Cervical Cancer Is Deadlier Than We Thought — Especially in Black Women
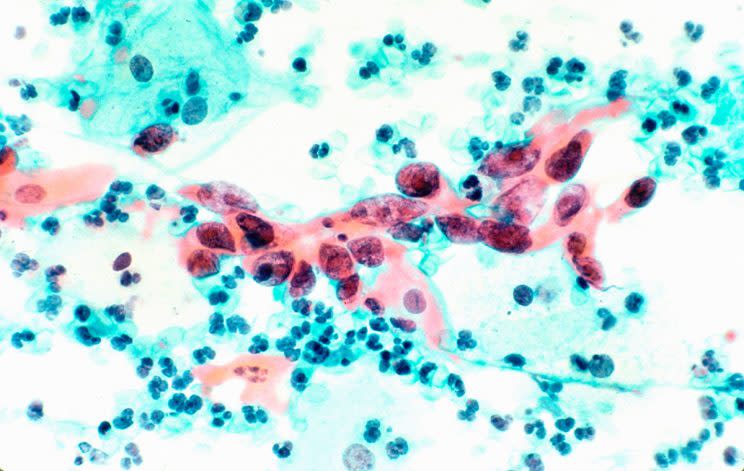
Cervical cancer is a highly preventable cancer that can turn deadly if it’s left undetected for too long — and a study published in the journal Cancer discovered that the death rate from cervical cancer is much higher than previous estimates.
The study analyzed data from the National Center for Health Statistics and, for the first time, adjusted for women who had had a hysterectomy, a procedure in which all or parts of the uterus are removed, including the cervix. Without a cervix, women cannot develop cervical cancer.
With the adjustment, the study’s researchers discovered that the death rate from cervical cancer dramatically jumped. For black women, the corrected mortality rate was 10.1 per 100,000 women (up from 5.7 per 100,000 women), and for white women, the corrected rate was 4.7 per 100,000 women (up from 3.2 per 100,000). “A correction for hysterectomy has revealed that cervical cancer mortality rates are underestimated, particularly in black women,” researchers wrote.
According to the Centers for Disease Control and Prevention (CDC), 11,955 women in the U.S. were diagnosed with cervical cancer in 2013 (the most recent year for which numbers are available), and 4,217 women died from the disease. Cervical cancer used to be the leading cause of cancer death for women in the U.S., the organization says. However, the number of cases has significantly declined in the past 40 years due to proper screening.
The main cause of cervical cancer is human papillomavirus (HPV), the most common sexually transmitted infection, the CDC states. Pap tests (also known as Pap smears) look for precancerous cells on a woman’s cervix that may develop cervical cancer if they’re not detected and treated properly, and the HPV test detects human papillomavirus; both tests are recommended by the CDC to help prevent cervical cancer.
The American Congress of Obstetricians and Gynecologists currently recommends that women receive a Pap smear every three years, but Lauren Streicher, M.D., an associate professor of clinical obstetrics and gynecology at Northwestern University Feinberg School of Medicine, tells Yahoo Beauty that many women don’t receive one at all, increasing the risk that they’ll develop cervical cancer that goes undetected until it’s too late. “People are just not being screened,” she says. “You only need a Pap test every three years, which turns into every 10 years for some women, which turns into not doing it at all.”
As for the discrepancy in risk due to race, Jessica Shepherd, M.D., an assistant professor of clinical obstetrics and gynecology and director of Minimally Invasive Gynecology at the University of Illinois College of Medicine at Chicago, tells Yahoo Beauty that it’s likely due to lack of access to care. “There’s a big difference in those who are insured and not insured, what type of education women get in cancer prevention and why Pap smears are so important,” she says. “Because of the lack of access to care, women are getting diagnosed with HPV — the leading cause of cervical cancer — later on rather than earlier, giving them an increased risk that it will progress into cervical cancer,” she says.
Shepherd stresses the importance of regular Pap smears for women, as well as follow-up care, if recommended. Women may require a biopsy if they have positive test results, she says, as well as other treatments that can lower the odds that their abnormal cervical cells will turn into cancer.
The HPV vaccine can also help prevent cervical cancer, Streicher points out, but it’s underutilized. (The CDC reports that in 2014, 40 percent of teen girls and 60 percent of teen boys had not received even one dose of the HPV vaccine.) “It blows my mind that we have a vaccine to prevent this cancer and there’s any question about getting the vaccine,” Streicher says.
Streicher stresses that cervical cancer is a preventable disease. “There should be no deaths from cervical cancer,” she says. “This is a travesty that this is happening.”
Related: I Was Diagnosed With Cervical Cancer Three Months After Giving Birth
Let’s keep in touch! Follow Yahoo Beauty on Facebook, Twitter, Instagram, and Pinterest.

