This state is counting the human casualties from a drug meant for animals
Dr. Steven Corder didn’t think his job treating people addicted to fentanyl in Wheeling, West Virginia, could get any harder, but then he began encountering patients who were addicted to both fentanyl and a second drug with its own destructive power — the livestock tranquilizer xylazine.
“Opioid withdrawal is hard enough,” Corder said. But his usual tools, he lamented, “couldn’t touch the withdrawal from xylazine.”
Xylazine is now present in one out of every nine overdose deaths nationwide involving illicit fentanyl, according to the Centers for Disease Control and Prevention.

But West Virginia, which remains ground zero in the American opioid crisis, with nearly twice as many overdose deaths per capita as its nearest competitor, seems to be taking a disproportionate hit from xylazine as well. It now shows up in at least half of the needles in Wheeling, and between 15% and 20% of the needles used statewide, according to 2023 data from West Virginia University.
The drug is known for leaving deep flesh wounds that can sometimes lead to amputations. The wounds develop from skin ulcers that can appear at the point of injection or elsewhere on the body.
Laura Weigel, who runs a treatment center for the local YWCA, said one patient recently had her breast and part of her shoulder amputated because of xylazine. “We are not being able to do anything fast enough to get ahead of it,” she said.
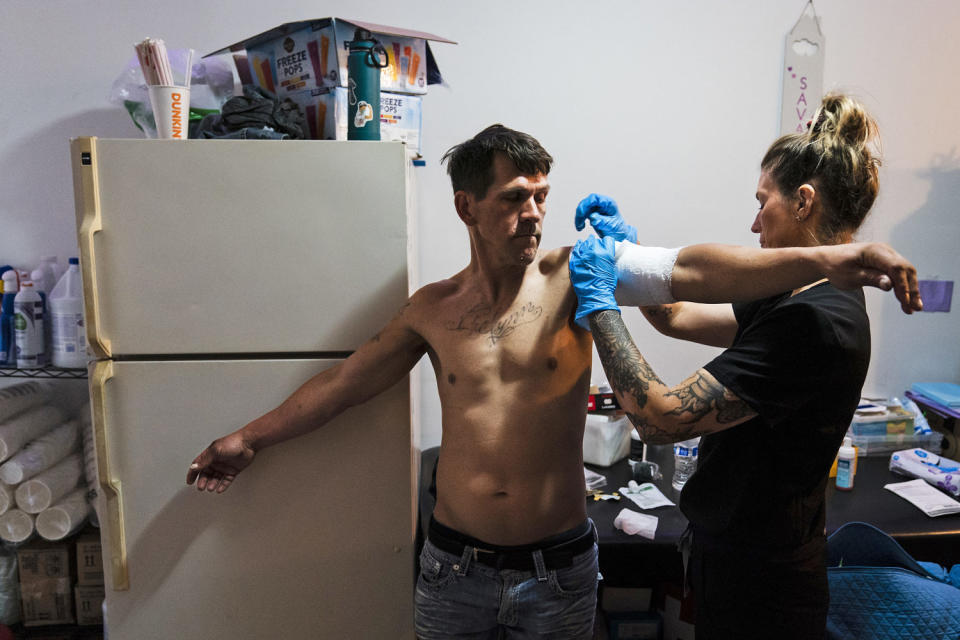
A homeless fentanyl user in Wheeling named Brooke has her wounds dressed twice a day with help from a nurse at Catholic Charities. Brooke, who asked NBC News to withhold her last name, said she is now using xylazine test strips to test for the presence of xylazine in her drug supply.
She also said that in addition to leaving wounds, xylazine threw her into repeat seizures. And she said Narcan, the drug used to reverse overdoses, seemed ineffective against xylazine, which is not an opioid.
“They Narcan’ed me four different times but it didn’t work against xylazine,” she said.
From Puerto Rico to Philadelphia
Xylazine is a sedative used by veterinarians to sedate large animals that need surgery. It has never been approved for human use.
There is not much research on what the drug does to people, but addiction and withdrawal from xylazine seems similar to that for another sedative used on humans in intensive care units called etomidate. Said Corder: “The fact that xylazine is mixed in with illegally manufactured fentanyl or [other opioids] is why you get such a severe withdrawal.”
He said his nurses at Northwood Health Systems often have to resort to sedating patients because they “are so ill and their brains are so hijacked by their addiction that our standard protocols with buprenorphine often do not give them much relief.”
He estimated that 90% of the patients he sees who have xylazine in their system struggle to stay in the first phase of treatment.
Experts said they weren’t sure how xylazine came to be mixed with fentanyl, but it is common for drugs like cocaine and opioids to be cut with other substances that are cheaper or widely available.
Why xylazine? “I’m not sure,” said Dr. Ayesha Appa, an expert on fentanyl at the University of California, San Francisco. “This is one of the challenges of our unregulated drug supply. … I imagine cost/availability is one of the factors, but [I’m] not sure. I will say from my work clinically that many patients do not necessarily want to consume the xylazine, it is just what is in a shifting supply.”
From conversations with patients, Corder said he understands that xylazine “augments and intensifies the fentanyl,” making the high stronger and longer-lasting.
According to law enforcement and researchers, xylazine made its U.S. debut in Puerto Rico and then surfaced in Philadelphia and Connecticut. Though it’s now showing up across the country, anecdotal information suggests its biggest early impact has been in Pennsylvania and the Northeast. West Virginia authorities say the drug came into the state from Pittsburgh, Cleveland and Detroit, similar to fentanyl.
While the Food and Drug Administration and the Drug Enforcement Administration have taken steps to stop some imports of xylazine, the drug appears to be easily available from overseas pharmacies.
Domestic pharmacies ask buyers for a prescription, but within minutes NBC News was able to engage at least five suppliers in India who were willing to ship xylazine immediately without a prescription. One seller wrote that getting through customs could be difficult but another said in a WhatsApp message, “It will get through Customs. If not received then we will send again,” the seller wrote.
The Indian supplier who flagged a customs concern also offered an alternative, “Dexmedetomidine,” which law enforcement officials in Philadelphia have already identified as a possible new alternative to xylazine.
‘Their hands are tied’
In the past month, local police and public officials in at least 11 states have issued warnings about xylazine. California Gov. Gavin Newsom has pledged a new crackdown.
A bipartisan group of lawmakers in Congress say a push to schedule xylazine — meaning to officially designate it as a drug with potential for abuse — is gaining steam, but so far the bill has not passed the House or Senate. Sen. Catherine Cortez Masto, D.-Nev., who introduced the bill in February and has led the effort, said she is optimistic.
“We have seen already what xylazine can do when it is diverted for illicit purposes, and it is incredibly destructive,” she said. “What I know from law enforcement in Nevada and really at a national level is that their hands are tied because it’s not scheduled.”
Thirty senators are on board, said Cortez Masto, and 39 state attorneys general pushed for it in a letter this past spring.
The attorneys general argued that if the federal government schedules the drug, it would let the DEA track the drug’s manufacturing, work to stop the drug’s diversion and crack down on misuse.
U.S. veterinary associations have expressed support for scheduling it as long as veterinarians can still obtain it legally.
In West Virginia, however, attitudes about scheduling xylazine are mixed.
Corder is skeptical about how much of an impact scheduling would have. “Scheduling xylazine would sure be nice,” he said, “[but] I don’t have much faith in methods that prevent access.”
Meanwhile, Charles Mueller, the public health professional at West Virginia University who oversaw the needle-testing study, said it let him give useful, real-time data to local law enforcement and health officials about the state’s illicit drug supply. “It’s not often you can create a new dataset that can be used to empower,” Mueller said.
Mueller said local officials were able to pivot quickly to provide users with test strips to check for the presence of xylazine in their drugs. He’s disappointed, however, that funding for the program was recently canceled.
Without the rapid-response testing, Mueller said, law enforcement and public health officials have to rely on data from medical examiners that can be delayed by up to 30 days.
Mueller hopes the funding is revived. A native West Virginian, he said he lost two people from his community last year from fentanyl overdoses. “I’ve been to way too many funerals to not be 40 yet.”
This article was originally published on NBCNews.com

