How Cord Blood Turned This 4-Year-Old’s Life Around
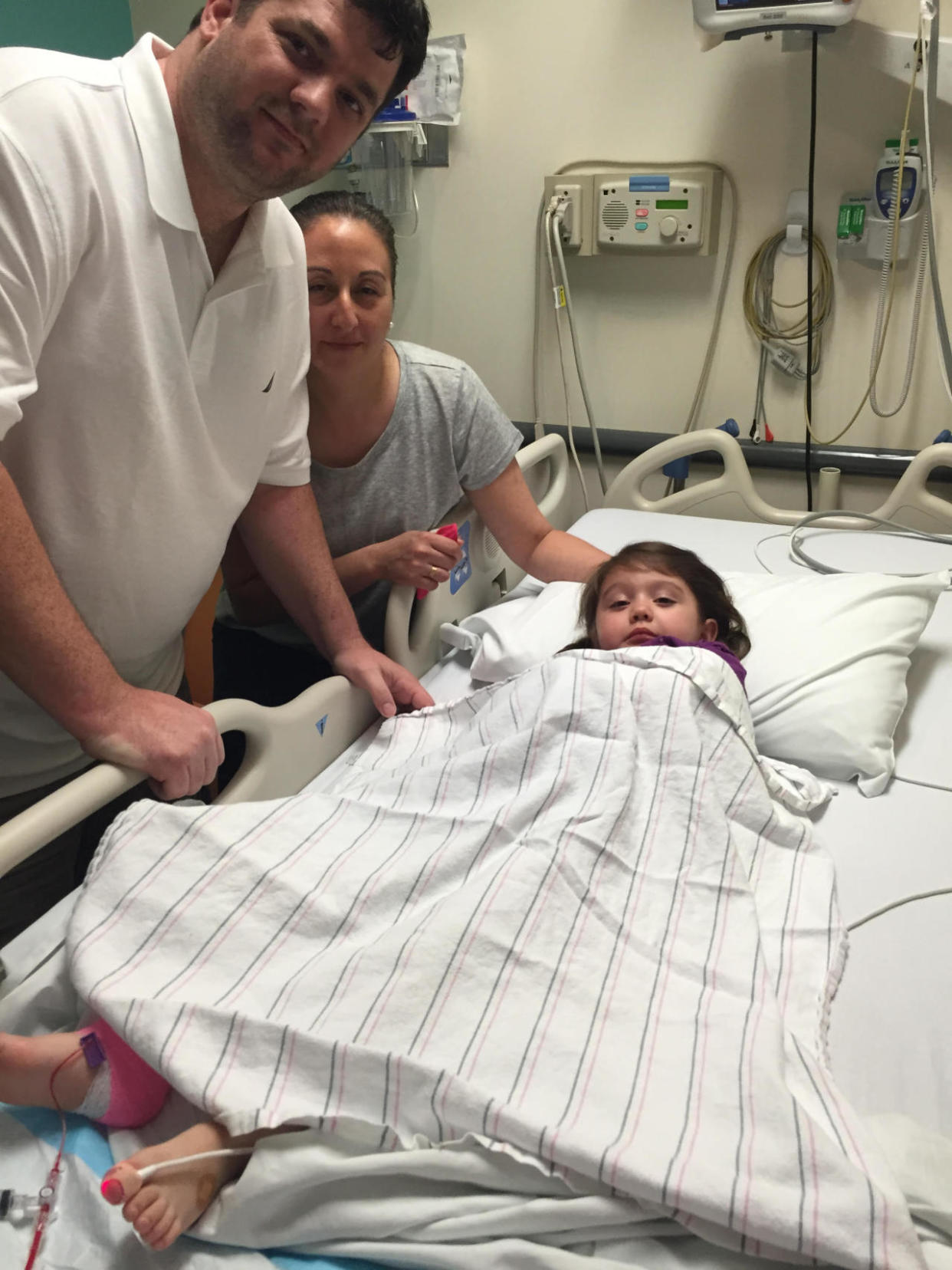
When Steve and Rosa Barney’s daughter Isabella, now 4, was born, the couple decided to take a preventative medical measure that felt both mysterious and hopeful: They banked their baby girl’s cord blood with a private company, thinking that its rich stem cells could be there to help treat an unforeseeable issue, such as childhood leukemia. They also considered that it might someday benefit their older son, who suffers from a motor speech disorder called childhood apraxia.
They wound up using it sooner than they thought, and in a way that totally amazed them — for Isabella’s own apraxia, discovered at 18 months and largely turned around when she was 3, after a 15-minute, cutting-edge procedure, in which a their daughter had an infusion of her own stored cord blood. “It was like her being born again,” says Steve (pictured above with his wife and daughter), of Queens, New York, who notes that he and his wife were stunned by the results.
STORY: Is Cord Blood Banking Worth It? The Great Debate
Theirs is an inspiring tale about a decision that expectant parents are bombarded to make over and over again through the pamphlets, posters, and sales reps — even the oft-paid-off doctors themselves — each time they visit their obstetrician’s office: whether or not to choose the pricey service of cord blood banking, which is when stem cells are removed from an newborn’s umbilical cord once it’s been clamped and cut. Those cells are then sent to a lab and frozen as a type of insurance, in case one day, if needed, they can be thawed and used to treat certain health conditions and diseases.
The whole process has become big business, and while many parents wind up convinced to (or pressured into) taking part, the American Academy of Pediatrics recommends that parents forgo it, and most experts agree with the reason why: Chances are slim to none that a baby will ever be able to use the stem cells from his own cord blood, for a huge variety of reasons — including that, if a child develops a genetic disease, the stored stem cells will have the same genetic flaws, and will not be a useful treatment.
STORY: Is Cord Blood Banking the Future or Full of It?
And yet every once in a while, a success story like Isabella’s emerges that could turn even the biggest cord-blood skeptic into a believer.
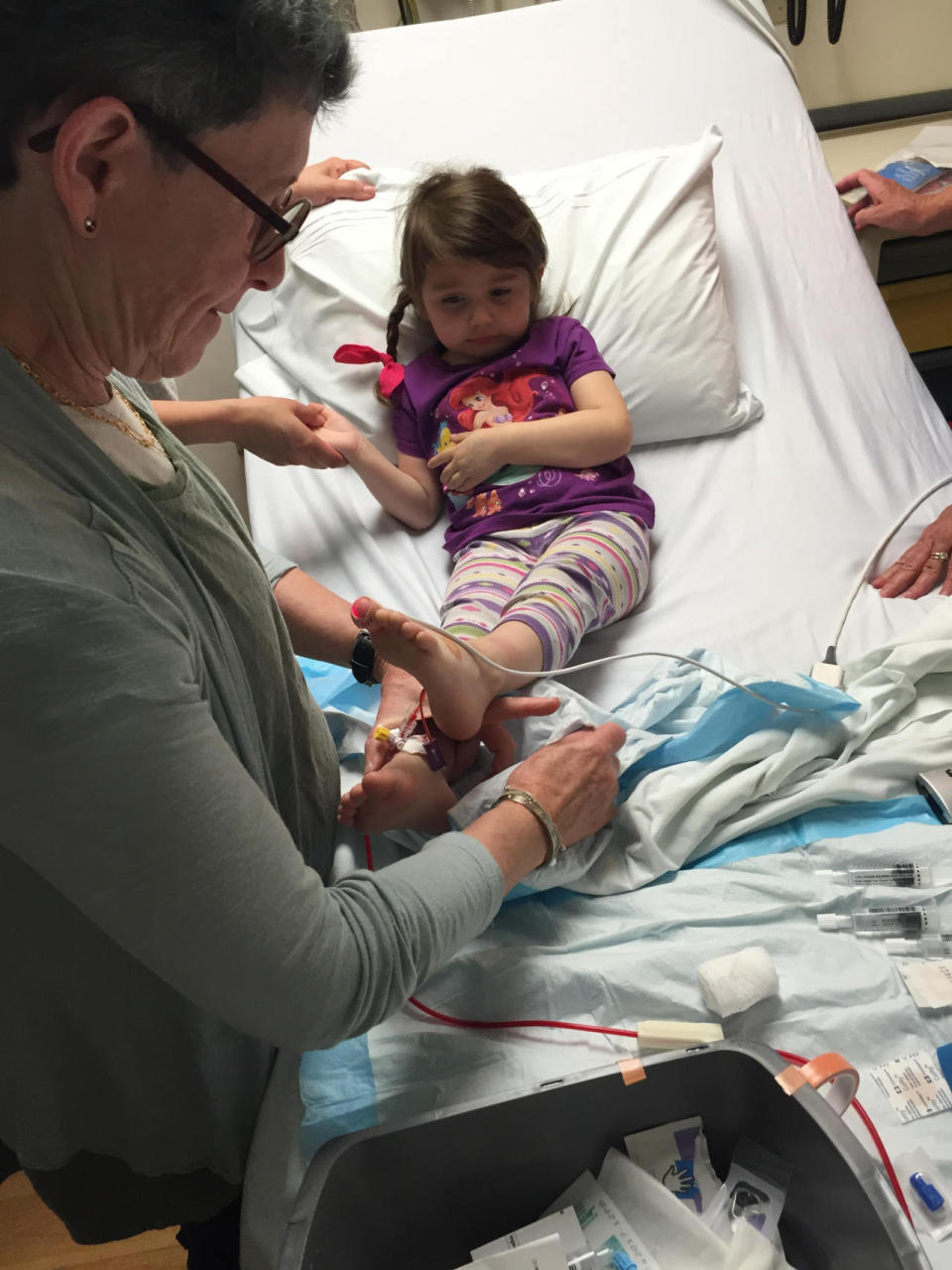
Isabella with Dr. Kurtzberg, receiving her treatment at Duke. (Photo: Steve Barney)
“Apraxia is a relatively new treatment, and people are banking on technology catching up. Who knows? Maybe autism will be next,” Martin Smithmyer, CEO of Americord, which the Barneys chose to bank with, tells Yahoo Parenting. “It’s a biological insurance policy. Odds are you’ll never use it.”
Steve, a former equipment manager with Major League Baseball and now co-owner, with his wife, of an indoor play space for kids, recalls being pushed to consider the issue each time he accompanied Rosa on obstetrician appointments while she was pregnant with their daughter. “There were always salespeople,” he says, particularly from the Cord Blood Registry and ViaCord companies. But they were sold on the idea. And so, after a bit of research, the couple landed on using Americord, a New York–based bank that had a lot going for it, in Steve’s opinion — including a focus away from marketing and a policy against paying off doctors to hawk their services (which some competitors do, says Smithmyer, noting that it is “not really that ethical.”)
“Martin was easy to deal with, and others were pushy,” Steve says. He also felt the storage fee was reasonable — about $2,500, compared with other company’s fees that could be upwards of $3,500 with additional storage fees of several hundred dollars a year.
But from the start, the Barneys figured it would be their teen son Matthew, now 16, who would most likely benefit from the stored stem cells. “He didn’t start speaking until 3 or 4, though it was more whining and pointing, and he still has a very limited vocabulary,” Steve explains about his son’s apraxia — a disorder in which the brain has difficulties moving parts of the body needed for speech. They relied on early-intervention education to help him improve, but kept in the back of their minds what they’d heard about an experimental new treatment that relied on the use of stem cells from cord blood.
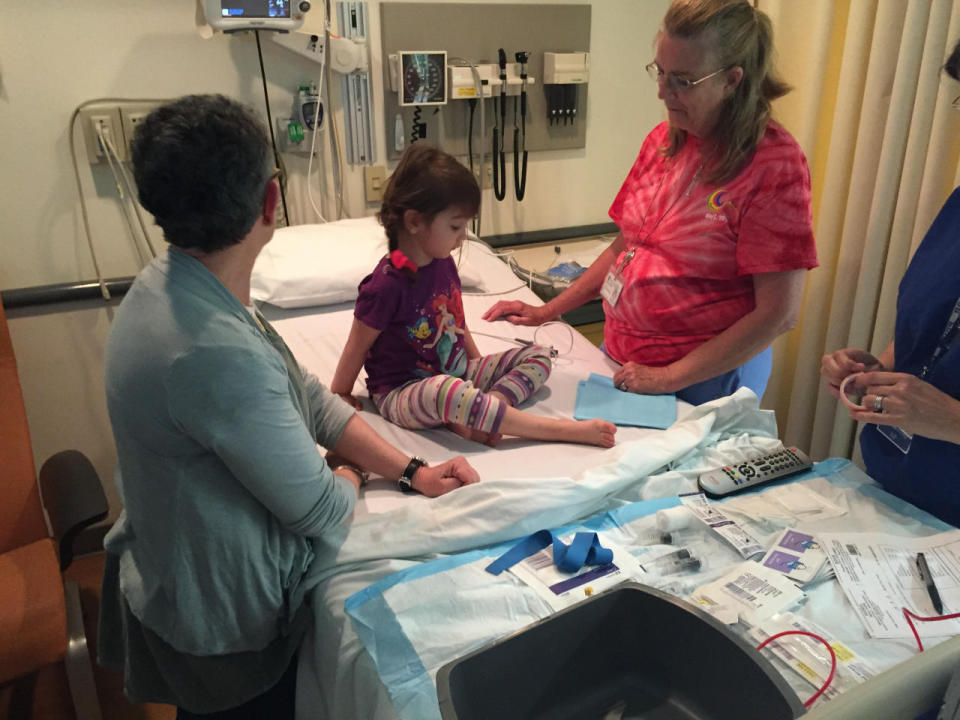
Photo: Steve Barney
The Barneys paid Americord the fee, had Isabella’s umbilical cord cut and stored by the company, and moved on — until their daughter was around 18 months old, and she, just like her brother, was diagnosed with childhood apraxia.
“We got on the ball a bit quicker with her,” Steve explains, having her tested and utilizing early intervention services when she was very young. But she went to preschool at 2 ½ with “very limited vocabulary,” he says, and, after preschool, had only about 15 words that could be understood (typically, a 3-year-old would have about 500 words at his or her disposal). Her parents dove into research about using stored cord-blood for treating apraxia, and found a cutting-edge program at Duke University, where stem-cell pioneer Dr. Joanne Kurtzberg had already overseen a handful of similar, successful treatments — including for a 5-year-old with cerebral palsy, Grace Rosewood, who experienced vast improvements after receiving infusions of her stored cord blood as part of a clinical trial.
“We were still hesitant,” Steve recalls about taking the chance. “One thing they don’t tell you with banking is that it’s basically a one-time use.” Still, after speaking with another parent about having success with the treatment at Duke, he says, “it was a no-brainer for me.”
Then came the elaborate process of looking into whether or not Isabella was a good candidate. “We look at the cord blood, as some banks get a higher quality than others, and we need make sure we have enough cells, with a minimum amount of information, plus good sterility,” says Kurtzberg — who also runs a public cord-blood bank and Carolina Cord Blood Bank, accepting donations from moms who deliver healthy babies but who have no risks, and is the president of the new Cord Blood Association, created to harmonize education, regulation, and advocacy around the issue of cord-blood banking.
Regarding the decision of whether to bank a baby’s cord-blood privately or publicly, Kurtzberg explains, “A mom has to know she’s really giving up her rights to the cord blood with a public donation. If it happens to be there, she can have it. There’s no risk, no cost, and is the truly altruistic choice.” Publicly donated cord blood is available to anyone, and doesn’t necessarily have to be a full match; it’s particularly useful for both children and adults who have conditions that cannot be treated with one’s own cord blood — including some cancers, sickle cell, and metabolic disease.
“So there’s lots of confusion, because of the way [private] banks market themselves,” Kurtzberg says. “If they’re honest about it, it’s an investment for the future, or in the rare case of a problem, like with this family.”
Isabella received her treatment after receiving a full workup, including tests to make sure there was no genetic disease present. She checked out, and the cord blood was shipped to Duke.
The family was there for three days with their daughter, but the whole infusion process, given through an IV, took just 10 to 15 minutes, Steve says. As Kurtzberg explains, “The child gets an IV — sometimes the veins in the feet are easiest to access — and they get Benadryl and a steroid to prevent reactions.” Then they infuse the cells, which have been washed in a lab, through a drip, similar to how a blood transfusion works. Duke typically does about three to four infusions a week, though that number will soon go up to 10, she says.
“After they put a needle in her foot, she slept for over an hour, and woke up smelling like a can of creamed corn, from the chemicals,” Steve recalls. “It was the most beautiful smell you could smell.” Isabella’s speech abilities were immediately improved, he adds — “like night and day.” She’s now up to about 60 words, he adds, and though is still relying on extra speech-therapy services, “the biggest thing is that she picks up new words without telling us, and that catches us by surprise all the time.”
The cost of the procedure, Kurtzberg says, averages $7,500 to $10,000, and is only sometimes covered by insurance. In the Barneys’ case, the family’s insurance covered about 40 percent. “It was very worth it,” Steve says — especially the cord blood banking part. “I suggest it to everybody, because you just never know.”
(Top photo: Steve Barney)
Please follow @YahooParenting on Facebook, Twitter, Instagram, andPinterest. Have an interesting story to share about your family? Email us at YParenting (at) Yahoo.com.


