Crackdown on opioids has its own victims: People who need them to live
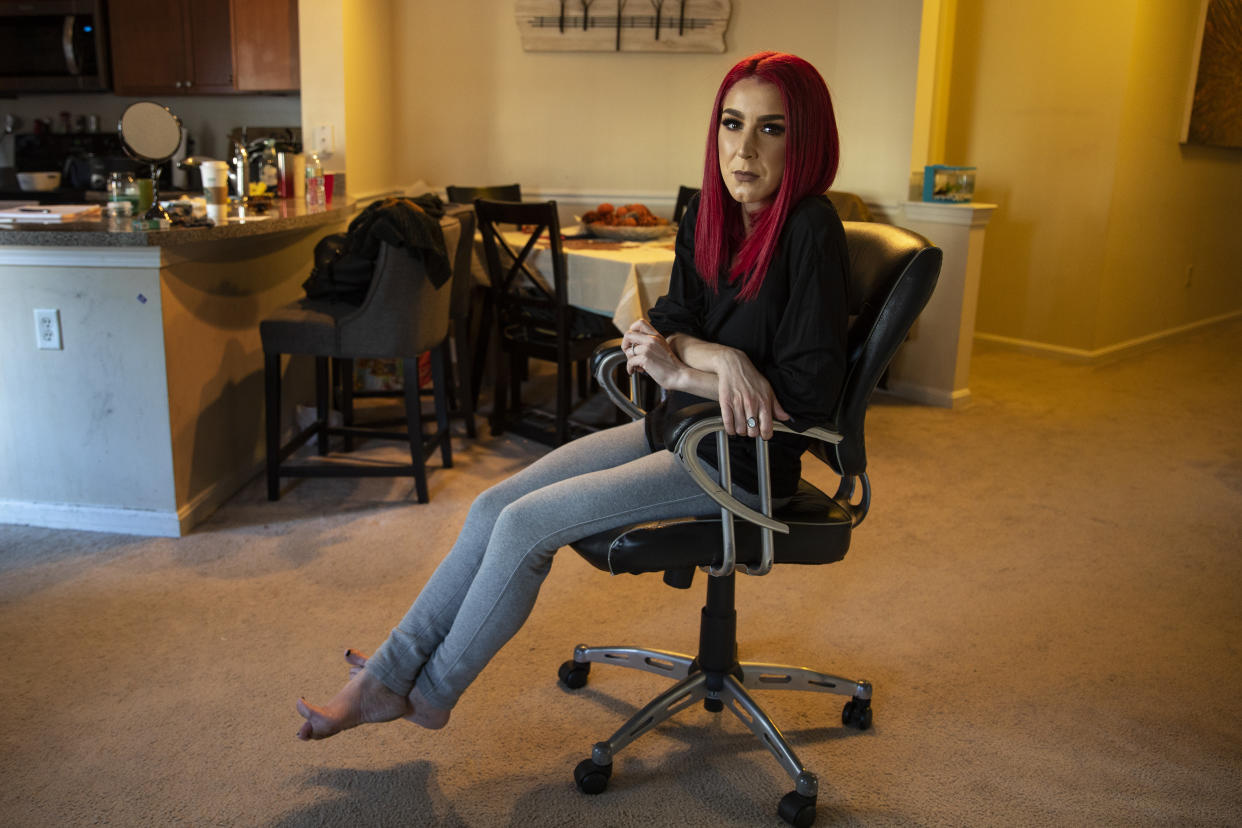
Caylee Cresta, 27, a wife and mother of a young son, is a victim of the opioid epidemic, although not in the way you might think. She doesn’t have needle tracks on her arms; she gets her dosages legally and has never overdosed. But she has a problem shared by many Americans who depend on painkillers to get through life: the well-intentioned effort to discourage doctors from writing unnecessary prescriptions has made opioids harder to get for people who actually need them.
Sometimes she runs out altogether.
“I hide on my really bad days,” she says — the times when she can’t get a prescription filled — “and on my better days, which are always days that I have my full dose of opioids in me, those are the days when people see me.”
Cresta has a rare condition called stiff person syndrome (SPS), which affects the brain and spinal cord and causes painful spasms that can be strong enough to break her bones. Sudden stimuli like stubbing a toe or a hug from behind can trigger a spasm that lasts for hours. While the disease is most common in people between the ages of 30 and 60, disabling them more and more over time, Cresta was 18 when she had her first spasm. It took a couple of years and dozens of doctors before she knew what was happening to her body.
“I was a senior in high school,” recalled Cresta. “I was sitting at lunch one day and I just got this terrible throbbing pain in my jaw. The first place I thought of was my dentist. Then they referred me to the orthopedic surgeon and when I got there, the nurses looked at my mouth. As she’s looking around, my jaw slams shut. And it stayed like that for 18 days … until somebody put me under anesthesia and broke it out of place.”
Cresta spent a year and a half seeing 30 different kinds of specialists before she was diagnosed with SPS. By this time, the muscle spasms had progressed down her body and in one instance, she could hear the bones in her hands breaking. Her doctor, a neurologist who specializes in rare diseases, offered opioids as a treatment to slow down her nervous system and help relieve the pain prompting the spasms, but Cresta refused to take them.

“I had grown up watching a fair amount of addiction” in her family, said Cresta. “I have seen what addiction could do.”
Eventually, after being confined to a wheelchair for months and in the emergency room with a spasm, Cresta acceded to a doctor’s insistence on giving her an intravenous opioid. After it was administered, she felt near instant relief.
When her neurologist again offered opioid medication as a treatment option, this time Cresta agreed. “Within 25 minutes of taking that first pill, my life completely changed,” she said. “It was like somebody handed me this little tiny piece of my life back. And as my willingness and the dosage grew, I got a bigger and bigger piece back.”
She added with a sigh, “Opioids saved my life.”
However, in recent years, due to the crackdown on opioid prescriptions, Cresta has increasingly encountered doctors unwilling to prescribe to her and pharmacies reluctant to fill her prescriptions. Caught between the fear of overdosing and of the prospect that their pain could drive them to suicide, people like Cresta are fighting to stay alive. While the blame for the epidemic is handed off from addicts to doctors to the pharmaceutical industry, chronic pain patients are collateral damage in a fight that leaves doctors wary of treating them.
In his State of the Union address Tuesday, President Trump boasted, “In the last Congress, both parties came together to pass unprecedented legislation to confront the opioid epidemic.” In October 2018, he had signed a bipartisan bill, the Support for Patients and Communities Act, to fight the crisis that claimed over 70,000 lives in 2017 and kills 115 every day. The bill would set new provisions for Drug Enforcement Administration’s opioid manufacturing quota, increase access to prescription monitoring databases, and require the Department of Health and Human Services to annually notify “outlier prescribers,” excluding those who have hospice or cancer patients or are already being investigated by the inspector general.
“So here’s this tragedy and here’s this message that something went wrong with the prescribing culture, said Stefan Kertesz, an addiction scholar and professor of medicine at the University of Alabama at Birmingham School of Medicine, told Yahoo News. “If that were all, that would be plenty to change physician behavior, [because] you can’t ignore 70,000 people dying.”
But, Kertesz continues: “It’s hard to think about the patient’s best interest when the doctor feels like they could be taken down at any moment.” He says every week or two he learns about a suicide related to reduced opioid supply. “And the patient who’s been on opioids for long-term pain comes to look like a serious threat and a liability to the physician’s own survival.”
Twenty-eight percent of medical professionals including doctors, nurses, pharmacists, chiropractors and physical therapists admitted to feeling complicit in the opioid crisis, according to a survey by Delphi Health Group, a rehab center in Florida. Forty percent of doctors said they are prescribing fewer opioids than in previous years.

“Most medical professionals believe they’ve prescribed opioids to an addict, so yes, we can say that the pressure is justifiable,” said Gesa Pannenborg of Delphi Health Group. “They are aware that they are sometimes portrayed as one of the villains when it comes to opioid deaths.”
Cresta felt the effects of this pressure on her doctors.
“A few years ago, primarily in 2016, everything started to get a little bit more uncomfortable,” she said. Her Connecticut-based doctor, who is a three-hour drive from Cresta’s home in Reading, Mass., started to receive letters from her state’s prescription drug monitoring program (PDMP). He also got letters from Connecticut, she said.
“My pill is a rare milligram,” said Cresta, who is prescribed opioids up to 400 morphine milligram equivalents (MME) per day, which is well over the over the 50 MME/day threshold for what is considered safe prescribing to avoid overdose. According to the Centers for Disease Control and Prevention’s guideline for prescribing opioids, “physicians are recommended to avoid increasing dosage to ≥90 MME/day or carefully justify a decision to titrate dosage to ≥90 MME/day.”
Between 2006 and 2017, the annual prescribing rate for high dosage opioid prescriptions (90 MME/day or more) declined by 56.5 percent. In 2017 alone, these prescriptions fell by 46.5 percent.
“With a high enough dose,” said Cresta, “opioids can stop me from spasming, but more than anything, they allow me to retain some functionality and keep some quality of life.” She adds that she’s never gotten high from the drug.
Even so, Cresta and her doctor, both fearful for the doctor’s practice and livelihood, agreed that she’d instead see a pain physician, someone who could prescribe her the high dosage she needed without being flagged. Finding a pain management doctor proved challenging. “They don’t know my disease,” said Cresta, who worried that her various doctor visits looked like “doctor shopping.” “I never got a script from any of those doctors,” she said, “but going to see multiple doctors doesn’t look good either.”
Not long after she’d found a doctor willing to take a risk on prescribing the high dosage she needs, Cresta was right back where she started. “One day I walked into [the doctor’s] office and she had gotten a letter from Medicare and Medicaid,” said Cresta, whose voice softened as she recalled the moment. “She said that she’s gotten this letter about her Medicare, Medicaid patients that said she was over the prescribing line. I’m on private insurance; that letter didn’t have anything to do with me, specifically. But she looked at me and she said, ‘For you as a high-dose opioid patient, you’re somebody that influences my prescribing and I have two kids to put through college.’”
Cresta said she sympathized with the doctor, but felt deeply hurt. “I left that day, and within two days one of my lungs had collapsed. Within three days after that, the other lung collapsed.” She inevitably returned to her specialist, the one who had received PDMP notices because of her dosages. “He said to me, ‘I’m not gonna let you die,’” said Cresta. “And he took me back on as a patient.”
With over 191 million opioid prescriptions dispensed to American patients in 2017, including those for methadone, OxyContin and Vicodin, according to the CDC, the opioid epidemic is a problem almost entirely confined to the U.S. There were nearly 218,000 lives lost to overdoses related to prescription opioids between 1999 to 2017. As a result, state and federal regulatory bodies are cracking down on prescribers.
Physicians like Ajay Manhapra told Yahoo News the pressure to prescribe — or not prescribe — opioids “becomes a damned-if-you-do-and-damned-if-you-don’t situation.”
“Five, 10 years back, I started tapering a lot of people because they were dysfunctional,” said Manhapra, who is now an addiction medicine specialist at a Virginia clinic, but previously worked in a hospital intensive care unit. “A bunch of them got better, a bunch of them kept coming back to the hospital.”

Manhapra said he made the “medical and ethical” decision to taper opioid prescriptions when he saw patients weren’t improving and were becoming dependent on the prescribed drugs. “I said to them, for your best interest, I’m not willing to make the prescriptions, but I will work with you, and if you don’t want that, I will recommend you to another physician.”
The backlash to his decision was swift and enduring. “I was written up so many times,” he told Yahoo News. “Nurses complained about me. Patients complained to the government about me. It was significant stress to stand up against this whole movement of prescribing opioids for anybody who [thinks they] deserve it.”
Today, Manhapra treats patients who are voluntarily trying to stem their opioid dependence, among other addictions. But years ago, not all of his patients chose to have their opioids tapered. It was his decision, one he felt confident about making.
But many physicians are making similar decisions based on outside pressure from regulators or insurers.
“In most circumstances. I would tell patients to trust their doctors when they have a medical problem or to trust their children’s doctors,” said Andrew Kolodny, president of Physicians for Responsible Opioid Prescribing (PROP) and co-director of opioid policy research at Brandeis University.
“But in the case of opioids,” continued Kolodny, “it’s hard because the reason we have this epidemic, the reasons so many Americans became opioid-addicted starting in the mid-’90s, is because doctors began to prescribe very aggressively.”
The epidemic began in 1996, when drugs like OxyContin hit the market and opioids were prescribed not only for terminal illnesses like cancer treatment but for relief from even routine pain, such as a toothache, instead of an over-the-counter NSAID. The national movement to reel in prescriptions, however, has left some patients in so much pain they attempt or commit suicide when their drugs are taken away.
“We were taught that opioids are safe and effective for common chronic conditions like lower back pain; we were told to give opioids,” reflected Koldony. “Chronic headaches — we were taught to give opioids. Fibromyalgia — we were taught to give opioids. You are much more likely to harm the patient than help them If you prescribed opioids aggressively like that.”
He also blamed the ongoing crisis on drug companies like OxyContin manufacturer Purdue Pharma and their “brilliant, multifaceted marketing campaign disguised as education.”
“The answer there isn’t so much restricting what doctors can do,” said Kolodny, “the answer is restricting what drug companies can do. We need better regulation of the drug companies so that the doctors can make the decision on the basis of medical evidence without drug companies influencing what they’re doing and giving them deceptive information.”
Currently, Purdue Pharma is being sued by the Massachusetts attorney general, who’s accused the company of misleading doctors into prescribing potentially addictive OxyContin. According to court documents released mid-January, Purdue executives planned to “bury the competition” in a “blizzard of prescriptions” and blamed the crisis on abusers, who they referred to as “reckless criminals.”
Yet the fight against the opioid epidemic has fallen squarely on doctors’ shoulders.
“To protect public health, we must continue to improve opioid-prescribing practices,” wrote Dr. Gery Guy, a health economist at the CDC, in an email to Yahoo News. “Almost all prescription drugs involved in overdoses come from prescriptions originally. … However, once they are prescribed and dispensed, prescription drugs are frequently diverted to people using them without prescriptions.”
The CDC guidelines for prescribing opioids provide recommendations that are “are voluntary, rather than prescriptive standards,” said Guy. Still, as of last year, over a dozen states have turned the guideline’s dosage and duration limits — “start low and go slow” — into laws. In many cases, they are indiscriminately applied to all chronic pain patients, despite being unsuitable for people with cancer or other certain serious illnesses. The risk of addiction then outweighs pain relief for someone with a terminal disease.
The CDC says it has documented a connection between prescribed opioids and illicit drugs. “Opioid overdoses related to prescription opioids and heroin have taken the lives of too many Americans,” said Guy. “In 2017, prescription opioid overdose took the lives of 17,087, heroin overdoses took the lives of 15,482, and synthetic opioids other than methadone (such as illicitly manufactured fentanyl) took the lives of 28,466 Americans. These epidemics are closely related. The dramatic increases we see in opioid overdoses are a tragic consequence of exposing too many people to prescription opioids.”
It is this “crossover,” as Cresta put it, that stigmatizes legitimate opioid users as drug addicts.

But a just-published study projects that “interventions targeting prescription opioid misuse such as prescription monitoring programs may have a modest effect, at best, on the number of opioid overdose deaths in the near future.”
“Even patients who have been on therapeutic doses of opioids for a long time, with no evidence of other problems like substance use disorders, are being involuntarily tapered because physicians or other prescribers are afraid,” said Kelly Dineen, co-director of the Bander Center for Medical Business Ethics at Saint Louis University. “It’s not great for anybody to have an opioid use disorder no matter what the substance is. But, frankly, it’s probably less dangerous to have opioid use disorder when you’re using prescription drugs because at least there are quality controls on that.”
Beyond prescription limits, the CDC guidelines recommend technological surveillance like prescription drug monitoring programs (PDMP) that track which drugs are prescribed and dispensed to whom, how many and how often. The data is sent out in report cards, comparing doctors to their peers and influencing them to be more conservative with their prescription pads.
“They were meant to inform primary care physicians on what would be reasonable,” said Halena Gazelka, a practitioner of pain medicine at the Mayo Clinic, about the CDC guidelines. “But when we try to make absolutes out of them, that this is all you can give a patient and this patient is the same as another patient, it just doesn’t work because medicine is so individualized. And it has to be.”
Gazelka argued that the guidelines are based on data that may not capture the full spectrum of opioid users. “When someone comes in with an overdose, we don’t necessarily know whether they’re taking a prescription that they were given or that their mother was given or if they bought it on the street,” she said. “Trying to separate that out, where the prescriptions end up and who is really dying from them, is really difficult.”
Donna Meyer, a nurse and co-leader of Investors for Opioid Accountability, a coalition that scrutinizes the role of pharmacies like Walgreens in the opioid crisis, agrees with Gazelka’s critique but believes common sense restraint is warranted. “There shouldn’t be any dictator dictating how doctors do things, because every patient is different,” Meyer told Yahoo News. “But on the other hand, there should be guidelines and we should not go back to the ’90s, where we just gave 90 opioid pills to someone who broke their little finger.”
Cresta has tried non-opioid alternatives for her bone-breaking spasms, some of which have recently deformed her feet. “Plasmapheresis, IVIG (intravenous immunoglobulin) therapy, out-of-pocket stem cell trials,” listed Cresta. “Anything you can think of, I tried it.” But time and again, opioids, she said, proved most effective for treating her disease.
“The past three months I’ve had a brutal problem at the pharmacy,” she said, as she recalled a 13-hour day when she attempted to fill a prescription. A number of pharmacies have either refused to fill prescriptions for her or claimed the drug was out of stock.

“Nobody wants to bounce between pharmacies because you don’t want to be questioned, and you don’t want to be made out to be a criminal,” said Cresta. “But when you have pharmacists today that look at you and say, ‘I’m refusing to fill that,’ and that’s the only thing keeping your bones from breaking, there is no choice.”
Even at the hospital, Cresta has faced reluctance to administer opioids. “I could go to the ER, and the ER doctor that I had established a relationship with over time knew what they had to do,” she said. “They had to administer IV opioids quickly, one on top of the other, and they could break the spasm. It saved my life multiple times. But I don’t have that option anymore because nowadays ERs don’t treat pain and a lot of them do not want to give out opioids.”
Cresta said her prescriptions are routinely flagged by the PDMP system, which exists in some form in every state except Missouri. She has sometimes paid for her medication herself when her private insurance wouldn’t cover the cost.
Cresta became a pain advocate after posting a video to her YouTube channel, “outing” herself as someone living with chronic pain. “Everybody has an idea of a chronically ill patient as being disheveled and unstable and mean and they’re sitting in piles of dirty laundry, rocking back and forth, being hypochondriacs,” she said. “It’s very hard to sympathize with that image.”
She expected “people whose whole life is devoted to getting rid of opioids,” to respond to her video, but instead was flooded by messages from supporters who felt validated by her story, including some who were struggling with thoughts of suicide.
“Being chronically ill without the opioid issue is isolating,” said Cresta, who literally understood the pain of her viewers. “Then you add the opioid [fight] and it’s a really dark world for so many because we know that this the only way that we can survive.”
Cresta’s husband, Ryan, who is a veteran, had to stop working to take care of Cresta and their 5-year-old son after she began having trouble getting her prescriptions filled. They are being helped by their families. “I’ve been really fortunate,” said Cresta. “But family help runs out; it doesn’t last forever.”
Still, Cresta counts herself as lucky. “I am so grateful that I have a doctor that hasn’t abandoned me,” she said. “You don’t only have fear for yourself, you have fear for these physicians … and also for their families who they have to support. This mountain of fear that just never quite goes away.”
Whether it’s to put on makeup, record a video, or have a five-minute appointment turn into a four-hour ordeal, everyday Cresta makes a point of getting out of bed no matter how much pain she is in. “The first day I don’t get out of bed is the last day I’m going to be able to,” she said.
She continued: “A day in the life is pain. It’s fighting; it’s pushing. But the really important part is that I still have a day in the life because I have an opioid prescription. I wouldn’t otherwise.”

_____
Read more from Yahoo News:
Ann Coulter: ‘Lunatic’ Trump could be challenged in 2020 — from the right
As Trump administration negotiates with Taliban, some retired U.S. generals see defeat
Inside a key Hawaii intelligence outpost listening in on the Pacific
As 5G war with China heats up, could a Cold War-inspired plan be the solution?



