This Drug Can Help Monkeypox. But The FDA Makes It Hard to Get.
The government agency charged with helping Americans obtain treatment for monkeypox may once again be allowing red tape to stand between doctors and the treatment their patients need.
As the global monkeypox outbreak continues to grow across Europe and the United States, public health authorities have consistently been several steps behind an illness that has infected at least 5,000 Americans in the past three months. Now, with access to the nation’s vaccine supply finally loosened after months of bureaucratic back-and-forth kept hundreds of thousands of doses trapped overseas, epidemiologists, physicians, elected officials and advocates for LGBTQ communities say that red tape is still restricting their ability to actually treat the virus.
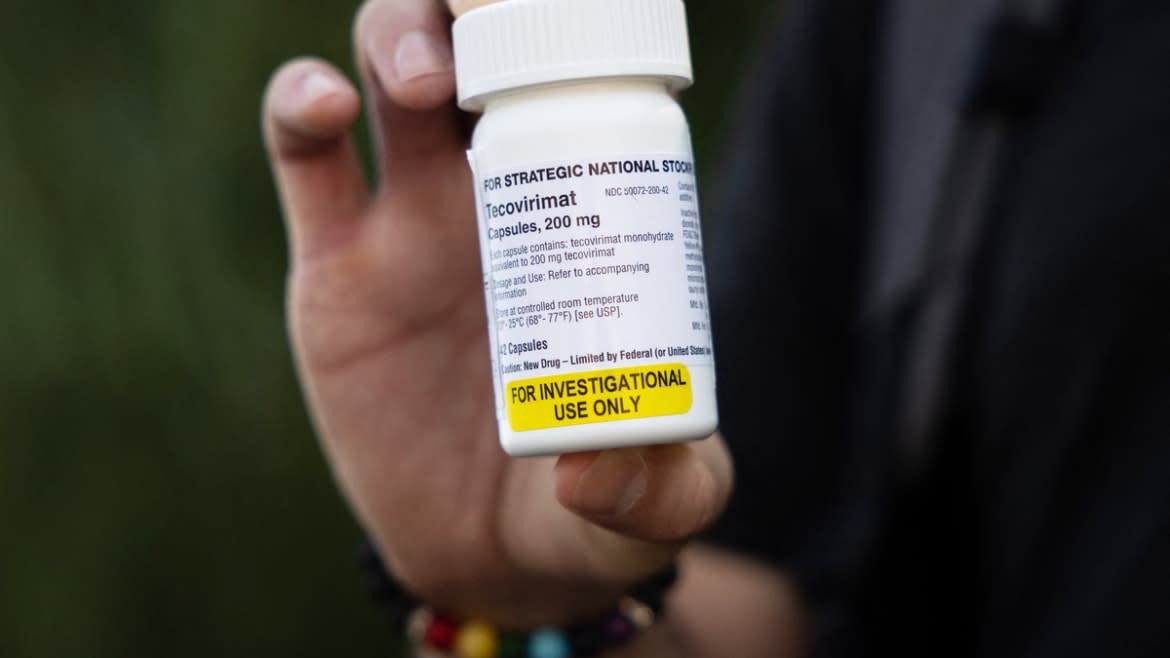
Tecovirimat—also known as TPOXX—an antiviral drug approved by the Food and Drug Administration four years ago for the treatment of smallpox, has quickly become one of the most important tools in treating monkeypox infections. The disease, which causes deeply painful blisters in addition to flu-like symptoms, is the same genus as smallpox, which has prompted physicians to prescribe it as an off-label treatment for severe cases.
But TPOXX was only approved to treat smallpox infections under animal studies rather than human trials, which are impossible to conduct, given its global extinction four decades ago. Without human trials for monkeypox, TPOXX’s use must be conducted only by doctors who are part of a hospital’s internal review board, each of whom is required to fill out dozens of pages of paperwork in order to secure TPOXX for their patients. With some cities seeing scores of new cases on a daily basis, doctors are facing an increasingly unmanageable patient backlog.
“Only certain individuals are allowed to do consent… that limits it to a small number of individuals,” said Dr. Timothy Brewer, a professor of epidemiology at UCLA's Fielding School of Public Health and of Medicine. “At UCLA, we’re trying to expand the number of people who have that authority, and I’m sure other institutions are as well, but that clearly is the limiting factor.”
The labyrinthine process requires physicians to submit reams of information to the Centers for Disease Control and Prevention, state or local health departments, or sometimes all three. Until recently, paperwork required clinicians and patients to fill out a half-dozen forms, as well as to schedule multiple examinations, collect and ship specimens to the CDC and to provide photos of monkeypox—a near-impossible request for patients with internal lesions.
“The requirements for prescribing this were incredibly onerous,” said Dr. Jay Varma, a professor of public health and director of Cornell University’s Center for Pandemic Prevention and Response.
World Health Organization Sounds Its Highest Alert Over Monkeypox
One week ago, CDC changed that process, allowing physicians to order the drug from the National Strategic Stockpile of medical supplies and begin treatment before submitting the paperwork. The number of forms was also reduced, and the required samples and lesion photos became optional. But continued enforcement of bureaucratic red tape by the Food and Drug Administration has blunted the changes, according to doctors, who are concerned that some providers may forgo prescribing TPOXX for all but the most serious cases rather than spend time sifting through paperwork.
“Some clinicians and hospitals may not elect to use Tecovirimat because of these requirements given that patients aren’t dying,” said Dr. Abraar Karan, an infectious disease researcher at Stanford University. “The antiviral could reduce suffering and may reduce duration of viral shedding, both important effects, so making it more accessible would be an important step.”
With the World Health Organization—as well as New York City and San Francisco—declaring monkeypox a public health emergency, public health advocates say that the Department of Health and Human Services is dragging its feet on doing the same, which they say would allow doctors and health authorities to sidestep some of those hurdles. An emergency use authorization for TPOXX, physicians propose, would allow clinicians who are not members of an internal review board to prescribe TPOXX, and would eliminate requirements for informed consent prior to use and post-prescription reporting by patients and doctors.
“It would allow clinicians to use this medication without the cumbersome barrier of putting together an IRB,” said Karan, who called the requirement “quite an involved process.”
“If a patient can get access, TPOXX is providing relief,” said David C. Harvey, executive director of the National Coalition of STD Directors. “We understand that TPOXX is an investigational drug, but in a public health emergency, the federal government should use every option at its disposal to cut red tape and make this drug immediately available to clinicians to treat their patients. It’s the right and moral thing to do.”
To go the ordinary route for an emergency use authorization, said said Dr. David Freedman, a professor emeritus of infectious diseases at the University of Alabama and an expert in tropical diseases, would require TPOXX’s manufacturer to submit “reams of clinical data in real patients of efficacy in real people infected with the pathogen.”
“FDA has specific guidelines for an investigational new drug application in general,” Freedman said. “These would have to be changed in terms of documentation required, and I doubt that would be a quick process for a 50-year-old way of doing things.”
Physicians have also suggested that doses of TPOXX could be preemptively shipped from the National Strategic Stockpile to regional stockpiles or local pharmacies in cities with high case numbers in order to expedite treatment.
“If every time you need a treat and dosage has to be released from the National Stockpile, that’s going to take more time and logistical hoops to jump through than if it were available at regional stockpiles, or, in the best-case scenario, at pharmacies and local pharmacies,” said Brewer. “Anything that delays getting the medicine, that is going to impact on its effect and on treatment.”
The Department of Health and Human Services’ continued resistance to declaring monkeypox a public health emergency is part of a pattern of government inaction on an illness that has almost entirely affected gay and bisexual men, community advocates told The Daily Beast. They point to White House press secretary Karine Jean-Pierre’s apparent unfamiliarity with TPOXX when asked about lack of access in a press briefing on Wednesday, as well as HHS Secretary Xavier Becerra’s flippant response to a reporter on Thursday when asked if there was still a chance of preventing the illness from becoming endemic in the United States, a moment that some epidemiologists fear has already passed.
On a press call I asked @SecBecerra if he believed it was possible to end the monkeypox outbreak or if the virus would become endemic.
He replied: "Well, I almost turn that question back to you, Ariel and asked, how many vaccines do you think we need at this stage?"
...— Ariel Cohen (@ArielCohen37) July 28, 2022
“Yet again, the FDA and their boss, HHS Secretary Xavier Becerra, seem to be living in la-la land,” said Michael Donnelly, a data scientist and a prominent critic of the public health response to monkeypox. “Listen: We ALREADY have a drug, TPOXX, that is highly effective at limiting symptoms and shortening disease duration. We ALREADY have supplies for well over a million doses. The European Medicines Agency has ALREADY approved it for treating monkeypox. And yet, the FDA refuses to approve it to treat people in the U.S. for monkeypox, even though they have ALREADY approved it for treating smallpox!”
“Hasn’t the FDA ALREADY screwed up enough for one crisis?!” Donnelly vented.
An HHS official, asked about plans to potentially follow the WHO in declaring monkeypox a public health emergency, or whether it was considering issuing an emergency use authorization for TPOXX, noted that an emergency use authorization for any medication would require the declaration of a public health emergency.
Some doctors defended the government’s more recent response to the monkeypox outbreak, noting that until recently, no public health authority in the world could have expected the virus—which has historically been almost entirely restricted to children in Central and West Africa—to become this widespread.
“I understand the frustration, but in general, I think the government, public health agencies and the FDA have done an excellent job of trying to move things along,” said Brewer. “These are big bureaucratic systems and it’s hard to to move them, but I think, given that recognition, I actually would say, gee, we’re three months into it and we already have drugs available that you can get access to, we have two vaccines, potentially, we could use.”
But the early missteps in addressing the outbreak, public health experts told The Daily Beast, echo the worst days of the coronavirus pandemic.
“The nation’s use of TPOXX as a monkeypox therapy has been chaotic and bureaucratic,” said Lawrence Gostin, director of the O’Neill Institute for National and Global Health Law at Georgetown Law Center. “The U.S. is now repeating the catalog of missteps we took during COVID-19 in terms of accessing vaccines and therapeutics for monkeypox.”
For the United States, which was perhaps best prepared of any nation to address a monkeypox outbreak, Varma said, the mistakes should have been entirely avoidable.
“In the month of May, there was a very clear, albeit narrow, window to mobilize everything that the U.S. government has available for monkeypox—and the U.S. had more than any other country on Earth,” Varma said. “It had tests, it had vaccines, it had a drug, and it had pretty good epidemiology clinical data that have been funded by the U.S. government over the years.”
“Things have moved much better in the month of July—we just really should have seen this level of action back in May, not now.”
Get the Daily Beast's biggest scoops and scandals delivered right to your inbox. Sign up now.
Stay informed and gain unlimited access to the Daily Beast's unmatched reporting. Subscribe now.

