The Cuban Health Paradox

A newborn rests beside his mother’s bed at the Ana Betancourt de Mora Hospital in Camagüey. The World Health Organization on Tuesday declared Cuba the first country in the world to eliminate the transmission of HIV and syphilis from mother to child. (Photo: Alexandre Meneghini/Reuters)
How did a country that can’t provide soap or bedsheets to its hospitals manage to achieve first-world life expectancies? And what, if anything can we learn from it?
Back in 2002, when dengue fever was detected in the Cuban capital, a public health protocol that had been created decades earlier was launched into action. At the behest of their government, average citizens took leaves from work and school and formed brigades that went door to door, repairing water leaks and disposing of waste to control mosquitoes. Construction workers and college students were trained in the basics of vector control and teamed up to fumigate public spaces and treat sewer systems. And schoolchildren tackled their own neighborhoods with a vengeance, searching beneath sinks, in basements and around house after house for standing water. In all, some 11,000 people were mobilized, more than 173,000 housing units fumigated and nearly 46,000 cubic meters of waste collected. The island did not completely conquer dengue, which continues to pose a threat there today. But it did avert a full-scale epidemic, even as several of its wealthier neighbors did not.

To prevent dengue, Cuban health ministry workers fumigate the entrance of an old building in Havana’s “Habana Vieja” neighborhood. (Photo: Jose Goitia/AP)
A dozen years later, Cuba is still pioneering boots-on-the-ground, low-cost health care solutions — now with a pennies-per-dose cholera vaccine that the beleaguered country created all by itself and that has the potential to stymie cholera’s spread throughout Latin America. Cuba also sent more doctors than any other country to fight the Ebola epidemic in Africa last year, a gesture for which U.S. Secretary of State John Kerry praised the country directly. But the dengue campaign highlights what many researchers agree is Cuba’s most significant achievement — a public health program so comprehensive it actively involves every member of society.
Much has been made in recent years of what public health and policy experts call the Cuban Health Paradox. Despite its third-world economy, the country has managed to achieve some first-world health indices — namely, a life expectancy (officially, 78 years) that matches that of the U.S., and an infant mortality rate (4.63 deaths per 1,000 live births) that’s slightly better than the States’. It has also achieved one of the highest doctor-to-patient ratios in the world and established a legitimate pharmaceutical sector, producing a suite of urgently needed drugs and vaccines — not only an affordable inoculation against cholera, but also the world’s only one against hepatitis C — and several effective chemotherapy and hypertension drugs.
At the same time, however, health care in Cuba is actually abysmal. The island may be producing some novel pharmaceuticals, and its doctors have indeed become first responders to all manner of global catastrophes. But its own clinics are woefully short of basic supplies, from aspirin and antibiotics to soap, bedsheets and latex gloves. And they’re so understaffed that Cubans themselves often joke that if you want to see a Cuban doctor, you should go to Venezuela. Castro has sent thousands of doctors there and to other developing countries, not only as a humanitarian gesture but in exchange for oil, cash and, in some cases, depending on whom you talk to, a public relations boost.
For all the debate, though, the biggest question of all may be how these disparities came to inhabit the same small island in the first place, and what, if anything, the rest of the world can learn from it.
*****
Let’s start with a quick history lesson. It’s no stretch to say the revolution that put Castro in power was at least partly over health care. Life expectancy was already on an upward trajectory by then, largely thanks to infrastructure projects launched in the late 1800s that helped curb vector-borne diseases. But while rich city-dwellers were living longer and staying healthier, the vast majority of people, living in the countryside, were still poor and struggling against tuberculosis and other infectious diseases.

Fidel Castro near a housing project in Jibacoa, May 13, 1975. The Castro regime installed a health clinic in every neighborhood. (Photo: AP)
Castro’s regime addressed this inequality head-on. The “human right to health care,” and the government’s responsibility to provide it free of charge, were both explicitly detailed in the new constitution. And in time, a three-tiered health care system was established, devoted almost exclusively to primary, preventive health care.
The root of this system was the consultario, or primary health clinic. Every neighborhood in Cuba has one, and in the beginning at least, each consultario was staffed by a doctor and nurse who lived on the premises and were responsible for 120 or so families (fewer in the countryside). This responsibility included much more than just treating patients who turned up at the clinic. It meant being proactive: visiting people at home, making sure that everyone got an annual checkup and making doubly sure that they were educated in basic health matters. Each consultario was linked to a polyclinic where more specialized care was provided. And all of the polyclinics were linked to the national ministry, which coordinated various health campaigns, collected data from the population and held doctors and citizens alike accountable for their health outcomes. All three levels of the system were responsible for addressing not only medical issues, but also nonmedical issues like nutrition, housing and environmental cleanup, that might affect a person’s health. “They created a framework where they could systematically address all the determinants of health at once,” says Jerry Spiegel, a global health researcher at the University of British Columbia. “That’s something we’ve been trying to do in every developing country around the world, and failing at.”
To be sure, there were downsides to this comprehensive approach, stemming in part from the authoritarianism of the Castro regime. It’s been widely speculated that abortion was (and is) used to improve infant mortality rates by eliminating compromised fetuses before they became compromised infants. And it’s easy enough to imagine that not every citizen wanted to attend health education groups, or skip school to fumigate sewers, or live out their days in a sanitarium if they tested positive for HIV, or be sequestered in a home for pregnant mothers if their pregnancy was deemed high risk.
But the upshot was that Cubans themselves quickly came to expect basic health care as a matter of course. Nancy Burke, a medical anthropologist from U.C. Berkeley who studies Cuban health care, remembers one colleague who treated Latin American migrants living near the Mexican border, on the U.S. side. “Doctors at the university were used to very compliant undocumenteds [sic],” she says. “And then they had Cubans come in who knew exactly what was wrong with them and demanded a very clear explanation of what medication was being given to them and what the tests were showing and what the next steps were going to be. And the doctors would get irritated and try to pass them off to the pharmacists. But the Cubans didn’t want the pharmacists. They wanted the doctors. They were embodying health care as a human right.”
*****
It’s no mystery how this system crumbled. In the early 1990s, the Soviet Union fell apart, leaving Cuba bereft of billions of dollars in economic assistance. Two years later, the U.S. tightened its trade embargo against the country. The combined effects were devastating. Rampant food shortages led to rampant malnutrition, which in turn led to an epidemic of neuropathy, a neurological condition that stems from lack of nutrients and can cause blindness. Essential medical equipment and drugs, including mammography machines, pacemakers, and anesthesia, became all but impossible to obtain. And basic infrastructure began to crumble under the weight of neglect. Before too long, infectious diseases were ticking upward again, and health indices were slipping.

A pharmacy with empty shelves in Managua. With the dissolution of the Soviet Union and the U.S. embargo, drugs became almost impossible to obtain. (Photo: Suzanne Kreiter/The Boston Globe via Getty Images)
In response to the crisis, the government made several strategic decisions that still influence the country’s health today. It cut hospital spending and doubled down on maternal health. Pregnant women got extra food rations and nutritional supplements, even as other segments of the population went hungry; those whose pregnancies were deemed at risk were sent to special homes for close monitoring. And in 1994, with the economy near its nadir, the government opened a clinic devoted exclusively to the problem of low-birth-weight babies. Cuba also began nurturing its own biotech sector to compensate for the loss of U.S. supplies, ramped up its doctor export program in an effort to generate income and flung open its gates to U.S. currency and to tourists everywhere.
The legacy of those maneuvers has been mixed. By some accounts at least, they helped stave off a full-blown humanitarian disaster. Not only did the health indices rebound relatively quickly, they actually improved; infant mortality, for example, went from 11 out of 1,000 live births in 1989 to 9.3 out of 1,000 in 1993, and it has continued to fall. But the original ideal of equal health care for all has evaporated in the face of doctor shortages and foreign currencies. And in its wake, two separate systems have emerged: one for tourists and party elites and one for everyone else. While “everyone else” health care is still free, critics say that it is no longer even remotely efficient or reliable. Patients who can afford it bribe their doctors with cash or food to get themselves to the front of unfathomably long queues or to secure urgently needed medical tests. Patients who can’t afford to offer bribes often skip the formal system altogether.
The situation promises to get worse as the country opens up to the rest of the world. “Not only are doctors reaching the limit of their willingness to work for a few hundred dollars a year,” says Richard Cooper, MD, chair of the Department of Public Health Sciences at Loyola Medical College in Chicago, “but now they’re attempting to emulate the outside models of ramping up specialty care.” According to those outside models, he says, that’s where the money is.
In the past, Cuban health indices of note — life expectancy and maternal health — were seen as a collective responsibility and a matter of national pride. Doctors would chase after patients, pregnant women especially, to make sure they got the care they needed to stay above the margins. But doctors themselves are beginning to question the value of this paternalism. “There’s this growing sense that women should be responsible for their own pregnancies,” says Burke. “And that doctors who are being stretched ever thinner shouldn’t have to go chasing after them.”
And it’s not just ideas that are changing with the times. Growing tourism, especially sex tourism, is already leading to a rise in sexually transmitted diseases, including HIV. And as infrastructure continues to deteriorate, dengue and cholera are also on the rise. By some accounts, the island is in the midst of another mortality transition — where infectious disease will once again become the leading cause of death — and it’s only a matter of time before the numbers reflect that shift. “They may be cooking the books a little,” says Katherine Hirschfeld, a medical anthropologist at the University of Oklahoma who has studied the Cuban health care system. “The USSR did this successfully for many years; it was only in the mid-1990s that people realized that life expectancy had been falling for a long time.”
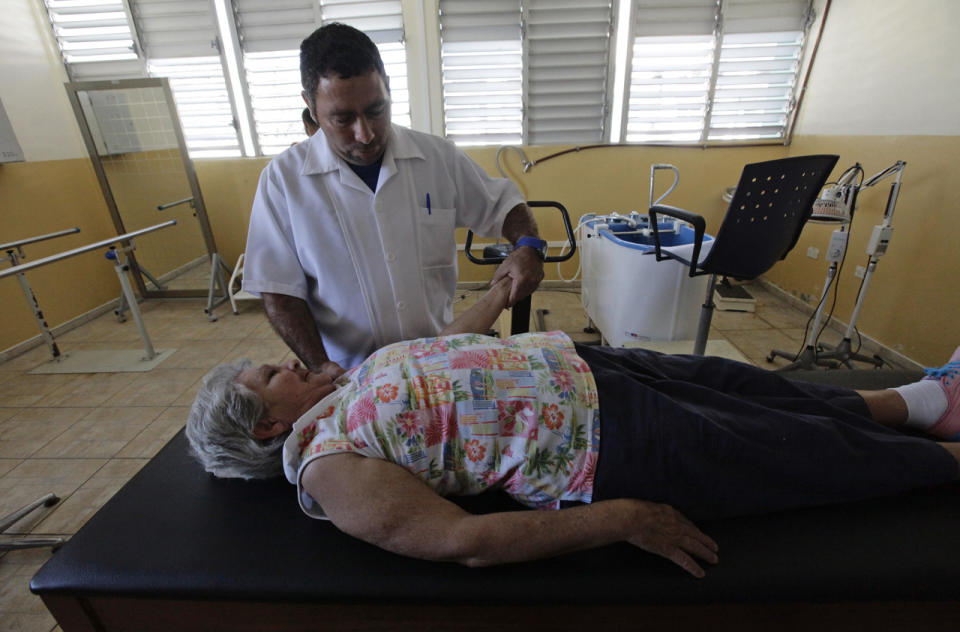
A woman undergoes physiotherapy at the Heroes de la Playa de Giron hospital in Cienfuegos, 150 miles southeast of Havana. Education and health care are free to all citizens. (Photo: Desmond Boylan/Reuters)
For proof that Cuba’s life expectancy data was real at some point, one need only look at Cuba’s current demographics: The country has one of the fastest-growing elderly populations in the Western Hemisphere. But even this unmitigated success will present a challenge going forward. The parks of Havana are often filled with elderly folks doing tai chi to stay healthy, but the government that has seen them into their 60s and early 70s with good nutrition, exercise and regular checkups is not quite ready to manage the suite of medical complications that will arise in the coming years. The average Cuban pension covers only the most basic needs, according to a report by University of Miami’s Institute for Cuba and Cuban American Studies. And a lack of supported living facilities may already be contributing to a rise in suicides among older Cubans. “Many elderly people perceive themselves to be a burden on their families,” writes Steven Ullman, the report’s author. “And, at least implicitly, the Cuban government perceives them as a burden on the state.”
*****
So, how do we make sense of the Cuban Health Paradox? It helps to remember that life expectancy and infant mortality, while important, are not the same thing as total health. Nor is public health the same as medical care such as one receives in a hospital. In both cases, Cuba has exceeded at the former and done abysmally at the latter.
Still, whatever its shortcomings, the Cuban healthcare program does offer some lessons. Regardless of how well or poorly it’s been sustained, the country succeeded in conquering infectious diseases and building a comprehensive primary health care system despite its lack of resources. What’s more, it did it at a time when virtually every other developing nation was being pushed by the World Bank to do the exact opposite: to curb public health spending for the sake of austerity, in exchange for desperately needed loans. Cuba’s health infrastructure may be no better for having taken the less traveled path, but for now at least, its population is indisputably healthier than the populations of countries with comparable economies. “There’s a paradox to the paradox,” says Spiegel. “Why would we think that attention to health would do something other than produce good health outcomes?”

Women at the entrance of a special maternity unit for high-risk pregnancies in Havana. Cuba has long prided itself on its care of pregnant women and newborns, and officials boast of an infant mortality rate lower than that of the United States. (Photo: Ramon Espinosa/AP)
As far as the U.S. is concerned, the takeaway might be trickier. Sure, our hospitals are better and our medicine cabinets fuller. Cost aside (and Michael Moore be damned), there’s no question where you’re better off if you need a new heart valve. But most people go through life without needing open-heart surgery; all of us, though, were once newborns, and live with the consequences of the care we received before and after birth. And if the Cuban experience has a lesson for us in that respect, it’s one we would do well to heed.


