This nursing home chain stood out for nationally high death rates as pandemic peaked
***
Martha Miles, one of the first to die, gasped for air. She pressed her nursing home call buzzer but got no help.
Ed Windholtz, Imelda Balbach, Byron Eggemeyer – farmer, nurse, engineer – died hundreds of miles apart within the span of a week in seemingly isolated COVID-19 outbreaks.
The deaths across a scattering of Midwestern nursing homes began surging around Thanksgiving. In the span of a week, the count of the dead nearly tripled in Michigan. Then residents started dying by the dozen in Ohio and Indiana. By Valentine’s Day last winter, the death toll had climbed into the hundreds.
***
A USA TODAY investigation has traced the casualties back to one nursing home chain, Trilogy Health Services, owned by a real estate venture with a new business plan for the cutthroat world of elder care.
The deal promised a historic investment opportunity, then delivered the highest death rates reported by any large nursing home chain at the height of the pandemic.
Residents at Trilogy’s 115 campuses died of COVID-19 last winter at twice the national average for nursing homes, USA TODAY found, based on figures facilities must file weekly with the federal government.
Presented with USA TODAY’s findings, the company said it had mistakenly reported hundreds of deaths during the surge. Trilogy offered a revised tally that would reduce its COVID-19 death count by more than 40%. The company declined to provide documentation needed to vet those claims but said Wednesday it had filed new numbers with the federal government.
Even by its own drastically lower numbers, Trilogy’s death rates still would have ranked well above the national average for nursing homes during the winter surge.
Until now, such pervasive failures escaped notice. In a first-of-its-kind analysis, USA TODAY has revealed ownership webs invisible to consumers. Problems across chains eluded federal officials overseeing nursing homes, who were focused on individual facilities during the pandemic.
Reporters scored the performance of every nursing home in America to probe questions of corporate responsibility left unanswered by dozens of research papers on COVID-19’s more than 140,000 nursing home deaths.
Martha Miles died after going to Bethany Pointe in early 2020 to recover following a fall. One night, the 70-year-old had called her son crying, “I can’t breathe.”
Her purse and new pajamas were dumped in an oversized bag in the foyer, he said, before her family learned what went wrong from a notation in her death certificate: “CORONAVIRUS.”
Miles, formerly a social worker, raised three boys and spoiled 18 grandchildren. She died before meeting three of her six great-grandchildren.
Nearly two years later, her son, Marvin Miles, still misses the smell of her pot roast and candied yam dinners. He teared up to learn from USA TODAY about the investment strategy behind the nursing home run by Trilogy.
“They are making money off people’s lives,” he said.
THE BUSINESS MODEL
Danny Prosky, Jeff Hanson and Mathieu Streiff live a world away from the chain of small Midwestern nursing homes, in spacious, multimillion dollar Orange County, California, homes replete with whirlpool baths, architectural pools and panoramic views.
The trio has worked together for years building real estate investment portfolios. In an interview, Prosky recalled how they bailed in late 2011 from a sponsoring firm headed into bankruptcy. To safeguard an investment, he said they shut down on a Friday and by Monday had relaunched with new support.

Their expertise is Real Estate Investment Trusts, known as REITs. These companies can own most any property that generates rent. Buying shares of REIT stocks lets individuals invest in large properties, from office buildings to the land under cell towers.
REITs are exempt from corporate income taxes, just like mutual funds, so long as most of their income gets paid out to investors in the form of dividends. The concept has become yet another way to make money from health care, following a trend of private equity firms buying up dental chains and hospital mergers driving up pricing.
In 2015, Prosky and his team led the REIT purchase of a majority stake in Trilogy. The $1 billion acquisition of the growing nursing home chain doubled the size of their portfolio, which was targeting the future needs of a booming senior population known as the “silver tsunami.”
Until Trilogy, major nursing home operators and their REITs had separated the real estate from the care delivered inside. But Trilogy wasn’t for sale under that kind of arrangement, Prosky told USA TODAY.
So the REIT purchased not only Trilogy’s properties, but also the health care operations inside its campuses. The approach meant a chance at bigger profits – as well as more risk in an economic downturn.
“This was an operator of real estate that we wanted to be associated with,” Prosky said.
Nursing homes looking to boost profits have limited options. The business is heavily subsidized by government-funded health care programs for seniors and people with disabilities. Improving relationships with local hospitals, for example, can shore up more referrals, industry insiders say.
One approach is cutting staff costs, typically half of the operating budget in nursing homes, said Tyler Braun, an assistant professor at Cornell University studying health economics.
“It is ultimately going to have effects on patient care and quality,” he said.
"PRESSURE BUILT UP"
Administrators who ran individual Trilogy facilities said they never heard from the California landlords, but several recalled years of tight budgets and an increasingly competitive culture that ranked facilities by business performance metrics.
“That pressure built up,” said Jessica Trinko, former executive director at The Heritage in Findlay, Ohio, who now works at a non-profit nursing home.
In the years after the REIT takeover, staffing cuts became the norm, USA TODAY found in its review of federally filed expense reports. Paid hours per resident for nurses and aides, a figure that includes sick leave and vacation, fell by 13% over four years at facilities Trilogy currently operates. By contrast, nursing homes nationally cut 2% on average in that timeframe.
The cuts did not play out evenly. As of early 2020, Trilogy’s registered nurses provided slightly more care hours than most large chains, although the levels still fell one-third below recommended federal minimums. These nurses are trained to assess medical conditions and matter the most in how the government rates nursing homes on quality.
Trilogy’s staff reductions targeted a different category of caregiver. At facilities operated by Trilogy, staffing of certified nursing assistants, called CNAs, fell to among the lowest levels of major operators. These frontline caregivers feed and bathe residents, help them to the toilet and change diapers, and make sure they do not get bed sores.
“CNAs are the foundation,” said Charlene Harrington, professor emerita at the University of California, San Francisco, who has studied nursing home quality for over four decades. Without sufficient staffing, she noted, “the work just doesn’t get done. It’s impossible.”
CNAs at Trilogy, including trainees and medication technicians, had about two hours a day to spend with each resident when the pandemic started, according to data submitted to the government from nursing home timesheets. Recommendations from a 2001 federal study urged close to three hours at a minimum.
The author of that study, Vanderbilt University Center for Quality Aging Director John Schnelle, reviewed USA TODAY’s analysis of Trilogy’s CNA staffing levels during the pandemic. He called the staffing hours “awful,” “terrible,” “abysmally low.”
“You don’t even have time to take somebody to the bathroom, much less take all the steps that you need to prevent infection spread,” he said.
The pandemic left CNAs harder pressed for time with sicker patients while juggling new requirements to guard against the spread of infection. Gowns and gloves had to come on and off constantly. More handwashing. Shifting public health guidance on the use of masks. Patient interactions could take twice as long.
Asked about its years of cuts, Trilogy provided USA TODAY with figures that showed far higher staffing levels – some of the best among large chains. The difference? Trilogy included the hours logged by nurses for administrative duties.
A recent academic review of three dozen major studies on nursing homes during the pandemic later suggested that having a larger staff increased the odds of COVID-19 entering a nursing home. But once the virus got in, more care could keep residents alive.
At Trilogy, people started dying.
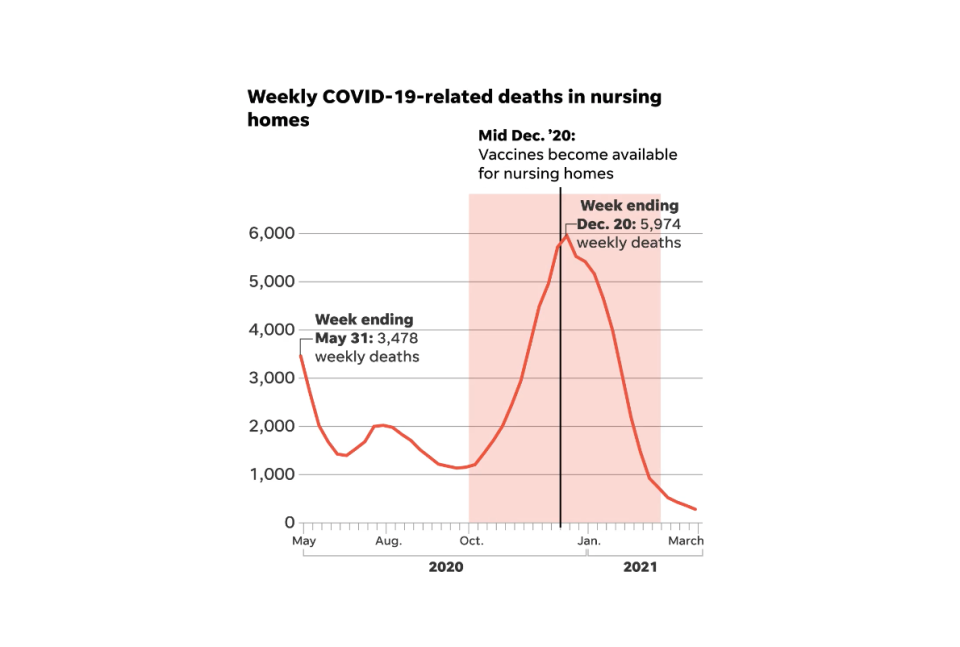
COVID-19 DANGER ZONES
Trilogy’s COVID-19 game plan called for dividing campuses into red, yellow and green zones to limit exposure to the virus. Eyewitness interviews and the reports filed by health inspectors indicate this safety regimen was often a charade.
A Trilogy facility in Battle Creek, Michigan, cordoned off a “red zone” by hanging a plastic wall on one side of a hallway, a December inspection report showed, but did nothing to block off the other end beyond putting a sign on a table that read “no entry.”
Doors were left wide open to the COVID-19 patients’ rooms, state health inspectors found. Aides didn’t know how long to wipe down equipment for proper sanitation. Soon all but two residents were infected. According to its reported figures, 21 residents died.
As winter started, infection swept through Cobblestone Crossings Health Campus in Terre Haute, Indiana, earlier cited for failing to enforce proper hand cleaning. Workers fell sick from the kitchen to the laundry to the bedside. Eighteen residents died.
Natalie Hornback, a former aide there, recalls feeling powerless. “There wasn’t anything we could do,” she said.
An outbreak in Kokomo, Indiana, lasted nine weeks and infected 88 residents at Trilogy’s Waterford Place Health Campus. By the end of January, 29 had died.
Overnight, the facility turned into a scene from a sci-fi movie, with plastic barriers and bins set out for discarded masks and gowns. CNA Nicole Steele remembers feeling shocked, then her work routines turned into chaos.
She recalled sick and frantic residents “on their lights constantly” calling for help.
Showers used to come before breakfast. But in COVID-19, she had to wash residents in bed. Doing that right could take 45 minutes. Two nurses and two aides on some days had to cover residents on three hallways, she said. Mornings passed in a blur of trying to deliver bites of breakfast off trays wrapped in plastic.
“By the time you’re done, it’s lunch time,” Steele said. “You couldn’t get people fed completely.”
Frustrated and emotionally spent, Steele posted a remembrance on Facebook to a patient who died from COVID-19, an action she says led her to be fired for violating patient privacy. Asked about it, Trilogy officials declined to comment on an employee’s situation. They also denied reporters permission to visit several of the company’s hard-hit campuses.
In early December 2020, Waterford resident Sue Miller ran a 103-degree fever, her only COVID-19 symptom. Two weeks later, a hospice nurse called, urging relatives to come fast. The facility was on lockdown, but they could say their final good-byes.
Four of Miller’s children, their spouses, a granddaughter and a niece were allowed inside, one at a time, each for 15 minutes, according to a daughter, Shana Driver. They weren’t questioned when they stretched their permitted visits into a four-day, round-the-clock deathbed vigil.
The first day, they were given masks, face shields, gowns and gloves. They rarely saw staff after that, Driver said. No one checked their temperatures or refilled the box of gloves they had quickly used up in the entryway of a standalone building designated the red zone.
Inside, Driver said they saw a nurse slip her mask down at Miller’s bedside. Staff touched Miller without gloves. A nurse went to her car and back without changing her gown. Used masks, gloves and gowns eventually spilled out of the entryway trash.
“I don’t know that they had a clue what they needed to do,” said Driver, who felt guilty removing her mask briefly for a kiss and sliding off her own gloves to rub cocoa butter lotion into her mom’s arms.
Miller, 77, died with family by her side in a cold, beige room on a Monday, four days before Christmas. Her holiday tree was still in a box.
Her family had not been notified when health inspectors documented COVID-19 violations. In November, state inspection reports show, an aide got caught chatting at a nursing station with a mask down. Multiple staffers needed training on how properly to put on and take off gowns.
A later inspection in January found a resident without a mask wandering from room to room in the memory care unit, finally grabbing a used mask from the trash. The same resident earlier had roamed freely with a 101-degree fever and then a dry cough.
Waterford Place ended up with more than $20,000 in fines, while its reported death rates spiraled.
TRILOGY STANDS OUT
COVID-19 marched into almost every nursing home in America during last winter’s surge, when 71,000 residents died – the most of any wave of the pandemic. Still, at more than a quarter of the nursing homes reporting outbreaks, no one died.
USA TODAY’s analysis adapted a statistical model created by the federal government to assess how well nursing homes controlled COVID-19 infections and deaths. Reporters also calculated average death rates from information that facilities reported weekly under federal mandate to ensure uniform COVID-19 tracking across the nation’s nursing homes.
Over and over, Trilogy stood out compared to other major national chains based on its own reports to the federal government. Here’s one example of how Trilogy emerged from the pack:
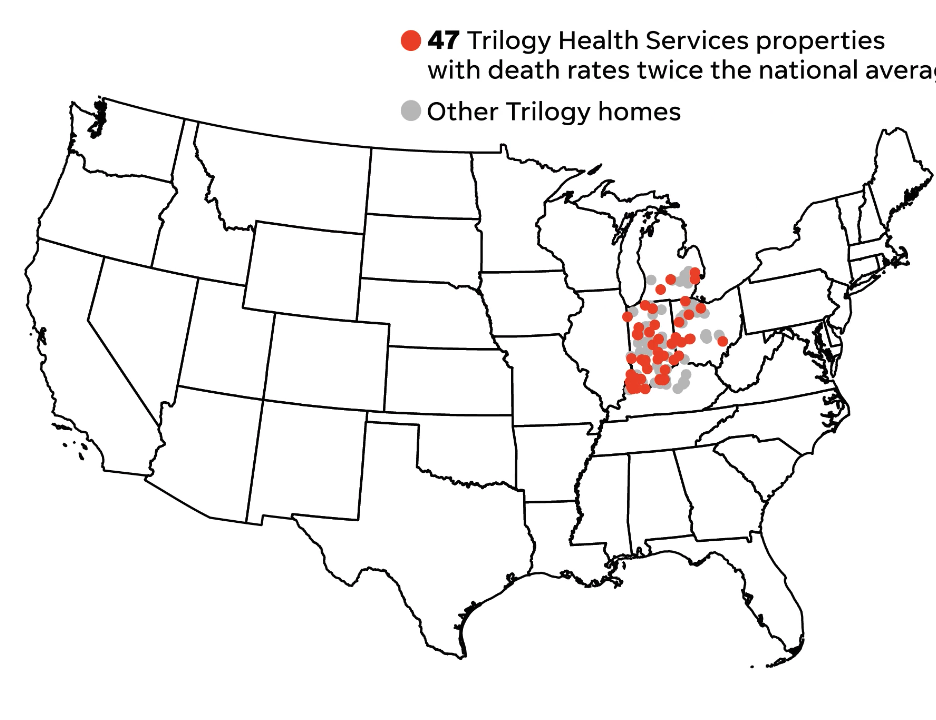
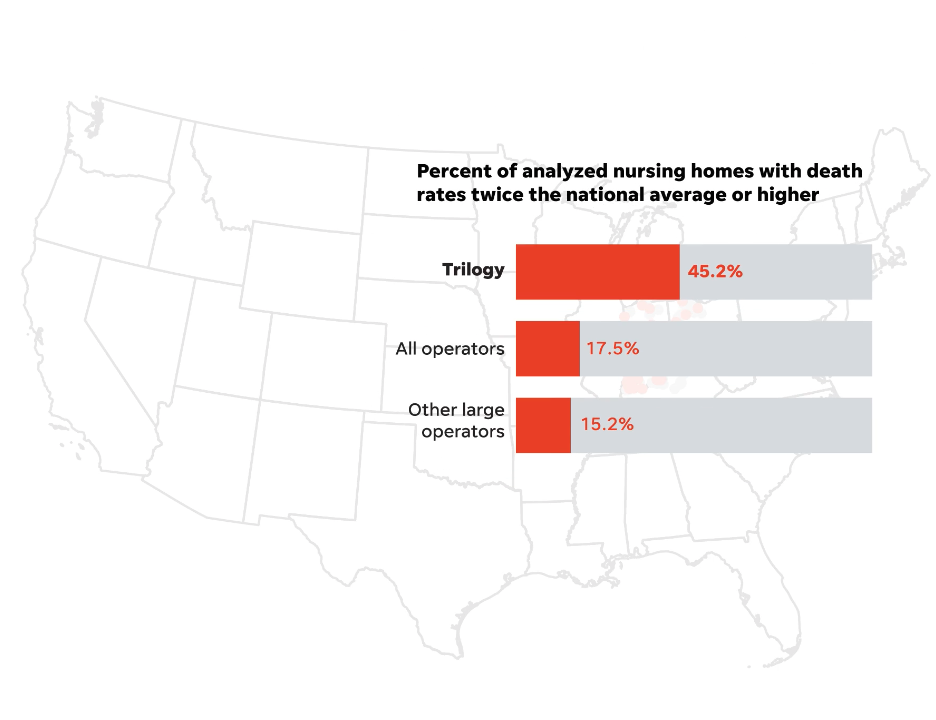
Not all Trilogy homes were among the nation’s worst; based on the company's original filings, 17 of them had no deaths during the surge. But the chain overall stood out for how often people died once they became sick. In all, the chain reported 772 COVID-19 deaths last winter.
U.S. nursing homes averaged 3.3 deaths per thousand residents each week, while Trilogy's initial reports revealed 7.0 deaths per thousand. The new figures provided by Trilogy to USA TODAY are not detailed enough to allow a precise comparison. However, Trilogy’s revisions would appear to put its death rate about 40% above the national average, still ranking it among the highest for leading chains.
After spending weeks reviewing USA TODAY’s findings, Trilogy responded with a written statement in which its CEO, Barney, called the government data “demonstrably unreliable and incorrect.”
“Trilogy has always made residents our top priority, and our caregivers are health care heroes having worked day and night to preserve the safety and health of seniors in our facilities,” she said in the statement.
Barney referenced a report from the U.S. health department’s inspector general, which examined the early days of the federal reporting. At the time, there were news reports of errors at individual facilities. The report found the vast majority of nursing home submissions appeared complete. An updated OIG evaluation is due to be published this September.
By last winter’s wave, facilities had been reporting COVID-19 deaths and cases to the federal government for months. The data has been used extensively by researchers. Health regulators relied on it to monitor and respond to hot spots in real time.
The federal public health office working with nursing homes on the weekly surveys said it had not heard of a large chain needing to make a correction that would eliminate hundreds of previously reported deaths.
USA TODAY was unable to substantiate Trilogy’s explanation for reporting 318 deaths that it now says should not have counted. The company failed to respond to requests for detail and documentation of the reasons. Nor did Trilogy provide its revised counts at the facility level as required for the government database, the National Healthcare Safety Network (NHSN).
“Recently, as a result of the inquiry by USA TODAY, Trilogy performed an internal audit of its NHSN reporting and engaged an independent third-party firm to review the results of the internal audit in order to ensure accuracy,” a company statement said.
USA TODAY did its best to examine Trilogy’s concerns. For instance, the company noted that it operates in four Midwest states that had high levels of community transmission during the winter surge.
This was already accounted for in USA TODAY’s analysis. Because academic research on COVID-19 consistently linked outbreaks in nursing homes to the level of virus in the county at large, USA TODAY drilled down into the counties where Trilogy operates nursing homes. Reporters found its communities had 15% higher infection rates than the nation while Trilogy’s original reported death rates were 112% greater than the national average.
Trilogy told USA TODAY another issue in its reporting involved confusion between nursing home residents and those receiving assisted living services on the same campuses. But the limited breakdown provided by the company of its assisted living deaths represented a small fraction of the total Trilogy says it incorrectly reported.
Other factors that Trilogy cited – such as duplicate reporting or residents who tested positive for COVID-19 but died from other causes – either did not hold up upon further review, or could not be validated by USA TODAY.
Trilogy’s reported numbers do show, however, that the chain rapidly refilled its beds as the virus raged on. Trilogy reported 204 deaths over two weeks in December 2020 but its resident population only dropped by 99.
On Facebook, Trilogy advertised a move-in special at many of the facilities battling outbreaks. “Hurry in,” it wrote. “Offer ends soon.”
THE DEAD
Emergency calls from a dozen Trilogy facilities at the height of the winter surge show how people’s final moments played out: He’s hypoxic, turning purple … Screaming, respiratory distress … Dry-heaving, pulse elevated, shortness of breath … He’s a hot mess … Fighting with the family all day on code status, there’s not much we can do.
In conversations with USA TODAY Network reporters, families who lost loved ones at Trilogy facilities grieved for lives cut short and the loss of final good-byes.
Those who died at the start of the pandemic, such as 65-year-old Bill Malone, never made the federal government’s official count because reporting was not yet required. Malone, a community theater star, went to a Trilogy facility in Anderson, Indiana, to recover after a heart attack. He died without his wife by his side.

“I did not get to talk to him,” said his wife, Carlynn Malone, who still sleeps with an oversized stuffed gorilla to fill his empty spot in the bed. “I wanted to say ‘I love you.’”
Ann Clay, 78, was a quiet intellectual who preferred quilting and reading to socializing before developing dementia. When the pandemic prevented her husband from visiting in person, he felt reassured to see staff wearing masks and gowns in the background of their Zoom calls.
Ron Burgess, 71, and John Kline Jr., 73, died in early December in an outbreak at a Trilogy facility in rural Ohio. Burgess, a former nurse, for years had put his flowing beard to use as the town Santa in Bellville, Ohio. Kline’s wife of 47 years snuck him a milkshake during their final visit.
Phyllis Thompson, a minister’s wife enjoyed piecing together 1,000-piece jigsaw puzzles. She died on her fourth day in COVID-19 isolation at a Trilogy facility in Louisville, Kentucky.
Ed Windholtz, 83, liked to tell dirty jokes. He was a farmer and lifelong bachelor with eight sisters, and selected the Trilogy facility where he died in Batesville, Indiana for its Catholic name. His surviving sisters remain heartbroken that friends couldn’t attend his funeral.
Imelda “Mel” Balbach, 89, a retired nurse, quickly declined after she tested positive for COVID-19 at a Trilogy facility. She died during an outbreak during which her Evansville, Indiana nursing home reported that half of residents infected with COVID-19 died.
Reba Hammons, 96, baked lemon meringue pies before dementia eroded her quality of life. Her daughter, Sharon Williams, praised the vigilance of workers at her Trilogy home in Battle Creek, Michigan, against a virus running rampant. “They tried very hard,” she said.
Byron Eggemeyer’s daughter worried but could do little more. She spent their final visit shivering outside his window at a Trilogy nursing home in Terre Haute, Indiana. The 87-year-old former engineer – “Boppy” to his grandchildren – could barely open his eyes as she held up a photo of a newborn great-grandchild that he would never meet.
In her father’s obituary, Brenda Weeks purposely wrote that he died of COVID-19 while living at Cobblestone Crossings Health Campus.
“I was mad then, and I’m still mad now,” she said. “I was shaming them.”
HISTORIC STOCK LISTING
The real estate venture behind Trilogy came out of the winter surge with cash on hand and planning underway for its next business move. What is today called American Healthcare REIT proposes a major stock offering. It touts a now-$4 billion portfolio as potentially “the largest healthcare REIT listing in history.”
Trilogy is central to the pitch. “Trilogy was our best performing manager before COVID hit,” Prosky, the CEO, said on a call with investors last summer. “They've had the best recovery so far in 2021.”
A 158-page annual REIT financial report from the pandemic’s deadliest year for nursing homes contains many facts and figures. It does not detail the chain’s COVID-19 death toll.
It shows that Trilogy’s share of the company reported $107 million in net operating income, a metric used to gauge profitability. That includes revenue from resident fees and services, as well as federal COVID-19 relief, minus property operating expenses.
This view of financial performance does not break down nursing home income from that contributed by independent and assisted living services on the same campuses. Skilled nursing accounts for more than half of Trilogy’s business, REIT officials said in an interview.
Prosky highlighted the financial challenges of the pandemic and noted that government aid saved its bottom line in 2020.
“I would by no means call it a healthy year,” Prosky said.
The REIT reported, under its Trilogy business segment, receiving $53.9 million in federal COVID-19 relief. Multiple REITs involved in its complex ownership arrangement benefited, according to filings with the U.S. Securities and Exchange Commission. A minority REIT stakeholder, NorthStar Healthcare Income, said its share was $12.5 million.
USA TODAY provided officials with American Healthcare REIT with details from its analysis and written questions and asked for further discussion around the complex financial statements. AHR offered no response beyond referring to its SEC filings. Northstar did not respond to inquiries emailed to company officials and media representatives.
David Grabowski, a health care policy professor at Harvard University medical school who studies nursing home performance, said USA TODAY’s findings underscore the need for greater transparency about ownership and financial accountability.
“Places can’t just siphon off dollars,” he said. “They actually have to put those dollars back into direct patient care.”
Financial filings required of REITs offered insight into how corporate chains and REITs can make money off Medicare and Medicaid, the federal health insurance programs for seniors and people with disabilities.
The nursing home industry’s corporate layers can result in individual facilities posting losses while investors profit off their parent companies, according to attorney Ernie Tosh, who maintains a national database of nursing home financial information used by other lawyers filing lawsuits for families and prosecutors fighting fraud.
“That is why people die,” Tosh said. “The facilities would rather take that profit than staff correctly.”
The stock listing proposed for later this year involving Trilogy will explore Wall Street’s appetite for using a federal law known as RIDEA, or the REIT Investment Diversification and Empowerment Act, in a big nursing home chain.
Since 2008, this law has enabled health care REITs to make profits from operations beyond collecting rent on real estate. The concept was permitted earlier for REITs outside of health care to allow them to offer basic services for their properties, such as cleaning.
A possible upshot, experts say, is better collaboration between a landlord and the tenant, who together figure out how best to run the businesses inside their property. That model is commonly used in assisted and independent living.
Still, Trilogy’s arrangement puts a REIT in the business of running a large nursing home chain delivering life-and-death care, industry insiders said.
“When you get into personal care and health care, there can be a slippery slope,” said Stephanie Krewson-Kelly, author of the industry guide Educated REIT Investing, who helped review USA TODAY’s analysis of Trilogy’s REIT profitability.
During COVID-19, this model would have left a REIT on the hook for “the financial implications of unfortunately a lot of death, and certainly a lot of illness in the four walls of the facility,” said Rich Anderson, a senior Wall Street analyst who covers the industry for investment firm SMBC Nikko Securities America.
The concept, by law, requires an independent manager to oversee the health care operations inside the REIT’s properties. But the lines appear blurry.
The REIT behind Trilogy focuses on “buy and sell” real estate and development decisions, general counsel Gabe Willhite told USA TODAY.
“Making sure that you’re on track on budget and understanding how the performance is going is important to everybody here, so those are the things that we focus on a lot,” he said.
Employees and the day-to-day operations fall to a management entity led by Trilogy’s CEO, Barney, who described seeking approval from the parent company for longer-term plans.
In separate interviews with officers from the REIT and Trilogy, USA TODAY was told the REIT also closely watched COVID-19 numbers.
Sabra Health Care REIT, traded on the NASDAQ stock exchange, prefers a landlord role with nursing homes. In a typical industry arrangement, its nearly 300 nursing homes sign leases agreeing to rents that can increase each year by 2% to 2.5%.
CEO Rick Matros said he would not consider RIDEA for a health care business as complex and regulated as nursing homes.
“All of a sudden,” he said, “you have direct responsibility for what happens there.”
Letitia Stein reported this story while participating in the USC Annenberg Center for Health Journalism’s 2021 National Fellowship. This report was also supported by the Economic Hardship Reporting Project. Jeff Kelly Lowenstein is the Padnos/Sarosik Endowed Professor of Civil Discourse at Grand Valley State University.
This article originally appeared on USA TODAY: Nursing home chain logs high death rate during COVID. What went wrong?

