Drug-Resistant Superbugs Kill At Least 23,000 People in the U.S. Each Year
Each year, more than two million people in the United States develop antibiotic-resistant infections, and at least 23,000 of them die as a result, says the first-ever national snapshot of the issue. That toll only rises when other conditions exacerbated by these infections are included in the count. Because it’s difficult to attribute a death directly to antibiotic-resistant microbes (as opposed to illnesses that put the person in the hospital to begin with), the U.S. Centers for Disease Control and Prevention says these figures probably underestimate the scale of the problem.
CDC today released the findings as part of a blueprint for addressing the issue, which the agency says is an urgent and growing threat. “Even when alternative treatments exist, research has shown that patients with resistant infections are often much more likely to die, and survivors have significantly longer hospital stays, delayed recuperation and long term disability,” wrote CDC director Thomas Frieden.
The report authors ranked 18 microorganisms associated with drug resistance as urgent, serious or concerning by considering the pathogens’ clinical and economic impact alongside current and future projected incidence; transmissibility; availability of effective antibiotics; and barriers to prevention. Healthcare costs that arise from antibiotic resistance are challenging to pin down, but previous non-CDC estimates suggest that it can boost healthcare costs annually by $20 billion and cost another $35 billion in lost productivity.
“Urgent threats” to human health include the serious diarrheal infection Clostridium difficile, a family of germs that includes Escherichia coli called Carbapenem-resistant enterobacteriaceae (CRE), and Drug-resistant Neisseria gonorrhoeae-the bacteria responsible for the sexually transmitted infection gonorrhea. Collectively, they claim more than 14,500 lives each year, primarily from C. difficile. Although resistance to the antibiotics that treat C. difficile infections is not yet a problem, CDC included it in the list because it is naturally resistant to many drugs used to treat other infections which enables it to spread quickly.
Microbes that present “serious threats,” according to CDC, include multidrug-resistant Acinetobacter, drug-resistant Campylobacter, and fluconazole-resistant Candida (a fungus) and drug-resistant tuberculosis, among others. “Concerning threats” include Vanomycin-resistant Staphyloccous aureus (VRSA).
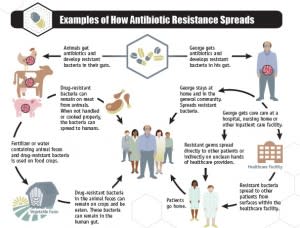
Antibiotic-resistance most often arises when commercial antibiotics kill good bacteria that protect the body from infection alongside bacteria that cause illness-setting the stage for drug-resistant bacteria to flourish and take over. Some drug-resistant bacteria are then able to exchange genes with other bacteria, spreading resistance and helping sideline drugs normally capable of treating infection.
CDC scientists have long said that the overuse of antibiotics in both humans and animals has contributed to the spread of drug-resistant “superbugs.” In fact, multiple studies during the last decade have found that about half of all antibiotics prescribed in the U.S. are not needed or are inappropriate.The most acute antibiotic resistance problems arise in hospitals, Frieden said today on a conference call. “The most resistant organisms in hospitals are emerging in those settings because of poor antimicrobrial stewardship among humans.”
Antibiotic resistance poses a particular threat to people with compromised immune systems, such as patients undergoing chemotherapy or complex surgeries or individuals with chronic diseases such as diabetes, asthma or rheumatoid arthritis. Most deaths linked to antibiotic-resistant infections happen in hospitals and nursing homes.
Image: CDC
CDC’s prescription for combating these infections has four main components: Preventing infections and the spread of resistance; better tracking of resistant bacteria in order to understand the scope of the problem; improving the use of current antibiotics; and promoting the development of new antibiotics and better diagnostic tests for resistant bacteria.
The report does not say exactly how those objectives should be achieved or how much such an effort would cost. It does, however, recommend steps that states and communities, health providers, healthcare officials, and patients can take. Hospital patients, for example, should insist everyone wash their hands before touching them.
Image: CDC
Two budget items on CDC’s wishlist for FY 2014 give some insight into how the agency hopes to improve its antibiotic-resistance efforts. In the President’s budget, CDC proposed an allocation of $40 million for a new Advanced Molecular Detection initiative, which would advance technologies such as high-throughout genome sequencing and improving bioinformatics. The agency also requested an increase of about $12.5 million for improvements to the National Healthcare Safety Network, which provides an integrated reporting system for healthcare-associated infections. The funds would expand that system to another 1,800 facilities.
To calculate the toll from antibiotic-resistance in this national snapshot CDC gathered existing data on the proportion of antibiotic resistant isolates and multiplied it by the total number of cases or deaths attributed to that bacterium. Since there is no total count for several pathogens, CDC says their estimates of antibiotic-resistant infections are conservative.
Follow Scientific American on Twitter @SciAm and @SciamBlogs. Visit ScientificAmerican.com for the latest in science, health and technology news.
© 2013 ScientificAmerican.com. All rights reserved.