Illegal midwives and border babies: The determined fight for home birth in Alabama

Ashley Loper, 27, is in the throes of labor.
She’s on her hands and knees, naked, alternately quiet and screaming expletives, on a bed in a room in a rented house in southern Mississippi. Classical best-ofs — Pachelbel’s “Canon,” Debussy’s “Clair de Lune” — play softly from an iPhone. A forest of flickering white pillar candles stretches out on the headboard behind her, and the father-to-be, Joseph, a kind-faced 28-year-old commercial fisherman, stands anxiously alongside the bed, awaiting the arrival of what will be the couple’s third child. Loper flips onto her back, and her doula places a cool blue washcloth on her sweaty pink forehead.
“Goddammit! I can’t do it!” she yells, propping one foot on the shoulder of Colleen Tullis, her midwife, who is sitting near her on the bed, a calm and steadfast presence.
“You’re doing it,” Tullis tells her firmly.
This is a home birth — of sorts. It’s just not at the home of either Loper or Tullis, who each live about 40 miles away and over the state line, in Alabama, where this sort of activity could get Tullis arrested.

Home-birth midwives are banned from practicing there, so the birth is happening where most do in Tullis’s practice — in a white guesthouse, just over the border in Mississippi, where the owner allows women to have their babies.
“I work in Mississippi, and I live in Alabama, where I’m a criminal,” Tullis, 54, a certified professional midwife, tells Yahoo News. “It’s ridiculous. People driving four hours for prenatal care is ridiculous.” Many of her clients travel that far to see her for checkups and births of these so-called “border babies.” A handful of other midwives in the state cross borders in different directions, such as north into Tennessee, or east into Georgia, with their clients following them there. But Alabama is vast, says Tullis, who also makes it a point to train midwifery students, adding, “There needs to be more of us.”

It’s why an army of home-birth advocates has been pushing the state legislature to change the legal standing of midwives with legislation called the Childbirth Freedom Act (House Bill 284). But the work to pass it, led by the consumer-focused Alabama Birth Coalition and the professional Alabama Midwives Alliance, began a decade ago and has been stuck in the state House of Representatives’ Health Committee ever since.
A new crop of activists is confident that 2017 will be their year.
“We have a strong presence at the statehouse now,” Kaycee Cavender, president of the Alabama Birth Coalition, tells Yahoo News — the result of recent lobbying efforts, she says, to educate legislators on the millions of dollars that licensed midwives could save the state’s health care system. If the bill’s supporters can just get it out of committee — and there’s the rub — she believes they’ll have the votes. Her group is about to pre-file its latest version of the bill to both the House and Senate, which reconvene in February.

Such a change in the law would be welcome news to many women. Although not even 2 percent of U.S. births take place out of hospitals, the amount has been increasing: In 2012, births at home amounted to less than 1 percent of all American births, up from 0.79 percent in 2004, according to federal data — but that 2012 figure still totaled more than 35,000. The rise is largely the result of more women wanting to avoid medical interventions such as induced labor, epidurals, cesarean sections, episiotomies and the risk of “obstetric violence” — a growing, collective term that refers to when OBs bully or force laboring women into one or more of these interventions.

The trend of nonhospital births has drawn national attention to issues of midwife training and licensing, coordination between midwives and doctors, and arrangements for transferring women to hospitals should problems arise. And nowhere, perhaps, are the issues more clearly illustrated than in Alabama — a state that is consistently rated among the worst to give birth in the nation, according to the March of Dimes Premature Birth Report Card, which recently issued Alabama another “F” (a grade it has maintained for years).
It’s where access to quality maternal care is scarce because of a rash of hospital labor-and-delivery room closings over the years for economic reasons, leaving 38 of 67 counties with no hospital delivery units. It’s also where mother-of-four Caroline Malatesta recently won her high-profile, $16 million obstetric violence case against a Birmingham hospital that had sold her on the chance at having a personalized, natural birth — but instead had her restrained by nurses during labor to the point of suffering intense physical and emotional injuries. The case highlighted just the type of traumatic birth that so many women seek to avoid.
Add into that messy mix the state’s outlawing of certified professional midwives (CPMs), and you’ve got a real watershed moment for women in Alabama.

“We have a maternity crisis in this state, and it’s getting bigger and bigger and bigger,” Jennifer Crook, a CPM in Birmingham, tells Yahoo News. “And we’re not talking about one little niche population that’s just gung-ho about midwifery care. We’re talking about a group of women who want access to quality, evidence-based care, and can’t find it. So not only do we have women driving hours over the state border to access legally recognized midwives, we have women who want hospital births and are having to drive hours to access the less than a handful of obstetricians in the state.” Crook, who stopped practicing in recent years to devote full-time efforts to lobbying on behalf of the Childbirth Freedom Act, addresses the topic with a mix of exasperation and hard-to-temper passion.
CPMs become accredited either through an apprenticeship or educational program, or a combination of the two. They differ from certified nurse midwives (CNMs), whose professional path includes graduating from a CNM education program, maintaining an active registered nursing license, and having a bachelor’s degree. In Alabama, CNMs cannot attend home births but can legally practice in hospitals; still, they rarely do because of highly restrictive physician-supervision rules. There are currently only about 25 CNMs in the entire state (Colorado and South Carolina have similar populations and, for comparison, have 372 and 123, respectively).
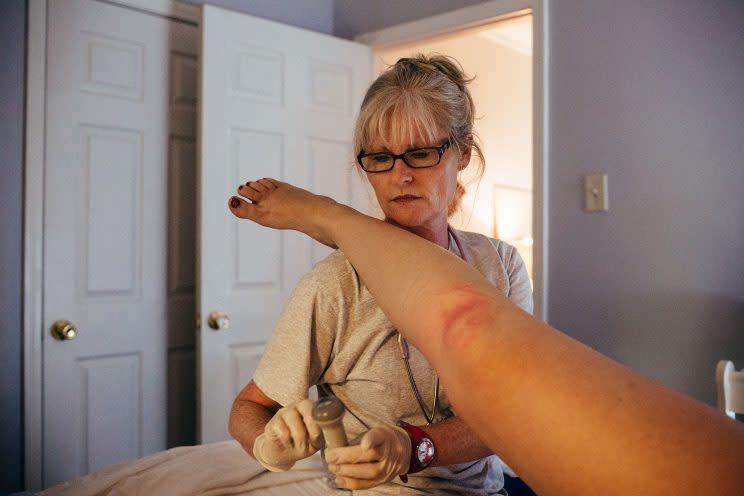
CPMs, meanwhile, are banned — not explicitly, but by legal precedence, and by the state’s having dissolved any path to licensure back in 1976. While 20 other states also ban or restrict CPMs to some degree, Alabama has shown it’s one of a handful (including California, Connecticut and Illinois) that will actually arrest midwives caught assisting a birth — as it did in the early 1990s, and again in 2002.

But the ban, rather than snuff out the practice of midwifery in Alabama, has effectively made home-birth midwives and the women who desire to work with them even more determined, as they’ve gone underground and across state lines.
As bluntly stated by Simone Jones, a woman who defiantly gave birth to her baby at home in Birmingham in 2011 with a midwife who risked prosecution by operating in the state (a handful still do): “It’s a bunch of bulls***. Why is it so important to control women’s bodies? Why is it so important to have the state involved when it isn’t necessary? The truth is we do what we want to do, clearly. There’s always a way around it.”
* * *
Loper is one of many women who have found their way around the law with the aid of Tullis in this cozy Mississippi birthing house. After unhappy hospital experiences and what she believes were unnecessary C-sections with her first two babies, including one given because the doctor said her baby (8 pounds, 7 ounces) was “too big” to be born vaginally, she yearned this time around to have a VBAC — vaginal birth after C-section — a practice that’s banned or heavily regulated by every hospital policy in the state. (“The doctors say it’s a risk of rupture, but that risk is still less than all of the risks that come with a C-section,” Tullis tells me.)
Here, Loper is allowed to give birth in any position she desires, and is supported by her husband, her midwife, and a team of skilled and soothing women composed of a doula, two midwifery students and Tullis’ assistant. They all seem to know just when to close in on her with focused, supportive energy, when to hand Tullis her small pink flashlight or fetal Doppler, and when to fan out through the house, fetching ice cubes or ice water or a rice sock heated in the microwave, or grabbing sustenance for themselves — a steaming bowl of noodles, a Bolton’s berry smoothie, carrot juice in a jelly jar.
Still, Loper’s labor has been going on since early morning, and now, in the late afternoon, she’s begun to lose strength, both physically and mentally.
“VBACs are just a different breed,” Tullis explains while taking a break from Loper’s side. “They’re more scared. She’s going to be filled with a lot of doubt and extra anxiety.”

Soon Loper, red-faced, sweaty and angry, stalks out of the bedroom and announces, “I can’t do this anymore.” She gives it one more shot, squatting as she hangs onto Joseph’s middle, as if he were a tree. The coy angel tattoo on her lower back glistens with sweat as Tullis feels inside for the baby, telling her, “Push! He’s right there!”
But she’s too exhausted to continue.
Tullis sits alone on a stool for several moments, looking back over the day’s meticulously kept labor notes and thinking intently about their options. She could take Loper to the hospital for some fluids and possibly drugs, though she knows it would most likely mean a C-section. (An average of 6 percent of Tullis’ birthing moms will wind up requiring midlabor transport to the hospital, for reasons ranging from placental bleeding to fevers to sheer exhaustion.) She’s wearing her company T-shirt, which says, “Mothers Comfort Birthing Services: Create Your Own Birth Story. Birth Is As Safe As Life Gets,” and rubbing her temples.
“Nothing is wrong,” she says softly in her gentle Southern twang. “She’s just exhausted.”
* * *
Safe, healthy, empowering birth experiences are what any midwife really wants. They just come from a place that’s different from a physician’s, who sometimes look at birth as something inherently dangerous, and are instead guided by the woman-centered Midwifery Model of Care. The approach looks at birth as a normal physiological event, stressing individual education and counseling, minimal technological interventions, monitoring of the mother’s physical and psychological well-being, and the referral of high-risk pregnancies to obstetricians.
That latter goal is particularly tricky in states like Alabama, where few doctors will collaborate with CPMs because of their legal status, creating fear and friction where there needs to be openness and support, particularly if it becomes necessary to transfer a patient to the hospital in the midst of labor.

“The best situations are where the midwives may work with a range of providers — the receiving physicians know the midwife, and is confident, and they’re a team and nobody’s afraid of the other,” Arkansas-based CPM Ida Darraugh tells Yahoo News. Darraugh serves as a board member on the North American Registry of Midwives and is part of an effort to create federal recognition of the CPM credential. “That’s the ideal situation.”
It’s a big part of what women like the Alabama Birth Coalition’s Kaycee Cavender are fighting for — and what they ideally want as patients. Cavender, a part-time paralegal who had her second child with Tullis in Mississippi in November, drove there frequently for her prenatal checkups — which required a nearly two-hour trip each way from her home in southwest Alabama.
I made the trip with her one morning, along with her supportive husband, Robert, and then-14-month-old, Doriella, and after procuring some warm biscuits at a Hardee’s drive-thru, she tells me that she found her way to home birth as a result of miscarriage, and how dismissed she felt by her medical provider.
“There was no sympathy, no empathy, no nothing — just, ‘You need to go home and bleed it out.’ And I just had this feeling of, I’m already overwhelmed with emotion and this is not the kind of care I want if I become pregnant again. I don’t want to ever be treated like this again,” she says, raw emotion creeping into her voice. “So I started researching other options, and that’s when I came across midwives, and started reading about midwives and watching documentaries, and found [pioneering midwife and author] Ina May Gaskin and read her books. From there I was, like, well, I wonder if I can find a midwife in Alabama? And I couldn’t.”
As Cavender speaks of her own journey, and how she eventually found the Alabama Birth Coalition (ABC) and began her life as an advocate, we fly along Interstate 10 with a sweeping Southern backdrop: cornfields, a Waffle House, fireworks shops, lush trees dripping with Spanish moss, Mobile’s skyline, the Escatawpa River, a billboard for a Roots & Boots country music tour, 14 churches. She shares statistic after statistic with a disarming confidence and ease, such as, “There are only 474 ob-gyns in the state serving over 2 million women of childbearing age,” and “10 to 12 percent of Alabama families don’t even own a single vehicle — so with half of the state not even having a hospital with obstetrical care available, you’ve got families with no options but to be at home.”
She notes how deeply underground midwives practicing in Alabama have gone. “It’s so tight-lipped that unless you know a mother who delivered with one, you’ll never find one,” she explains. “The thing about these midwives is they do it for the mothers: You have mothers who are giving birth unassisted in Alabama because they have no other option. And that’s why ABC is working so hard to give them that option, so midwives can openly practice and collaborate with physicians.”
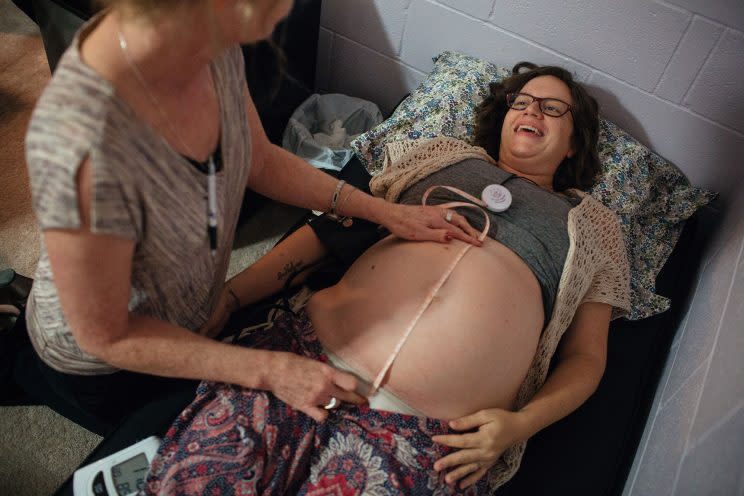
At Tullis’ office, Cavender has a relaxed checkup while her husband and bouncy, curly-haired infant hang out in the living-room-like waiting area in a house next door to the birthing house. Her exam room feels like a warm office, with a dark wood desk and a low exam table that Tullis kneels alongside on a plush gray carpet, to prod pregnant bellies and check their size with a measuring tape and listen to fetal heartbeats with her Doppler. A bookcase holds titles like Heart & Hands: A Midwife’s Guide to Pregnancy and Birth, A Child Is Born, and Color Atlas of Life Before Birth, as well as a model of a birth canal that holds a blank-faced baby doll, and pamphlets about the Bradley Method of birth. A framed sign on the wall reads, “She believed she could do it so she did.”
Tullis’ first over-the-border rental property, she recalls, “was a little yellow house, a guesthouse on a German lady’s property. She let people come and have babies. Then I was temporarily in a 750-square-foot cottage on a lake.” The current spot, though — on a half-acre of property with graceful, shady trees, and additional structures that provide room to grow — has been ideal. “I want to be able to have a classroom,” she says. “I can put a playground out there, I have parking, and I’m nine-and-a-half miles from a hospital.”

I sit with Tullis and her clients through two days of prenatal appointments, with patients explaining they’ve come mainly because previous hospital births were “highly medicalized.” One recalled feeling “so defeated the whole time,” and others described “terrible” inductions. These checkups feel like mellow, one-sided social visits, with women answering questions about eating and sleeping habits in between measures of blood pressure and weight. They sometimes stay for up to an hour.
“Don’t forget to bring a one-gallon-size bag for your placenta,” Tullis says. “Have you been taking your alfalfa?”
One expectant mom, Heather McClain, has driven two hours from Florida. She has three kids — ages 2, 6 and 8 — and is due in a week. She has been having persistent contractions, and reports that she’s been seeing a chiropractor to alleviate sacral pain.
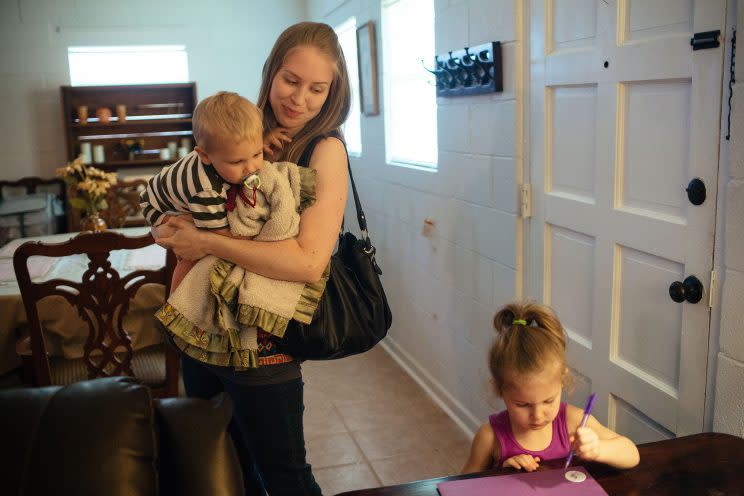
“Don’t stop if you’ve found something that works,” Tullis tells her. Then she goes over a checklist for the day of the birth. “Supplies are gathered?” she asks. “Do not come without food. If labor’s long, we have to have food.” (McClain’s baby, a rare footling breech, arrived safely in Tullis’ hands.)
Some express resentment for having to drive here rather than give birth at home. “It sucks,” says Dana Warner, 33, a stay-at-home mom of three married to a Navy shipbuilder. “I was born and raised in Alabama; my kids’ birth certificates are all Mississippi. … Colleen makes it as homey as possible, it’s comfortable and everything, but it’s not your home. I wish I could just go squat in my bathroom, push the baby out and get in my bed, and be done with it.”
Tullis, with her strawberry blond hair and porcelain skin, is like a shaft of light — both ethereal and reassuringly powerful, in charge at all stages of a birth but humble enough to take a back seat at any mom’s request. (A recent such incident, she explains, concerned a third-time mom determined to labor unassisted and catch her own baby; Tullis dutifully waited in the next room, rushing in to assist only at the end, when the infant’s head was out and its shoulders wouldn’t budge.)
A former schoolteacher and a mother of seven — including six daughters, one of whom has become a birth educator and doula — Tullis learned about the world of home birth more than 20 years ago, when she volunteered at a crisis clinic for girls and wound up teaching childbirth classes there. She first became a doula, then a certified professional midwife.
When she spoke before the Health Committee about H.B. 284 last spring, she was serene but unwaveringly knowledgeable and professional, prompting some legislators to exclaim behind the scenes that Tullis was “not what we’d expected.” (“Not a Birkenstock-wearing hippie with hair down my back, I guess,” the bemused midwife surmised upon hearing this.) She calmly answered questions from legislators about how many births she had attended so far (525) and the farthest she had traveled to serve women in need of maternal care (four hours).

The reworked and refined legislation has been modeled on successful laws in other states, including Indiana, Rhode Island and Maryland, which have approved midwifery licensing in recent years. But efforts here and elsewhere have lagged because of strong opposition from medical groups, including the Medical Association of the State of Alabama (MASA) and the Alabama Department of Public Health — which are practically one and the same, say critics. The nonprofit MASA controls 12 of the 16 seats on the Department of Public Health’s governing committee, as well as all 16 seats on the Alabama Board of Medical Examiners and Medical Licensure Commission.
“Essentially, what we have here is a private, nonprofit organization whose mission it is to protect the bottom line of its 7,000 physician members overseeing the operation of a state governmental agency,” Crook told Weld for Birmingham recently.
Yahoo News made repeated requests to MASA for comment for this story, although none were returned. The Alabama Department of Public Health also did not respond to requests for comment.

But MASA president Mark Jackson testified in opposition to the bill at the hearing in April, saying, “If this were to pass and just one child were to suffer, just one child were to have irreversible brain damage or die, it would not be worth it.” Still, Cavender says, they’ve had productive meetings since then.
Also speaking against the bill, on behalf of the Alabama Department of Public Health, was Dr. Grace Thomas, using statistics from a recent New England Journal of Medicine study on planned home-birth outcomes.

The study, which has been praised by both doctors and midwives for its approach and tone, looked at nearly 80,000 births in Oregon. It found that although severe complications were rare in all locations, in planned out-of-hospital births 3.9 out of 1,000 cases resulted in a baby’s death during the birth process or within four weeks afterward, compared with 1.8 deaths out of 1,000 in planned hospital births. On the other hand, out-of-hospital births were far less likely to involve cesarean sections — 5.3 percent compared with 24.7 percent in a hospital — which are high-risk surgeries.
It’s just one of many studies in circulation about in- vs. out-of-hospital births — including a landmark 2014 study of 17,000 home births, the largest-ever such analysis. It showed that among low-risk women, planned home births resulted in low rates of interventions and extremely healthy outcomes, including excellent birth weights, a low 5.2 percent C-section rate, high rates of breastfeeding and a 10.9 percent rate of hospital transfer for babies, for the majority non-emergency reasons.
In any event, what it often comes down to for proponents of legalizing certified professional midwives is accessibility and choice.
“It’s a freedom issue,” says Cavender. “What other medical decision doesn’t let you have a choice? Oh, right — anything involving a uterus,” she adds. “And that makes me angry.”
* * *
The practice of midwifery in Alabama is far from new. In fact, it has a very long and complex history studded with themes of racism, classism and sexism. And it’s the medical establishment’s “orchestrated effort to paint midwives as dirty, uneducated and backwards” that’s unfortunately had the most lasting effect, according Steff Hedenkamp, spokeswoman for the Big Push for Midwives, an organization that supports efforts across the country to legalize CPMs.
Historically, “lay” or “granny” midwives in Alabama were predominantly African-American women who served poor populations — those kept out of hospitals because of segregation and economics. In 1921, the federal Sheppard-Towner Maternity and Infancy Act became law. And while its suffragist-supported aim to lower mortality rates of mothers and newborns had good intent, it helped support the idea of midwifery as a “negative, horrible thing,” according to Shafia Monroe, founder of the International Center for Traditional Childbearing, which aims to expand the number of black doulas and midwives.
“White America stopped having their babies at home long before black women,” Monroe, who is based in Oregon but has roots in Alabama, tells Yahoo News. In the past, authorities shamed black women for choosing midwifery care, she explains, so some have been slower to reembrace it. “For a lot of African-American women,” she says, “having a baby at home means you’re not progressive.”
Still, Monroe reports, she’s seen a rise in the number of black women who are studying midwifery, as well as those who are seeking out and advocating for home births, including in Alabama. That includes Jones — the woman who had given birth at home in Birmingham in 2011, who says her mom’s attitude “was all about, ‘you go to the hospital.'” But after negative hospital experiences with her first two births as well as with a miscarriage, Jones was determined not to return — and was pleasantly surprised to learn along the way that her great-great grandmother had actually been a lay midwife.

In 1931, Alabama’s lay midwives became strictly regulated, with a rigorous screening program reducing the number by half. Those who remained were required to attend a long training course, pass a written exam, wear white uniforms and submit to monthly inspections of their equipment bags and homes, according to a history summed up by the Alabama Midwives Alliance (AMA).
Then, in 1976, the state legislature passed a line-in-the-sand law. “The purpose of this act was to legislatively redefine midwifery to include only the practice of nurse-midwives. Simultaneously, it placed stringent regulations on the practice of nurse-midwifery, preventing autonomous practice,” the AMA history explains. But enforcement, placed in the hands of county health departments, was inconsistent: Some counties actively revoked permits, some grandfathered in those that already existed, and still others continued to refer pregnant women to such midwives, sending mixed messages across the state.

By the 1990s, Alabama, like the rest of the country, was seeing a rising interest in out-of-hospital birth, with mainly Caucasian, middle-class women seeking alternatives, according to AMA. Toni Kimpel, a woman who gave birth with a permitted “granny” midwife, became a midwife herself — but was soon charged, twice, with practicing nurse-midwifery without a license, both times after transferring women to the hospital; in one instance the baby was delivered at the hospital, stillborn, and in another the infant was born at home but died at the hospital. Although a judge threw out charges based on the law against lay midwives being unconstitutionally vague, the state appealed one of the cases and won.
“The bottom line with midwifery is political,” Kimpel, who received probation and now lives and practices in Texas, tells Yahoo News. Midwife Karen Brock was arrested on the same charges, of practicing without a license, in 2002.
But none of this means that midwives don’t want regulation. “I think it’s important to have standards,” Crook says. “I think it’s important for parents to make an informed decision and to know that when they’re choosing a midwife to attend them that that midwife has met a certain educational level. And the way it is now, anyone can call themselves a midwife in Alabama.”
Yet another layer of the licensing conflict is financial, as it hampers reimbursement for midwifery. Medicaid agencies in only a dozen states authorize payment for certified professional midwives, the National Association of Certified Professional Midwives told the Washington Post recently. And seizing on this angle could get midwifery proponents the most leverage, suggests the International Center for Traditional Childbearing’s Monroe.
“I think it’s economic in the Old South — it’s a patriarchal system, and they need education,” she says about Alabama’s fight. “So it’s about coming to them in a way that talks about economics, people with abject poverty, and not so much as ‘we have our right to have a baby at home.’”
Alas, tensions between midwifery and obstetrics remain. Big Push for Midwives’ Hedenkamp says, “It’s about power, influence, money — about Big Medicine not wanting any kind of competition for maternity care.” She notes, “Hospitals get over 30 percent of revenue from maternity wards, so it’s very important to continue the non-evidence-based approach, keep the moms coming, and make them feel like it’s a train wreck waiting to happen.”
* * *
That’s thankfully not what happens during Loper’s increasingly difficult labor, when everything shifts and a decision is made that she will be transported to the hospital — back over the state line into Alabama, where Tullis’ backup doctor (whose name she won’t disclose, owing to the delicate balance he faces in such an illegal environment) is fortunately on call.
“Everyone else hates us,” she says, referring to ob-gyns who seem more intent on punishing home birthers who show up at hospitals needing help than on providing supportive care.
And so, with Loper at her wits’ end and Tullis still calm but sharply focused, they trade the cool dark cocoon of the birthing house for the blinding 90-degree heat of the afternoon and then pile into Loper’s van, with Joseph at the wheel. Then it’s a mad dash for an ER in Mobile — where Loper rallies and pushes for just 45 minutes, quickly achieving the vaginal birth she’d wanted so badly. It wound up being the most ideal type of midwife-doctor collaboration, and illustrates why Darragh and most others in this movement are so intent on getting physicians onboard as allies.
“I would have regretted transferring if I had wound up with another C-section,” a blissful Loper discloses to me the next day from her hospital bed, with sleepy Gavin at her breast and tots Maya, 2, and Ethan, 3, doing their best to hijack mom’s attention. “But because it worked out this way, it doesn’t bother me. It’s still a great birth story.”



