New models indicate COVID-19 is declining in Canada, but we aren't in the clear yet, PM warns

The latest modelling data on COVID-19 in Canada is encouraging, showing the country is continuing to make progress, with a low in many communities, with the ability to trace where they came from.
“That’s an encouraging sign that the virus is slowing, and in places even stopping. But I want to be clear, we are not out of the woods, the pandemic is still threatening the health and safety of Canadians,” Trudeau urged Canadians.
The projected short-term epidemic trajectory, which uses actual case data, estimates Canada could see between 97,990 to 107,454 cases by June 15.
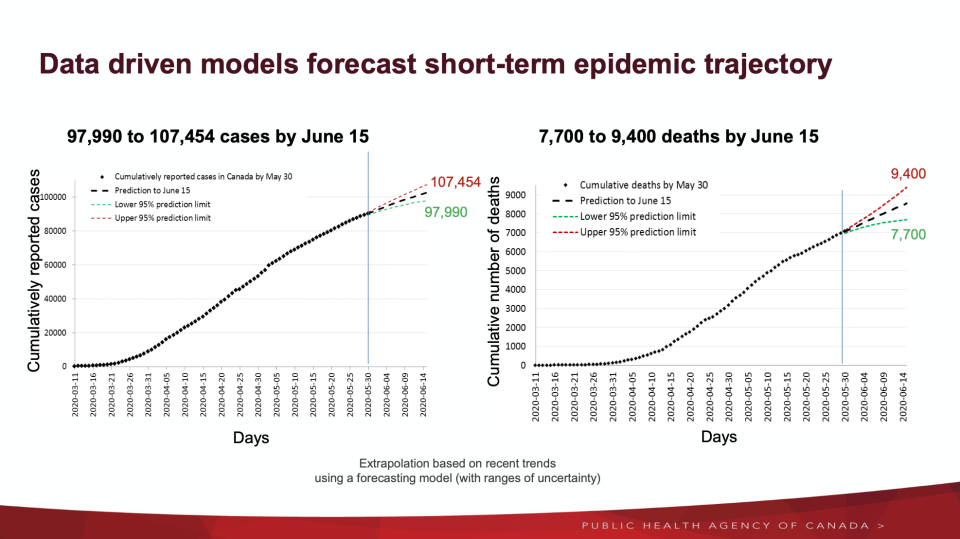
It also shows the country could see between 7,700 to 9,400 COVID-19 deaths by the same date.
The second wave still looms
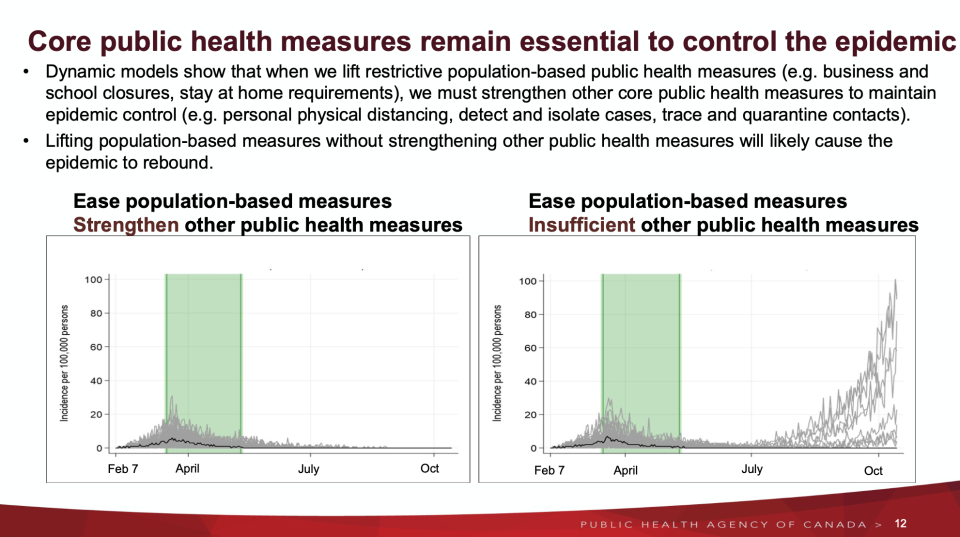
The dynamic models presented show as exiting restrictions are lifted, core public health measures must be maintained in order to prevent a surge in COVID-19 cases in the fall, until a vaccine is widely available. These core measures include personal physical distancing, detection and isolation of cases, and tracing and isolating contacts.
“At the end of the day, it all depends on what Canadians do across the country,” Dr. Howard Njoo, Canadian deputy chief public health officer said. “If we do that as a country then I think we’re in a good shape and not going to have this resurgence of cases in the fall.”
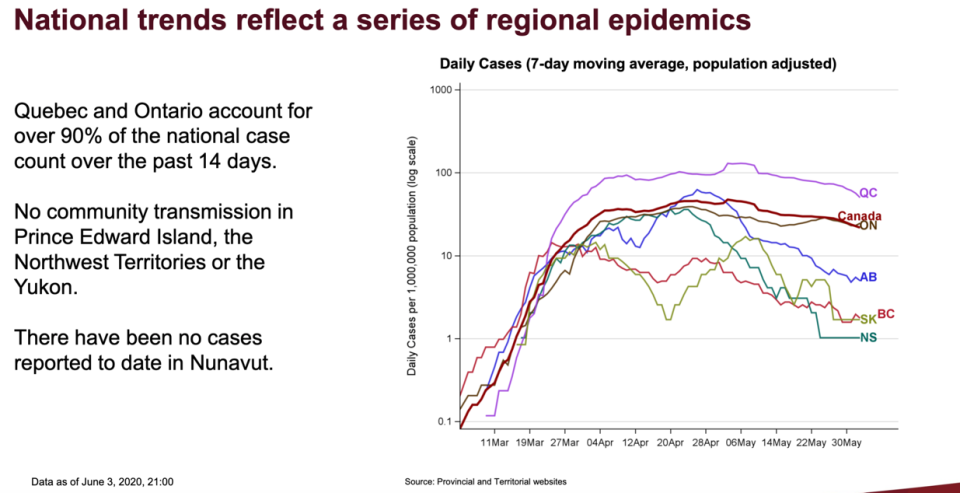
Dr. Theresa Tam, Canada's chief public health officer, stressed the country is seeing “regional epidemics,” with 90 per cent of cases over the last 14 days coming from Ontario and Quebec, primarily in and around Toronto and Montreal.
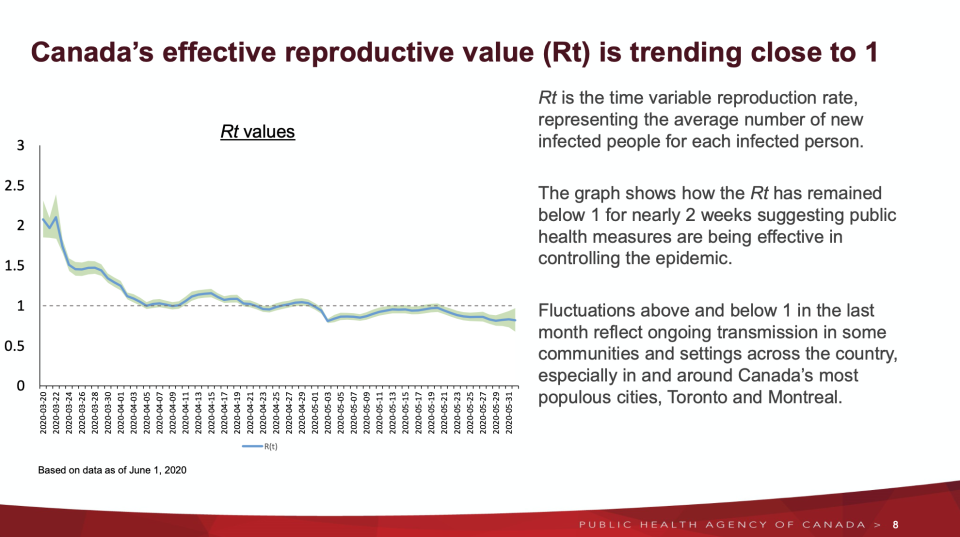
The effective reproduction number (Rt) nationally has remained under one for nearly two weeks. Federal health officials have indicated any increases in this rate over the past month has largely been driven by ongoing transmission around Toronto and Montreal.
“We will need to keep Rt consistently below one for more than three weeks before we can be sure that our public health measures are effectively controlling the pandemic,” Dr. Tam said.

Aside from regional differences in the COVID-19 pandemic in Canada, there are a number of more specific communities that have been identified more vulnerable to the virus.
“COVID-19 has exploited social and economic vulnerabilities, and inequality,” Dr. Tam said.
She went on to say there is a disproportionate number of cases in overcrowded areas, communities with lower incomes and health disparities. Crowded spaces can lead to what Dr. Tam called “larger cluster” or “super spreading” events.
Canada’s chief public health officer said although national information on ethnic specific data is not available at this point, the outbreaks that have been present to date have shown links with racialized populations and communities with more crowded living spaces.
“The outbreaks themselves, when we looked at them, points to the fact that a lot of the workers who support long-term care, who work at some of the workplaces like the meatpacking plants, are in those populations who are in a lower socioeconomic spectrum,” Dr. Tam said. “They have more crowded housing and they are in some of the racialized populations. We can tell that there’s a disproportionate impact.”


