Harvard scientist's 'doorknob' question leads to skin cancer diagnosis
Jeff Karp had just undergone his first full-body routine skin cancer check in the spring of 2022 and was about to walk out of the exam room, when, on a whim, the 47-year-old decided to ask his dermatologist about a spot on his cheek.
It was small — less than half an inch across — and faintly red. Karp first noticed it a year or two earlier, but thought it was part of the aging process. Everything during his full-body scan was normal and the visit was over, so the question came out of the blue.
“I kind of debated whether I should ask about it or not,” Karp, Ph.D, a biomedical engineer and professor of medicine at Brigham and Women’s Hospital, tells TODAY.com. “The thought didn’t even cross my mind that it could be skin cancer.”
But that’s exactly what it was. Karp’s dermatologist took a closer look and recommended a biopsy.
The results: basal cell carcinoma, the most common type of cancer in the world, according to the American Academy of Dermatology.

This skin cancer tends to grow slowly and isn’t life-threatening for most people, but it needs to be treated before it can grow deep and injure nerves and blood vessels, the AAD noted. It's most common in people with fair skin who rarely use sunscreen.
The cancer can look like a pink or reddish growth that dips in the center, a sore that doesn’t heal or a spot that feels scaly.
Karp recalled getting “some pretty severe (sun) burns” when he was younger. He used to play two rounds of golf a day, staying out in the sun for eight to 10 hours. The scientist said he used sunscreen “here and there” but wouldn’t necessarily reapply it.
Karp’s wife had been encouraging him to get a skin check, but it wasn’t until March that he finally went.
The question he asked at the very end of his visit is known as the “doorknob phenomenon,” when a patient waits until the doctor has his or her hand on the doorknob to leave the exam room to reveal something that often provides crucial information.
After his diagnosis, Karp was getting ready to have surgery to remove the skin cancer when the surgeon noticed it wasn’t too deep and recommended using Aldara, a cream to treat superficial basal cell carcinoma, instead.
Karp was prescribed a six-week treatment, applying the cream five days a week, with weekends off. He chronicled the startling skin changes during that time by taking a photo most every day.

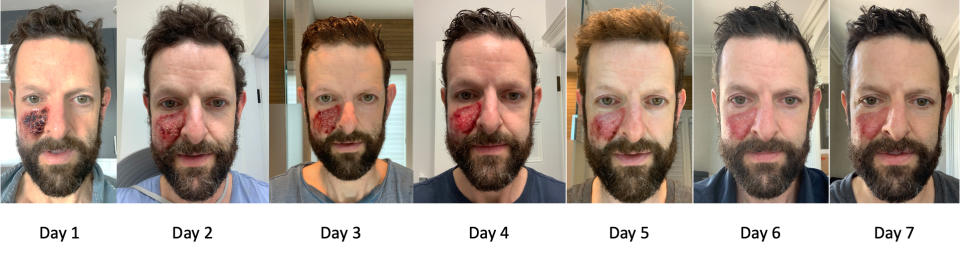
As a scientist who invents medical technologies and is fascinated by how things work, Karp explained the treatment this way:
“This cream is actually topical immunotherapy. It activates the local immune system in a very major way so that your immune system can then recognize the cancer cells and kill them,” he said.
“But in the process of activating the immune system, there’s a lot of inflammation that is caused, and what’s interesting is that inflammation also allows the cream, the therapeutic agent, to get in even deeper because your skin is more permeable because now it’s inflamed."
Karp finished the treatment in the summer of 2022. When TODAY.com caught up with him in May 2023, he said he is doing great, noting the spot has fully healed and the skin in the area is "super smooth," but with an "ever-so-slight pink tinge."
Navigating the world during the treatment was challenging, he recalled.
That area of his face was uncomfortable and sometimes oozed with blood, so he had to sleep with a towel on his pillow. Children stared at Karp when he was out in public, and he avoided making eye contact with people or walking near them because he didn’t want to make them uncomfortable. It took a toll on his mental health.
“When it got to the last couple weeks of the treatment, I debated whether I should stop it because I was just getting really down about it,” he said in 2022. “Now, I’m in this very positive space because the treatment is over. I’m clearly on the road to recovery, and I’m not as self-conscious about it.”
Looking back on the episode in 2023, Karp said he decided to proceed with the cream because doctors told him he could spread it over a larger area and help prevent future occurrences, which "sounded good at the time."
"However, based on my experience, I would definitely go for the surgery next time," he noted.
Karp now wears a wide brimmed hat outside and takes an umbrella with him for extra sun protection at outdoor events, like watching his son play football. He hopes others can learn from his ordeal and be more motivated to protect their skin, he wrote online. Karp says he now sees his dermatologist every six months and monitors his skin carefully.
"It’s so easy in the early spring or summer to forget about re-initiating a rigorous active plan for sun protection. I think pain and discomfort are strong motivators but can fade with time," he warns.
One way he's tried to address this is to keep sunscreen and hats in his car and in various locations around his house so they're always accessible.
When it comes to skin checks, dermatologists stress that patients need to be a partner in the process. Think of yourself and your dermatologist as a team. In between appointments, scan your body and take pictures of your moles to track any changes and show them to your physician.
“Everyone should get really familiar with their own moles because that’s what’s going to save your life,” Dr. Julie Karen, a board-certified dermatologist in New York City, previously told TODAY.
As for the “doorknob” question, Karp wasn’t surprised that that’s what it took to receive a diagnosis and stressed the importance of "collaboration with the dermatologist."
“(It’s) not just going in for a routine check, but also bringing to the attention of the dermatologist changes that you’ve observed over time that may require a deeper look," he said.
This article was originally published on TODAY.com

