Emotional support animals can endanger the public and make life harder for people like me who rely on service dogs

In 2017, Marlin Jackson boarded a cross-country flight. When he got to his row, another passenger was already in the middle seat with an emotional support dog in his lap.
According to Mr. Jackson’s attorney, “The approximately 50-pound dog growled at Mr. Jackson soon after he took his seat…and continued as Mr. Jackson attempted to buckle his seatbelt. The growling increased and the dog lunged for Mr. Jackson’s face…who could not escape due to his position against the plane’s window.” Facial wounds requiring 28 stitches were the result.
Untrained emotional support dogs don’t just attack people. They attack highly trained service dogs, as well, sometimes ending their working lives.
I can relate. I am a visually impaired person partnering with my fourth guide dog over a 20-year period. In the past decade, I have increasingly needed to cope with clueless handlers allowing their pets to interfere with my dog’s work.
As a professor of ethics, I teach students to consider first the needs of the most vulnerable. I wish I could teach the same lesson to those who risk public safety with their ill-trained dogs, most of whom are emotional support animals, a category not recognized by the Americans with Disabilities Act.
Dogs, dogs, dogs
Over the past decade, purported emotional support animals have increasingly appeared in stores, restaurants and airports. While peacocks, pigs and kangaroos make the headlines, almost all the animals found in no-pet zones are dogs. Dog biting, barking, growling, urinating and defecating are top complaints, with one airline reporting an 84% increase in dog-related incidents from 2016-2018.
The influx of inappropriate dogs has also generated unwarranted suspicion toward the approximately 10,000 Americans who, like me, partner with legitimate, trained guide dogs.
Animal public access in the U.S. is currently governed by a patchwork system of inconsistent laws, creating confusion for people with disabilities, citizens and, particularly, gatekeepers – the store managers, restaurant owners and building supervisors tasked with deciding which dogs should be allowed in their no-pet spaces.
In other countries, IDs are issued only to professionally trained service dogs who have demonstrated ability to behave in public. In the U.S., there is no such validation. As a result, pet owners have become increasingly brazen in fraudulently claiming their animals warrant legal public access.
Service dogs versus emotional support animals
The Department of Justice, which enforces the Americans with Disabilities Act, allows people with physical, sensory, psychiatric, intellectual or mental impairments to have public access with service dogs who have been individually trained to perform tasks that mitigate their owners’ disabilities.
The Department of Transportation and Department of Housing and Urban Development allow service dogs on public transportation and in housing, respectively, but also grant access to people with mental and emotional disorders accompanied by emotional support animals – untrained animals who need only to contribute to their owners’ emotional well being, as any good pet would.
Technically, the individual seeking access with an emotional support animal must have certification of a mental or emotional disorder, which is a much lower standard than the disability requirement of DOJ.
Some mental health professionals have been willing to attest to an individual’s “need” for an emotional support animal without having a professional relationship with them. And none vouches for the appropriateness of specific animals.
ADA service dogs may legally accompany their handlers almost anywhere. Emotional support animals may not. For example, emotional support animals currently allowed in aircraft cabins are not legally permitted in airport shops and restaurants. Emotional support animals allowed to live in college dorms may not go with their owners to class or the cafeteria.
Online purveyors of official-looking letters, vests and patches guaranteed to get dogs access in pet-free zones take advantage of the confusion between service dogs and emotional support animals, liberally mixing the classifications. They also fail to mention that the individual seeking such accommodation must have proof of a mental disorder. This omission, itself, is an ethical problem.
A predicament for gatekeepers
Gatekeepers have to weigh the consequences of confronting an individual accompanied by a dog. Denial of access to a disabled handler with a legitimate service dog can result in a US,000 fine by the DOJ. The fine for a handler who falsely portrays a pet as a service dog or emotional support animal ranges from
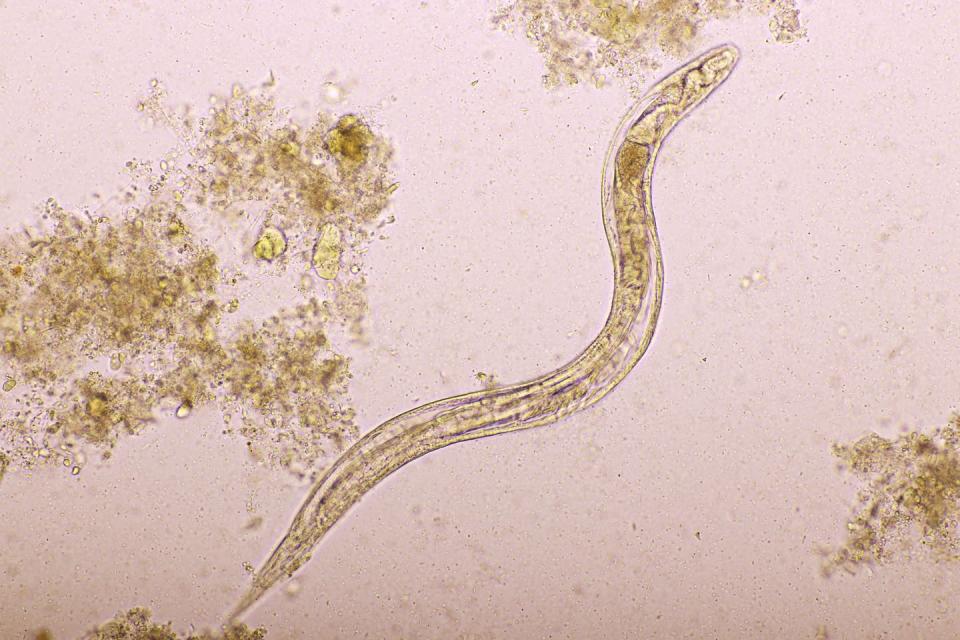
0 to Ivermectin is an over 30-year-old wonder drug that treats life- and sight-threatening parasitic infections. Its lasting influence on global health has been so profound that two of the key researchers in its discovery and development won the Nobel Prize in 2015. I’ve been an infectious disease pharmacist for over 25 years. I’ve also managed patients who delayed proper treatment for their severe COVID-19 infections because they thought ivermectin could cure them. Although ivermectin has been a game-changer for people with certain infectious diseases, it isn’t going to save patients from COVID-19 infection. In fact, it could cost them their lives. Let me tell you a short story about the history of ivermectin. Ivermectin was first identified in the 1970s during a veterinary drug screening project at Merck Pharmaceuticals. Researchers focused on discovering chemicals that could potentially treat parasitic infections in animals. Common parasites include nematodes, such as flatworms and roundworms, and arthropods, such as fleas and lice. All of these infectious organisms are quite different from viruses. Merck partnered with the Kitasato Institute, a medical research facility in Japan. Satoshi Omura and his team isolated a group of chemicals called avermectin from bacteria found in a single soil sample near a Japanese golf course. To my knowledge, avermectin has yet to be found in any other soil sample in the world. Research on avermectin continued for approximately five years. Soon, Merck and the Kitasato Institute developed a less toxic form they named ivermectin. It was approved in 1981 for commercial use in veterinary medicine for parasitic infections in livestock and domestic pets with the brand name Ivomec. Early experiments by William Campbell and his team from Merck discovered that the drug also worked against a human parasite that causes an infection called river blindness. River blindness, also known as onchocerciasis, is the second leading cause of preventable blindness in the world. It is transmitted to humans from blackflies carrying the parasitic worm Onchocerca volvulus and occurs predominantly in Africa. Ivermectin underwent trials to treat river blindness in 1982 and was approved in 1987. It has since been distributed free of charge through the Mectizan Donation Program to dozens of countries. Thanks to ivermectin, river blindness has been essentially eliminated in 11 Latin American countries, preventing approximately 600,000 cases of blindness. These two decades of extensive work to discover, develop and distribute ivermectin helped to significantly reduce human suffering from river blindness. It’s these efforts that were recognized by the 2015 Nobel Prize in Physiology or Medicine, awarded to both William Campbell and Satoshi Omura for their leadership on this groundbreaking research. Infectious disease researchers frequently attempt to repurpose antimicrobials and other medications to treat infections. Drug repurposing is attractive because the approval process can happen more quickly and at a lower cost since nearly all of the basic research has already been completed. In the years since it was approved to treat river blindness, ivermectin was also shown to be highly effective against other parasitic infections. This includes strongyloidiasis, an intestinal roundworm infection that affects an estimated 30 to 100 million people worldwide. Another example is amphotericin B, originally approved to treat human yeast and mold infections. Researchers discovered it can also be an effective treatment for severe forms of leishmaniasis, a parasitic infection prevalent in tropical and subtropical countries. Likewise, doxycycline is an antibiotic used for a wide variety of human bacterial infections such as pneumonia and Lyme disease. It was later found to also be highly effective in preventing and treating malaria. Not every attempt at repurposing a drug works as hoped, however. At the start of the pandemic, scientists and doctors tried to find inexpensive medications to repurpose for the treatment and prevention of COVID-19. Chloroquine and hydroxychloroquine were two of those drugs. They were chosen because of possible antiviral effects documented in laboratory studies and limited anecdotal case reports from the first COVID-19 outbreaks in China. However, large clinical studies of these drugs to treat COVID-19 did not translate to any meaningful benefits. This was partly due to the serious toxic effects patients experienced before the drugs reached a high enough dose to inhibit or kill the virus. Unfortunately, lessons from these failed attempts have not been applied to ivermectin. The false hope around using ivermectin to treat COVID-19 originated from an April 2020 laboratory study in Australia. Although the results from this study were widely circulated, I immediately had serious doubts. The concentration of ivermectin they tested was 20 to 2,000 times higher than the standard dosages used to treat human parasitic infections. Indeed, many other pharmaceutical experts confirmed my initial concerns within a month of the paper’s publication. Such high concentrations of the drug could be significantly toxic. Another commonly cited paper on ivermectin’s purported effects against COVID-19 was withdrawn in July 2021 after scientists found serious flaws with the study. These flaws ranged from incorrect statistical analyses to discrepancies between collected data and published results to duplicated patient records and the inclusion of study subjects who died before even entering the study. Even more concerning, at least two other oft-cited studies have raised significant concerns about scientific fraud.
Developing ivermectin for animal use
Developing ivermectin for human use
Repurposing drugs for other uses
Repurposing drugs for COVID-19
At the time of this writing, two large randomized clinical trials both showed no significant benefit from the use of ivermectin for COVID-19. Reputable national and international health care organizations, including the World Health Organization, the Centers for Disease Control and Prevention, the National Institutes of Health, the Food and Drug Administration and the Infectious Diseases Society of America, unanimously recommend against the use of ivermectin to prevent or treat COVID-19 unless in the context of a clinical trial.
Consequences of using ivermectin for COVID-19
Unfortunately, many organizations with dubious intentions have continued to promote unsubstantiated use of invermectin for COVID-19. This has led to a dramatic rise in ivermectin prescriptions and a flood of calls to U.S. poison control centers for ivermectin overdoses. Many calls were due to ingestion of large amounts of veterinary products containing ivermectin – two deaths linked to ivermectin overdose were reported in September 2021.
Ivermectin, when used correctly, has prevented millions of potentially fatal and debilitating infectious diseases. It’s meant to be prescribed only to treat infections caused by parasites. It’s not meant to be prescribed by parasites looking to extract money from desperate people during a pandemic. It’s my sincere hope that this unfortunate and tragic chapter in the otherwise incredible story of a lifesaving medication will come to a quick end.
Article updated to indicate that the brand name for veterinary ivermectin is Ivomec
[Like what you’ve read? Want more? Sign up for The Conversation’s daily newsletter.]
This article is republished from The Conversation, a nonprofit news site dedicated to sharing ideas from academic experts. It was written by: Jeffrey R. Aeschlimann, University of Connecticut.
Read more:
New treatments for COVID-19 may stave off the worst effects of the virus
Get ready for the invasion of smart building technologies following COVID-19
Jeffrey R. Aeschlimann has received funding from the NIH for collaborative research projects focusing on bacterial antibiotic resistance.