nail catching on to things
Treatment
Brittle-splitting nails that occur secondary to a body-wide problem should involve treating the primary dermatological or systemic condition. Cure of the brittle nails typically requires the following strategies:
Limit contact with water and detergents
Regular use of emollients on the nail
The following treatments may also be effective:
Oral supplementation with biotin (a water-soluble vitamin)
Prolonged treatment with zinc in cases of zinc deficiency
Prolonged treatment with iron supplementation plus vitamin C
Nail moisturizers
Nail lacquers known as hail hardeners or nail strengtheners
Onychogryphosis
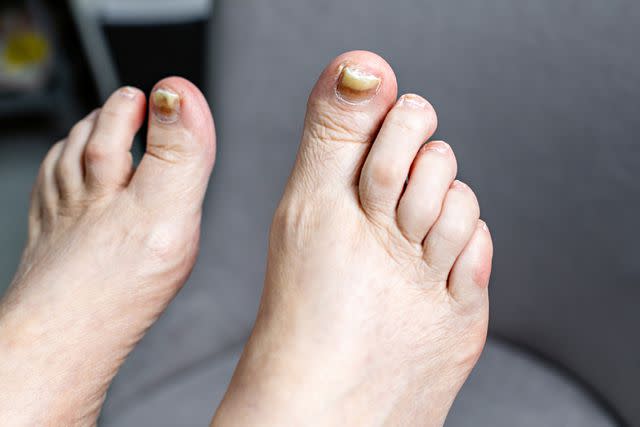
Ekaterina Rekina / Getty Images
Onychogryphosis, also called Ram’s horn nails, is a condition in which your nails become very thick, long, and curved.
Causes
While the exact cause of onychogryphosis is not known, it can be triggered by:
Trauma such as burn injuries or other nail injuries
Ichthyosis: a group of skin disorders that causes dry, scaly, or thick skin
Nail psoriasis
Nail bed deformities
Bony deformities like hallux valgus (bunion)
Nail fungal infections (onychomycosis)
Long-standing poor personal care or neglect
Impairment of peripheral circulation, such as varicose veins
Improperly fitting shoes or footgear
Symptoms
Symptoms of onychogryphosis typically affect the large toenail. They can include:
Distortion of the nail
Yellow-brownish color
Nail thickening
A nail plate that is skewed, grossly thickened, and partly curved like a ram's horn
Pain
Paronychia: a skin infection
Onychocryptosis (ingrown toenail)
Treatment
Treatment for onychogryphosis depends on the cause and comorbidities. The problem is typically handled with conservative treatments that include:
Avoiding excessive pressure on the nail bed
Wearing appropriate fitting shoes
Using electric drills for mechanical debridement with a dual-action nail nipper to maintain a reduction of nail plate thickness and length
Applying cryotherapy (the use of freezing temperatures to destroy abnormal cells) on the nails before trimming to make it easier to trim your nails with an even edge
Ingrown Toenails
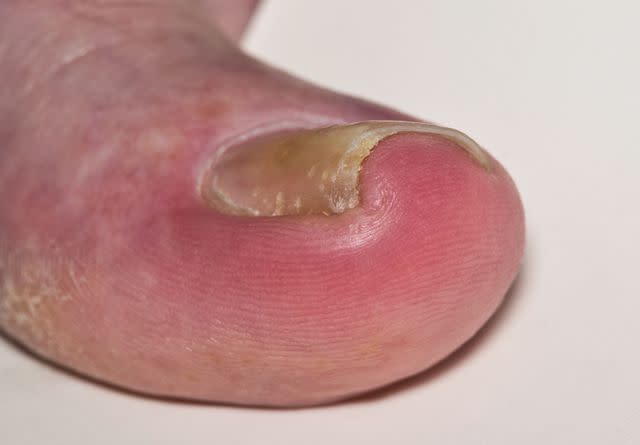
Brett_Hondow / Getty Images
An ingrown toenail, or onychocryptosis, occurs when your toenail grows into the skin surrounding it. The affected area can become painful and inflamed.
Causes
Causes of an ingrown toenail include:
A toenail that is cut too short
A toenail cut rounded at the edges, allowing it to grow into the skin
Shoes that are too tight
Sweaty feet
A genetic toenail shape called a "pincer" toenail is a nail deformity that causes over-curvature in the affected nail
Diabetes or other conditions that can cause water retention in your feet or chronic venous insufficiency in your legs
Medication to treat cancer
Repetitive activities like kicking a soccer ball
Symptoms
Symptoms of an ingrown toenail typically occur on your big toe, though it can happen on any toe. Symptoms include:
Pain
Redness
Swelling of the skin that surrounds the affected nail
Infection at the site
Weeping, blood, pus, or foul odor from the affected area, especially if infection occurs
Granulation tissue, which is a growth of new tissue over the ingrown toenail
Treatment
Contact your healthcare provider if you have a condition like diabetes, nerve problems in your leg or foot, any condition that causes poor circulation, or signs of a toenail infection. Do not attempt to treat the ingrown nail at home.
To treat an ingrown toenail at home:
Soak the foot in warm water three to four times daily.
Keep the foot dry during the rest of the day.
Wear sandals or comfortable shoes with adequate room for the toes until the problem resolves.
Use Motrin (ibuprofen) or Tylenol (acetaminophen) for pain relief.
Contact your healthcare provider or a podiatrist if you do not notice improvement in two to three days.
Depending on the severity of your ingrown toenail, your healthcare provider may use one or more of the following treatments:
Partial nail avulsion: surgery to remove part of the toenail
Gutter splints or braces to help guide the nail back to normal growth
You can help prevent the recurrence of an ingrown toenail by doing the following:
Cut your nails straight across with a clean, sharp nail trimmer. Avoid tapering or rounding the corners of your nails.
Protect your foot from trauma.
Wear shoes and socks with adequate room for your toes.
Keep your feet clean and dry as much as possible.
Learn More: How to Treat Your Ingrown Toenail
Fungal Nail Infections
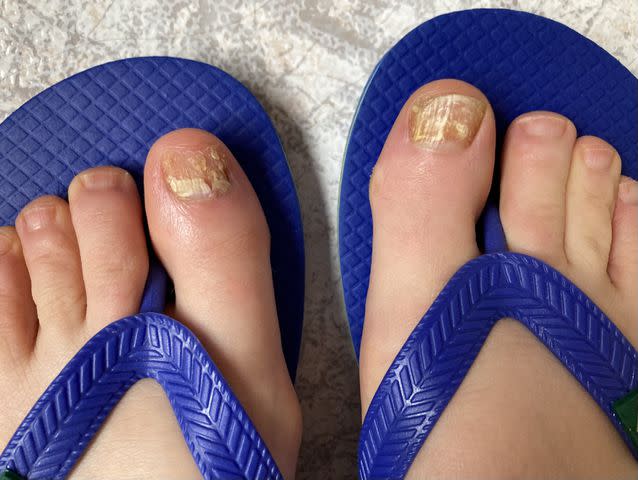
Nitya Dambiec / Getty Images
A fungal nail infection, also called onychomycosis or tinea unguium, is a fungal infection that occurs on your fingernails, toenails, or nail beds. For most people, the infection isn't a serious problem.
Causes:
Fungal nail infections are caused by tiny, microscopic organisms called fungi. These organisms thrive in warm, moist environments. You can pick up the fungi in the following ways:
Skin-to-skin contact with another person who has a fungal infection such as ringworm on their hands or athlete's foot on their feet
Walking barefoot in a warm, moist area such as a locker room, shower, or pool
Having moist feet or sweaty socks and shoes
Nail infections occur when the fungi invade your nail and then grow in the warm, moist environment under your nail. Fungi typically attack your nail via one of the following entry points:
A small cut in the skin around your nail
A crack in your nail
A separation between your nail and finger or toe
Symptoms
Symptoms of nail fungus develop slowly and include:
A progressive change in nail color to white, yellow, or brown
Thickening of the nail
Nail brittleness resulting in the nail crumbling, splitting, or separating from your skin
Pain when you walk, stand, or wear shoes for long periods
Treatment:
Contact your healthcare provider or a podiatrist if you notice any thickening, discoloration, or deformity in your nail. The earlier you start a toenail fungus treatment, the greater your chance of cleaning your nails and preventing it from spreading to other nails or other areas of your body.
You may be able to treat a mild fungal infection with home treatment that involves:
Cleaning your toenails regularly
Debriding or filing off white marks
Applying an over-the-counter (OTC) topical antifungal treatment
While at-home treatment can relieve symptoms, it does not eradicate the problem and will likely return. Your healthcare provider can prescribe one of the following treatments:
Topical toenail infection medications approved by the U.S. Food and Drug Administration (FDA):
Curanil, Loceryl, others (amorolfine)
Penlac, Loprox, others (ciclopirox)
Jublia (efinaconazole)
Rerydin (tavaborole)
Oral antifungal medications can be used for a laboratory-confirmed toenail fungus. They may be used in combination with topical treatment for difficult cases. The most commonly used treatment is an 8 to 12-week course of one of the following medications:
Lamisil (terbinafine)
Diflucan (fluconazole)
Grispeg, Fulvicin (griseofulvin)
Sporonox (itraconazole)
Nail removal
Nonsurgical nail removal using a chemical applied to your nail
Surgical nail removal of your nail
You can reduce your risk of having another nail fungal infection by taking the following precautions:
Wear flip-flops or shower sandals in warm, moist areas like gyms, locker rooms, public showers, and spas.
Discard any shoes, boots, or socks worn before you start treatment for a fungal infection.
Wear clean socks every day. Wash your socks when they get sweaty.
Keep your nails short.
Sanitize nail clippers with soap and water, followed by rubbing alcohol, before using them
Learn More: The 6 Best Toenail Fungus Treatments of 2024
Onycholysis
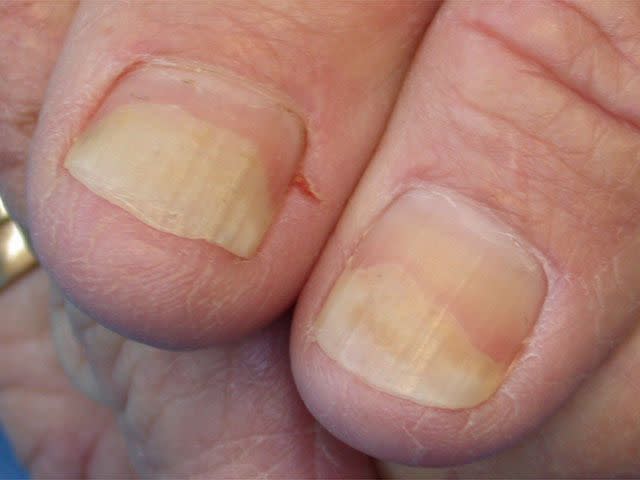
Reproduced with permission from © DermNet dermnetnz.org 2023
Onycholysis is when your nail plate separates from your nail bed.
Causes
Causes of onycholysis can include:
Nail fungal infection
Nail psoriasis
Pseudomonas: A bacterial infection common in people who frequently have their hands in water
Long fingernails that act as a lever to pull the nail away from your skin
Trauma or injury
Symptoms
Onycholysis can appear with one of the following symptoms:
Distal onycholysis: Nail plate separation begins at the far edge of the nail and proceeds down toward the cuticle (most common)
Proximal onycholysis: Nail plate separation starts in the cuticle area and continues up the nail
The disease often causes substantial distress, which can affect your quality of life and cause significant physical and occupational limitations.
Treatment
Onychomycosis is difficult to treat. The main goals of treatment include eradication of pathogens, restoration of healthy nails, and the prevention of recurrence. Based on your condition, your healthcare provider may use one of the following treatments:
Systemic therapies like Lamisil (terbinafine) andSporonox (itraconazole)
Topical antifungal therapies after removal of the unattached nail like Penlac, Loprox, Jublia (efinaconazole), and Kerydin (tavaborole)
Laser therapy
Paronychia
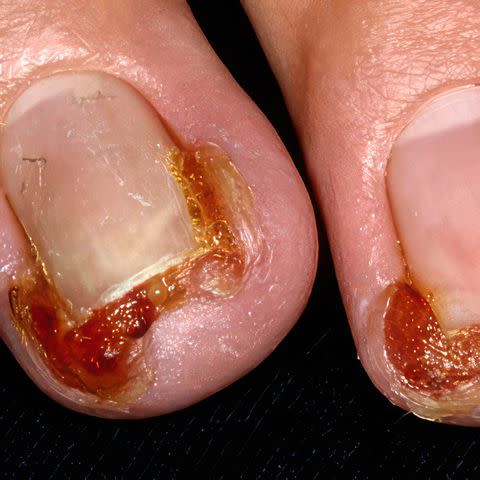
Reproduced with permission from © DermNet and © Raimo Suhonen dermnetnz.org 2023
Paronychia is an infection of the skin surrounding the nail known as the perionychium. The condition usually isn't serious.
Causes
Paronychia can occur as a result of injury, such as biting or picking a hangnail or trimming or pushing back your cuticle. The infection occurs as a result of the following:
Bacteria
Candida: a type of yeast
Other fungi
Exposure to water in jobs such as bartending or waitressing
Diabetes
Direct trauma to the nail
Symptoms
Symptoms of paronychia occur at the cuticle or the site of a hangnail or other injury. They can include:
Pain
Redness
Swelling
Pus-filled blisters
Nail changes in color or shape
Detachment of the nail
If the infection spreads to the rest of your body, symptoms may include:
General ill feeling
Fever, chills
Development of red streaks along your skin
Joint pain
Swelling of the lymph nodes in your elbow and armpit
Muscle pain
Treatment
Home treatment for paronychia involves the following treatment:
Soak your nail in warm water two or three times to reduce swelling and pain
Contact your healthcare provider if you have pus or an abscess (a pus-filled pimple). A portion of your nail may need to be removed. The type of treatment you receive depends on the cause of your infection. Your healthcare provider may advise one of the following:
For acute, bacteria-associated paronychia:
Biocef, Daxbia, and others (cephalexin)
Dicloxacillin
For chronic, antifungal paronychia:
Topical Nizoral, Kuric, and others (topical ketoconazole)
When to Contact a Healthcare Provider
Symptoms of common nail diseases can overlap and be difficult to identify. Getting an accurate diagnosis is important because some nail diseases can be a sign of systemic diseases that require medical care.
Contact your healthcare provider if your nail condition has any of the following symptoms:
Blue nails
Distorted or clubbed nails (enlargement of your fingertips and downward sloping of the nail)
Horizontal ridges in the nailbed
Pale nails
White lines
White color under your nails
Pits in your nails
Painful nails
Peeling nails
Ingrown nails
Contact your healthcare provider immediately if your nail disease has the following symptoms:
Brown-black pigmentation of the nail
Hemorrhages under your nail
Summary
Your nails can reflect a lot about your general health. Changes in nail color, strength, texture, and shape can be caused by a range of acute and chronic problems. These changes can also affect how your nails look and function, leading to frustration and sadness.
You can help prevent nail disease by keeping your nails clean and groomed. Avoid wearing tight-fitting shoes and sweaty socks that can create an ideal site for germs. Cut your nails straight to reduce your risk of giving germs access to your nails.
While you may be able to treat minor nail diseases at home, most should be examined by a healthcare provider. An accurate diagnosis can ensure you get the right treatment as early as possible. This can be key to finding and managing underlying diseases affecting other parts of your body.
Read the original article on Verywell Health.

