Steroid injections for osteoarthritis may not be safe
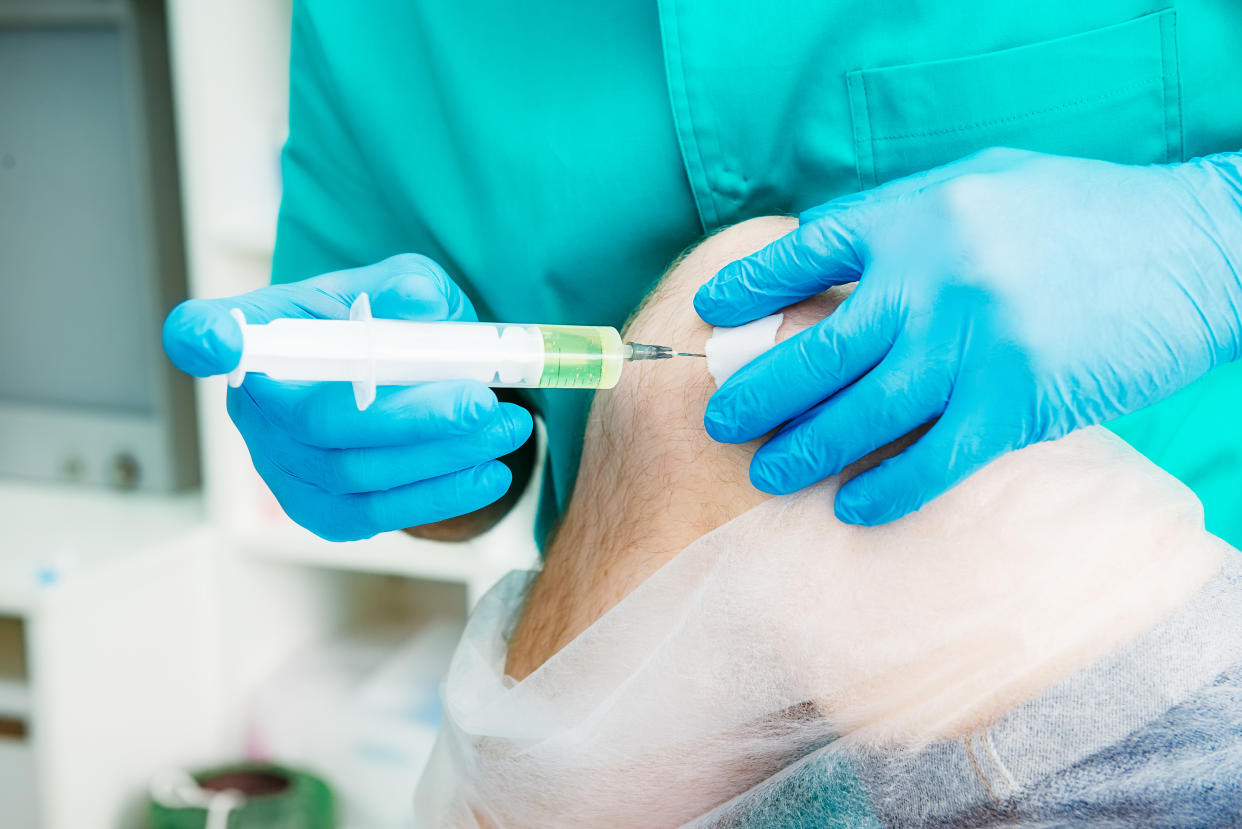
Steroid injections that relieve painful osteoarthritis (OA) may not be as safe as previously thought, research suggests.
Cortisone is often injected into the hip and knees of OA sufferers to ease aching joints. Athletes also rely on the jab to mask pain. However, studies have thrown up mixed results as to its safety.
In the new research, scientists from Boston University looked at 459 OA patients up to 15 months after they had the injection in their hips or knees.
The team found 10% of those who had cortisone put into their hips saw their symptoms, namely joint pain and stiffness, worsen. The jab also left them more at risk of fractures and joint degeneration.
Of those who had the injection in their knees, 4% suffered side effects.

“We've been telling patients: ‘Even if these injections don't relieve your pain, they're not going to hurt you,’” lead author Dr Ali Guermazi said. “But now we suspect this is not necessarily the case.
“We are now seeing these injections can be very harmful to the joints with serious complications.”
OA, or “wear-and-tear arthritis”, occurs when the cartilage in the joints breaks down, which commonly affects the elderly.
READ MORE: The diet that may help treat joint stiffness and pain
Nearly 9 million people in the UK suffer from OA, the NHS says. In the US, more than 30 million people have the disease, according to the Centers for Disease Control and Prevention.
Corticosteroid injections are recommended for those who do not get relief with painkillers. Studies into their safety, however, suggest they may trigger everything from joint swelling to back pain and infections.
To learn more, the scientists looked at OA patients who had between one and three corticosteroid injections last year. The patients came back two to 15 months later for a check-up.

Scans showed 6% of the patients had worse OA than before the injection, the scientists said in the research, published in the journal Radiology.
Some 0.6% were suffering a subchondral insufficiency fracture, which occurs when the bone is not strong enough to withstand day-to-day forces.
READ MORE: Arthritis sufferers can avoid disability with 'less than 10 minutes' of daily exercise
And 0.7% had joint destruction, including bone loss, with the same number of patients enduring “complications of osteonecrosis”, when bone tissue dies due to a lack of blood supply.
On the back of their results, the scientists are calling for scans to be carried out on patients before corticosteroid injections to ensure they have no existing fractures that may be made worse.
READ MORE: Arthritis diet tips: Include these foods in your diet to ease pain
“What we wanted to do with our paper is to tell physicians and patients to be careful, because these injections are likely not as safe as we thought,” Guermazi told The Telegraph.
“Physicians do not commonly tell patients about the possibility of joint collapse or subchondral insufficiency fractures that may lead to earlier total hip or knee replacement.
“This information should be part of the consent when you inject patients with intra-articular corticosteroids.”

