Norovirus, aka stomach flu, on the rise in the US: Know these signs
Norovirus, a highly contagious stomach bug that causes diarrhea and vomiting, is on the rise across the United States. Also known as the "stomach flu" or winter vomiting bug, norovirus is very common and spreads easily from person to person.
Noroviruses are a group of viruses that cause acute gastroenteritis, or an inflammation of the lining of the stomach and intestines, which leads to nausea, vomiting, diarrhea and stomach cramps. Symptoms are often severe and start suddenly. If you’ve ever had norovirus, you know how miserable it can be.
Anyone can get infected with norovirus, and it spreads year-round, but outbreaks are most common during the colder winter months.
A recent outbreak of norovirus in North Carolina made headlines when more than 240 people complained of illness after dining at a sushi restaurant in Raleigh. The Wake County Health Department confirmed three cases of norovirus linked to the local restaurant, according to a statement.
Last month, health officials in Evanston, Illinois, also investigated a norovirus outbreak connected to a dollar-burrito event for students at Northwestern University, NBC Chicago reported.
Unlike its nickname suggests, norovirus is not related to the flu, which is caused by influenza viruses.
Annually, norovirus causes 19 to 21 million cases of vomiting and diarrhea in the U.S., 465,000 emergency room visits, 109,000 hospitalizations, and 900 deaths, per the CDC.
Last winter, cases and outbreaks surged in the U.S., peaking in March 2023, and norovirus activity remained high well into the late spring. After a summer lull, cases are expected to keep rising.
England also had an exceptionally severe norovirus season this past winter. In March 2023, cases soared to the highest levels seen in over a decade, according to the U.K. Health Security Agency.
What’s more, norovirus outbreaks on cruise ships spiked in 2023, reaching the highest levels seen in 11 years. Between January and June 2023, there were 13 confirmed norovirus outbreaks on U.S. cruise ships — that’s more outbreaks in six months than there have been during any full year since 2012, according to CDC data.
The 2023–2024 norovirus season is already underway, and cases are ramping up in most parts of the country as temperatures drop.
According to the most recent data from the CDC, the rate of norovirus tests coming back positive, averaged over three weeks, was nearly 13% as of Dec. 30. This is down from a peak of 17% in March but more than double the rate in September and October. During this time of year in 2022, less than 10% of tests were coming back positive.
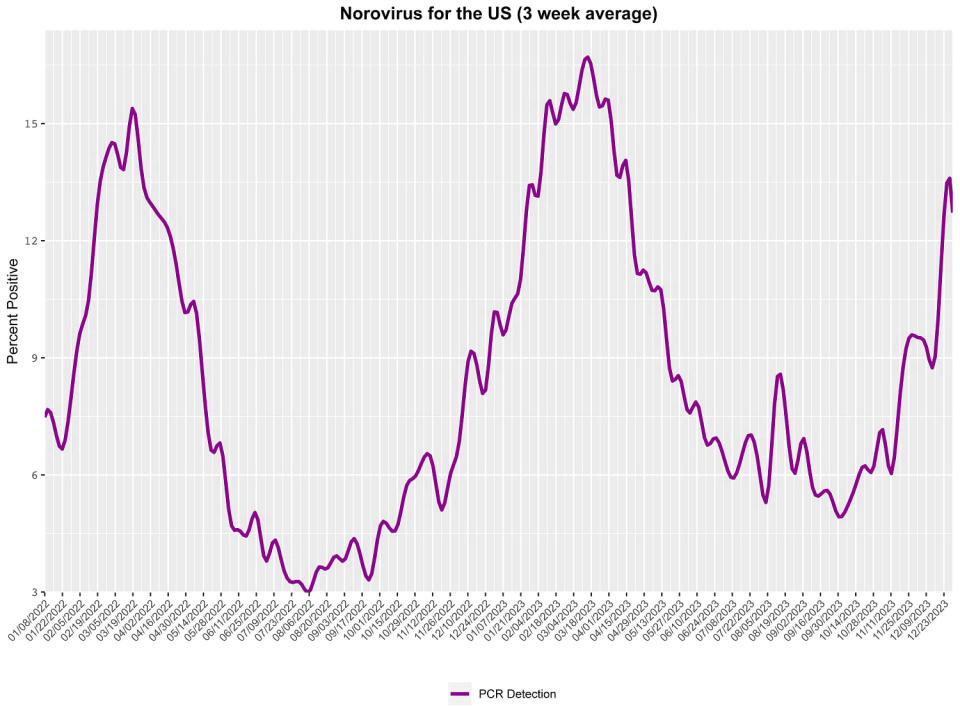
Will norovirus surge again this winter?
Norovirus is expected rise across the U.S. through the end of 2023 and early 2024 because it has a wintertime seasonality in the U.S., Kate Grusich, CDC spokesperson, tells TODAY.com. In temperate climates, activity tends to peak during the colder winter months.
Historically, the vast majority of outbreaks have occurred between November and April, according to the CDC.
While other intestinal viruses are more common in the summer, norovirus is known as the "winter vomiting disease," Dr. William Schaffner, professor of infectious diseases at Vanderbilt University Medical Center, tells TODAY.com.
As the holiday season approaches, there will be an uptick in indoor gatherings and travel — which can unfortunately spread germs like norovirus as well, says Grusich.
We can expect norovirus to sweep the country in the coming months, but it's too early to tell whether norovirus will surge like it did last winter or surpass the previous season's peak.
While it’s unclear how severe the upcoming 2023-2024 season will be, understanding why norovirus spiked last winter may offer clues into what we can expect this winter.
Why did norovirus surge in early 2023?
During the initial months of the COVID-19 pandemic, norovirus outbreaks plummeted to unusually low levels, per the CDC, and rates remained relatively low until the 2021-22 season. Prevention measures implemented to curb COVID-19 were likely effective in preventing norovirus outbreaks as well, says Grusich.
During 2022-2023 season, cases began ramping up in December and surged in the first few months of 2023. Dr. Ali Alhassani, a pediatrician at Boston Children’s Hospital and head of clinical at Summer Health, told TODAY.com in February that norovirus cases at the time were going up “quickly” and it started “pretty suddenly.”
CDC data show that norovirus cases peaked between February and March of 2023. Norovirus activity remained high in the U.S. through the late spring, causing numerous outbreaks in schools.
In June, Dr. Luis Ostrosky, an infectious disease specialist at UTHealth Houston and Memorial Hermann in Houston, told TODAY.com that “it’s not unusual to be see (norovirus) cases in April and May, (and) we are continuing to see many cases.”
Ostrosky also told TODAY.com back in February that in 2023 “norovirus activity (was) higher and earlier than usual, but definitely not a big outlier compared to pre-pandemic levels.”
One CDC chart shows that the highest number of outbreaks (106) reported per week during the 2021-2023 seasonal years was higher than the peak number of outbreaks (92) reported per week through the 2012-20 seasonal years.
One possible reason for the surge in 2023, according to experts, is that many children who evaded the stomach bug over the past few years were exposed to norovirus and other viruses that tend to circulate among schools in the winter and early spring.
"We've always had seasonal increases and waves of norovirus, and our hospitals would be filled with kids," Dr. Albert Ko, infectious disease physician and professor of public health, epidemiology and medicine at Yale School of Public Health, tells TODAY.com. "What kind of took us off was the pandemic," Ko adds.
Now that pandemic restrictions have relaxed and many children and adults have given up measures like distancing or masking, the number of norovirus outbreaks has returned to levels similar to pre-pandemic years, the experts note.
The post-pandemic tourism boom may have also played a role. As travel increases, travel-related illnesses are expected to surge, as well, said Ostrosky. “I think our travel frenzy after COVID is partially fueling this continued spread (of norovirus),” he added.
"I think ... post-COVID ... there may have been a bit more (norovirus) infections, just as there has been with many other (viruses) now that people are behaving in a pre-COVID manner," says Schaffner.
How does norovirus spread?
Norovirus is highly contagious and it only takes a few virus particles to cause infection.
It is spread primarily through the fecal-oral route or "when bacteria or viruses shed in stool ends up on our hands and surfaces then eventually ends up in our mouth and we ingest it and get infected," said Alhassani.
Norovirus may be transmitted directly from an infected person or indirectly through contaminated surfaces, objects, foods or drinks.
"Anybody who is in close contact with someone who has an active infection with norovirus is at high risk of getting it," said Alhassani. Norovirus can spread through activities like caring for an infected person, changing diapers or sharing utensils.
"Norovirus is so infectious that even if somebody throws up and there's droplets of vomit aerosolized in the air, that can actually cause infection," Alhassani added.
It takes a very small number of virus particles to transmit the disease, said Ko, which is why norovirus causes so many explosive outbreaks. Per the CDC, less than 100 norovirus particles can make you sick, and infected people typically shed billions of particles.
Most people are infectious from the time symptoms begin until about two or three days after symptoms resolve, Ko said, but some people can remain contagious or up to two weeks after recovery.
Outbreaks often occur in congregate settings such as schools, day cares, health care settings, nursing homes and cruise ships, says Schaffner.
What are the symptoms of norovirus?
According to the experts, the most common signs and symptoms of norovirus include:
Vomiting
Diarrhea
Nausea
Stomach pain or cramps
Other possible symptoms include a headache, body aches and a low-grade fever, says Ko. Norovirus symptoms usually develop within 12 to 48 hours after exposure, per the CDC.
"Norovirus ... will just last a few days," said Ostrosky. "For the majority of the population, it’s going to be just a nuisance."
Those at higher risk of developing severe or prolonged symptoms include babies, the elderly and the immunocompromised, said Ostrosky. If symptoms transition into chronic diarrhea and weight loss, this can lead to complications like dehydration or poor absorption of medications, he added.
What is the treatment for norovirus?
"There's actually no specific treatment or antiviral for norovirus," said Ostrosky. Hydration is key to replenish fluids lost from vomiting and diarrhea, the experts noted, which means drinking plenty of water, Pedialyte or sports drinks.
"Then it's just eating bland foods and trying to let it pass through the body, which usually takes like one to three days," said Alhassani, adding that over-the-counter anti-nausea medicine and pain relievers may also be used to ease symptoms.
“The vast majority of people can be managed at home and, in fact, should be isolated at home until they’re improving, given how contagious norovirus can be,” said Ostrosky.
However, it's important to watch for signs of severe dehydration and to contact a health care provider if these occur, the experts noted. These include dry mouth, decreased urination, dizziness and, in children specifically, crying without tears, fussiness or unusual sleepiness, per the CDC.
Children under the age of 1, immunocompromised people, and those with prolonged or severe symptoms should also be seen by a physician, said Alhassani.
A person can be infected with norovirus multiple times in their lifetime. After recovering, you may possibly develop some short-term immunity, said Ko, but it won't be robust and wanes quickly.
“It's only partial immunity ... because there are different types of norovirus, and being exposed to one doesn’t give you complete protection to another,” he explained.
To prevent norovirus infection, don't make this mistake
"We do not have a vaccine against norovirus yet, although there are scientists trying to create a norovirus vaccine but that's down the road," says Schaffner. However, there are steps you can take to prevent infection and transmission.
Hand hygiene is extremely important — but the way you clean your hands matters, Ostrosky noted, and it has to be with soap and water. Hand sanitizer does not work against norovirus.
“Norovirus is one of the few viruses that doesn’t get deactivated by alcohol. You actually need to use soap and water to physically destroy it and remove it from your hands,” said Ostrosky.
Wash your hands after using the restroom, before eating or cooking and after caring for someone with norovirus.
"Good hand-washing is really important for everyone, especially for people who handle food or are around children, older adults, or people with weakened immune systems," says Grusich.
When cleaning surfaces or objects that may be contaminated with norovirus, Ostrosky suggested using a high-level disinfectant like bleach.
If you or your child are sick with norovirus, isolate to prevent the virus from spreading within the household, said Alhassani. Anyone sick with norovirus should stay home until they feel better. Added Grusich: “Avoid food preparation until at least 48 hours after symptoms stop.”
It's also important to continue washing your hands often even after you feel better.
"We can expect to continue seeing more viral illnesses, both respiratory and gastrointestinal, in this post-COVID era we're sort of approaching," said Ostrosky, adding that the basics of hand-washing, isolation and respiratory etiquette can go a long way.
This article was originally published on TODAY.com

