Inside the National Quarantine Center, There Is No Fear. There Is Only Urgency.
The National Quarantine Center, this nation’s only federal quarantine facility, sits on a single floor of a new building on the campus of the University of Nebraska Medical Center west of downtown Omaha. It holds 20 beds, 15 of which are occupied by patients exposed to the novel coronavirus, or SARS-CoV2, including several passengers from cruise ship Diamond Princess.
A couple of blocks away sits the UNMC biocontainment unit, the largest of its kind in this country, which takes up part of an upper floor in a large inpatient-care facility. Ten beds, with a 35-bed surge capacity. Two pressurized entrances providing constant negative air pressure via a HEPA airflow system, and decontamination autoclaves for waste disposal. Currently four of the beds are occupied by contagious COVID-19 patients. (“COVID” means coronavirus disease.)
From the hallway outside, the staff entrance is just a plain wooden door, with a coded keypad on the wall. There’s a plaque at the other end but not much else to signify the location as particularly important. This is a health-care facility, peopled by a calm—and, yes, exhausted—staff, otherwise busy with the industry of care.
And as the new coronavirus continued its attack on the globe, the sole diversion from normalcy in the area is the presence of two federal marshals sitting in at a folding table. On the day I visited, one of the marshals was eating a graham cracker. On the table: Aquafina water bottles, two government-issue laptops, Clorox disinfectant spray, and hospital-grade sanitizing wipes. The marshals wore short-sleeved button-down shirts, khakis—they could’ve been on their way to hit some balls at the driving range. On the wall behind them, next to an alcove, a sign said “Soda Machine.”
This is normalcy. And this is the new code red.

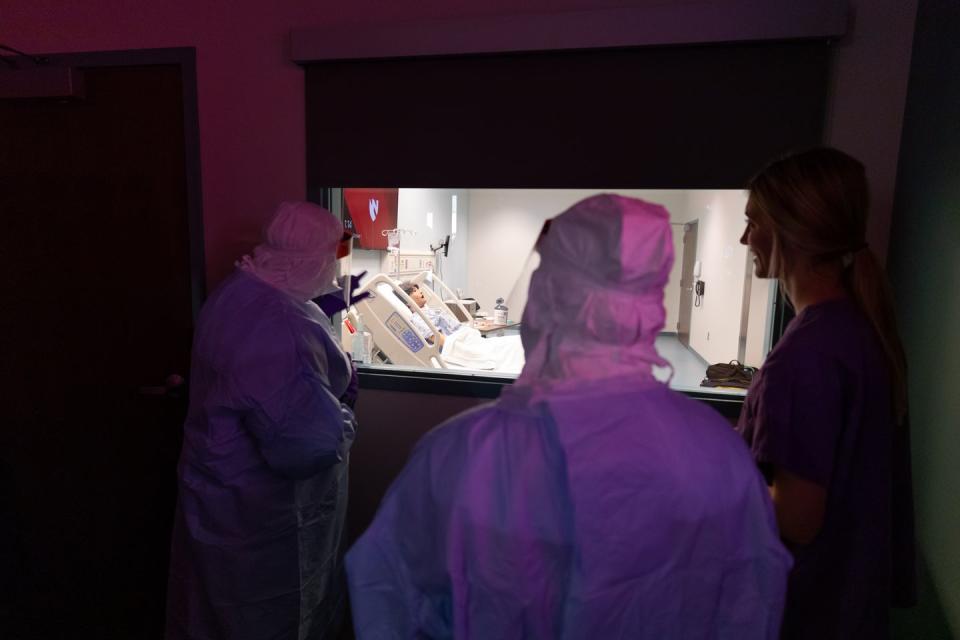
Beyond that, behind the unmarked door, in the patient isolation rooms, the air is completely turned over—old air sucked out, new air piped in—at least 15 times per hour. There is a handwashing station, of course. Before entering the unit, every staff member must don a full PPE suit (personal protection equipment)—gowns, masks, safety glasses, hood, apron, respirators, redundant eye protection, redundant gloves. They dress for entry in pairs, working with a donning partner, who checks the donning process in a prescribed step-by step manner.
Upon leaving the unit, the doffing process, in which the armor of the PPE is stripped away, is even more complicated and time-consuming, because all contact with exposed surfaces must be avoided. This too is done with a partner.
I was granted access to see them at work at the height (so far) of the pandemic and I interviewed several staff members who make the place work, putting their lives at risk every day.
For one of them at least, the days do not end.
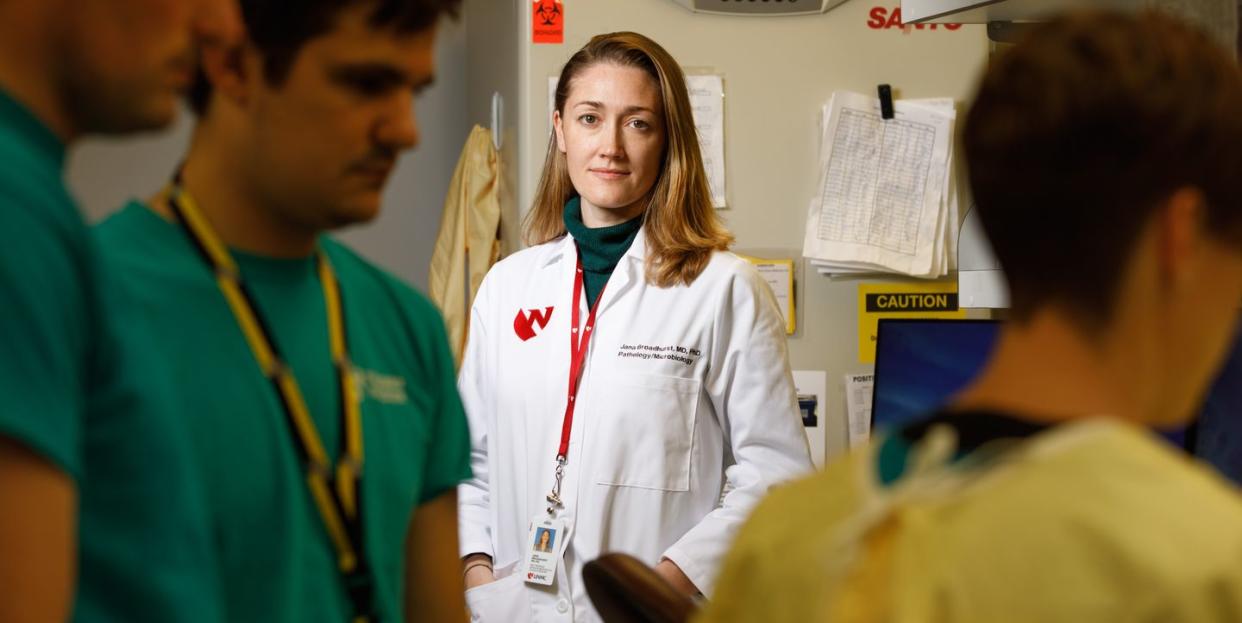
Jana Broadhurst, Ph.D. and M.D.
Director, Nebraska Biocontainment Unit Clinical Laboratory

At some point maybe six weeks ago, she can’t be sure, Jana Broadhurst had a cot brought into her office. She began sleeping on-site so as not to lose time in the race to develop a reliable diagnostic test for the novel coronavirus. Sleep came catch-as-catch-can at first, two hours at a time, then two hours a night, then not at all. She brought in an acoustic guitar and tried playing herself to sleep. She favored Gillian Welch, with a little Grateful Dead mixed in. Middle of the night, sometimes.
Even then, she slept fitfully, and once again not at all.
The energy of the lab—with the arrival of test results and data sets at ungodly hours, online consultations with colleagues doing lab work in other countries—proved entirely too relentless.

Broadhurst, 37, joined the lab in mid-fall of last year, and within three months the novel coronavirus split the world open. And while her work keeps her from sleep, she is passionate about where she finds herself every day. “This place is the beating heart of a novel infectious disease response. It’s what I always wanted a piece of as a scientist,” she says.
A lab supervisor charged with developing a diagnostic test better, faster, stronger than what the CDC has provided for healthcare providers thus far, Broadhurst says, “The challenge is that every day we run into protocols and procedures that demand solutions we can’t look up in a manual or textbook. This work is all about big decisions in real time.” This is where it’s happening.
These days, she’s rarely in that office, which sits hunkered in a tricky little piece of academic architecture at a relative distance across the chaotic campus geography from the lab. When she meets a supervisor for an update, or an outsider for a quick layman’s lesson in the broad brushstrokes of work with the RNA of the virus or clarification on the importance of accurate diagnostic technique in understanding the spread of a virus across the planet, she’ll use the office.

In there, it’s as if she doesn’t see the cot or the guitar. The lab—that’s where the action is. Peopled by lab assistants, with sequencers and autoclaves humming their mechanical soundtrack in the background, the working lab feels like a loft for working artists. Energy permeates every action. Whereas the scene in her office looks like a set in a Neil Simon play that never got written.
She looks exhausted in every contour of her face. She’s caught in the sheer grind of the race to deliver to the world a clinical testing device to replace the slow, clumsy procedure devised months ago by the CDC. The prospect of this discovery thrills her instinct for usefulness, invention, economy.
Some people—the president, for example—have wondered aloud whether diagnosis might cease to be a relevant function of ending a full-blown pandemic. Isn’t the virus here to stay, whether we can diagnose it or not?
Broadhurst asserts the med-school paradigm that outlines three stages of responding to an outbreak: the diagnostic stage, in which carriers are identified and studied; the therapeutic stage, in which the appropriate care is provided; and the vaccine stage, when future outbreaks are prevented.
“In conceptualizing the diagnostic response, we consider the individual first—the individual patient, who gains the advantage of an informed response, and the individual doctor, who is freed to offer care shaped to the needs of a patient who understands the limits of his condition,” she says, leaning in. “Diagnosis liberates them.”
The current test, in which a blood draw must be mailed to the CDC lab, and which takes days for the results to come in, and be mailed back, is the same test the president declared “perfect” when he visited the CDC in February. No one at UNMC wants to take on the president or assess the operations of the CDC. They want to create a path forward in treatment of the disease.
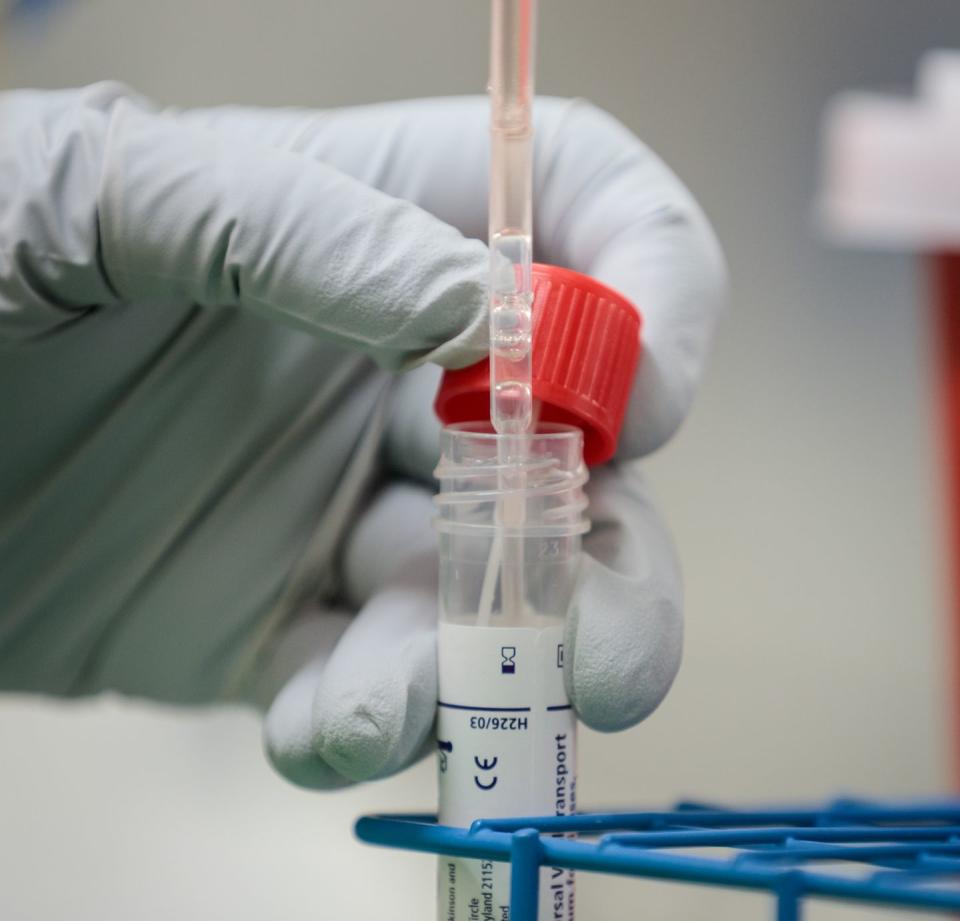
The doctor looks pained by the thought of Trump’s comment. “Not perfect,” she declares just as clearly as Trump had trilled the opposite assessment. “Not even close to perfect.”
Hence the race to replace it. That’s the why of her sleeplessness, and conversely her bottomless energy for a task. The relentless pursuit of a new test, one that produces results in four hours instead of four days, one that might ultimately be made into a kit.
“Race is a perfect word,” she tells you. “It is a race. A race against an increasing demand. A race to create a new diagnostic tool, for use against a previously unknown viral force. It’s less about being first and more about getting it done.”

And recently they nailed it. The test worked for incoming patients. The results were duplicated. Soon after, UNMC received permission to use the test in their own work with COVID-19 patients.
The race must have seemed won by Dr. Broadhurst and her team.
Wasn’t it?
“Have you ever been hiking in the mountains?” she asks. “Are you familiar with a false summit?” I can figure it. “You look up as a climber and think you see the end of your climb, only to discover the true peak has been obscured by your perspective.”
So begins, for Broadhurst and her team, the race for accelerated approval of the UNMC clinical lab test procedure by the FDA. Normally this would be a matter of years. A distant summit. This time it has to be a matter weeks before they see the top of their climb.
I ask her what courage means, and how it applies to her and her team.
“I don’t think anybody would use the word courage, but it takes courage to come to work here. But you trust your team and the people you work with, and you move forward,” she says. “Everybody puts the mission first.”
LuAnn Larson
Director of Clinical Research Operations, UNMC

LuAnn Larson, born in Norfolk, Nebraska, now 30 years in the business of clinical research on infectious disease at Nebraska Medicine, meets me in a waiting room at the end of the hall outside the biocontainment unit. She’s carrying two three-ring binders on her arm and a bag of an investigational antiviral medicine called remdesivir, newly rushed into clinical trials at UNMC, bound for an IV in the biocontainment unit.
She’s overseeing an NIH-approved study of a therapeutic medicine for the treatment of novel infectious diseases like COVID-19. Make no mistake, the dawning of the COVID-19 era is a dire moment in the world of infectious-disease treatment. But it is a singular one too. Infected patients willing and able to participate in research efforts are a unique opportunity in clinical research on infectious disease.

Six months ago, there weren’t any COVID-19 patients. Anywhere. In a month, there will be a world of patients who may need the very medicine in this bag, due to the unclamped spread of the virus people are concurrently developing a diagnosis, treatment and containment for. Urgency hereabouts.
But not fear.
“When we dealt with Ebola in 2014, there may have been a thread of fear,” Larson says. “But we learned how to deal with the demands. The team that runs the biocontainment unit dealt with things so thoroughly in how they vetted things in the aftermath. They thought through the what-ifs. And we practiced all the time. We went through the donning and doffing so many times. And we learned.”
It’s not like there is no room for fear in her, as if she somehow crammed fear out of her world-view. It’s that Ebola—the process they learned during Ebola—prepared them for this. “This is the place where we do this,” she says. “We get better. There isn’t a choice.”
She pauses for a moment.
“I don’t have fear,” she says. “That was your question.”

The process to me, a normal human, seems overwhelming—the donning, the doffing, the care that must be taken with every step. Just delivering this bag of meds…my God, could I do that?
I ask her: Aren’t you afraid of slipping up?
This irks her, I can tell—my certainty that everybody screws up from time to time, forgetting a step, or leaving behind some Personal Protection device, simply forgetting. I forget things all the time, I tell her. I offer an example. “I’m supposed to get receipts for my meals,” I tell her. “I understand the process, but I’ve been forgetting them for years.” That inglorious comparison irks her even more. She actually scoffs, and until that moment, I had never realized that a scoff is a bona fide onomatopoetic sound utterance.
“There’s a difference between forgetting a receipt for an expense report and breaking your PPE in a contagious environment,” she says. Consequence means something. Second chances aren’t there. “Those are just very different levels of needing to be thoughtful.”
Nebraska Medicine CEO and renowned pathologist James Linder told me before I met a soul at UNMC: “The men and women who choose to work in the field of infectious disease are highly qualified. And they pretty much self-select. It’s like selecting to specialize in surgery, where you’re dealing with open bodies on a surgical table. There’s risk in it, peril. You have to be able to rely on yourself. And trust the team around you. These men and women are interested in the discipline of their process. They must trust their own abilities above all. The rigors appeal to them, and define them.”
I also leave my glasses behind in restaurants all the time, but I’m not telling them that.

The pace of the response to infectious disease appeals to Larson. “I’m going to go hang this bag,” she says of the medicine. “Then I’m going to go downstairs and begin training a new group of seven new nurses, who are going to come onto the staff. A full second team to work with and trust. More lab work to be done. More blood that can be worked with. That’s more work. That’s urgency.”
Urgency can be debilitating. The demands of the novel coronavirus crisis, and the ramped-up research effort, have led her to weeks of 16-hour days. She admits she is exhausted. “No one has a special right to claim they’re tired,” she says. “Not while this is happening.”
She is tough, LuAnn Larson.
She returns home to her husband and college-aged daughter every night, if only for some baked chicken and a little sleep. They lived together through the worries of Ebola. “At the end of the day, whenever that finally comes, I go home,” she says. “I take off my scrubs. I throw them in the wash. Our house is a clean zone. We take that on. We work on understanding that. There’s plenty to respect. But no fear.”
She doesn’t bite when asked about the culture of Nebraska, where she was born, being particularly well shaped to this kind of work. “I think it’s an excellent culture,” she says. “Yes. But there are a lot of places where this sort of work could happen. People just need to be schooled. Prepared. You have to live through it.”
Do people beyond her family ever react to her presence? I mention the rumors about the children of quarantine workers being shunned from birthday parties. “Parties? No,” she says. “But months after Ebola, I was asked to leave a hospital in Texas because they found out I had done work in the biocontainment unit.”
She sighs. Preparing people came into play: “They just didn’t know. I schooled them. I informed them about what they should be actually looking for, about what we do here,” she says. This too is the work of the place, the lessons that come between the plagues. “And in the end, I left. I respected their wishes.”
She doesn’t think that act took any particular courage. She seems to have rethought courage. “I think what drives the culture of work with infectious disease is less about courage than it is resiliency. Maybe that’s Nebraska,” she says. “And this is energy. It’s exciting. It’s good to be on the forefront of this event. And being a part of something larger than yourself. It’s energizing. Important.” She stands, offers an elbow bump—the defining gesture of a moment of closure in this, the defining moment of physical distancing—before she goes to hang her bag of remdesivir.
Grant Fabry
Nurse and Clinical Instructor, UNMC College of Nursing

Sometimes he wakes up in Omaha to news of a distant planet where it rains iron. For reals. Raindrops of iron. He reads this on his phone while lying in bed.
He gets up, walks his dog, thinks about the lacrosse game he has this Saturday.
Grabs a shower, eats something, scans the newspaper.
The news there? The president has banned travel from Europe. Not to Europe, just from it. It’s a puzzle.
He drives to work. As he does, he considers his dog, a Great Dane. A good girl. She weighs 127 pounds, which makes her a small Dane, which he decides is pretty much true of any Dane. Man or dog, 127 pounds is not that much. By the time he gets there, the news from the satellite radio is: Tom Hanks has the virus. His wife, Rita Wilson, has it, too. And on this day, that news feels serious.

He’s a nurse. He works for Nebraska Medicine. Normally, he works in oncology and critical care unit, but now, during this coronavirus crisis, having trained and volunteered for assignment in UNMC’s biocontainment center, he’s on an upper floor of the Durham Outpatient Center. Corner 43nd and Emile.
He goes into the locker room, changes into his scrubs. Then he pads into the hall, where the two federal marshals sit at a table outside the staff door, monitoring all entrances and exits.
He gives a good morning, they check his ID, make a notation, and wave him past. Most days, that’s about all he gets. One time, his guest asked them if they were actual marshals. “We can’t comment on that,” they said in unison.
He has to be conversant with the process and its standards, and for this he has trained long in advance. Drilled often. He has to be diligent in clinging to individual subtleties of donning. A beard, for instance, even the presence of facial stubble, requires a different masking procedure to create a safe seal against the face.

It is a grind. And he accepts that it is dangerous. But he’s a nurse. He knows his family is proud of the work he’s chosen here. His wife is proud of him. But like nearly every sensible person in Omaha, in Nebraska, in the country, or, yes, the entire world at this moment in history, they have worries. For him. About him, about what he does, about what might come out of there with him.
Sometimes he feels the eyes of his neighbors, who know where he works without fully understanding the protection he is offered on the unit. During the Ebola crisis, the children of medical staff assigned to the unit were sent home from birthday parties by concerned neighbors. Some wanted them out of the schools.
In the weeks and months that followed, word spread about the demands of the protection provided. Locals began to accept that this might just be a part of the work that makes living in Nebraska what it is—a kind of heartiness, a resilience. The calling of work is elemental in Nebraska. People here seem to agree on that much.
After the full donning process is complete, a solid 12 minutes after it began, 34 minutes after he arrived in the building, and three hours after waking, he just wants to get on the unit. To reach his patients. He stands in his suit of plastic and linen, rubber and tape. He breathes against one mask, from behind another, breathes from behind a shield of plastic. He takes stock. He ticks off the donning lists. He confers with his partner. He tries to make eye contact. He always makes eye contact.
He has learned to not let eagerness substitute for readiness. He surrenders the world behind him—the car ride, the waffle, the news of that planet with the metal rain—before he enters the unit. The news of the day stops coming to him then. He refuses to give in to weariness, in order to give in to the process that protects him, his partners, his team, and the world beyond the doors.
He passes through the donning area, past a nursing station, through a set of pressurized double doors, where he encounters a set of patients in separate isolation rooms. Just sick people, who need water. Comfort. A better blanket.
Help with breathing.
Just help.
Then he goes to work.
With additional reporting by Bronwen Dickey.
You Might Also Like

