A Tragedy in the Kennedy Family Saved My Preemie — and I Got the Chance to Thank Them

- Oops!Something went wrong.Please try again later.
- Oops!Something went wrong.Please try again later.
- Oops!Something went wrong.Please try again later.
- Oops!Something went wrong.Please try again later.
Courtesy Holly Jordan
Holly Jordan, who works in business development in New York, gave birth to her son prematurely. Like Patrick Kennedy, her son was born with Respiratory Distress Syndrome, (RDS) but unlike Patrick, he survived. Below, Jordan writes about her experience in the NICU and her fateful meeting with Caroline Kennedy, the last surviving member of Patrick's immediate family.
The day before Easter, my husband and I decided to take our pup, Wally, to Central Park. Pete and I needed to get out too—we had been spending our time in shifts at the neonatal intensive care unit since December and hadn't been on a walk together in ages.
Wally immediately took a keen interest in another woman's dog. The woman looked familiar. As I walked closer, I realized she was the one person I most wanted to meet if given the chance.
It was Caroline Kennedy. And what I wanted to tell her was that my son was alive because of her brother, Patrick.
We had gotten Wally a year before, at the height of lockdown. I had been trying to manage a hollow grief from losing my mom suddenly to cardiac arrest, the same way my father passed in 2005. I was just starting to come out of the fog when COVID hit.
Wally helped heal my pain. People had joked that having him around would help me get pregnant, something about igniting maternal instincts and being more relaxed. A few months later, two pink lines appeared on a pregnancy test.
The first trimester brought the expected nausea, fatigue, and cravings. We signed up for "your baby is now the size of an avocado" emails and shared the news with friends.
In the middle of the second trimester, things got trickier. My blood pressure, always on the low side, began to increase for short intervals, and I had occasional shortness of breath that made me uncomfortable and anxious. We bought a blood pressure monitor and started recording the numbers. I was aware of blood pressure complications with pregnancy and tried to stay off Google.
RELATED: Identical Micro-Preemie Twin Girls Among Youngest Babies to Be Born at Iowa Hospital
Then, at a routine scan during my 24th week, after staring intently at the doppler for several minutes, the technician asked me about my blood pressure. I told her about the occasional bursts of 140s over 90s. Without a word, she left the room to fetch the doctor. He came in and looked closely at the monitor. He faced me and told me he was admitting me to labor and delivery at the hospital.
I cried, grabbing his shoulders. "I'm giving birth today?"
"I'm not saying that, Holly, but I'm also not not saying that either."
He diagnosed me with hypertension and ordered more tests. I called my husband and shared the news in a whisper. We were shocked in disbelief, yet privileged to be at one of the best hospitals in New York with health insurance. The attending physician told me that the goal was to get me to 34 weeks—two and a half months away. "Try to get comfortable," she said.
Pete brought over books and friends sent soft pajamas and games. A few days after being admitted, I could no longer sit without intense shortness of breath. My energy all but disappeared.
The next two weeks were spent lying in the hospital bed, white knuckling it through every scan, praying, and listening to my baby's heartbeat at night. My condition deteriorated. I needed several interventions to lower dangerously high blood pressures, and lab results showed elevated liver enzymes and low platelets. I had full blown preeclampsia and HELLP syndrome, life-threatening pregnancy complications. The conditions were unstoppable and had no known causes other than placenta insufficiency.
They pumped me with high doses of magnesium to prevent seizures and protect my baby's brain, gave me several rounds of steroids to help his lungs, and told me that my son needed to come out, 14 weeks early, for his sake and mine. NICU doctors tried to prepare me for what was coming next. "Rollercoaster" is the word they kept saying.
I knew next to nothing about preemies except for the occasional story I saw on morning television about miraculous, one-pound triplets born under touch-and-go circumstances, now healthy and in the laps of their beaming parents.
I would learn.
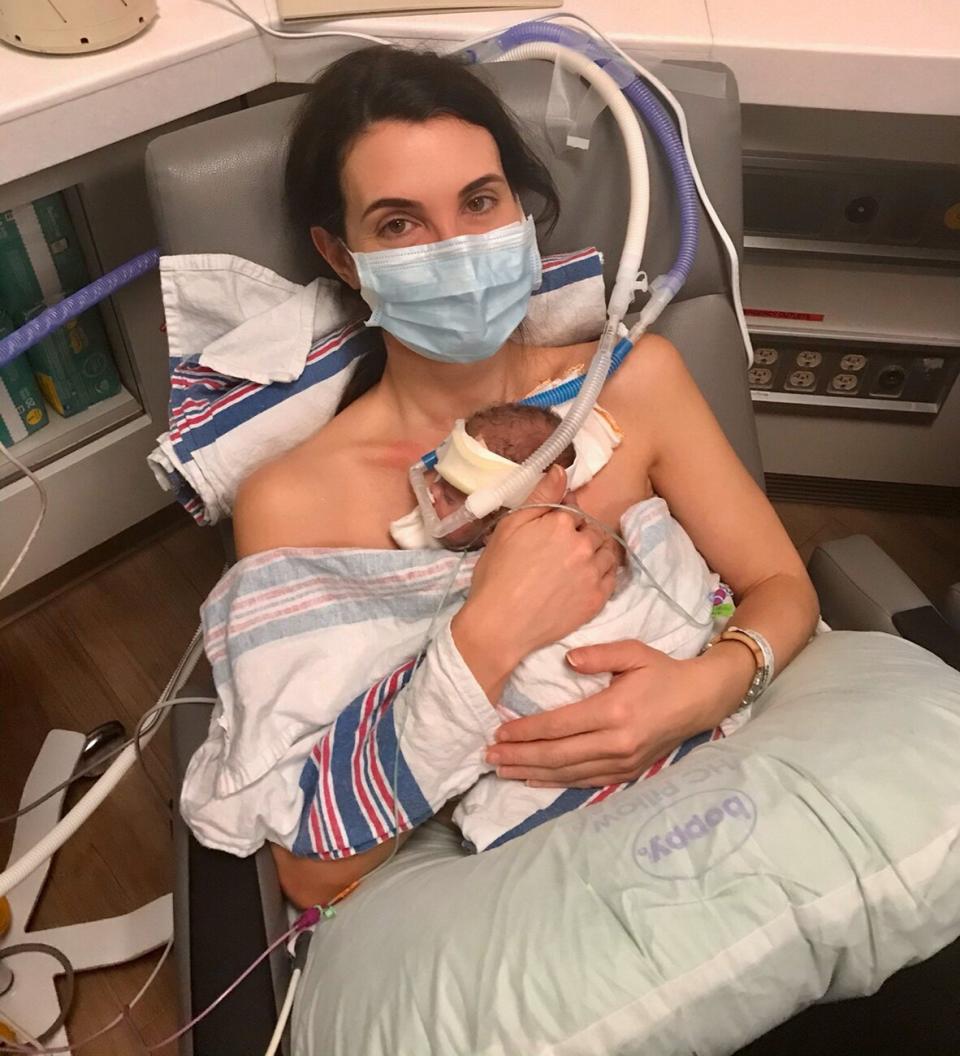
Courtesy Holly Jordan
The first time I saw my son was in the NICU. It was late, the lights were dim, and it was quiet and hot. I was guided to his bedside where they had a chair waiting for me. Recovering from a c-section, I couldn't stand or walk without support. Through the tubes, machines, and wires, I saw a thick swath of dark brown hair that I immediately recognized. He was mine.
I surveyed the room. We were in the most critical part of the unit. The weights written by each isolette were all under two lbs. Disoriented, I tried to make eye contact with another mom whose baby was born earlier than my son, but she didn't look over. I later learned she had been there for months and understood her need to block out the surroundings.
The nurses went about their days seemingly unfazed, measuring breastmilk in cc's, changing diapers the size of mini candy wrappers, keeping laser-like focus on the babies' pulse oxygen levels. The neonatologists rounded twice a day, discussing each baby by their isolette. We learned a new language as they reviewed the cases: "the jet," "bubble c-pap," "desat," "brady," "room air". We were living in a separate world, and these were now our people.
At first, the only thing we could do for our son was "hand hugging," reaching through the small openings of the isolette and placing our hands with a steady touch at the head and foot of his swaddle. We spoke to him quietly so he could hear our familiar voices without being overstimulated.
As our son got a little bigger and more stable, I started holding him skin-to-skin, which is known to benefit preemies and their mothers. Each day, he slept against my chest for hours. Several times while holding him, his heart rate and blood oxygen levels plummeted, setting off the alarms. He had to be taken off my chest and stabilized in his isolette. We were living in a constant state of fight or flight, and I was always bracing.

Courtesy Holly Jordan
The unit was cramped, with babies right next to each other. I had never seen life this close-up before. These tiny creatures, physically not ready for the world, yet doing their best to adapt and keep going. I didn't know that fragility and resiliency could co-exist like this. It was terrifying. It was miraculous.

Courtesy Holly Jordan
Want to get the biggest stories from PEOPLE every weekday? Subscribe to our new podcast, PEOPLE Every Day, to get the essential celebrity, entertainment and human interest news stories Monday through Friday.
To try and make sense of what was happening, I read a book, Early: An Intimate History of Premature Birth and What it Teaches Us About Being Human. I learned about a preemie who lived less than two days but whose life became part of medical history. The baby's name was Patrick Bouvier Kennedy.
This is the reason I wanted to meet Caroline. She was Patrick's sister, and the last surviving member of his immediate family. My husband and I were immeasurably grateful for what her father did following Patrick's death. I wanted to share my gratitude.
After several minutes of neighborly small talk in the park, I asked her name.
"It's Caroline," she said.
My opportunity to say something was now or never.
I took a deep breath. "Caroline, my son is alive because of your brother Patrick."
She froze. "What do you mean?" she said.
"My son was born very early at 26 weeks and 4 days at Lenox Hill hospital," I said. "His lungs weren't fully developed, and he had Respiratory Distress Syndrome, just like Patrick."
"Patrick had Hyaline Membrane Disease," she said.
"Yes," I nodded. "That's the same as RDS." I shared what I had learned after reading so much about her brother. Patrick was what the NICU would call a 34 weeker, born 6 weeks early in August 1963. Jackie had suffered painful complications with her pregnancies, including miscarriage, stillborn and premature birth. She faced all of them, showing no woman is immune from experiencing these potential risks, not even the First Lady.

John F. Kennedy Presidential Library and Museum President Kennedy travels with Caroline Kennedy and John Kennedy Jr. to visit Patrick Kennedy in the hospital
After Patrick's birth at a small military hospital in Cape Cod, his mother's obstetrician placed him in an incubator and pumped in vast amounts of oxygen, despite the risk for blindness. The President and First Lady's baby wasn't doing well. He was struggling to breathe. His skin was turning blue, and his chest retracted with each breath. He was transferred to Boston Children's Hospital, where more doctors and nurses were on hand. But the science didn't exist to properly treat him. NICU's hadn't been established.
Headlines across the country announced Patrick's early birth with uncertainty and Americans nervously awaited an update. Desperate to save him, his medical team's last resort was to put him in a hyperbaric oxygen chamber located in the hospital's basement. With President Kennedy watching through portholes, Patrick's condition improved for a short time but then declined. He suffered the final agonizing stages of RDS, his tiny body fighting until he could do it no longer. He lived 39 hours.

Kennedy Library Jackie Kennedy places flowers on the grave of her husband at Arlington National Cemetery in March 1967. Patrick and their stillborn daughter Arabella lie next to his gravesite.
After learning about Patrick, my thoughts went to his mother, left behind in a Cape Cod hospital as they tried to save her baby. I thought about how she faced the trauma of losing him in the public eye, and then, just three months later, she faced another tragedy when her husband was killed. The country, in despair over the assassination, forgot about what had just happened to their son.
Yet in those few months between, a medical transformation took place.
The President started asking questions about why his son didn't survive. He learned only a handful of doctors were beginning to study prematurity. His grief called him to action. He shone the Presidential spotlight on RDS, and as a result, the National Institutes for Health (NIH) received funding for research.
"And what did that do?" Caroline asked.
"They figured out they could put babies on ventilators," I said.
They also figured out they could give preemies surfactant, a protein derived from cows that opens airways and makes it possible for immature lungs to function. Surfactant and breathing intervention became the main treatments for RDS. And once that was determined, babies born as early as 23 weeks could survive.
We stood there. The Jackie Kennedy Onassis reservoir gleamed in the background.
"I was so young," she said. "I didn't know."
Never miss a story — sign up for PEOPLE's free daily newsletter to stay up-to-date on the best of what PEOPLE has to offer, from juicy celebrity news to compelling human interest stories.
Of course she didn't know. People working in Neonatal Intensive Care are aware of Patrick's impact, but those outside this world are not.
"Four hundred thousand babies are born early in the U.S. every year," I said, "and because of Patrick and your dad, they have a chance not only to survive but to thrive."
In 2022, a 34-weeker in the U.S. has close to a 100 percent survival rate; in 1963, babies like Patrick faced almost a 100 percent fatality rate.

SAEED KHAN/AFP/Getty Caroline Kennedy, who is now serving as the United States Ambassador to Australia
She understood: In her lifetime, countless babies had been saved because of her brother's short yet consequential life and her father's impact. I, a New Yorker standing in Central Park, was proof of it; and so was my warrior baby, 20 blocks south in the expert care of neonatologists and NICU nurses.
"What's your son's name?" she asked.
I told her, and she smiled.
"Happy Easter," she said, before making her way west with her dog.

Courtesy Holly Jordan
The day my son was discharged, the NICU team wheeled us out together even though I had been walking around the unit for months. His medical team lined up and applauded. Graduation music played and I cried tears of relief, joy and exhaustion. At long last, the monitors showing his blood oxygen levels, heart rate and respiratory rate were shut off. He was free of neonatal intensive care interventions and overcame RDS and prematurity because of them.

Courtesy Holly Jordan
Our son is a healthy, happy toddler, full of joy and curiosity. Every milestone is meaningful, and every giggle is treasured. We go to Central Park often as a family, and Wally being protective, stays right beside the the stroller. He doesn't know our son is the most resilient of the pack.
