Health
- HealthNBC News
Are migraines getting worse?
New research suggests that climate change, which causes more erratic and severe weather conditions, may be a trigger for more intense migraines.
4 min read - HealthYahoo Life
Drinking at the beach can be risky. Here's what experts want you to know about dehydration, drowning.
Here's what experts suggest to avoid the pitfalls that come with drinking at the beach, pool or lake.
4 min read - HealthAssociated Press
Hawaii study shows almost 75% of Maui wildfire survey participants have respiratory issues
A University of Hawaii study examining the health effects of last year's deadly wildfires on Maui found that up to 74% of participants may have difficulty breathing and otherwise have poor respiratory health, and almost half showed signs of compromised lung function. Researchers released early results from that research on Wednesday. Dr. Alika Maunakea, one of the researchers and a professor at the university's John A. Burns School of Medicine, said those who reported higher exposure to the wi
3 min read - HealthNBC News
To protect new mothers, a federal panel prescribes maternity centers for mental health support
Many new mothers in the U.S. don't get treatment for depression or opioid use because there's no widely deployed system for mental illness screening in the first year after giving birth.
8 min read - HealthThe New York Times
Diabetes, heart problems and kidney disease are closely linked
Heart disease, diabetes and kidney disease are among the most common chronic illnesses in the United States — and they’re all closely connected. Adults with diabetes are twice as likely to have heart disease or a stroke compared with those who don’t have diabetes. People with diabetes — Type 1 and Type 2 — are also at risk of developing kidney disease. And when the kidneys don’t work well, a person’s heart has to work even harder to pump blood to them, which can then lead to heart disease. The t
4 min read - HealthWashington Post
Advice for picky eaters: Liking a variety of foods linked with brain health
Older people who aren’t picky eaters appear to have better brain health than those who prefer more limited diets, according to a large study of British adults. The research tracked the dietary preferences of nearly 182,000 older adults in Britain. The study was unusual because rather than focusing on the health effects of a particular diet, it examined the link between the foods individuals liked and disliked and their mental well-being and cognitive health.Subscribe to The Post Most newsletter
4 min read - HealthUSA TODAY
FDA approves self-tests for cervical cancer, as an alternative to the dreaded pelvic exam
FDA approved a new method to screen for cervical cancer, using two self-screening tools.
6 min read - BusinessBusiness Insider
Neuralink knew years ago that wires from its brain chip could retract and cause it to malfunction, report says
Noland Arbaugh received Neuralink's implant in January, but it didn't quite go to plan as some of the wires pulled away from his brain weeks later.
2 min read - USUSA TODAY
'Salvation' in polished nails and fashion tips, as CDC tackles suicide deaths
Suicide deaths in the U.S. surpassed 49,000 deaths in 2022, for the second consecutive year.
5 min read - HealthYahoo Life
Sucking in your stomach, waiting to use the bathroom: Here are 7 things pelvic floor health expert Sara Reardon wants you to stop doing
A pelvic health expert shares why you shouldn't hold it — and why your bathroom might need a stool.
5 min read - BusinessReuters
Roche shares jump on obesity drug results from early-stage trial
(Reuters) -Roche shares gained as much as 4.7% on Thursday after an early-stage trial showed that a newly-acquired obesity drug candidate led to significant weight loss, a key step in Swiss drugmaker's race to join the booming obesity treatment market. Roche said the study in the first of three trial stages required for regulatory approval showed the compound known as CT-388 yielded weight loss of 18.8%, when adjusted for a placebo effect, after 24 weeks in otherwise healthy adults with obesity
3 min read - BusinessReuters
AstraZeneca's COVID prevention drug cuts risk of disease in vulnerable patients
The long-acting antibody therapy called sipavibart showed a "statistically significant reduction" in symptomatic COVID-19 cases among immunocompromised patients, the company said. Immunocompromised people include those with blood cancer, organ transplant recipients, patients with end-stage renal disease requiring dialysis, patients receiving B-cell depleting therapy within the past year, and those taking immunosuppressive medications, it said. These patients make up about 25% of COVID-19 hospi
1 min read - BusinessReuters
Pfizer offers up to $250 million to settle Zantac cancer lawsuits, FT reports
The drugmaker was set to pay between $200 million and $250 million in the settlement, the newspaper reported, citing two people briefed on the deal. The settlement was disclosed in a court filing in Delaware last week, and is aimed at reducing Pfizer's potential liability, the report added. Pfizer did not immediately reply to Reuters' request for comment.
1 min read - HealthYahoo Life
Raw milk's popularity is surging. Here's why experts say that's dangerous.
Despite the current outbreak of bird flu among dairy cattle, sales of raw milk continue to rise — and experts say there are no benefits that outweigh the risks of illness from untreated dairy.
5 min read - HealthGood Morning America
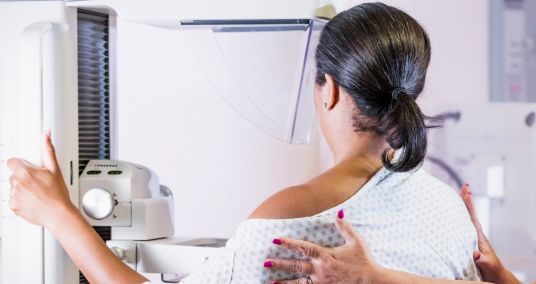
Major disparities exist in women of color's access to breast cancer care, report finds
A major new report shows stark disparities in breast cancer care, with non-white Americans and those without health insurance far less likely to be up to date with recommended screenings. Women under the age of 65 who do not have health insurance are 50% less likely to be up to date with breast cancer screening, according to the findings of the 2024 AACR Cancer Disparities Progress Report 2024, released Wednesday by the American Association for Cancer Research, a nonprofit organization focused
3 min read - HealthReuters
US FDA approves expanded use of Bristol Myers' cancer cell therapy (May 15)
The U.S. health regulator on Wednesday approved the expanded use of Bristol Myers Squibb's cancer cell therapy Breyanzi for the treatment of adults with a type of blood cancer called follicular lymphoma, that has returned or has not responded to prior treatments. The Food and Drug Administration's decision marks the fourth approval for Breyanzi, which can now be used to treat follicular lymphoma patients who have received two or more prior lines of therapy. The approval provides an option with
2 min read - HealthCBS News
More employees are cheating on workplace drug tests. Here's how.
Experts call for better drug testing procedures as more states legalize marijuana and societal norms change.
3 min read - HealthVerywell Health
Relieving Hormonal Headaches: What Helps?
Hormonal headaches from estrogen and progesterone fluctuations happen around menstruation, menopause, and in pregnancy. Learn what relieves head pain.
8 min read - LifestyleYahoo Life
Extreme heat can be dangerous for kids. Here's how to keep them safe in high temperatures.
"Kids' bodies produce heat faster than adults and they can't get rid of that heat as quickly," an expert warns.
5 min read - BusinessGood Morning America
Walgreens announces it will sell generic version of over-the-counter Narcan
Walgreens Boots Alliance announced Wednesday that it plans to sell its own generic version of the overdose reversal drug Narcan. Narcan is given as a nasal spray and the active ingredient in the medication -- naloxone -- can quickly restore breathing if someone is experiencing an opioid overdose and if it is administered in time. In March 2023, the U.S. Food and Drug Administration approved Narcan to be distributed without a prescription -- a milestone advocates have said will make it easier t
3 min read - EntertainmentAssociated Press
Movie Review: ‘Babes’ is a giddy, raunchy, moving and (very) gooey look at childbirth and friendship
“They don't tell you about this part,” notes her friend, Dawn. “Babes,” written by Glazer with Josh Rabinowitz, loves bodily secretions of any kind. This is a film about two women, Eden and Dawn, lifelong buddies, and how pregnancy and childbirth change them.
5 min read - HealthCBS News
Scams on TikTok targeting weight loss drugs
A joint investigation by Digital Citizens Alliance and Coalition for a Safer Web found dozens of TikTok profiles offering to ship weight loss drugs for lower prices and without a prescription. In nearly every situation, it was a scam.
3 min read - USNBC News
Overdose deaths decreased for first time in 5 years but still topped 100,000
Drug overdose deaths decreased slightly last year, falling for the first time since 2018, early data from the Centers for Disease Control and Prevention published Wednesday shows.
5 min read - LifestyleWashington Post
Even remote and hybrid work can burn you out. Here’s how to avoid it.
We’ve entered a new era of work: One where rules have been bent and lines blurred. Many workers feel simultaneously less connected and more stressed by digital communication tools. The result is burnout, or feeling exhausted or cynical about your job. Burnout doesn’t care if you work exclusively from the comfort of your home. It can happen if you have a light workload, if you like your colleagues, even if you’re passionate about what you do.Subscribe to The Post Most newsletter for the most impo
6 min read - USAssociated Press
Fewer US overdose deaths were reported last year, but experts say it's too soon to celebrate
The number of U.S. fatal overdoses fell last year, according to Centers for Disease Control and Prevention data posted Wednesday. It would be only the second annual decline since the current national drug death epidemic began more than three decades ago. Another noted that the last time a decline occurred — in 2018 — drug deaths shot up in the years that followed.
4 min read - BusinessVerywell Health
FDA Recalls Insulin Pump App After 200+ Injuries
The FDA has recalled the t:connect insulin pump app over reports that it crashes and drains the pump's battery, causing it to shut down.
3 min read - USGood Morning America
Drug overdose deaths fell in 2023, 1st decrease in 5 years: CDC
Drug overdose deaths fell in 2023, marking the first decrease in five years, new provisional federal data published Wednesday showed. An estimated 107,543 Americans died of drug overdoses in 2023, according to the Centers for Disease Control and Prevention's National Center for Health Statistics. This is a 3% decrease from the estimated 111,029 overdose deaths that occurred in 2022 and the first annual decrease in drug overdose deaths since 2018.
3 min read - BusinessNBC News
Walgreens is launching a generic version of over-the-counter Narcan
Walgreens said Wednesday that it will sell its own generic version of over-the-counter Narcan, the lifesaving opioid overdose reversal drug that first rolled out to drugstore shelves last fall.
2 min read - BusinessReuters
Walgreens launches own brand of opioid overdose reversal drug
The launch comes weeks after Walgreens' brand was approved by the U.S. Food and Drug Administration in April. Opioid abuse has plagued the United States for more than two decades and killed more than half a million Americans, with fentanyl and synthetic versions being a major culprit in recent years, according to government data. Naloxone rapidly reverses or blocks the effects of opioids, restoring normal respiration, especially when given within minutes of the first signs of an overdose.
1 min read - HealthVerywell Health
Causes of Thumb Pain and Treatment Options
Thumb pain could happen with repeated strain from phone use or video games. Learn when thumb pain in the joint signals arthritis and other conditions.
7 min read - HealthGood Morning America
What Kristen Bell actually packs in her kids' lunch boxes
Like many parents, Kristen Bell regularly flips over food labels to read the nutrition facts -- only to find herself dissatisfied and exhausted after scanning packages with overwhelmingly high sugar contents. In an effort to effect positive change, the actress and mother of two announced she's teaming up with former first lady Michelle Obama to help champion a healthier generation of kids nutrition. "I am at a constant impasse with my kids of encouraging them to consume healthy options -- part
5 min read - USCBS News
Aldi recalls cream cheese spread sold in 28 states for possible salmonella contamination
A string of recalls connected to Wisconsin-based supplier Schreiber Foods has now extended to Aldi stores after similar recalls at Hy-Vee and other grocery chains.
2 min read - HealthAssociated Press
If you’ve tried meditating but can’t sit still, here’s how — and why — to try again
The first time Marcelle Hutchins sat down to meditate, she put on a guided session, relaxed her shoulders and tried to close her eyes. “I had a deadline, and I thought, ’I don’t know if I can sit still this long,'” said Hutchins, who was working as a radio journalist. Hutchins has since become a certified meditation teacher — and serves as an example that busy, restless people who try once should try again.
4 min read - WorldThe Conversation
Florence Nightingale overcame the limits set on proper Victorian women – and brought modern science and statistics to nursing
Among her 5 decades of accomplishments, Nightingale founded the world’s first nursing school and advocated health care for all.
7 min read - WorldAssociated Press
UN agency authorizes second vaccine against dengue amid outbreaks in the Americas
The World Health Organization on Wednesday authorized a second dengue vaccine, a move that could provide protection for millions worldwide against the mosquito-borne disease that has already sparked numerous outbreaks across the Americas this year. In a statement on Wednesday, the U.N. health agency said it approved the dengue vaccine made by the Japanese pharmaceutical Takeda, recommending its use in children between six to 16 years old living in regions with high rates of dengue. The two-dos
2 min read - USNBC News
More than half of Black women ages 15-49 live with little to no abortion access
57% of Black women ages 15-49 live in states with abortion bans, heavy restrictions or plans to implement them, according to a new report from a pair of reproductive rights organizations.
4 min read - WorldBusiness Insider
A lawyer who wrote a book about sleepwalking is cleared of misconduct after she dozed off for 2 hours during an inquest
A British barrister was representing a nurse witness but nodded off and missed her client giving evidence during a coroner's inquest.
2 min read - WorldReuters
WHO clears Takeda's dengue vaccine
The approval, called a prequalification, comes amidst a surge in mosquito-borne viral infections across Asia, Africa, and the Americas, including new spread into previously unaffected areas. Takeda's vaccine, given in two doses over a three-month interval, protects against four serotypes of the dengue virus. It was cleared by WHO for use in children aged 6 to 16 in areas with high infection rates.
1 min read - BusinessReuters
Exclusive-Musk's Neuralink has faced issues with its tiny wires for years, sources say
Neuralink's disclosure last week that tiny wires inside the brain of its first patient had pulled out of position is an issue the Elon Musk company has known about for years, according to five people familiar with the matter. The company knew from animal testing it had conducted ahead of its U.S. approval last year that the wires might retract, removing with them the sensitive electrodes that decode brain signals, three of the sources said. Neuralink deemed the risk low enough for a redesign n
5 min read - BusinessBusiness Insider
These are the 13 mental health startups that could IPO, make acquisitions, or get bought this year, according to analysts
Analysts named these mental health companies as top targets for M&A or public market debuts.
14 min read - WorldReuters
New Zealand looking into Indian spice brands over contamination
New Zealand's food safety regulator on Wednesday said it is investigating possible contamination in spice products of top Indian brands MDH and Everest after they faced scrutiny in other countries. The United States and Australia have been looking into contamination after Hong Kong last month suspended sales of three spice blends of MDH and one of Everest, saying they contained high levels of a cancer-causing pesticide, ethylene oxide. In a statement to Reuters, the regulator, New Zealand Food
1 min read - BusinessReuters
Novo Nordisk owner buys majority stake in Austrian life science tools company
Novo Holdings, the controlling shareholder of Danish obesity drugmaker Novo Nordisk, said on Wednesday it would buy a controlling stake of about 60% in Single Use Support, an Austria-based life science tools company. Novo Holdings is the investment arm of the Novo Nordisk Foundation and has 77% of voting shares in Novo Nordisk, which produces blockbuster obesity drug Wegovy and diabetes treatment Ozempic. Novo Holdings CEO Kasim Kutay told Reuters in October that the huge Wegovy windfall would
2 min read - WorldReuters
No shortage of Wegovy weight-loss drug in Denmark, Novo Nordisk says
Novo Nordisk does not expect a shortage of its Wegovy weight-loss drug in Denmark despite an earlier warning by the Danish Medicines Agency of strained supply of two separate doses in the coming weeks, the company said. The Danish regulator on Monday issued two statements saying the country faced a shortage of the Wegovy Flextouch 1 mg injection pen from late May to mid-June and the 0.5 mg Wegovy Flextouch injection pen between mid-June and mid-July. "Novo Nordisk is experiencing a high demand
1 min read - HealthNBC News
Bird flu virus possibly found in a handful of wastewater sites, CDC says
There’s no solid evidence that bird flu is spreading among people, the Centers for Disease Control and Prevention said Tuesday amid an outbreak of the virus in dairy cows.
2 min read - BusinessReuters
Eisai starts rolling submission for injectable version of Alzheimer's drug with US FDA
The companies are seeking the Food and Drug Administration's (FDA) approval of a weekly dose of Leqembi to be given as an under-the-skin injection. Under a rolling submission the regulator assesses the data as and when it becomes available, and the process continues until there is enough data for a formal marketing application.
2 min read - USABC News
8 teens taken to hospital after ingesting marijuana edibles during school field trip: Authorities
Eight teenagers got "acutely ill" and were transported to the hospital after ingesting marijuana edibles during a field trip to the La Brea Tar Pits in Los Angeles, authorities said. An on-site security officer found the sickened male and female students and called 911 around 2:30 p.m. PT Tuesday, the Los Angeles Fire Department said. "LAFD Paramedics arrived quickly to determine each had an altered level of consciousness, following their reported ingestion of cannabis edibles," LAFD said in a
1 min read - LifestyleCBS News
Philadelphia health care company provides culturally competent care for Asian communities
The founder of Century Health Care in Philadelphia helps connect caregivers and clients who have similar cultural backgrounds.
2 min read - HealthUSA TODAY
Seriously, don't drink the raw milk: Social media doubles down despite bird flu outbreak
Raw milk fans are going as far as intentionally seeking out unpasteurized dairy products contaminated with H5N1 to consume for perceived "benefits."
5 min read - HealthYahoo Life
Words matter when it comes to healthy aging and your current well-being, a new study finds. Here's what to know.
People who open up about their feelings toward aging tend to have better current well-being, study finds.
4 min read - HealthUSA TODAY
In states with abortion restrictions, 8,000 people each month get abortion pills elsewhere
A new survey by #WeCount found that around 8,000 women a month in restricted states receive the abortion pill by mail thanks to telehealth options.
2 min read