A new vaccination approach: Reaching those who weren't planning to get the shot
On the second Saturday in April, Dr. Karen Smith was able to easily find a parking space at the Freedom Chapel AME Zion Church — the first sign that something was off.
Smith, who has a family medicine practice in the rural North Carolina town of Raeford, had come to the church with enough doses to vaccinate 1,000 people.
The last time she’d held a vaccination event at Freedom Chapel, two weeks earlier, she said cars were parked “three-deep” on the grass and spilled onto the sides of the highway. In two hours, her team had vaccinated more than 240 people.
But on the morning of April 10, there were only a few takers in a community where plenty of local residents remained eligible for a shot. Only 14 percent of residents in Hoke County have been fully vaccinated. The rate is the second lowest in the state and trails well behind the nation’s average of nearly 31 percent.

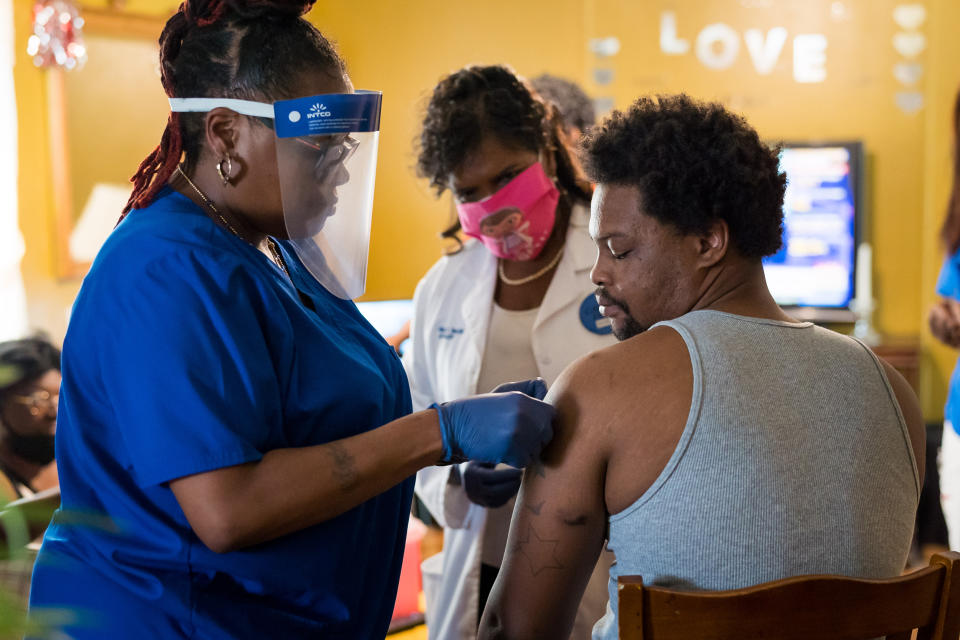
The gap is worrisome in the racially diverse county — 49 percent white, 36 percent Black, 14 percent Latino and 9 percent Native American — where many already suffer from poor health and work in industries like the service sector and agriculture that provide little room for social distancing. Smith routinely treats new Covid-19 cases, and Hoke County is one of several in North Carolina in the orange zone for new cases, one rung below the state’s worst category.
After vaccinating about 50 people at the church that day, Smith turned to making sure the rest of the 100 doses she’d thawed weren’t wasted.
Full coverage of the coronavirus outbreak
She called the county’s sheriff and asked if deputies and incarcerated people had been vaccinated. He told her yes. Then her husband drove her to the town’s poultry plant, where she asked for permission to vaccinate workers. She received the go-ahead, but once again, she walked away with a surplus. A few workers stopped her team in the parking lot and rolled up their sleeves there.
Now, 29 doses were left.
One of her staff members joked they should go to a convenience store. A short drive later, she walked into a gas station and asked the manager and employees if they were interested in getting the shots.

For many communities, the next leg of the country’s vaccination push could look increasingly like this, as providers shift their focus from mass vaccination sites to “microtargeting,” said Hemi Tewarson, a visiting senior policy fellow with the Duke-Margolis Center for Health Policy, who has closely tracked equity efforts with the nation’s vaccination rollout.
“You have to think: Let’s look geographically — where do we have low vaccination rates?” she said. “And then drill down within that: Who are the people and what’s going to resonate with them?”
That might range from a smaller site near a community hub where people can easily walk up to receive a shot, or a van bringing vaccinations to an apartment complex. Such approaches are already being deployed in cities like Baltimore, which recently launched a pop-up clinic at a community college. The idea is to use door-knocking campaigns and social media advertisements to spread the word in nearby neighborhoods before each clinic.
In Baton Rouge, Louisiana, officials are planning an outreach event outside a popular nightclub. In Chicago, youth ambassadors with Increase the Peace, an anti-violence initiative, have also started sharing information about the shots.
For more of NBC News' in-depth reporting, download the NBC News app
The shift could be critical as more states and local health officials confront thinning demand for the vaccinations. Dozens of counties where vaccination rates sit in the low double digits, like Hoke, also have a high social vulnerability index from the U.S. Centers for Disease Control and Prevention. That’s an indicator that some of the communities facing a greater risk of being devastated by the pandemic have the scarcest defense.
Even with the pandemic’s disproportionate impact on communities of color, Black people and Hispanic people are underrepresented in most states’ vaccination totals, according to an analysis from the Kaiser Family Foundation. Lack of access to transportation or to the internet can make it impracticable to obtain a shot. And while surveys from the foundation show a decline in vaccine hesitancy among both groups, distrust fueled by past and current mistreatment in health care can remain a deterrent.
For communities with a history of mistrusting medical establishments, partnerships between vaccine providers and grassroots groups that have earned trust is critical, said Dr. Helene Gayle, who co-chaired a committee for the National Academies of Sciences, Engineering, and Medicine dedicated to advising officials on how to equitably distribute doses.
“It’s very important that health care providers think about how they can team up with organizations that really understand communities and community needs,” she said.
In Washington, D.C., several health care providers worked together to bring doses to the Southeast Tennis and Learning Center located in Ward 8, which has been hit hard by the pandemic. Only 12 percent of residents in the ward have been fully vaccinated, the lowest percentage in the city.
The effort was launched after the city’s former first lady, Cora Masters Barry, expressed concerns about disparities in vaccination rates. Ward 8 has the second highest concentration of Black residents in the city. Poor health outcomes are endemic.

Dr. Jehan El-Bayoumi, the founding director of the Rodham Institute at the George Washington University School of Medicine and Health Sciences, said some patients have to take three buses to travel to appointments. It’s just one illustration of how underserved the community is.
“I can walk to the pharmacy and trip over the Safeway and Trader Joe’s,” Bayoumi, who also serves on the steering committee for the Black Coalition Against Covid, said of her neighborhood in Ward 3, which is in a different and more well-resourced part of Washington. “There’s only one full-service grocery store in Ward 8.”
On April 3, a vaccination event at the recreation center was made exclusive to residents of Ward 8. Free Uber rides were provided for those who needed transportation.
Almost 900 people were vaccinated, and nearly 200 of them were walk-ins who hadn’t registered. Organizers also offered food boxes and referrals to aid organizations and information about affordable preventive health care. A DJ specializing in Go-Go, a funk genre that originated in the city, blared tracks to make the affair upbeat.
One woman told El-Bayoumi she was enjoying herself so much that she didn’t want to leave.

While such events may not bring in large numbers as quickly as mass drive-thrus, they can be an effective tool in reaching those who otherwise might go unprotected.
Smith, in North Carolina, said that as she sat at a table in the convenience store a couple weeks ago, it was evident that plenty of people she vaccinated there wouldn’t have made their way to Freedom Chapel. Some didn’t visit doctors regularly; others cited religious objections, or told her they worried the vaccine would affect their ability to have children — a false claim that continues to proliferate on social media.
That day, Smith said, made it clear that the “typical” approach did not work.
Of the 29 doses her team used at the gas station, 25 went to men who identified as Black or Latino. For Smith, it was an indicator of who’s been left behind.

“We missed them,” she said. “For us to get 25, we’re not doing it right.”
One person told her he didn’t have a primary care provider. She gave him a card and started thinking about the next time she could return. A mobile home park sits behind the convenience store, and it would be easy for residents to walk up and get vaccinated. Easier still would be bringing the doses there, if management allows it. Her team is working to see if that would be possible.
“Now’s the time to come out of the typical sterile health care way of thinking,” she said.

